and Silvio Mazziotti1
(1)
Department of Radiological Sciences, University of Messina, Messina, Italy
Abstract
In this chapter the main iconographic patterns are illustrated related to the main different odontoiatric treatments as well as precising their issues and related terminology.
General Considerations
There is no doubt that OPT is not the methodology of choice for the evaluation and checking of odontoiatric therapy results.
Indeed, this function is generally performed during the treatment through endoral radiograms and in case of sequela and/or major complications, through computed tomography.
However, it is true that the radiologist, while analysing an OPT radiogram, often has to face different treatment results and can have difficulty in making the report, especially if a precise query and/or a clinical recall are absent.
It must be said that the evaluation, based only on radiological findings, turns out to be very limited and sometimes misleading, if considered separately from the clinical context.
The aim of this chapter is to illustrate the main iconographic patterns related to the results of the different odontoiatric treatments as well as precising their issues and related terminology.
Radiological aspects related to extractive therapy and conservative endodontic treatments along with some of the issues related to implantology will be discussed.
Radiological Findings of the Extractive Treatments
Radiological findings related to the results of a previous dental avulsion mainly refer to the morphological analysis of the so-called extraction site.
It seems to be evident that radiological evaluation must always be supported by a minimum of clinical integration because the exclusive morphological interpretation can be misleading.
Propaedeutical to the evaluation of the pathological extractive site is the knowledge of its normal morphology and its modifications occurring over time. The latter parameter is subjected to significant and very heterogeneous individual variations.
The main characteristic of a recent extraction site, in absence of pathological conditions, is the clear observation of all the anatomical components of the empty alveolus, which can be detectable for a variable time (30–40 days) from one subject to another.
Successively, the empty alveolus starts losing the sharpness of its outlines and assumes a blurred aspect. This is due to the proliferation and organisation of the granulation tissue, followed by mineralisation phenomena, which will lead in about 6–8 months to the complete bone obliteration of the alveolar cavity (Fig. 8.1a–c).
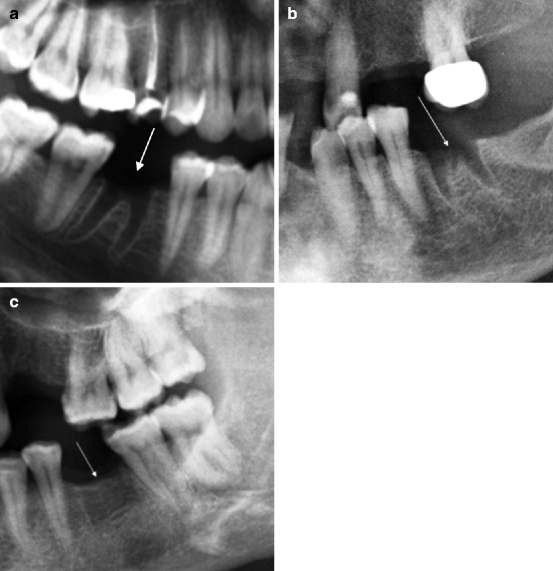

Fig. 8.1
Normal extraction sites (indicated by arrows). (a) Extraction site after 3 days. (b) Extraction site after 1 month. (c) Extraction site after 1 year. In (a, b) all the alveolar components are evident. In (b) the outlines start to lose their sharpness. In (c) the bone obliteration of the alveolar cavity is almost complete
In some cases the blood clot, which is normally expected to occupy the extraction site, can be lost and the healing process interrupted or delayed.
The blood clot is, in fact, an important factor for the protection of the alveolar bone, and its loss can determine a painful complication called alveolar osteitis or dry socket.
In its early stage, obviously, such complication cannot be demonstrated through OPT.
The persistence of such pathological condition, generally linked to infection, determines the subacute and chronic post–extractive alveolitis.
As consequence the site can assume altered connotations which modify its characteristics. The main pathological modification comprises the reduction in sharpness of the alveolar cavity’s outlines.
This finding (typical also of the site’s normal evolution) has pathological meaning only if associated to the loss of the normal alveolar morphology.
Another significant element is represented by the diffuse osteosclerosis of the perialveolar cancellous bone, indicative of sclerosing alveolitis or sclerosing osteitis (Figs. 8.2a–c and 8.3).
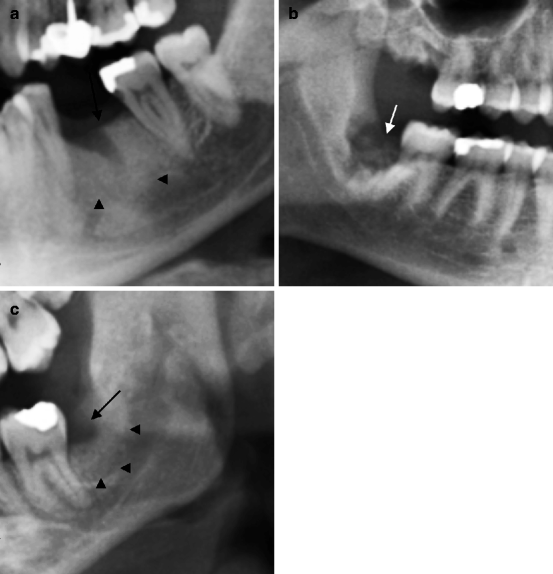
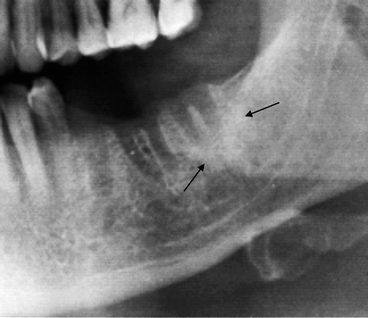

Fig. 8.2
Three situations of post-extraction alveolitis. In (a) alveolar morphology is maintained (indicated by arrow), and sclerosis of the spongiosa due to sclerosing osteitis is observable (arrowheads). In (b) alveolar morphology is altered (indicated by arrow). In (c) alveolar morphology is totally modified. A focal osteolysis is observable (indicated by arrow). This is due to the abscessual collection surrounded by bony sclerosis (indicated by arrowheads)

Fig. 8.3
The image shows three extraction sites in different evolution. The site in position 3.5 is the oldest and appears to be approaching bone obliteration. Site 3.6 is the most recent and appears to be normal. Site 3.7 presents blurred outlines and is surrounded by sclerosis ring (indicated by arrows). Both signs are indicative of post-extractive osteitis
Other factors concerning the radiological evaluation of an extraction site are related to a possible detection of residual tooth fragments or of fracture lesions of the alveolar walls.
Residual tooth fragments are found, most of the time, through endoral examinations during an extraction procedure, when the dentist suspects their presence. However, such a finding can occasionally be detected during OPT. In such cases, the clinical-anamnestic evaluation of the patient is obviously crucial for a correct interpretation of this radiological finding, which can often have little pathological significance (Fig. 8.4a, b).
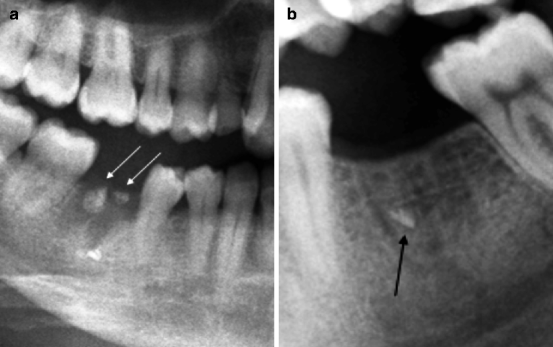

Fig. 8.4
(a) Dental fragments (indicated by arrows) in a recent extraction site. (b) Dental fragment (indicated by arrow) in an extraction site approaching bone obliteration. The finding does not have pathological significance
Alveolar fractures are a consequence of extraction manoeuvres. When these lesions occur in the alveolar walls, on the vestibular or lingual-palatal sides, they cannot be detected by OPT for well-known projective reasons.
Conversely, it will be possible to give evidence of the possible lesions affecting the interradicular crest, whose fragment can sometimes contribute to phenomena of post-extractive alveolitis. The fragment can assume the aspect of a small osteosclerotic sequestration inside the alveolus (Fig. 8.5a, b).
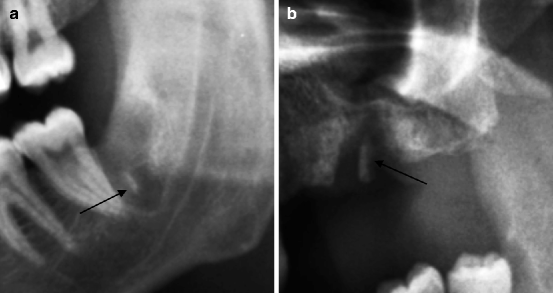

Fig. 8.5
In (a) a thin fractured fragment of the interradicular crest occurs (indicated by arrow). In (b) signs of chronic post-extraction alveolysis are present. The bony fragment (indicated by arrow) is sclerotic
Moreover, the radiological analysis of the extraction site must consider possible damages in the mandibular canal, or in the floor of the maxillary sinus, with the consequent formation of oroantral fistula (Figs. 8.6a, b and 8.7).
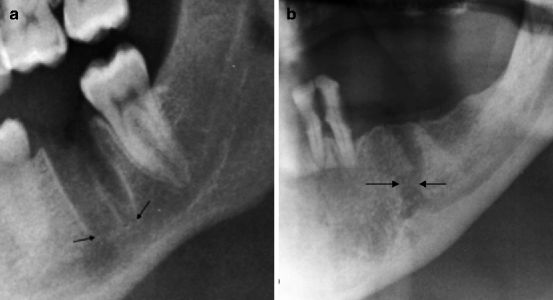
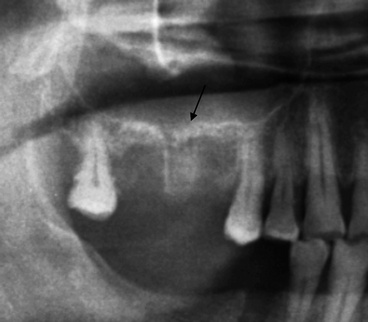

Fig. 8.6
In (a) disappearance of the cortical of the apical region (indicated by arrows). Hypotheses about the damage to the mandibular canal can be made. In (b) fistulous communication (indicated by arrows) between extraction site and mandibular canal is present

Fig. 8.7
Extraction site (indicated by arrow) communicating with the maxillary sinus
One must consider that during its evolution, the extraction site may not have its normal bone obliteration. This is most likely to happen for reasons related to chronic inflammatory phenomena, which are often oligosymptomatic.
In this eventuality, the extraction site will develop into an irreversible residual cavity, characterised by little clinical relevance.
In order to prevent this unfavourable situation, some dentists accumulate radiopaque and resorbable material in the post-extraction cavity (Fig. 8.8a, b).
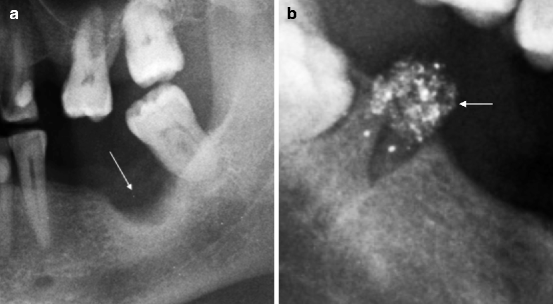

Fig. 8.8
(a) Extraction site evolved in residual cavity (indicated by arrow). (b) Extraction site with resorbable radiopaque material (indicated by arrow)
Finally, the possibility for the extraction site to be in continuity with the small residual cavity due to the apical granuloma must be taken in account (Fig. 8.9).
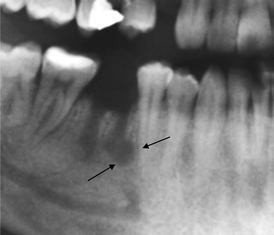

Fig. 8.9
Extraction site communicating with the cavity due to apical granuloma of the mesial root (indicated by arrows)
Effects of the Endodontic Therapy
This conservative therapy, aiming at saving the dental element, is fundamentally based on the techniques of endodontic treatment which consider penetrating caries, with infection of the dental pulp (pulpitis), to be the main indication.
The treatment consists of eliminating the carious lesion as well as the removal of the altered pulp from the pulp chamber and canals (devitalisation), followed by obliteration of pulp chamber and canals, through radiopaque resin-based material (gutta–percha), in order to seal the aforementioned cavities. This last procedure avoids persistence and/or diffusion of the infection (canalar therapy).
It is clear that all the aforesaid procedure can be evaluated by the dentist while operating, through the use of endoral radiograms.
In the evaluation of a panoramic radiogram, the morphological results of these procedures are often evident. Moreover, their analysis cannot be prescinded from a clinical-anamnestic evaluation.
Indeed, also in the presence of extremely insufficient results on the morphological aspect, it is not rare to notice clinical conditions which are totally normal and vice versa.
The main problems that must be considered in the presence of the canalar therapy results are irregular and incomplete canal filling, endocanalar overfilling and false routes.
The aforementioned evaluations obviously presume familiarity with a perfect realised treatment. In particular the filling must reproduce the morphology of the pulp chamber and of one or more canals (endodontic cone) in complete manner, without any irregularities or discontinuities (Fig. 8.10a–c).
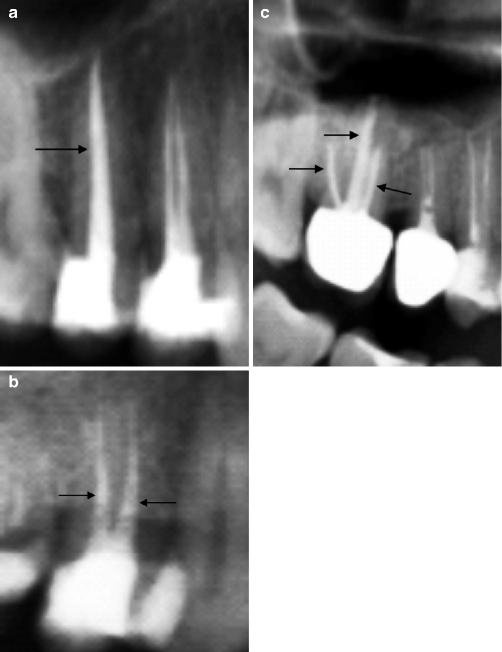

Fig. 8.10
Normal endodontic cones (indicated by arrows) in monoradicular tooth (a), biradicular tooth (b) and triradicular tooth (c)
Irregular and Incomplete Canal Filling
The finding of irregular, discontinuous and incomplete canal filling seems to contradict the rationale on which endodontic treatment is based.
Indeed, segments of the pulp-canal cavity which have not been obliterated by the radiopaque material cause a risk of microbial persistence and proliferation in this area.
However, it must be said that in presence of these morphological pictures, the radiological evaluation must be subordinated to the clinical one.
The existence of a periapical lesion indicates the inadequacy of this treatment (Fig. 8.11a–c).
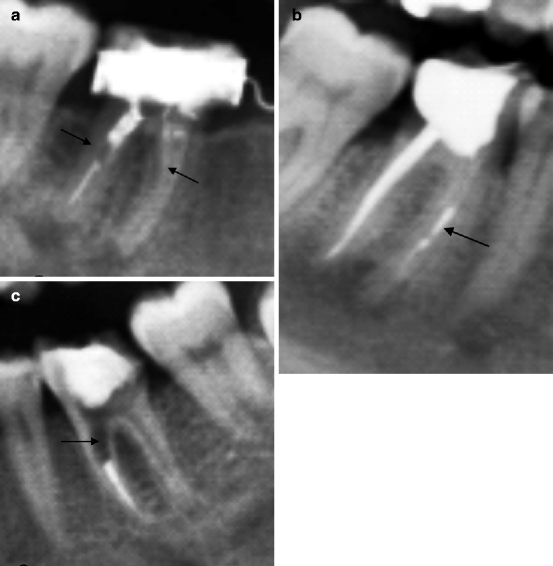

Fig. 8.11
Three examples of incomplete and irregular canal filling. In (a, b) periapical lesions are also present. In (c) widening of the radicular canal (indicated by arrow) due to endodontic damage is observable
Sometimes, periapical lesions can be detectable even in the presence of endodontic treatments which are morphologically impeccable (Fig. 8.12).
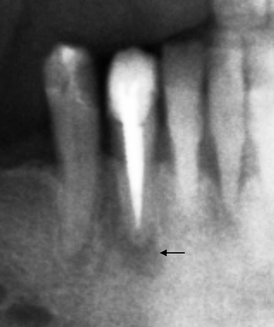

Fig. 8.12
Periapical lesion (indicated by arrow) in a tooth with endodontic cone which is absolutely normal. Only clinical examination and its evolution are able to define the significance of the radiographic image
In this case, they can be considered either a vestigial remain of a periapical lesion now eradicated and destined to bone obliteration or a conspicuous inflammatory lesion in evolution.
Apart from the clinical evaluation, the only criterion (although quite unpredictable) able to distinguish between two hypothesis is its evolution by the time.
As a matter of fact, vestigial lesions tend to disappear within the space of 3–4 years.
Similar considerations are related to the results of the surgical treatment through apicectomy.
Indeed, this therapeutic method entails the resection of the root tip of the tooth (previous microsurgical transgingival approach) and of the periapical lesion. This has to be obviously preceded by the endodontic treatment of the pulp chamber and the radicular canal.
In these cases, as remains of the surgical treatment, a lytic lesion adjacent to the resected apex can be detected. Such lesion, if therapeutic success occurs, will be obliterated as time goes by (Fig. 8.13).
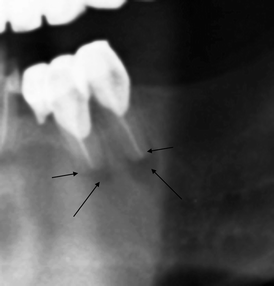

Fig. 8.13
Results of apicectomy (indicated by short arrows) with the presence of periapical residual demineralisation (indicated by long arrows)
The restoration of the crown completes the endodontic treatment.
This procedure can be realised with different techniques which see the employment of materials characterised by variable (from modest to marked) opacity.
The use of materials characterised by modest opacity or one which is otherwise inferior to that of the normal elements’ crown must not generate the erroneous interpretation of carious lesion (Fig. 8.14).
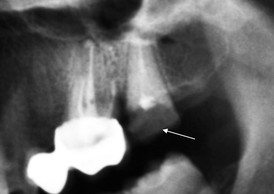

Fig. 8.14
Canalar therapy and coronal restoration with low-opacity material (indicated by arrow). This finding must not be confused with a carious lesion of the crown
The crown restoration device often becomes integral with the radicular complex through the insertion of a metallic post (endodontic post) (Fig. 8.15a, b).
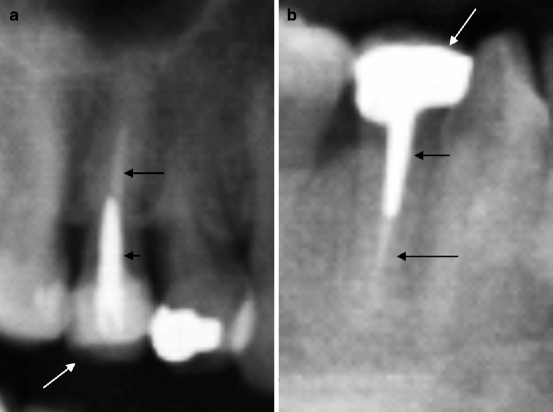

Fig. 8.15
Coronal restoration through endodontic post (indicated by short arrows) and canal obliteration (indicated by long arrows). In (a) the crown has been restored with less radiopaque material than in (b) (indicated by white arrows)
The endodontic post can also be associated to alterations of the adjacent dental tissue through resorption phenomena. On the clinical point of view, this event can be similar to those caused by situations related to insufficient or incomplete canal filling and, in addition, to more or less significant dental instability (Fig. 8.16
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


