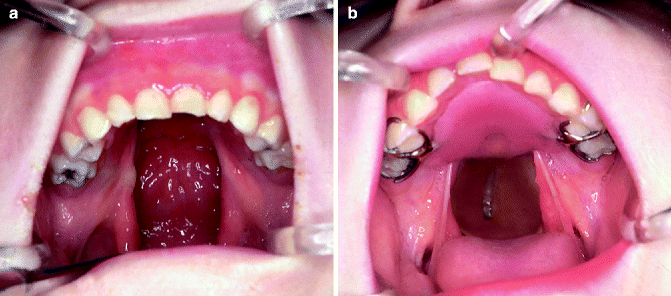
The design and construction of speech appliances and obturators have changed much in the last 20 years, mainly due to improved materials and methods. We have, for example, better wax, acrylics, and impression materials and superior stone and plaster for the investment process. We also have benefited from improved diagnostic tools for evaluating the results of prosthetic treatment. Greater coordination of interdisciplinary team efforts has helped establish a more ideal prosthetic concept, one that ensures that fixed or removable partial denture prostheses are managed so as to preserve the integrity of all remaining teeth and the surrounding soft and hard oropharyngeal structures.
The decision for prosthetic rehabilitation is made based on the individual patients’ needs, motivation for improvement, and availability of the suggested rehabilitative program. Approximately, 50 % of all patients with cleft lip and palate will need some type of fixed or removable prosthesis by 30 years of age.
As our knowledge and experience in the cleft palate field increased, those of us responsible for providing prosthetic care recognized the importance of establishing a better prosthodontic concept and principles regarding treatment. In rendering these patients the best service, we should first follow all the rules and principles governing the fixed and removable partial denture prosthesis and, secondly, should remove any fear of causing harm because of existing anatomic, functional, and physiologic deviation.
39.1 Diagnosis and Treatment Planning
In treating people whose oral-facial handicaps affect speech, the best results are achieved when the diagnosis and treatment are carried out by a group of clinicians who represent the various interested specialities and work together as a team rather than independently performing a series of procedures.
In diagnosis and treatment planning, full consideration should be given to (1) the type and width of the cleft; (2) the position and relation of the maxillary segments to each other in unilateral and bilateral clefts; (3) the form and lateral and anteroposterior dimensions of the maxillary arch; (4) the length, thickness, and mobility of the soft palate; (5) the perforations remaining in the hard and soft palate area and labial sulcus after surgery; (6) the posterior and lateral pharyngeal wall movement and the size of the nasopharynx; (7) a loose premaxilla; (8) the number of missing teeth; (9) malformed and malposed teeth; (10) partially erupted teeth; (11) teeth in the line of the cleft; (12) constricted maxillae; (13) the condition of the tonsils and adenoids; and (14) growth and development of the child. The patient’s articulation, voice quality, hearing acuity, mental attitude, and general health also must be considered.
Socially acceptable speech cannot be produced without proper velopharyngeal valving. Therefore, surgical closure of the palate without due consideration of the depth of the nasopharynx and the length and function of the velum during phonation cannot satisfy this objective. Better understanding of the nature of the cleft, anatomy, and the physiology of the area involved would eliminate many of these difficulties. The results of surgical treatment of cleft palates should be evaluated with the aid of cineradiographic studies, nasal endoscopy, serial cephalometrics, maxillary and mandibular casts, speech recordings made before and after surgery, sound spectrographic analysis, measurements of nasal and oral air pressure and flow, and speech and audiometric evaluations.
All members of the team should be thoroughly familiar with the problem at hand. Often, the best result is not achieved when the knowledge of the specialists is not all encompassing (Cronin 1957).
The total habilitation and rehabilitation in the field of oral, facial, and speech impairment is achieved only when the following objectives are kept in mind: (l) socially acceptable speech, (2) restoration of the masticating apparatus, (3) aesthetic facial and dental harmony, and (4) psychologic adjustment of the patient to the condition.
Use of a speech appliance simply as a last resort is poor procedure. Its use must be clearly indicated by the oral conditions. For example, the indications for a prosthesis are clearly defined for a patient who has undergone a series of unsuccessful palatal operations. There is no magic in a prosthetic speech aid. However, there are some patients for whom a prosthesis seems to be the only means of improving speech. In such situations, it fills a definite need. A prosthetic speech aid should be used for palatal conditions where it is indicated, just as the pharyngeal flap operation should be used only where it is indicated.
39.2 Treatment Planning
Treatment programs for cleft palate patients require careful planning and should include all factors involved in total health care. The interest of the dentist and physician in craniofacial growth and behavior of soft and hard tissues, both before and after surgery, has increased cooperation between surgeons and dentists. As a result, a dental specialist has the opportunity to examine the cleft palate child, with the surgeon, before any surgery is undertaken. Analysis of longitudinal maxillary and mandibular casts, cephalometrics, and radiographs has shown that two major factors cause growth disturbances of oral-facial regions in individuals with clefts: first, the inherent potential for growth disturbance present among cleft palate patients and, second, the trauma caused by surgical and orthopedic intervention. Because the first factor can be neither predicted nor reduced, efforts have been directed toward minimizing growth disturbance by performing surgery with the least amount of trauma and scar tissue. Longitudinal data obtained during the past 4 years regarding the surgical closure of the cleft with minimum amount of scar tissue and trauma are very encouraging (Millard 1966).
39.3 Requirements of a Speech Appliance
1.
The prosthesis must be designed for the individual patient in relation to his oral and facial balance, masticatory function, and speech.
2.
Knowledge related to removable partial and complete dentures should be used in designing the maxillary part of the cleft palate prosthesis. Preservation of remaining dentition and surrounding soft and hard tissue in cleft palate patients is of utmost importance. Improperly designed cleft palate appliances can result in premature loss of both hard and soft tissue, further complicating prosthetic habilitation.
3.
The prosthetic speech appliance should have more retention and support than most other restorations. The crowning and splinting of the abutment teeth in adult patients may increase retention and support of the prosthesis and may extend the life expectancy of abutment teeth.
4.
Mouth preparations should be completed before making final impressions. In cases where lateral and vertical growth of the maxilla is incomplete and partial eruption of the deciduous and permanent teeth is evident, careful mouth preparations should be made. To provide support of the prosthesis, these preparations may include gingivectomies to expose clinical crowns (to make them usable) and the placement of copings on remaining teeth to prevent decalcification and caries. Osseointegrated implants have been a great help in gaining adequate retention for the prosthesis.
5.
The weight and size of the prosthetic speech appliance should be kept to a minimum.
6.
The materials used should lend themselves easily to repair, extension, and reduction.
7.
Soft tissue displacement in the velar and nasopharyngeal areas by the prosthesis should be avoided.
8.
The velar and pharyngeal sections of the prosthesis should never be displaced by movements of the lateral and posterior pharyngeal wall muscles or the tongue during swallowing and speech.
9.
The superior portion of the pharyngeal section should be sloped laterally to eliminate the collection of nasal secretions. The inferior portion of the pharyngeal section should be slightly concave to allow freedom of tongue movement.
10.
The location and the changes of the speech bulb should include consideration of the following factors:
(a)
The speech bulb should be positioned in the location of greatest posterior and lateral pharyngeal wall activity, because voice quality is judged best when the speech bulb is at these positions.
(b)
The inferior-superior dimension and weight of the speech bulb may be reduced without apparent effect on nasal resonance. (The lateral dimension of the bulb does not change significantly as the position is varied.) (Fig. 39.2)
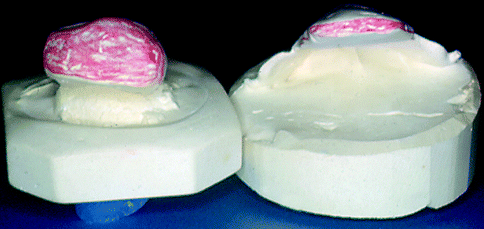

Fig. 39.2
As a result of our studies, we have concluded that the inferior-superior dimensions of the speech bulb do not have a significant effect on speech quality as long as the bulb is properly placed to facilitate good velopharyngeal closure. This dimension was reduced to one-quarter of its original size, as shown in cast made during fitting for one patient, without apparent effect on nasal resonance
(c)
The speech bulb should be placed on or above the palatal plane in cases where posterior and lateral pharyngeal wall activities are not present or where visual observation of the bulb is not possible, due to a long, soft palate (Fig. 39.3).
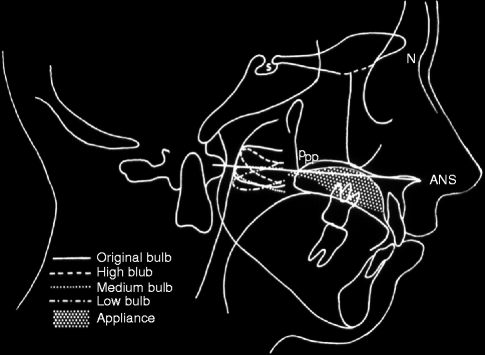

Fig. 39.3
Superimposed tracing of the original speech bulb and various experimental speech bulbs. The palatal plane was used as a plane of reference along with posterior pharyngeal wall activity, muscle bulge, or Passavant’s pad. The posterior nasal spine (PNS), absent in cleft palate subjects, is called posterior palatal point (Ppp) and represents the most posterior point of the remnants of the palatal shelves as shown in the lateral cephalometric film. Median position was judged best
(d)
The anterior tubercle of the atlas bone can be used as a reference point; however, investigation has shown that the relative position of the tubercle of the atlas bone varies in different individuals and that the positions of the velopharyngeal structures change in relation to the tubercle as the individual moves his or her head. Therefore, the atlas bone is no longer used as the reference point for positioning of the pharyngeal section of the bulb.
39.4 Indications for Prostheses in Unoperated Palates
Cleft palate surgery is not a stereotyped exercise, but rather a service that demands an assessment of all factors presented by each patient and a reparative surgical plan based on proven principles. The majority of cleft palates can be reconstructed by surgery, enabling the patient to develop acceptable velopharyngeal closure. However, in some situations, a prosthesis is the physical restoration of choice. This decision should be made by the group charged with the habilitation of the cleft palate patient.
Many clefts of the hard palate can be closed by a vomer flap (Mazaheri 1973; Veau and Borel 1931) and clefts of the soft palate by median suture with good anatomic and functional result. The wide cleft and the short palate demand further attention. Additional length may be gained by a Dorrance or V-Y type retropositioning operation. The raw nasal surface may be covered with a skin graft, nasal mucosa, or an island flap of palatal mucosa (Cronin 1957; Giles and Fry 1921; Veau and Borel 1931). The incompetent palatopharyngeal valve can be augmented by a pharyngeal flap, as either a primary or secondary procedure (Grabb et al. 1971). The need for additional tissue in a wide cleft can be satisfied by single or double regional flaps.
Despite the surgical advances available to the cleft palate patient, a need remains for cleft palate prostheses. The prosthodontist can assist both the surgeon and patient, and the mutual understanding among the specialists in a well-organized team is of great benefit to the patient. Some situations indicating a prosthetic approach are discussed in the following paragraphs.
39.4.1 A Wide Cleft with a Deficient Soft Palate
Some clefts of this type do not lend themselves to a surgical repair by means of local flaps. A prosthesis is preferable to the more time-consuming remote flaps in these situations. Many patients need a prosthesis to restore missing dental units, and the distant tissue provides only a dynamic mass (Figs. 39.4 and 39.5).
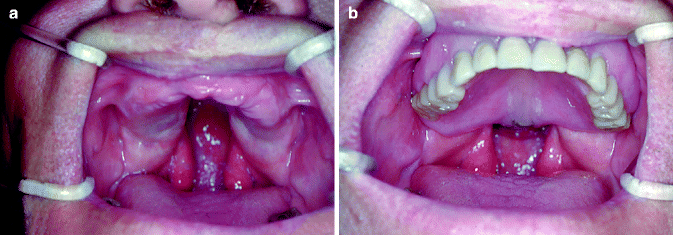
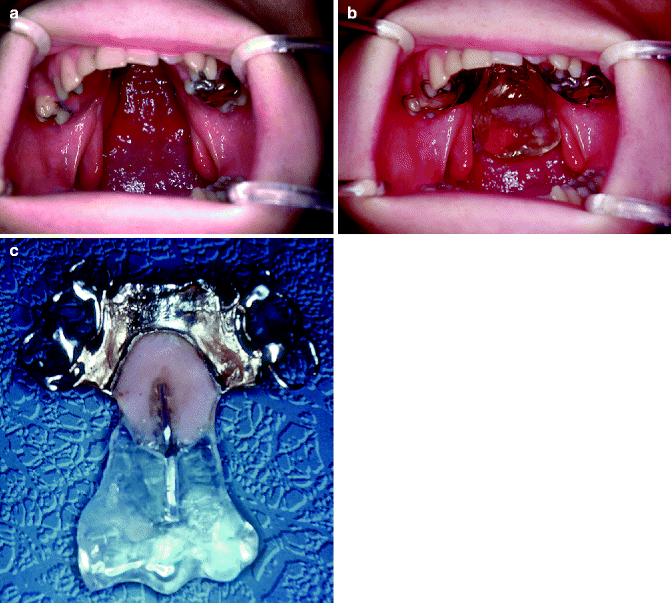

Fig. 39.4
(a) An edentulous patient with an unoperated cleft of the soft and hard palate that affects the retention and support of the prosthesis. At no time should a patient with a cleft, especially an unoperated cleft, be rendered edentulous. (b) The completed prosthetic speech appliance in position

Fig. 39.5
(a) Patient at the age of 16 years with a very wide cleft of the soft and hard palate. (b) Prosthetic speech aid in position. Note that the pharyngeal section of the speech aid is placed directly over the posterior and lateral pharyngeal wall muscle activities. (c) Oral view of prosthetic speech aid. The utilization of second bicuspids and first and second molars for retention and support will prevent this prosthesis from dislodging into the nasal cavity during swallowing and speaking
39.4.2 A Wide Cleft of the Hard Palate
In bilateral clefts, the vomer may be high and the cleft of the hard palate wide so that a surgical repair may produce a low-vaulted palate. It may be possible to close the soft palate with the aid of local flaps and to restore the hard palate with a prosthesis. A situation similar to that once advocated by Gillies and Fry (Limberg 1927) is created: the primary repair of the velum may create a more favorable spatial arrangement for subsequent surgery on the hard palate.
39.4.3 Neuromuscular Deficiency of the Soft Palate and Pharynx
Repair of the palate would not be conducive to the development of good speech. It is difficult to create and maintain a pharyngeal flap large enough to produce competent palatopharyngeal valving without obstructing the airway in the presence of a neurogenic deficiency of the critical muscles. A pharyngeal flap serves best when surrounded by dynamic musculature. When this situation does not exist, the pharyngeal section of a speech-aid prosthesis may serve better to reduce nasality and nasal emission. The prosthesis can also act as a physical therapy modality, providing a resistive mass for the muscles to act against. Should muscle function improve, definitive surgical measures can then be contemplated.
39.4.4 Delayed Surgery
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses