Fig. 31.1
(a, b) Reverse pull headgear given for retention
Minor complications are common during the distraction process and may have a bearing on the subsequent relapse rates (Hussain 2009). They need to be identified and managed as distraction proceeds. Incomplete osteotomy is the commonest cause of failure of distraction and a high rate of relapse. The commonest sites of incomplete osteotomy are the posterior-medial part of the maxillary tuberosity, the vertical plate of the palatine bone in the lateral nasal wall, and incomplete disjunction of the pterygoids. These areas need to be addressed with care while completing the osteotomy. Incomplete osteotomy even while allowing distraction to proceed initially may present as gradual increase in pain over the maxillary bone during the course of distraction. If this is not identified early and re-osteotomy performed, it may result in failure of anchorage of the distraction device and incomplete distraction. In some instances, distraction may continue by deformation of the unosteotomized part of the bone resulting in failure of distraction after some amount of advancement. It may rarely be possible to complete the distraction process, and if done, it will likely lead to a higher relapse rate in the postdistraction period. If one side is not osteotomized, it may result in asymmetrical advancement or increased unilateral relapse resulting in asymmetry. The other causes of asymmetrical distraction are improper adjustment of the device causing asymmetric movement of maxillary segments and dense fibrosis involving one segment. This needs to be identified, and the vector and the rate of distraction have to be adjusted deferentially. Another complication is the loosening of the pins holding the halo frame to the skull.
Consequences of the inevitable relapse are minimized by overcorrection. We routinely over-distract by 20–25 % to compensate for the expected relapse (Cohen et al. 1997; Cheung and Chua 2006). Open bite is another complication which can occur as distraction progresses and may be minimized by varying the vector of distraction. When this is not effective, postoperative orthodontics needs to be provided by using temporary anchorage devices to achieve a stable bite.
31.2.2 Evaluation of Relapse: Materials and Methods
We have evaluated the maxillomandibular skeletal changes including the relapse rates in adults following maxillary distraction with a mean follow-up of 3 years. This study was carried out at our University Hospital Craniofacial Center (Sri Ramachandra University, Chennai, India). Example of a case treated with rigid external distraction is illustrated in Fig. 31.2a–o.
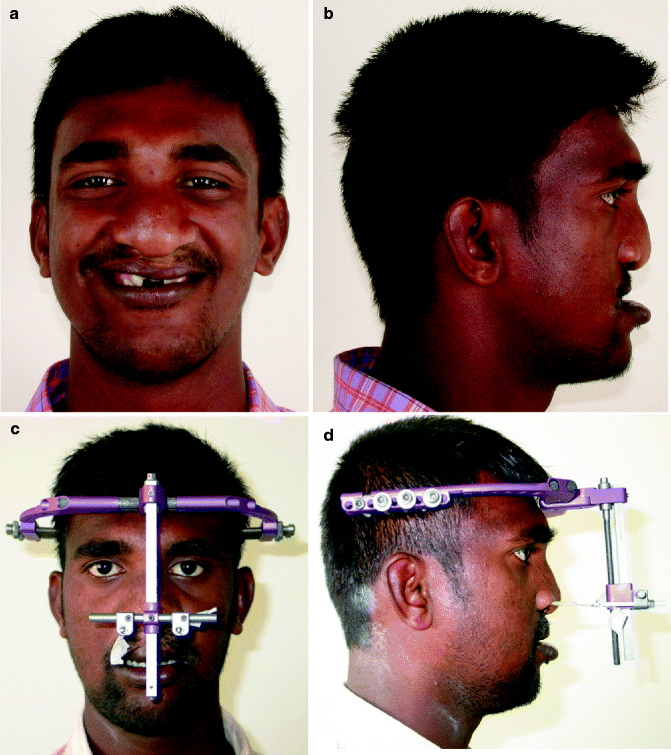
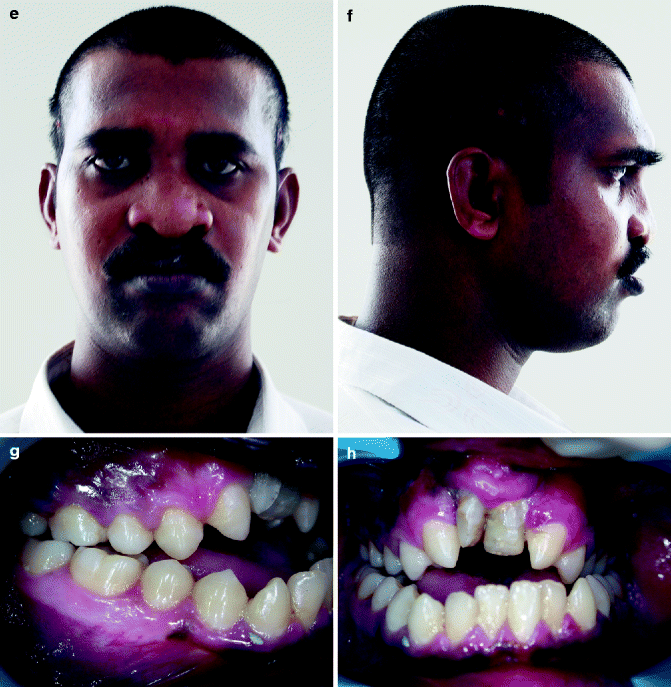
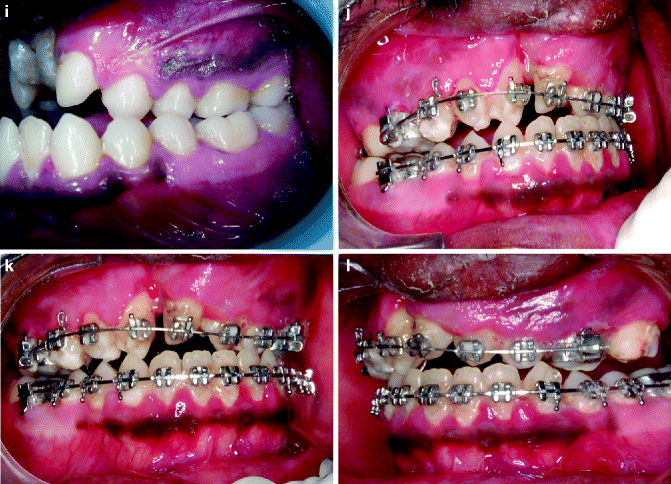
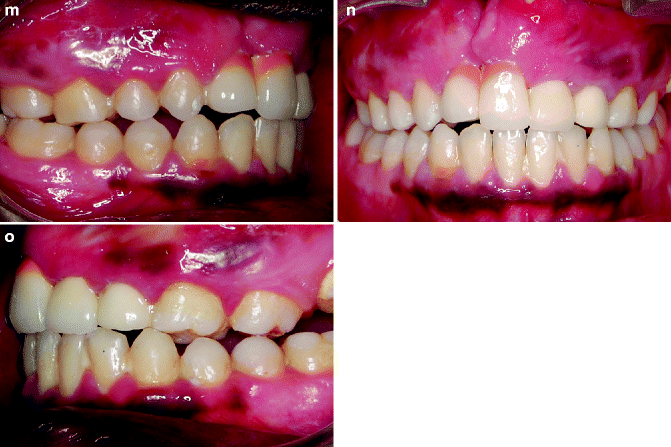




Fig. 31.2
a–o. (a, b) Pretreatment frontal and profile photographs. (c, d) frontal and profile photographs at the start of distraction (e, f) frontal and profile photographs at end of treatment. (g–i) Pretreatment photographs Intraoral photographs. (j–l) Post Distraction photograph. (m–o) End of treatment
Eighteen adult patients, eight men and ten women, who underwent maxillary advancement by distraction osteogenesis using an external frame distractor were studied for a mean period of 3 years. All the patients were operated by a single surgeon. The mean age was 24.8 years, with ages ranging between 18 years and 34 years. Twelve patients had unilateral cleft lip and palate, and six patients had bilateral cleft lip and palate. The inclusion criteria were as follows: Patients who had maxillary malformation with skeletal Class III malocclusion with a negative overjet ranging from −6 to −15 mm and a cervical maturation indicator 6 or more (CVMI 6 completed).
31.2.3 Serial Cephalometric Evaluation
Lateral cephalograms were used to determine and follow the maxillary position of overtime, taken at intervals: (1) Before commencement of distraction (T1), (2) immediate postdistraction period (T2), (3) 1 year following completion of distraction (T3), and (4) 3 or more years after completion of distraction (T4). T1, T2, and T3 radiographs of a bilateral cleft lip and palate patient treated with rigid external distraction are illustrated in Fig. 31.3a–c.
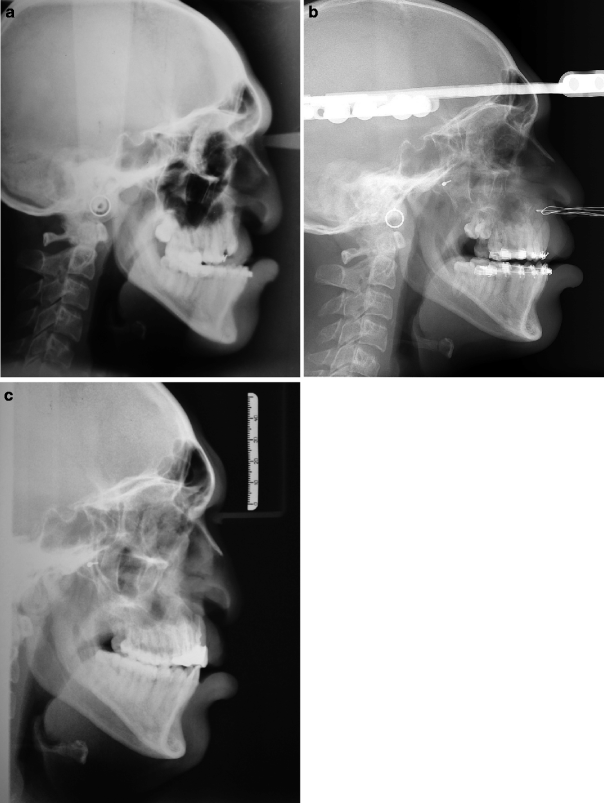

Fig. 31.3
(a–c) Lateral cephalograms at different intervals as follows. (a) Before commencement of distraction, (b) immediate post distraction period, and (c) three year following completion of distraction
The radiographs were traced and evaluated by a single experienced investigator. An X–Y coordinate system was made by drawing a line at an angle of 7° below SN plane for x-axis. Y-axis was drawn perpendicular to this and intersecting it at the sella (Fig. 31.4). The changes in position of ANS, point A, mandibular incisor, and pogonion (Pog) were measured in the x– and y-axis in cephalograms T1–T4 serially. A mean value was arrived at from all individual measurements, and paired sample t test was used to compare the difference between T1–T2, T2–T3, and T3–T4.
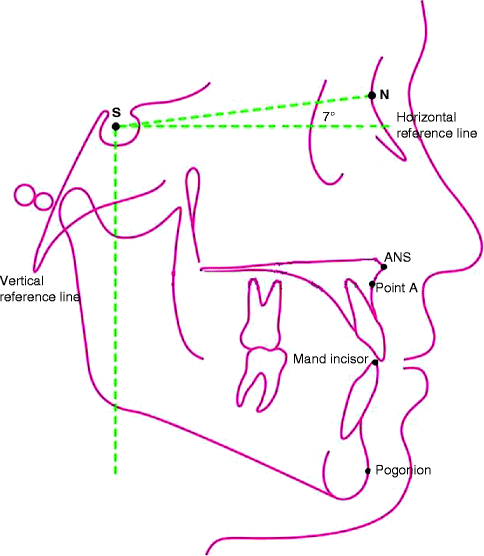

Fig. 31.4
X–Y coordinate system was used. The changes in position of ANS, Point A, Mandibular incisor, Pogonion (Pog) were measured on the X and Y axis
31.3 Results
Immediately following distraction (T1–T2), the maxilla moved forward at the ANS by 12.4 mm and also downward by 1.56 mm. In the first year following distraction (T2–T3), the maxilla moved backward by 1.5 mm, suggesting significant relapse. Between 1 and 3 (or more) years (T3–T4), maxilla remained stable in horizontal and vertical position. Similar changes with insignificant differences in values were seen in the positions of point A over the same time frame. The position of the tip of mandibular incisor showed significant downward movement of the mandibular incisors immediately after distraction; however, after 1 year following distraction, it moved forward. Similarly, pogonion (Pog) changed as follows: Between T1 and T2, there is backward and downward movement, and between T3 and T4, it remained stable in its new position. Comparison of maxillary positions between bilateral and unilateral cleft lip and palate that was done using the unpaired t tests showed no significant difference between these groups (Fig. 31.5). Comparison between patients who wore a retention device for a year as suggested by the protocol and those who did not wear it or partially complied with the instructions showed that the former group had better retention (Fig. 31.6
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


