Armamentarium
|
History of the Procedure
Since the first mandibular osteotomy (Hullihen, 1849), orthognathic surgical techniques have developed into the most commonly used surgical approach for correction of craniomaxillofacial deformities. The application of orthognathic surgical techniques involves complex, three-dimensional movements that require thoughtful preoperative planning. Early on, surgeons relied solely on their clinical and surgical experience to carry out osteotomies of the mandible (Hullihen, 1849; Blair, 1907). In 1935, Wassmund planned surgery by fabricating silver alloy splints from handheld segments of sectioned dental models. The use of the arbitrary face-bow transfer gained support after Schallhorn demonstrated that the arbitrary intercondylar hinge axis is within a 5-mm radius of the true hinge axis. In the 1960s and early 1970s, Obwegeser used a combination of handheld and mounted models on articulators to prepare for bimaxillary osteotomies. Lockwood developed a key spacer system for model surgery that used a plane line hinge articulator. Hohl advocated the use of an anatomic articulator and face-bow transfer in segmental maxillary surgery. Model surgery measurements using handheld millimeter rulers gave way to the Erickson Model Surgery Table (Great Lakes Orthodontics, Tonawanda, New York), allowing for more accurate model planning. Heggie challenged the accuracy of model surgery alone and suggested the use of a calibrator (modified Vernier caliper) to register the distance between the nasion (rhinion) and an arbitrary point on the nose and midline incisor tip, to assess the vertical maxillary position during surgery.
The traditional sequencing of bimaxillary orthognathic surgery, more commonly used by orthognathic surgeons, repositions the maxilla first, using the uncut mandible as a template. The mandible is then repositioned into occlusion with the repositioned maxilla. Contrary to established practice, Lindorf and Steinhauser, Buckley et al, Cottrell and Wolford, and Posnick suggested altering the sequence of bimaxillary model surgery planning and the step-by-step operative procedure. Their modified approach repositions the mandible first, and the maxilla then is placed into the most ideal occlusal relationship with the mandible. Only the vertical incisor position needs to be set at surgical repositioning of the maxilla. This sequence reduces laboratory time and avoids potential displacement of the repositioned maxilla during mandibular surgery, especially in cases with unreliable centric relation stops due to malformed or absent mandibular condyle (or condyles), large mandibular advancements, maxillary segmentation, and/or thin maxillary walls.
Both traditional and “reverse” planning methods obtain acceptable clinical outcomes, and both depend on the demands of the clinical problem, in addition to the surgeon’s knowledge, training, experience, and personal preference. Standard model surgery planning, although time-consuming in the laboratory, is still a predictable and reliable method for achieving accurate surgical repositioning in the operating room. Recently, virtual model surgery planning has gained popularity, and proponents have shown it to be an efficient and accurate alternative to standard model surgery planning. The learning curve and cost of virtual planning technology may be limiting factors. Certainly an accurate clinical examination must be performed and a thoughtful surgical plan developed before computer software planning.
History of the Procedure
Since the first mandibular osteotomy (Hullihen, 1849), orthognathic surgical techniques have developed into the most commonly used surgical approach for correction of craniomaxillofacial deformities. The application of orthognathic surgical techniques involves complex, three-dimensional movements that require thoughtful preoperative planning. Early on, surgeons relied solely on their clinical and surgical experience to carry out osteotomies of the mandible (Hullihen, 1849; Blair, 1907). In 1935, Wassmund planned surgery by fabricating silver alloy splints from handheld segments of sectioned dental models. The use of the arbitrary face-bow transfer gained support after Schallhorn demonstrated that the arbitrary intercondylar hinge axis is within a 5-mm radius of the true hinge axis. In the 1960s and early 1970s, Obwegeser used a combination of handheld and mounted models on articulators to prepare for bimaxillary osteotomies. Lockwood developed a key spacer system for model surgery that used a plane line hinge articulator. Hohl advocated the use of an anatomic articulator and face-bow transfer in segmental maxillary surgery. Model surgery measurements using handheld millimeter rulers gave way to the Erickson Model Surgery Table (Great Lakes Orthodontics, Tonawanda, New York), allowing for more accurate model planning. Heggie challenged the accuracy of model surgery alone and suggested the use of a calibrator (modified Vernier caliper) to register the distance between the nasion (rhinion) and an arbitrary point on the nose and midline incisor tip, to assess the vertical maxillary position during surgery.
The traditional sequencing of bimaxillary orthognathic surgery, more commonly used by orthognathic surgeons, repositions the maxilla first, using the uncut mandible as a template. The mandible is then repositioned into occlusion with the repositioned maxilla. Contrary to established practice, Lindorf and Steinhauser, Buckley et al, Cottrell and Wolford, and Posnick suggested altering the sequence of bimaxillary model surgery planning and the step-by-step operative procedure. Their modified approach repositions the mandible first, and the maxilla then is placed into the most ideal occlusal relationship with the mandible. Only the vertical incisor position needs to be set at surgical repositioning of the maxilla. This sequence reduces laboratory time and avoids potential displacement of the repositioned maxilla during mandibular surgery, especially in cases with unreliable centric relation stops due to malformed or absent mandibular condyle (or condyles), large mandibular advancements, maxillary segmentation, and/or thin maxillary walls.
Both traditional and “reverse” planning methods obtain acceptable clinical outcomes, and both depend on the demands of the clinical problem, in addition to the surgeon’s knowledge, training, experience, and personal preference. Standard model surgery planning, although time-consuming in the laboratory, is still a predictable and reliable method for achieving accurate surgical repositioning in the operating room. Recently, virtual model surgery planning has gained popularity, and proponents have shown it to be an efficient and accurate alternative to standard model surgery planning. The learning curve and cost of virtual planning technology may be limiting factors. Certainly an accurate clinical examination must be performed and a thoughtful surgical plan developed before computer software planning.
Indications for the Use of the Procedure
Craniomaxillofacial deformities involve both hard and soft tissues in all three planes of space. Prediction tracings provide an estimate of the amount and direction of maxillary and/or mandibular movement, but only in two dimensions and from a profile view. Definitive model surgery provides a more accurate assessment of planned surgical movements designed to establish an ideal, functional occlusion, with the condyles properly seated in the fossae and with simultaneous repositioning of the jaws in all three planes of space to enhance facial aesthetics. Model surgery planning ultimately allows the surgeon to take these goals, based on clinical and radiographic evaluation, to the operating room. Reasons for performing model surgery include (1) determining the magnitude and direction of skeletal movement; (2) assessing the position of planned osteotomies, especially interdental ones; (3) confirming the surgical plan; (4) allowing fabrication of surgical splints, to be used at the time of surgery, based on condylar function; and (5) providing a comparative reference to the occlusal result actually achieved after the release of intermaxillary fixation.
Face-bow transfer and articulator mounting are not necessary in surgery of the mandible alone. In isolated mandibular surgery, the mandible is repositioned into occlusion with the maxilla. The surgeon has determined that the maxilla is ideally positioned. Therefore, the maxilla is used as a template. Mandible-only surgical planning can easily be performed on a hinge (Giletti) articulator. Only a single (final) splint is required, which is fabricated from the planned ideal occlusal relationship.
Model surgery is especially important in the planning of bimaxillary surgery. When bimaxillary surgery is planned, accurate repositioning of the maxilla is critical because the maxilla must be ideally repositioned based on clinical and radiographic examination and using the current mandibular position as a template.
Occlusal splints make intraoperative surgical repositioning of the maxilla and mandible relatively simple, fast, accurate, and predictable. Given the three-dimensional complexity of maxillary repositioning, the intermediate splint accounts for anteroposterior and mediolateral positioning, in addition to pitch, roll, and yaw. Only the vertical position of the maxillary incisors needs to be planned for and addressed at surgery. The incisor vertical position is based on the presurgical clinical evaluation. Although model surgery planning and the fabrication of splints are time-consuming, it allows the surgeon to enter the operating room with confidence in the surgical plan.
Limitations and Contraindications
Although model surgery planning can provide consistently reliable results during surgery, there are many steps along the way. Each step has the potential to introduce inaccuracies that could ultimately affect the final outcome. Lapp outlined a number of arguments against model planning and splint fabrication, such as distortion of alginate impressions, inaccurate face-bow transfer, improper mounting of study models, dimensional distortion of acrylic splints, and a thin or overly thick intermediate splint acting as a potential factor in mandibular repositioning. A thin intermediate splint made without keeping a neutral pin position on the articulator leads to overreliance on condylar autorotation. A splint that is too thick can cause condylar distraction during maxillary repositioning. Lapp suggests that model planning and splint fabrication give the surgeon a “false sense of security.”
Technique: Model Surgery Planning
Step 1:
Presurgical Planning: Patient’s Clinical and Radiographic Evaluation and Records
A full history and clinical examination should always be obtained. Facial measurements (in millimeters) are recorded and include the maxillary dental midline to facial midline; mandibular dental midline to facial midline and to maxillary dental midline; presence or absence of maxillary cant; and maxillary incisor vertical position relative to the upper lip in repose and in posed smile. The surgeon must assess and plan for changes in the maxillary transverse dimension (buccal corridors), maxillary anteroposterior position, and maxillary and mandibular plane (pitch rotation). Maxillofacial plane rotation can have a positive influence on consonance of the maxillary incisors to the lower lip, incisor inclination, and nasolabial and profile esthetics.
A series of radiographs should be obtained (lateral cephalometric, posterior-anterior cephalometric, and panoramic radiographs), and cephalometric analyses should be performed using manual or computer software tracings. These should be available, if only as a guideline, at the time of clinical examination and planning.
The preferred repositioning of the maxilla, mandible, and chin is determined according to the patient’s desires and the surgeon’s preference, based on the overall clinical assessment (i.e., the patient’s objectives, the assessment of facial and smile esthetics, morphologic skeletal and dental limitations, and the cephalometric analysis).
Step 2:
Centric Relation Bite
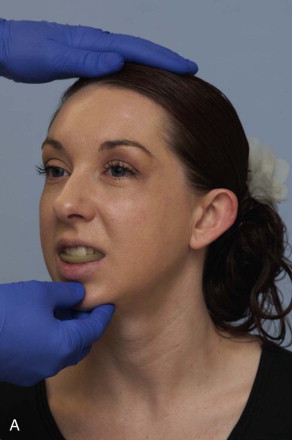
As defined in the Glossary of Prosthodontic Terms, centric relation (CR) is the maxillomandibular relationship in which the condyles articulate with the thinnest avascular portion of their respective discs with the complex in the anterior-superior position against the shapes of the articular eminencies. This position is independent of tooth contact. Centric relation is clinically discernible when the mandible is directed superiorly and posteriorly. It is restricted to a purely rotary movement about the transverse horizontal axis. To record the CR bite, place soft wax on the maxillary occlusion. Then register the patient’s maxillary occlusion into the soft wax. It is important that the surgeon be able to reproduce this centric relation bite with the patient in a neutral head position and the jaw relaxed. The centric relation bite is a bite the surgeon must accurately reproduce with the patient asleep on the operating table ( Figure 41-1, A and B ).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses