Chapter 17 Multilevel surgery for obstructive sleep apnea/hypopnea syndrome
Effective surgical treatment for obstructive sleep apnea/hypopnea syndrome (OSAHS) must be designed to eliminate collapsible soft tissue in the upper airway without interfering with normal function. Creation of a non-collapsible airspace and reduction of airway resistance enables maintenance of adequate airflow with normal inspiratory effort. This translates into elimination or reduction of apneic/hypopneic episodes during sleep, control of symptoms and further minimizes ongoing multi-system damage in OSAHS patients. OSAHS is often caused by multiple levels of obstruction and therefore requires multilevel treatment. In the last decade, several surgical advances have been made in the management of OSAHS.
1 CONCEPT OF MULTILEVEL TREATMENT – ESTABLISHING THE BASIS
1.1 INCIDENCE OF MULTILEVEL OBSTRUCTIONS IN OSAHS PATIENTS
The true incidence of multilevel obstruction is a subject of much debate. Fujita1 first described different anatomic levels of obstruction in OSAHS. He recognized that half of the patients who underwent uvulopalatopharyngoplasty (UPPP) were non-responders. Most of the non-responders were identified as having multilevel obstruction. Combined oropharyngeal and hypopharyngeal obstruction was noted in 54.5% (36/66) of patients in his study. Thus, it is clear that Fujita himself never intended to suggest that UPPP will cure most patients with OSAHS. In 1993, Riley et al.2 reported their surgical experience, outlining a multilevel concept. Each patient was classified as having single level obstruction involving oropharynx only – type 1 – or the hypopharynx only – type 3. Multilevel obstruction was identified as type 2 and implied a combination of oropharyngeal and hypopharyngeal obstruction. Of the 239 patients, 93.3% (223 patients) were identified as having multilevel obstruction, type 2. Only 16 patients (6.7%) had single level obstruction. Of these, 10 patients had type 1 obstruction and six patients had type 3 obstruction.
This early classification by Fujita and Riley was based on physical examination of the patients with vague guidelines. Specific criteria for identifying unilevel versus multilevel obstruction were not reported. Subsequent development of the Friedman tongue position (FTP) allowed for a simplified method of staging the levels of obstruction.3,4 The early data based on FTP indicated that approximately 25% of patients presenting with OSAHS had unilevel obstruction, while 75% had multilevel obstruction.
To more precisely identify the anatomic sites of obstruction during sleep, sleep endoscopy was proposed as a preferred method. den Herder et al.5 reported an unusually high number of single level obstructions. In their study of 127 patients, 63% had single level obstruction while only 37% had multilevel disease. The study, however, may have misidentified the level of obstruction; tongue base obstruction pushing the palate backward causing secondary palatal obstruction may have been classified as primary palatal obstruction.6 Another study by Abdullah van Hasselt confirmed the high incidence of multilevel disease and 87% of their 893 patient populations had multilevel obstruction.7
1.2 SINGLE LEVEL SURGERY CANNOT BE THE ONLY TREATMENT FOR MOST OSAHS PATIENTS
UPPP was designed to enlarge the oropharyngeal airway8 and remains the most common surgical intervention for OSAHS. Review of the literature indicates the success rate (a 50% reduction in Apnea/Hypopnea Index (AHI) and a postoperative AHI of less than 20) for UPPP as an isolated procedure ranges from 25% to 80%. However, Sher et al.9 reported success rates for UPPP around 41% based on a meta-analysis of unselected cases. Although there are many reasons UPPP may fail, uncorrected retrolingual obstruction has been clearly identified as a major cause. This seems to support the concept that multiple levels of obstruction exist and explains why UPPP alone frequently results in failure.
1.3 MULTILEVEL SURGERY IS NOT LIMITED TO SEVERE DISEASE
Many otolaryngologists presume that although UPPP may not cure the patients with severe OSAHS, it is likely to be effective for patients with mild disease. There are however many studies indicating that the severity of disease is not a predictor of success with single level surgery.3,4,10 Senior et al.11 studied a group of patients with mild OSAHS (AHI less than 15). These patients underwent UPPP and the success rate was only 40%. Friedman further studied a series of patients with mild disease and showed an overall success rate of approximately 40% as well.3,4 If indeed most patients have multilevel disease, the success for the surgical treatment of mild OSAHS is not better than those for treating severe disease. In fact, the basis of the Friedman staging system is that anatomic findings are the most significant factors, rather than severity of disease. Multilevel surgery should not be reserved exclusively for the treatment of severe disease. It is therefore reasonable that multilevel treatment should be considered for most patients with mild disease as well as most patients with severe disease. Since the majority of patients suffering from OSAHS do have multilevel disease and directing the therapy to a single anatomic level has a high potential for failure, the need for multilevel therapy is evident.
2 HISTORY OF MULTILEVEL TREATMENT
Published data on multilevel treatment can be divided into four groups.
3 MULTILEVEL MINIMALLY INVASIVE TREATMENT FOR MILD/MODERATE OSAHS
Many options are available for minimally invasive treatment of palatal obstruction. Minimally invasive treatment options for retrolingual obstruction are limited, but have been in clinical use. There have been a few studies that looked at multilevel minimally invasive treatment. Steward19 studied 22 patients who underwent combined radiofrequency reduction of the palate and the base of tongue and reported a success rate of 59%. None of the patients had concomitant nasal surgery. Fischer et al. presented a similar study about multilevel minimally invasive surgery with radiofrequency on the palate, tonsil and tongue base for 15 OSAHS patients.20 The results showed that the AHI changed from 32.6±17.4 preoperatively to 22±15 for a success rate of 33%. Whereas the majority of Fischer’s patients had moderate disease, Steward’s patients had mild-to-moderate disease.
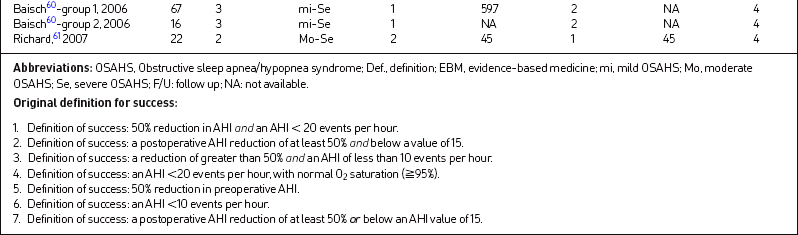
In 2004, Stuck et al.21 published their surgical results with radiofrequency on the palate and base of the tongue for 18 OSAHS patients with mild/moderate disease. They reported their success rate as 33.3% (by their definition of success, a postoperative AHI reduction of at least 50% and below a value of 15).
In 2007, we presented our experience on minimally invasive single-stage multilevel surgery (MISSMLS) for patients with mild/moderate OSAHS.22 Our patients underwent three-level treatment that included nasal surgery, palatal stiffening by pillar implant technique and radiofrequency volume reduction of the tongue base with a minimum follow-up of 6 months. The results in a retrospective review of a prospective dataset showed that both subjective and objective outcomes improved significantly, and treatment morbidity was minimal and only temporary. Mean bedpartner’s snoring visual analog scale (VAS) decreased from 9.4±0.9 preoperatively to 3.2±2.4 postoperatively. Epworth Sleepiness Scale (ESS) decreased from 9.7±3.9 preoperatively to 6.9±3.3 postoperatively. Mean AHI was reduced from 23.2±7.6 to 14.5±10.2. Classic success was achieved in 54 of 122 patients (47.5%).
4 SYSTEMATIC REVIEW OF LITERATURE ON MULTILEVEL TREATMENT FOR OSAHS PATIENTS
We recently reported on a systematic review of all English language literature on multilevel surgery for OSAHS patients as of 31 March 2007.23 Article titles and abstracts were reviewed to determine article eligibility. We also identified relevant publications from the lists of references in this subset of articles. The study design and its corresponding level of evidence were clarified as follows: (1) Level 1 – randomized controlled trials or a systematic review; (2) Level 2 – prospective cohort study; (3) Level 3 – case–control study; (4) Level 4 – case series; and (5) Level 5 – expert opinion.
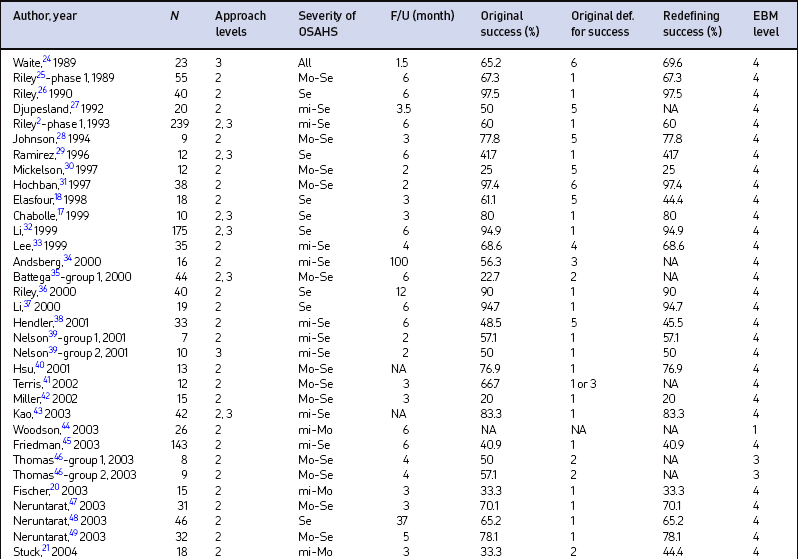
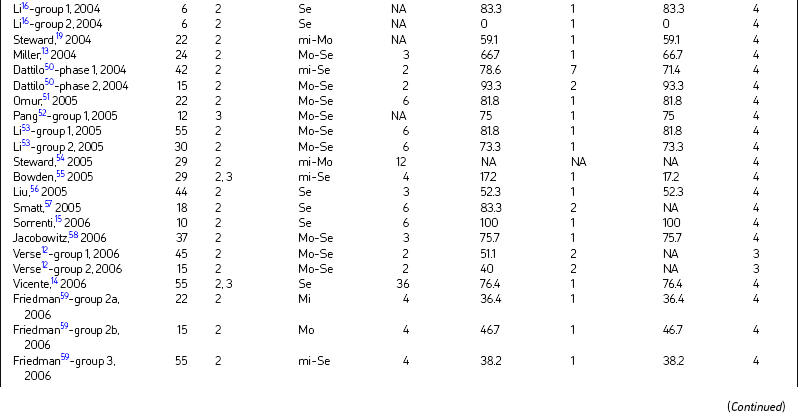
There were 49 papers (58 groups) selected for final inclusion after detailed review (Table 17.1). There were 1978 subjects included in the study with a pooled mean age of 46.2 years. The mean minimal time period from multilevel surgery to postoperative PSG was 7.3 months (range, 1–100 months).
< div class='tao-gold-member'>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses