and Silvio Mazziotti1
(1)
Department of Radiological Sciences, University of Messina, Messina, Italy
Abstract
Maxillary cystic lesions can be distinguished as odontogenic or non-odontogenic. Radicular cysts are the only acquired odontogenic cysts which are mainly caused by a preexisting apical granuloma. Non-odontogenic cysts always have a dysontogenetic origin. Odontogenic tumours are generally constituted by benign or mildly aggressive entities, even if they often tend towards local relapse. These neoformations are presented together with the cystic lesions, as the odontogenic tumours show considerable overlaps with the more common cystic formations, both on clinical and radiological levels.
General Considerations on Cystic Lesions
Maxillary cystic lesions can be distinguished as having either odontogenic or non-odontogenic origin.
All odontogenic cystic lesions, except radicular cysts, present a dysontogenetic genesis which is variably linked to developmental errors of the dental germ and/or the organ of the enamel.
Radicular cysts are the only acquired odontogenic cysts which are mainly caused by a pre-existing inflammatory lesion (apical granuloma).
However, it must be said that flogistic phenomena do not exclusively pertain to radicular cysts, as the dysontogenetic cysts can also be complicated by possible inflammatory phenomena.
Non-odontogenic cysts always have a dysontogenetic origin, linked to the cystic degeneration of the epithelial residuals which, during the embrionary development, remained inclusive in specific areas of the maxillaries (fissural cysts).
Before treating the single pathological entities, it is appropriate to consider the so-called lacunar images of the mandible, which are included, often erroneously, in the category of cystic lesions.
Lacunar Images of the Mandible
This chapter includes lacunar images which are localised and clearly marked off by the surrounding bone and by a thin sclerotic rim, which can often be detected in the inferior maxillary.
Such a finding has been, for a long time, erroneously called ‘Stafne’s cysts’.
There is no doubt that the term ‘cyst’ is completely erroneous and used improperly as the genesis of such an image is not supported by fluid content, but rather by the intraosseous intrusion of a modest amount of tissue deriving from the parenchyma of the submandibular gland.
This genesis explains the characteristic seat of the radiological image (mandibular angle region, beneath the mandibular canal) (Fig. 7.1a, b).
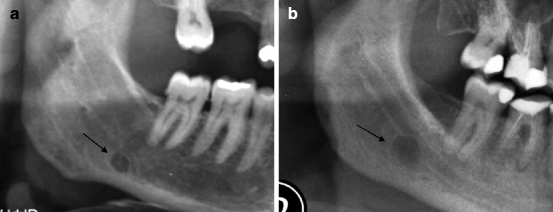

Fig. 7.1
(a, b) Two cases of Stafne’s lacuna (indicated by arrows)
On the basis of what is aforementioned, it is clear that Stafne’s lacuna is the most appropriate term to indicate such an image (moreover, without pathological meaning).
Radicular Cysts
Radicular cysts are the only odontogenic cysts with a primitive inflammatory origin.
Indeed, they are always supported by the presence of chronic flogistic phenomena localised in the periapical area or more rarely in the periradicular region.
In particular, it is believed that radicular cyst (apical or pararadicular) represents the cystic evolution of the epithelial remains (Malassez’ residuals), which are included in the untreated apical (or pararadicular) granuloma.
For this reason, it must be remembered (as explained in the Chap. 5) that radiological differentiation between a big apical granuloma and a small cyst is based only on dimensional criteria, where the diameter of about 10–12 mm represents the limit between the two entities.
Radicular cysts are constituted by a cavity with slow growth, lined by an epithelial membrane and are characterised by a fluid content which tends to increase progressively. This is a consequence of the continuous osmotic uptake in the cavity.
The lesion is firstly asymptomatic, but in its growth, tumefactions in vestibular or lingual seat begin to appear.
Radicular or Periapical Cyst
In its periapical variety, the radicular cyst represents the most frequent cystic lesion.
It more frequently involves the anterior-lateral teeth of the superior maxillary and the posterior ones of the inferior maxillary.
It always shows itself on the apex of the pathological dental element, or in the seat of previous endodontic treatment (Fig. 7.2a–c).
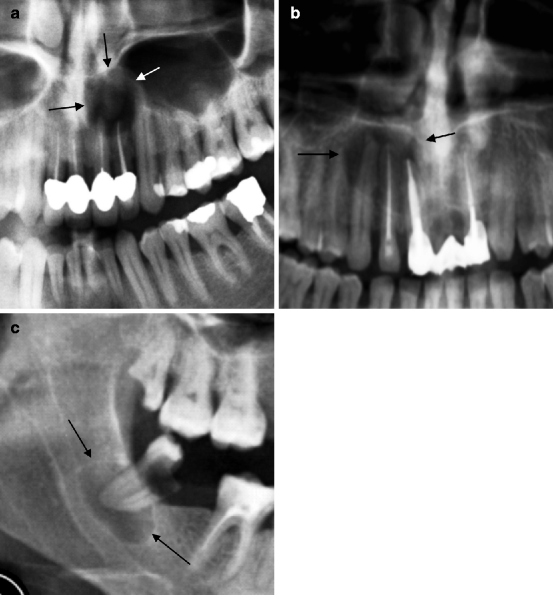

Fig. 7.2
(a, b) Radicular cysts (indicated by arrows) centred in the apical region of devitalised elements. (c) Radicular cyst (indicated by arrows) centred in the apex of an element with penetrating caries
Cystic localisations in the dental elements of the superior arch can be problematic because of such a particular seat of origin. A primary consideration which must be highlighted is the very close proximity of the cystic lesions to the maxillary sinuses.
This anatomical proximity can cause diagnostic errors (both positive and negative) which are linked to the difficulty of detecting the cyst, which can be confused with abnormal expansions of the sinus cavity (Fig. 7.3a, b and 7.4).
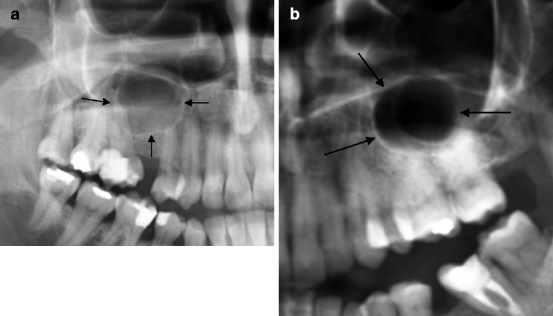
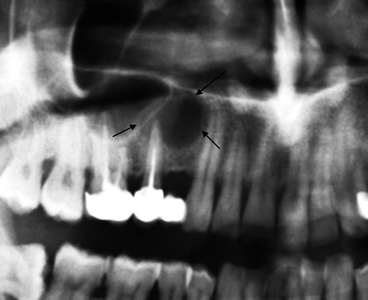

Fig. 7.3
(a, b) Two cases of abnormal expansion of the maxillary sinus (indicated by arrows) which can be confused with the presence of radicular cysts

Fig. 7.4
Radicular cysts (indicated by arrows) centred in the apex of 1.5, which can be confused with the abnormal expansion of the maxillary sinus
Another characteristic problem of the localised cysts in the superior arch is related to their possible endosinusal development.
Indeed, the growth of the cyst inside the maxillary sinus, above all if associated with calcification phenomena, can give rise to bizarre features of difficult interpretation (Fig. 7.5).
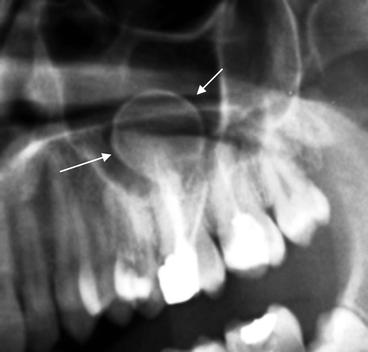

Fig. 7.5
Calcified radicular cyst with intrasinusal development (indicated by arrows)
In the inferior maxillary the most significant problem related to the volumetric increase of the cystic lesion is represented by the existing relations between the latter and the mandibular canal.
Indeed, this proximity entails the risk of iatrogenic lesions in the inferior alveolar nerve during surgical manoeuvres aiming at treating the lesion.
In such a situation CT examination is obviously the method of choice as OPT is not sufficient to clarify in detail the existing relations between these structures.
Residual Radicular Cysts
This term indicates all the cyst cavities remaining after the tooth extraction.
In such cases the cavity can be totally asymptomatic or can continue in its growth, causing damages to the adjacent structures.
In the field of such lesion typology, it is possible to detect an extreme dimensional variability of the residual cavities which can vary from lesions of small dimension to substantially sized cysts (Figs. 7.6 and 7.7).
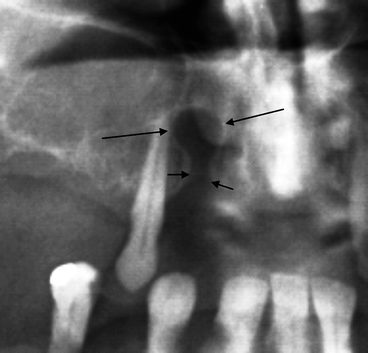
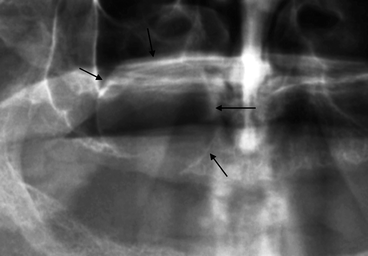

Fig. 7.6
Residual radicular cyst (indicated by long arrows). The short arrows indicate the empty dental alveolus

Fig. 7.7
Conspicuous residual cyst (indicated by arrows) developing in the maxillary sinus
The diagnosis of a residual cyst, especially if it has huge dimensions, can be difficult and is exclusively based (apart from the anamnestic finding) on the radiological detection of the remains of the empty alveolus (Fig. 7.8).
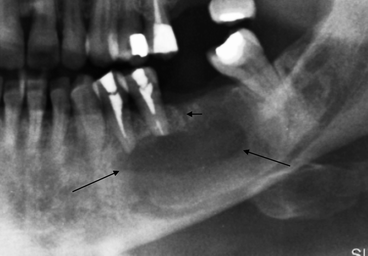

Fig. 7.8
Extended cystic lesion (indicated by arrows) which causes apicolysis of two elements. The residual nature of the lesion is shown by the detection of a subtle path (indicated by short arrow) which corresponds to the empty alveolus
Lateral Radicular Cysts
The lateral radicular cyst or periradicular cyst rarely occurs, and it stems from the cystic evolution of a periradicular granuloma, a pathological entity already discussed in Chap. 5.
It is easily diagnosticable when still characterised by modest volume (Fig. 7.9).
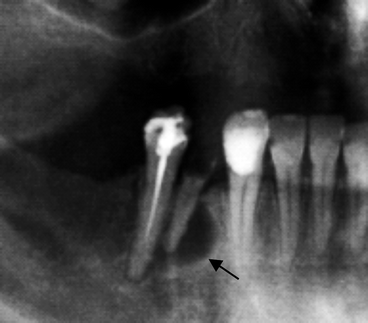

Fig. 7.9
Small radicular lateral cyst (indicated by arrow)
Conversely, in the presence of more extensive lesions affecting the adjacent dental elements, the diagnosis can be more difficult to make (Fig. 7.10).
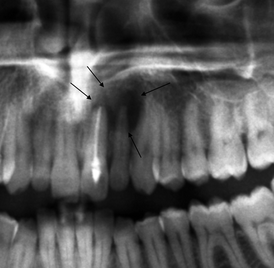

Fig. 7.10
Radicular lateral cyst of 2.1 (indicated by arrows) which, in its development overlaps 2.2, simulating its origin in this last element, which moreover, does not have any pathology
Follicular or Dentigerous Cysts
The follicular cyst, also known as a dentigerous cyst, represents a classic type of odontogenic cyst on a non-inflammatory base.
Indeed, it is the expression of the cystic degeneration of the enamel organ and in particular of the stellate reticulum tissue (see Chap. 2) in an inclusive element.
The missing eruption, the seat of the dental element and variable alterations of its orientation therefore represent favourable circumstances for the development of a follicular cyst.
From the morphological point of view, the most characteristic element of such lesion is represented by the protrusion of the crown (more or less pronounced) inside the cystic cavity. Conversely, the radicular axis generally turns out to be on its exterior.
The third molars, followed by the canines (most likely for their major tendency to inclusion), are the most affected teeth.
Radiologically the follicular cyst presents an extreme variability, and its innumerable variations can be noticed both in terms of localisation and dimension.
With respect to this, it must be said that the lesions characterised by modest size (which represent the majority of the radiological findings) are generally asymptomatic and are detected only occasionally (Figs. 7.11a–c and 7.12a, b).
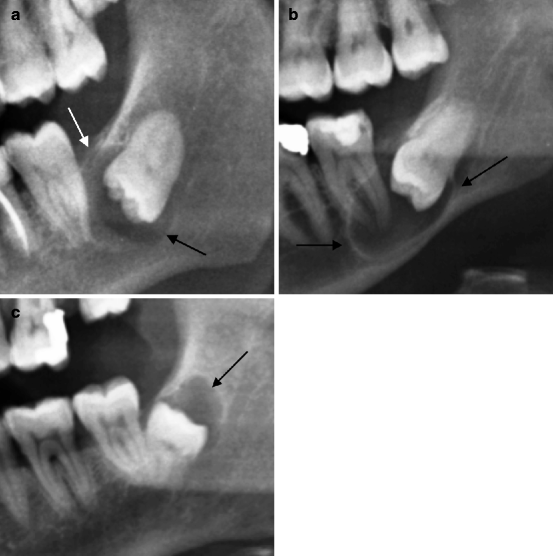
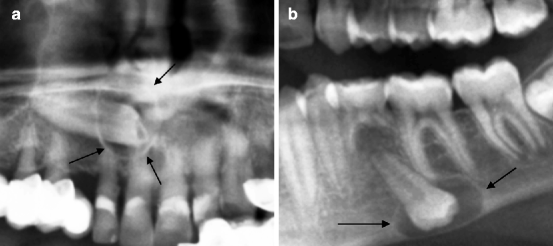

Fig. 7.11
(a–c) Three examples of small follicular cysts (indicated by arrows) of occasional finding

Fig. 7.12
(a) 1.3 is inclusive in mesiodistal angulation with a small follicular cyst (indicated by arrows). (b) Inclusive tooth in inverted orientation with a follicular cyst (indicated by arrows) which causes the thinning of the mandibular cortical is 3.5. Persistence of 7.5
Conversely, the more extensive lesions can have a clinical evidence for three reasons: the presence of tumefaction and deformity of the skeletal host segment, its relations to the surrounding critical structures (paranasal sinuses and mandibular canal) and, finally, the damages occurring in the adjacent normal dental elements (Fig. 7.13a, b).
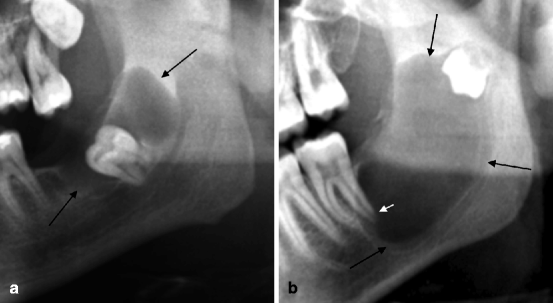

Fig. 7.13
(a, b) Conspicuous follicular cysts (indicated by long arrows). Both lesions present an extended surface of contact with the mandibular canal. Cyst in (b) also causes apicolysis of 3.7 (indicated by the short arrow)
The Eruption Cyst
It is a variant of the follicular cyst characterised by the presence of pericoronal cystic degeneration in an element which is totally or partially inclusive but whose orientation (normal or only slightly alterated) presupposes its eruption.
In these cases, if the eruptive push prevails on the resistance exerted by the cystic cavity, eruption occurs.
The eruption cyst clinically appears as a bluish swelling covered by the gingival mucosa, whose laceration reveals the tooth in eruptive phase (Fig. 7.14a, b).
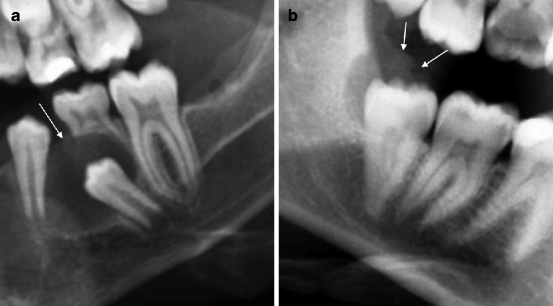

Fig. 7.14
(a, b) Two examples of eruption cysts. The arrows indicate the surface of the lesions appearing in the gum
Primordial Cyst and Odontogenic Keratocyst
For their similarity these two entities are considered to be variants of the same pathological phenomenon.
Moreover, both lesions have odontogenic origin.
Primordial cyst is the expression of the cystic degeneration of a dental germ, before the latter becomes mineralised.
The dental germ which is affected corresponds a normal or a supernumerary element.
Obviously, in the first case, the absence of a dental element (generally one of the molars) will correspond to the cystic lesion.
Conversely, in the second eventuality the lesion will coexist with all the elements of the permanent dentition.
Odontogenic keratocyst is related to the cystic degeneration of a portion of the dental lamina, in a greater or lesser extent.
Therefore, from the embryologic point of view, it is an older lesion than the primordial cyst. As a matter of fact, some authors categorise it in the field of hamartomas.
The distinctive structural feature of this lesion involves the presence of a keratinised epithelial lining.
Similarly to the primordial cyst, it can develop when the elements of the permanent dentition are normally represented or when absence of a permanent dental element occurs.
Both lesions typically occur in the mandibular angular region and are obviously mutually not distinguishable.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


