Use Nonextraction Treatment When Possible
The previous chapters have outlined in detail specific principles that are necessary to follow in order to consistently produce high-quality, stable results. These next traction and extraction cases is discussed.
It is important to understand the basic Alexander Discipline philosophy of treating skeletal malocclusions. In most cases, a skeletal Class II patient presenting with a Class II molar relationship is corrected by control of growth, not by the mesial and/or distal movement of teeth to obtain the proper occlusion. Occasionally, in patients with a skeletal Class I pattern and dental Class II malocclusion, maxillary molars may be distalized. However, the teeth must fit within the alveolar trough. Although this trough can be widened in the posterior areas, the mandibular anterior segments allow only limited changes. Therefore, the flaring of mandibular anterior teeth to reduce overjet in most patients is unstable and unwise.
In typical patients who are to be treated with nonextraction therapy, the mandibular arch has minimum to moderate crowding. As stated earlier, the arches are treated independently.
The question is how to correct the skeletal Class II problem. In growing children, this is best accomplished with facebow and class 2 elastics. In adults (nongrowing patients), the solution is either to extract maxillary premolars or to consider surgical mandibular advancement. Principle 14 discussed how the mandibular arch is leveled in nonextraction treatment of deep bite patients, both children and adults.
Assessment of Borderline Patients
In determining if a patient can be treated without extraction, the primary question is whether the mandibular arch crowding can be resolved while the anterior teeth are maintained in acceptable positions. This decision is based partly on the extent of the mandibular tooth size–arch length discrepancy. In general, 4–6 mm of arch length can be “controlled” with good mechanics. This additional 4–6 mm of space can be gained by slightly advancing the incisors and uprighting the molars. More space can be gained if the posterior transverse dimensions can be expanded.
In my experience, approximately 15% to 20% of patients are definitely extraction cases. Another 50% definitely do not require extraction. The critical area is the other 30% or so of patients who are borderline cases. In our practice, nearly all of these borderline patients are treated without extraction. Five factors allow the use of nonextraction therapy and enable the mandibular incisors to remain positioned upright over basal bone:
1. Space gained by transverse expansion with rapid palatal expanders and lip bumpers. Studies by Adkins et al1 and Chung and Font2 show that there is a 0.6–0.7 mm perimeter increase for every millimeter of posterior expansion.
2. The –5 degrees of torque built into the mandibular incisor brackets maintains proper uprighting, while, at the same time, the –6 degrees of angulation in the mandibular first molar brackets will upright the mandibular molars, creating more arch length in the distal segments.
3. The use of rectangular flexible archwires such as braided stainless steel, nickel, copper, and titanium wires allows mandibular anterior torque control, beginning with the initial archwire.
4. Judicious use of class 3 elastics with the initial archwire can prevent the mandibular incisors from excessive labial tipping. The elastics can also increase available space by helping to upright the molars.
5. Interproximal enamel reduction of the dentition can create several extra millimeters of space in each arch. At least 0.25 mm of enamel can be removed from each interproximal surface of the mandibular anterior teeth. If the teeth are large, even more enamel can be safely removed.
Interproximal enamel reduction
Interproximal enamel reduction, also called slenderizing, is the removal of interproximal enamel. Although slenderizing is most often practiced in the mandibular anterior dental segment, it is not confined strictly to this area. It is possible to slenderize in any segment of either arch.
It is perfectly safe3 to remove up to 0.25 mm from each interproximal surface, which translates to 0.50 mm per tooth. Therefore, the tooth mass of the six anterior teeth can be reduced up to 3.00 mm. If mandibular premolars and first molars are also slenderized, tooth mass can be reduced by a total of 6.00 mm.
In choosing specific teeth to be slenderized, the orthodontist may have to perform a Bolton analysis. A visual inspection of the mandibular arch to examine the anatomic design of each tooth can also help the orthodontist to clearly define which teeth can afford more reduction in the interproximal areas.
The mesiodistal width of the maxillary incisors has a major effect on the amount of possible mandibular anterior slenderizing. If the maxillary central and lateral incisors are oversized and the mandibular incisors are not especially large, mandibular anterior slenderizing should not be performed alone as this would increase the tooth size discrepancy. It is possible in such cases to slenderize in both the maxillary and mandibular arches.
More commonly, the maxillary lateral incisors are usually found to be narrower, mesiodistally, than the ideal. This condition allows more enamel reduction in the mandibular incisors.
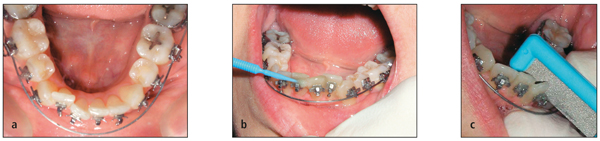
The initiation of mandibular interproximal enamel reduction can occur at the beginning of treatment or during treatment (Fig 17-1a). Furthermore, slenderizing remodels the mandibular anterior interproximal contact points into broader contact surfaces. The larger interproximal contact areas help to maintain the mandibular anterior alignment.
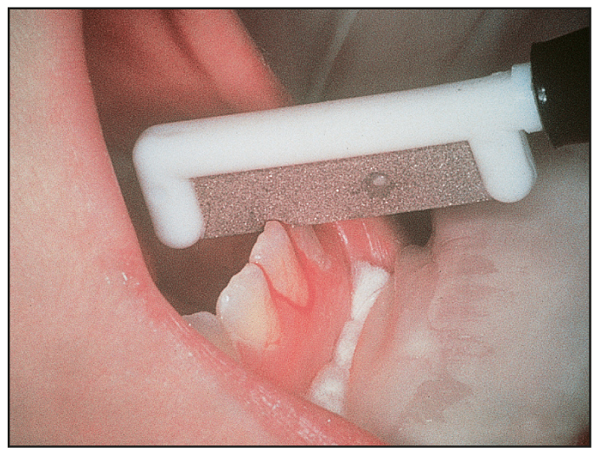
Slenderizing is performed with steel carborundum strips (Fig 17-1c), a diamond disk, or an air rotor handpiece. The diamond disk is used primarily on maxillary and mandibular anterior teeth that are large and bell shaped. The diamond disk removes enamel faster than carborundum strips, so it must be used with care. The abrasive strips can be used on all anterior teeth. I find them easier to use on crowded teeth during the early stages of treatment.
Fluoridated prophylaxis paste is used while slenderizing is performed (Fig 17-1b). The paste increases the life of the abrasive instrument because the paste becomes a part of the abrasive surface. When the diamond disk is used, the paste creates a smoother enamel surface. A rough surface could collect bacteria, which might cause interproximal caries.
Fig 17-1 Slenderizing procedure. (a) Crowded mandibular arch requiring slenderizing. Archwire is removed anteriorly for better access. (b) Prophylaxis paste with fluoride is placed before the procedure begins.(c) Interproximal enamel reduction with a steel carborundum strip (Dome).
Treating the newly exposed enamel with fluoride gel is important because the fluoride-rich enamel has been removed. Having performed this procedure on several thousand patients as well as myself, I have never seen interproximal caries develop.
In addition, the mandibular anterior teeth may be slenderized at the end of retention, immediately following removal of the fixed canine-to-canine retainer (Fig 17-2). This procedure allows for future anterior and lingual migration of the canines without concurrent mandibular anterior relapse.
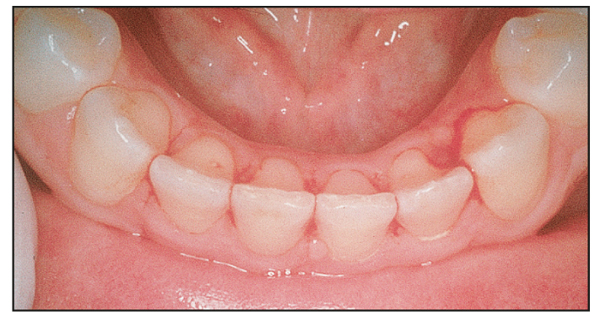
Fig 17-2b Immediately after slenderizing, note the flat contact surfaces from canine to canine.
Compliance
Another factor to consider in the treatment of a borderline case is patient cooperation. This type of case requires excellent cooperation to achieve the desired results. When such a case is to be treated, the parents must be thoroughly informed as to the treatment options at the consultation. In almost every situation, if the patient is willing to cooperate and is still growing, the case can be successfully treated without extraction of the permanent teeth. If, however, the patient is not willing to wear the extraoral and intraoral appliances as instructed, it may be best to perform the extractions.
In my early years in orthodontics, I had a tendency to be too idealistic and impose my beliefs on the patient and parents, without providing alternative treatment choices. However, over the years I have learned to be more realistic and to present all options to the patient and parents. If they are allowed to help make the decision, treatment becomes more of a team effort.
There are times when treatment will begin without extraction, but the patient is not able to fulfill his or her part of the agreement. As a result, extractions must ultimately be performed. In such instances, it is critical that the orthodontist closely monitor the progress of the patient. If not, 2 years can elapse before the clinician realizes that extractions are the only way to successfully complete the treatment.
By initially giving the borderline patient 6 to 9 months in treatment, the orthodontist can determine if the nonextraction therapy will be successful. If after that time the progress is not sufficient, extractions are recommended. Extraction choices in such cases are discussed in principle 18. A detailed description of treatment of borderline cases, which often includes expansion of both arches, will be presented in a future volume of this series.
Typical Nonextraction Mechanics
First, the maxillary arch is banded and bonded. At the same appointment, a 0.014- or 0.016-inch nickel-titanium archwire is placed to begin the process of unraveling the crowding, correcting rotations, and leveling the arch. At the next appointment 5 weeks later, the facebow is placed, if needed, to begin sagittal and/or vertical skeletal correction. At the third appointment, the initial wire is replaced with a 0.016-inch round stainless steel archwire to continue improving the dental alignment and leveling.
Arch consolidation
If the maxillary arch has any spacing, the 0.016-inch archwire is formed with curve of Spee (unless open bite) but without omega loops. Elastomeric chain is placed from f/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses