Introduction
The purpose of this study was to clinically evaluate miniscrew implant-supported maxillary canine retraction with corticotomy-facilitated orthodontics.
Methods
The sample consisted of 13 adult patients (5 men, 8 women; mean age, 19 years) exhibiting Class II Division 1 malocclusion with increased overjet requiring the therapeutic extraction of the maxillary first premolars, with subsequent retraction of the maxillary canines. Corticotomy-facilitated orthodontics was randomly assigned to 1 side of the maxillary arch at the canine-premolar region, and the other side served as the control. By using miniscrews as anchorage, canine retraction was initiated via closed nickel-titanium coil springs applying 150 g of force per side. The following variables were examined over a 4-month follow-up period: rate of tooth movement, molar anchorage loss, plaque index, gingival index, probing depth, attachment loss, and gingival recession.
Results
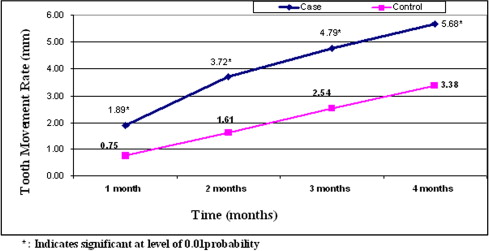
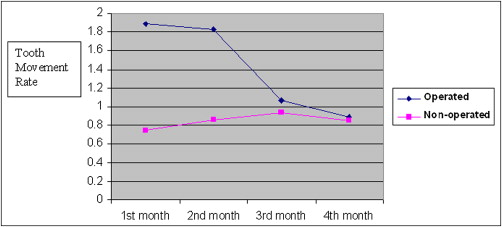
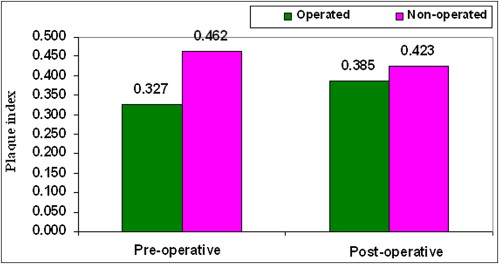
The average daily rate of canine retraction was significantly higher on the corticotomy than the control side by 2 times during the first 2 months after the corticotomy surgery. This rate of tooth movement declined to only 1.6 times higher in the third month and 1.06 times higher by the end of the fourth month. No molar anchorage loss occurred during canine retraction on either the operated or the nonoperated side. There was no statistically significant difference between preoperative and postoperative measurements of plaque index, probing depth, attachment loss, and gingival recession.
Conclusions
Corticotomy-facilitated orthodontics can be a feasible treatment modality for adults seeking orthodontic treatment with reduced treatment times.
The goal of orthodontic treatment is to improve the patient’s life adjustment through enhancement of dentofacial functions and esthetics. Reducing orthodontic treatment duration is an issue of importance, particularly for adults. Rapid orthodontic tooth movement with concomitant reduction in treatment time can be attained through a combination of orthodontic treatment and surgical alveolar corticotomies. Corticotomy is defined as any intentional surgical injury to cortical bone. In adult patients, this technique has been claimed to dramatically reduce the treatment time because the resistance of the dense cortical bone to orthodontic tooth movement is removed. The alveolar corticotomy technique has been revised and modified over the years to eliminate its possible risks, such as periodontal damage and devitalization of the teeth and osseous segments because of inadequate blood supply. According to Köle, the tooth embedded in a bony block of medullary bone served as the handle by which bands of less dense medullary bone surrounding the teeth were moved block by block. On the other hand, Wilcko et al attributed the increased rate of tooth movement after corticotomy-facilitated orthodontics (CFO) to a “regional acceleratory phenomenon” (RAP), which is characterized by an increase in bone turnover and a drop in mineral content.
Securing appropriate anchorage is an imperative factor for achieving the objectives of orthodontic treatment. Anchorage loss often produces unsatisfactory treatment results, particularly in patients who require maximum anchorage, with a resultant increase in the treatment period. Skeletal anchorage has evolved as a mainstream orthodontic technique with the introduction of temporary anchorage devices. These devices give the clinician an alternative anchorage system instead of conventional extraoral appliances that require full patient compliance. Titanium screws have been used as skeletal anchors because they can provide absolute anchorage without patient cooperation, and are useful for various orthodontic tooth movements with minimal anatomic limitations and simpler placement techniques. Orthodontic treatment combined with corticotomy and placement of a temporary anchorage device might have the advantage of shortening the orthodontic treatment period, especially in maximum anchorage situations. The purpose of this study was to evaluate miniscrew implant-supported maxillary canine retraction with and without CFO.
Material and methods
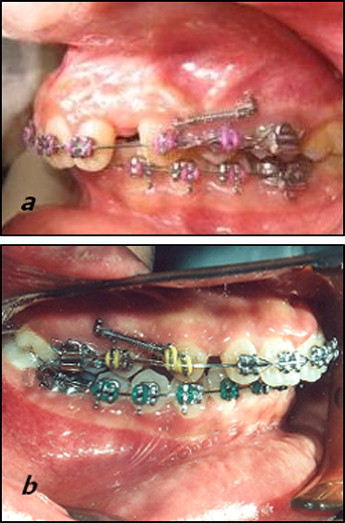
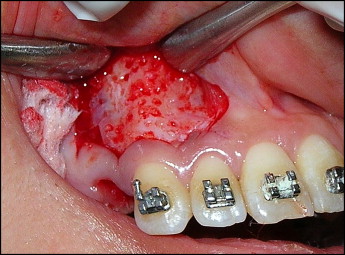
The sample consisted of 13 adult patients (5 men, 8 women; mean age, 19 years) exhibiting Class II Division 1 malocclusion with increased overjet requiring the therapeutic extraction of the maxillary first premolars, with subsequent retraction of the maxillary canines. Ethical approval was obtained from the Ethics Review Committee of the dental school at Cairo University, Cairo, Egypt. All patients had to fulfill the following criteria: healthy systemic condition, no previous orthodontic treatment, adequate oral hygiene, probing depth values (measured as the distance from the bottom of the sulcus to the most apical portion of the gingival margin) not exceeding 3 mm in the whole dentition, no loss of periodontal attachment (measured as the distance from the bottom of the sulcus to the cementoenamel junction), and no radiographic evidence of bone loss. All patients were informed of the procedure and signed an informed consent. After placement of maxillary and mandibular fixed appliances and completion of the leveling and alignment phase of treatment, miniscrew implants (AbsoAnchor, Dentos, Daegu, Korea; diameter, 1.3 mm; length, 8 mm), used as skeletal anchor units, were placed bilaterally between the maxillary second premolar and the first molar. On the day before the corticotomy surgery, 1 maxillary premolar was extracted on a random basis (coin toss). When the patient was scheduled for the surgery, the other premolar was extracted, and CFO was performed by using the submarginal Luebke-Ochsenbein flap design. By means of a periodontal probe, 4 mm were measured from the free gingival margin following the contours of the gingiva and extending from the mesial surface of the maxillary lateral incisor to the mesial surface of the maxillary second premolar ( Fig 1 ). A number 11 blade in a blade handle (Bard-Parker, Aspen Surgical Products, Lake Forest, Ill) was used to make the bucco-labial incision. The relieving incisions were placed vertically to avoid compromising the blood supply of the nonflapped tissue. A full-thickness mucoperiosteal flap was elevated via a muco-periosteal elevator, and the flap reflection was extended when possible beyond the root apex of the canine. By using a number 2 round bur in a low-speed hand piece under copious irrigation, corticotomy perforations were made extending from the lateral incisor to the first premolar area. The depth of the holes approximated the width of the buccal cortical bone. Thereafter, the flap was carefully repositioned and sutured with nonresorbable 4-0 black silk by using the single interrupted technique. The maxillary archwire (0.016 × 0.022-in stainless steel) was then ligated, and nickel-titanium closed-coil springs applying 150 g on each side were used for retraction, stretched bilaterally from the miniscrews to the canine hooks.
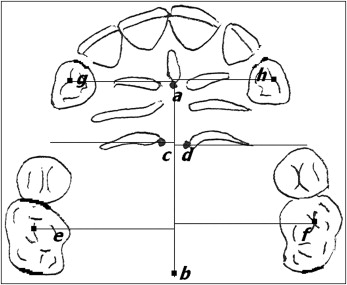
Periodontal health was assessed by evaluating the following parameters: plaque index, gingival index, probing depth, attachment level, and gingival recession according to the method of Silness and Loe. Dental casts were used for the quantification of the anteroposterior movement of the canines and the first molars ( Fig 2 ) every 30 days with the method described by Ziegler and Ingervall.
Statistical analysis
Descriptive statistics were computed for the variables of tooth movement (canine retraction and molar anchorage loss) and periodontal indices before and after canine retraction, and the results were graphically represented ( Tables I and II ; Figs 3-10 ). A paired t test was used to determine the statistical significance of the difference between the operated and nonoperated sides for preoperative and postoperative measurements.
| Operated | Nonoperated | |
|---|---|---|
| Mean (preoperative) | 13.79 ± 1.157 | 13.62 ± 1.062 |
| Mean (postoperative) | 13.73 ± 1.163 | 13.50 ± 1.100 |
| Month 1 | Month 2 | Month 3 | Month 4 | |
|---|---|---|---|---|
| Operated | 1.89 | 1.83 | 1.07 | 0.89 |
| Nonoperated | 0.75 | 0.86 | 0.93 | 0.85 |