Fig. 20.1
(a–e) Patient with a complete unilateral cleft lip and palate at birth (a), after presurgical orthopedic treatment according to the Zurich approach (b), after lip closure (c), frontal view at the age of 15.8 years (d), and palatal view at 15.8 years after secondary bone grafting and orthodontic treatment (e)
According to the scientific use at that time, conclusions regarding the effects of treatment were mainly based on observations: orthopedic guidance together with optimal timing of surgery has beneficial effects. Later evaluations claimed better results with two-stage palatal closure on speech; whether or not the presurgical treatment had an influence could not be demonstrated (Hotz and Gnoinski 1976, 1979; Gnoinski 1982; Van Demark et al. 1989). In 2009, longitudinal cephalometric results were published of a sample of 29 patients with BCLP from 5 years to the end of the growth period (Gnoinski and Rutz 2009). All 29 patients had been treated in Zürich according to the same protocol, operated on by the same surgeon and treated by the same orthodontist. The authors conclude that the multidisciplinary concept of maintaining the initially protrusive position of the premaxilla by means of a passive plate at the newborn and infant stage, as well as using surgical procedures with limited retrusive effect, proved to be correct in the long run: at the young adult stage, the ANB angle remained positive for almost all patients except for those with multiple-tooth agenesis in the upper arch.
We can conclude that the treatment principles of Dr. Hotz and Dr. Gnoinski have had a tremendous impact on cleft palate treatment, especially in Europe. Unfortunately, in the last two decades, not much has been published about the results of the Zürich approach, and the earlier papers have no strict research design that allows us to draw evidence-based conclusions about the effectiveness of neonatal orthopedics. It might very well be possible that the surgical timing and sequencing are the decisive factors in the final treatment result.
20.4.4 Nasoalveolar Molding Grayson
After nearly 40 years of neonatal maxillary orthopedics, the treatment started to drift away from its traditional aims and techniques with the publications from the cleft palate team at New York University Medical Center in the 1990s (Grayson et al. 1993; Cutting et al. 1998). To theirs and many others’ experience, it is very difficult to reach a good result in the neonatal treatment of cleft lip and palate due to the actual anatomical deformity of the nose, which includes abnormal nasal cartilage morphology, deviated nasal septum and columella, asymmetry of the alar base, and a short or even absent columella, depending on the type of cleft. In addition, fibers of the orbicularis oris muscle run superiorly along the margins of the cleft towards the nasal tip, while in bilateral clefts, muscle tissue is often lacking in the prolabium, which is seated directly at the short columella. Therefore, Grayson and Cutting (2001), who have used the Latham-Millard (POPLA) procedure for 15 years but did not note why it was abandoned, emphasize the importance of presurgical correction of the nasal cartilage and soft tissue deformity, which can be achieved by a combination of nasal and alveolar orthopedic molding. This therapy, now called NAM (nasoalveolar molding) or PNAM (presurgical nasoalveolar molding), makes a distinct difference with the other types of infant orthopedics, as described previously (Grayson et al. 1993; Cutting et al. 1998; Grayson and Cutting 2001; Barillas et al. 2009). In NAM, nasal stents are added to the alveolar molding plate. The molding plate itself is mainly used to approximate the alveolar segments and retract the protruding premaxilla in CBCLP in order to reduce the nasal deformity to a degree that enables the start of more precise nasal molding with stents (Grayson and Maull 2006; Santiago and Grayson 2009). Retention of the appliance in the mouth is secured by tapes on the cheeks, which engage the intraoral plate with orthodontic rubber bands. The appliance aims to improve nasal tip projection, and septal and lower lateral cartilage position, before cleft repair. In bilateral cleft lip and palate, the nasal stents are projected to gradually lengthen the deficient columella. A longitudinal study in BCLP patients on nasal morphology after NAM and primary alveolar surgical repair (gingivoperiosteoplasty) showed that near normal nasoalveolar morphology was reached until 12.5 years of age compared to reference values from the literature (Garfinkle et al. 2011). However, this paper does not discuss the effects on the facial profile and anterior occlusion.
The use of NAM is controversial because of reported midfacial recessiveness by other NAM users and polarizing professionals in the field of cleft lip and palate as happened before concerning the use of regular infant orthopedics. The claimed benefits of the procedure are (a) improved long-term nasal esthetics, (b) a reduced number of nasal surgical procedures, (c) a reduced need for secondary bone grafts if gingivoperiosteoplasty (GPP) is applied, (d) no larger growth disturbance than is found for other well-established procedures, and (e) savings in cost. In a series of papers that are discussed in their 2001 paper, the New York group attempted to substantiate these claims (Grayson and Cutting 2001). On the other hand, Berkowitz (2009) argues that NAM + GPP compromises future facial growth. This was confirmed in a retrospective study showing that midfacial growth was affected more negatively in a group with NAM + GPP than in a NAM non-GPP group measured at the age of 5 (Hsieh et al. 2010). Whether there was a negative effect by NAM alone could not be ruled out. Opponents also suggest that NAM places an extra burden on the family that already must adapt to having a newborn with a cleft (Sischo et al. 2012).
However, as for all other types of neonatal maxillary orthopedics, the research design for studies into the effect of NAM was not adequate to show scientific evidence for these claims so far. In line with the DUTCHCLEFT trial as described below, a two-group randomized controlled clinical trial would be the preferred design to investigate the effect of NAM before deciding whether to accept or abandon this therapy. Santiago and Grayson (2009) recognize this as they state that “Although these benefits have been demonstrated in multiple clinical publications there is no doubt that a need for long-term and perhaps federally supported clinical trials exists.” Nevertheless, in the USA, NAM is now employed in 37 % of 117 teams that have a case load of more than 25 patients annually (Sischo et al. 2012).
20.5 The DUTCHCLEFT Study
20.5.1 Background
As noted above, neonatal maxillary orthopedics was developed and introduced on theoretical grounds, and it became part of the treatment protocol in many centers although the actual effectiveness had never been tested nor were the possible adverse effects properly looked into. In Nijmegen, we have performed neonatal infant orthopedics according to the Zürich approach for over 20 years, but our clinical experience has convinced us that in unilateral cleft lip and palate patients, neonatal orthopedics is at best not necessary and at its worst could have negative side effects, even if considering only the cost-effectiveness. Gradually, we reached equipoise regarding whether or not to perform neonatal infant orthopedics. Being strong supporters of evidence-based care in general, and for cleft lip and palate patients in particular, a randomized controlled clinical trial was a next logical and inevitable step to try to solve the controversy regarding neonatal orthopedics.
After obtaining funding for a first period of 3 years, a prospective randomized clinical trial to investigate the effect of neonatal maxillary orthopedics in children with a complete UCLP, named “DUTCHCLEFT,” was begun in 1993 in three academic Cleft Palate Centers in the Netherlands: the Cleft Palate Centers of Radboud University Nijmegen Medical Center, Free University Medical Centre Amsterdam, and Erasmus Medical Centre in Rotterdam.
The following outcome variables were studied:
(A)
General effects: influence on feeding, body length and weight gain, parents’ satisfaction
(B)
Surgical and orthodontic effects: duration of lip surgery, esthetic outcome, maxillary arch form and dimensions, maxillofacial growth
(C)
Speech and language development: prelingual sound production, early speech and language development, intelligibility
(D)
Cost-effectiveness: medical and nonmedical costs
Results for feeding, general body growth, maxillary arch dimensions, facial growth, nasolabial appearance, speech and language development, and cost-effectiveness have been published in a series of papers between 1998 and 2009 and will be discussed below.
20.5.2 Experimental Design
The study was set up as a prospective two-arm randomized controlled clinical trial in three academic cleft palate centers in the Netherlands. The Institutional Review Boards of the three hospitals approved the study protocol. An extensive description of the design of the study is given by Prahl et al. (2001).
The intake started in January 1993 and ended in June 1996. In total, 54 babies (41 boys, 13 girls) entered the trial, 27 in each group. The patient inclusion criteria were complete UCLP, infants born at term, both parents Caucasian and, because of the speech assessments, fluent in the Dutch language, and trial entrance within 2 weeks after birth. The exclusion criteria were other congenital malformations (except for syndactyly) and soft tissue bands. The parents of eligible infants were informed about the trial, and written informed consent was obtained from all participants. A computerized balanced allocation method was used in order to reduce imbalance on relevant prognostic factors between the two groups. Patients were allocated based on birth weight (<3,300 or >3,300 g) and alveolar cleft width (<8 mm, between 8 and 12 mm, or >12 mm). Treatment allocation was concealed. A computer program assigned the infant to the group with infant orthopedics (= IO+) or without infant orthopedics (= IO−).
Lip surgery was performed at 18 weeks of age according to the Millard technique. The soft palate was closed at the age of 52 weeks according to a modified von Langenbeck procedure. Neonatal maxillary orthopedics was performed by means of passive plates, starting within 2 weeks after birth. The plate was fabricated on a plaster cast and consisted of compound soft and hard acrylic. The plate, with a small extension into the cleft nose, covered the palate and the alveolar ridges and obtruded the cleft of the hard and soft palate. The plate was worn 24 h a day. IO+ children returned to the clinic every 3 weeks to have their plates adjusted by grinding at the cleft margins to ensure proper approximation of the maxillary segments. Maxillary growth indicated the necessity for a new plate. After surgical lip closure, the plate was relieved in the frontal area and reinserted the same day. Checkup visits were now planned every 4–6 weeks. The plate was worn until surgical closure of the soft palate. Children in the IO− group did not wear plates. They visited the clinic for an extra checkup at the age of 6 weeks as well as before and after lip repair and soft palate closure.
20.5.3 General Effects
Available information in the literature of the effects of IO on feeding and subsequently on general body growth seemed to be inadequate, and therefore, feeding variables and the anthropometric variables weight and length were measured in DUTCHCLEFT. The feeding variables were measured using questionnaires that were given to the parents when the child was 0–2 weeks of age and at 3, 6, 15, and 24 weeks of age. The questions concerned: amount of food, duration of the feeding, feeding frequency, feeding velocity (time measurement), feeding method, breast milk or formula, and feeding problems. We also used questionnaires to measure the mother’s satisfaction in motherhood (Prahl et al. 2008).
Mother’s satisfaction was comparable for both groups. Only slight feeding problems were experienced, but there were no significant differences between babies who wore a plate and babies without a plate. Feeding velocity increased with time from 2.9 to 13.2 ml/min in the IO− group and from 2.6 to 13.8 ml/min in the IO+ group; no significant differences were found between groups. Weight-for-age, length-for-age, and weight-for-length (z-scores) did not differ significantly between groups, but overall the UCLP infants in both groups had significantly lower mean z-scores for weight-for-age and height-for-age than the reference during the first 14 months of life and had lower mean values for weight-for-length after soft palate closure (Prahl et al. 2005).
The data show that neonatal orthopedics with the aim to improve feeding and the consequent nutritional status in infants with UCLP can be abandoned. In addition, parents’ satisfaction proved not to be an argument to perform neonatal orthopedics.
20.5.4 Surgical and Orthodontic Effects
The purpose of this part of the DUTCHCLEFT trial was to evaluate the effect of neonatal orthopedics on maxillary arch form and arch dimensions from birth on and occlusion of the deciduous dentition in UCLP children, to evaluate cephalometric facial growth, and to rate facial and nasolabial appearance.
Maxillary arch dimensions were evaluated by means of plaster casts of the upper jaw at the ages of 0, 15, 24, 48, and 58 weeks and 1–1/2, 4, and 6 years. The maxillary casts were analyzed three-dimensionally by means of the Reflex Microscope (Reflex Measurement Ltd., Somerset, UK). In addition, contact or collapse of the maxillary segments, at the age of 11/2 year, were scored. Figure 20.2a, b shows a series of models from the study. Cephalometric radiographs were analyzed at 4 and 6 years of age. Facial appearance on full face photographs and photographs showing only nose and mouth was rated at different time points until 6 years of age.
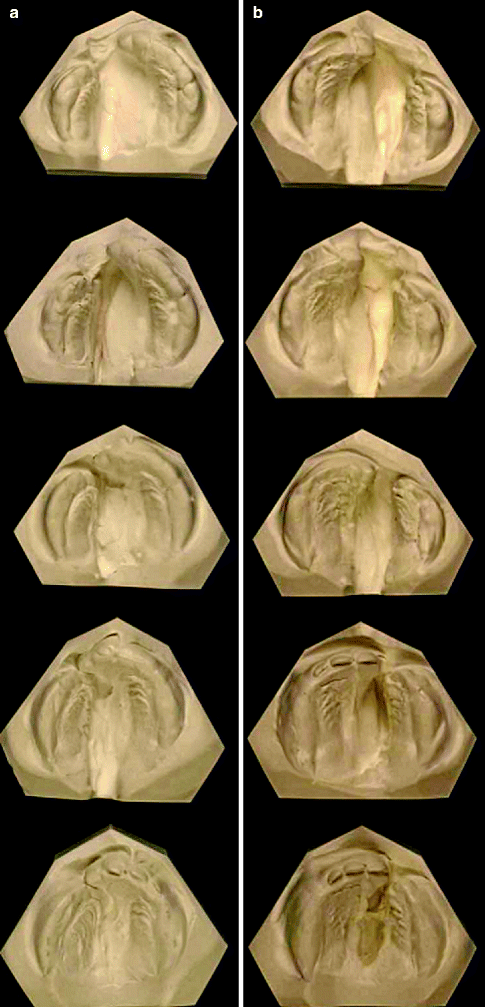

Fig. 20.2
(a, b) Series of study casts of two patients from the DUTCHCLEFT trial. The infant whose models are shown in (a) received no infant orthopedics; the infant whose models are shown in (b) received infant orthopedics. The five stages are (from upper to lower model) 0, 15, 24, 48, and 58 weeks of age
The results show that neonatal orthopedics does reduce the alveolar cleft width before lip surgery, which means that at the time of lip closure, the cleft width in children treated with plates was narrower than in the other group. However, after lip closure in both groups, the alveolar cleft width diminished further, and at the time of soft palate closure, the maxillary arch dimensions in the two groups were comparable. The same holds true for the palatal cleft width that was also reduced during the orthopedic treatment, but after lip closure no significant differences were found between the groups anymore. Furthermore, when a plate was used, the palatal vault flattened. An explanation for this finding could be that the plate keeps the tongue out of the cleft, allowing the palatal shelves to flatten in the treated group. Once the soft palate was operated, the effect of treatment disappeared, and at 1–1/2 year of age, the shape of the palatal vault was comparable for both groups (Prahl et al. 2001). Neonatal orthopedics also did not prevent collapse of the maxillary arch (Prahl et al. 2003). The long-term results until 6 years of age showed no significant differences between the IO+ and IO− groups for maxillary arch dimensions (Bongaarts et al. 2006). In addition, the 5-year-old index (Atack et al. 1997), which is a measure for the jaw relationship, overjet, overbite, presence of cross bites, and sagittal occlusion were comparable in the two groups (Bongaarts et al. 2004).
Facial morphology at 4 and 6 years of age also did not differ between the two groups, although it has to be mentioned that at 6 years of age some attrition of the original sample had taken place as about 20 % of the patients was lost to follow-up (Bongaarts et al. 2009). At younger ages, there was no difference in facial appearance between the groups (Prahl et al. 2006). At the age of 4 years, IO had a positive effect on full facial appearance of UCLP children, but at the age of 6, only professionals saw a positive effect of IO on the nasolabial photographs. This seems to be rather irrelevant since patients deal with laymen in their daily life (Bongaarts et al. 2008).
We concluded that infant orthopedics has only a temporary effect on maxillary arch dimensions which does not last beyond soft palate closure. It also does not improve the jaw relationship and occlusion in the deciduous dentition, and it has no measurable effect on facial morphology and facial and nasolabial appearance until 6 years of age. Therefore, from the orthodontic and surgical point of view, neonatal maxillary orthopedics could be abandoned.
20.5.5 Effect on Speech
Evaluation of speech and language development showed that at the age of 1 year, the children who wore plates presented enhanced production of alveolar sounds in babbling; however, at the age of 1 and 1/2 years when the plate was no longer used, consonant production in babbling was comparable in the two groups (Konst et al. 1999).
Reports on the later speech and language development of the children in the DUTCHCLEFT study showed a limited effect on speech (Konst et al. 2003a, b, c). The speech results at 2.5 years of age showed differences in intelligibility between the groups. In two different experiments, untrained listeners as well as experienced speech and language therapists gave higher intelligibility ratings to the children who formerly used plates (Konst et al. 2003c). However, data obtained by a transcription task indicated no differences in actual intelligibility (Konst et al. 2000), but compared to their non-cleft peers, the children with clefts were significantly less well understood.
At 2.5 years of age, the phonological development of the IO+ children was normal or delayed, whereas most children who were not treated with a plate had abnormal development. Half a year later, it appeared that the IO+ children had acquired more initial consonants than the IO− group (Konst et al. 2003b). In the same age groups, the IO+ children used longer sentences than the IO− children, indicating that their grammatical development was more advanced. At the age of 6, no differences in expressive language skills between the two groups were found (Konst et al. 2003a). Hence, neonatal maxillary orthopedics did not have long-lasting effects on language development.
Regarding the claimed benefits of neonatal maxillary orthopedics on speech development in unilateral cleft lip and palate children, it can be concluded from this trial that there is a beneficial but rather limited effect until the age of 2 and 1/2 years. However, irrespective of neonatal maxillary orthopedics, the speech of children with clefts remains far behind that of their non-cleft peers. Due to lack of funding, the speech samples at the age of 6 years have not yet been analyzed.
20.5.6 Cost-Effectiveness
Nowadays, cost-effectiveness is an important issue, as costs of health-care interventions are often topic of debate. Especially in cases of reimbursement decisions, cost-effectiveness estimates can be useful. Together with the results of clinical effectiveness studies, cost-effectiveness information can be used to determine whether a certain treatment should become available to patients. The main principle of cost-effectiveness analysis is to estimate the costs and the treatment outcome (= effectiveness), compared to an alternative treatment (Drummond et al. 1997). Based on this explicit comparison, the difference in costs is related to the difference in effectiveness between alternative treatments. A prospective study in a randomized clinical trial design, such as DUTCHCLEFT, in combination with an economic evaluation is a good vehicle to analyze the cost-effectiveness (Severens et al. 1998; Cunningham 2001).
In DUTCHCLEFT, a cost-effectiveness analysis was planned for all three research areas that were mentioned above (see A, B, C). For the cost-effectiveness analysis, a so-called societal point of view was used, indicating that cost of treatment was based on real prices rather than fees. Besides this, a differential approach was used, aiming to calculate the difference in cost between yes or no neonatal maxillary orthopedics. A more extensive description of the cost analysis methods used in DUTCHCLEFT can be found in our earlier publications (Severens et al. 1998, 1999), which together with the publication by Cunningham [99] provide a good starting point to learn more about economic health evaluation.
In a preliminary report, the short-term cost-effectiveness of neonatal maxillary orthopedics was based on the duration of the operation for surgical lip closure (Severens et al. 1998). However, this effectiveness parameter has little to do with effectiveness in terms of clinical outcome, but at that time, as the trial was still running, no other effectiveness variables were available. In 2004, we published data on cost-effectiveness of neonatal maxillary orthopedics compared to no such treatment, focusing on speech outcome at 2 and 1/2 years of age (Konst et al. 2004
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


