Armamentarium
|
History of the Procedure
The earliest descriptions of mandibular fractures appeared in ancient Egyptian texts. The first case description, in 1650 BC, discussed the examination, diagnosis, and treatment of mandibular fractures.
Hippocrates was the first to describe reapproximation and immobilization of these fractures using circumdental wires and external bandaging. The importance of establishing proper occlusion was first described in a textbook written in Salerno, Italy, in 1180. The use of maxillomandibular fixation (MMF) was first mentioned in 1492, in the book Cyrugia, printed in Lyons. Chopart and Desault used dental prosthetic devices to immobilize the fracture segments. Guglielmo Salicetti first used intermaxillary fixation (IMF). Orthodontic bands and arches were used for establishing the fixation. However, Glimer revolutionized the treatment of fractures when he fixed full arch bars on both the mandible and maxilla.
Gordon Buck, in the United States, is credited with being the first to place an interosseous wire in mandibular fractures, in 1847, just after the introduction of ether anesthesia. Wire internal fixation in mandibular fractures was always supplemented with MMF. To overcome the lack of stability at the fracture site, more rigid hardware and a newer technique were developed.
The use of external pin fixation became popular during the World War II in the treatment of compound, comminuted, and infected fractures. The major advantage of external fixation is that it does not require extensive dissection and stripping of soft tissues. The current diminished role for external devices does not preclude their usefulness. There are still several indications for their application. However, surgeons must still be familiar with their applications due to their use in special circumstances. External pin fixation for maxillofacial applications has become synonymous with the term “Joe Hall Morris appliance.” The Joe Hall Morris appliance consisted of external pins with an acrylic bar apparatus used for closed reduction of mandibular fractures.
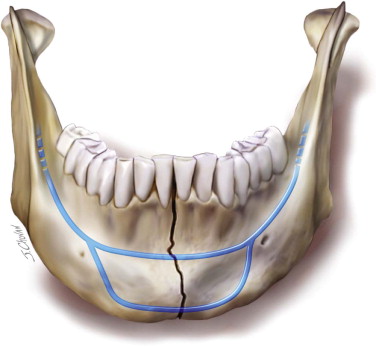
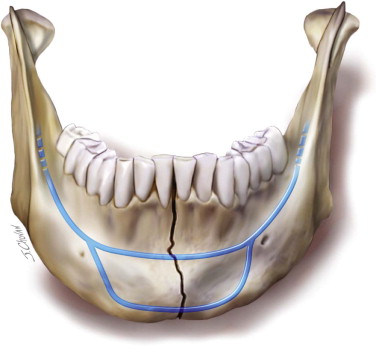
The technique of rigid internal fixation was advanced and popularized by the AO/ASIF (Arbeitsgemeinshaft fur Osteosynthesefragen/Association of the Study of Internal Fixation) in Europe in 1970. Champy et al developed the concept of adaptive osteosynthesis. He advocated transoral placement of small, thin, malleable miniplates with monocortical screws along the ideal lines of osteosynthesis in the mandible ( Figure 65-1 ). The locations of bone plate fixation should provide the most stable means of fixation. Arch bars or a plate placed along the superior border of the mandible provides the ideal position to resist tension forces in body fractures. This plate must be monocortical because of the presence of teeth. Additional fixation is required to achieve the appropriate stability. Functional stable fixation with miniplate fixation remains controversial. Large load-bearing plates are recommended in the treatment of mandibular fractures, especially in the following situations: comminution, continuity defects, and/or infection ( Figure 65-2 ).
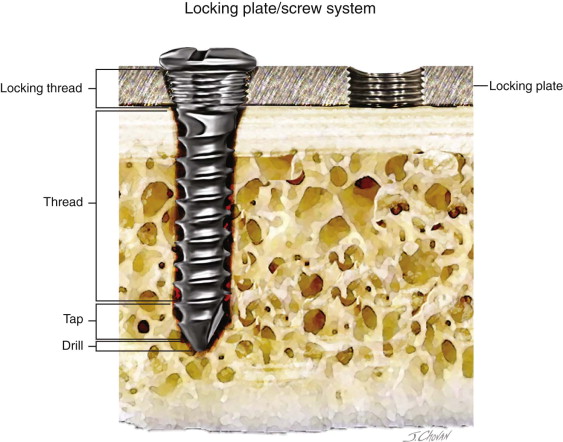
Locking Versus Nonlocking Plates
Locking plate/screw systems offer several advantages over the conventional type:
- 1.
Conventional plate/screw systems require precise adaptation of the plate to the underlying bone. The fixation in a locking plate allows the screw to lock into the plate, stabilizing the plate screw fractured segments without alteration of the reduction.
- 2.
Theoretically, locking plates fixation may also prevent disruption of the underlying cortical bone perfusion.
- 3.
Screws inadvertently inserted into a fracture gap will not loosen because they are locked into the plate.
History of the Procedure
The earliest descriptions of mandibular fractures appeared in ancient Egyptian texts. The first case description, in 1650 BC, discussed the examination, diagnosis, and treatment of mandibular fractures.
Hippocrates was the first to describe reapproximation and immobilization of these fractures using circumdental wires and external bandaging. The importance of establishing proper occlusion was first described in a textbook written in Salerno, Italy, in 1180. The use of maxillomandibular fixation (MMF) was first mentioned in 1492, in the book Cyrugia, printed in Lyons. Chopart and Desault used dental prosthetic devices to immobilize the fracture segments. Guglielmo Salicetti first used intermaxillary fixation (IMF). Orthodontic bands and arches were used for establishing the fixation. However, Glimer revolutionized the treatment of fractures when he fixed full arch bars on both the mandible and maxilla.
Gordon Buck, in the United States, is credited with being the first to place an interosseous wire in mandibular fractures, in 1847, just after the introduction of ether anesthesia. Wire internal fixation in mandibular fractures was always supplemented with MMF. To overcome the lack of stability at the fracture site, more rigid hardware and a newer technique were developed.
The use of external pin fixation became popular during the World War II in the treatment of compound, comminuted, and infected fractures. The major advantage of external fixation is that it does not require extensive dissection and stripping of soft tissues. The current diminished role for external devices does not preclude their usefulness. There are still several indications for their application. However, surgeons must still be familiar with their applications due to their use in special circumstances. External pin fixation for maxillofacial applications has become synonymous with the term “Joe Hall Morris appliance.” The Joe Hall Morris appliance consisted of external pins with an acrylic bar apparatus used for closed reduction of mandibular fractures.
The technique of rigid internal fixation was advanced and popularized by the AO/ASIF (Arbeitsgemeinshaft fur Osteosynthesefragen/Association of the Study of Internal Fixation) in Europe in 1970. Champy et al developed the concept of adaptive osteosynthesis. He advocated transoral placement of small, thin, malleable miniplates with monocortical screws along the ideal lines of osteosynthesis in the mandible ( Figure 65-1 ). The locations of bone plate fixation should provide the most stable means of fixation. Arch bars or a plate placed along the superior border of the mandible provides the ideal position to resist tension forces in body fractures. This plate must be monocortical because of the presence of teeth. Additional fixation is required to achieve the appropriate stability. Functional stable fixation with miniplate fixation remains controversial. Large load-bearing plates are recommended in the treatment of mandibular fractures, especially in the following situations: comminution, continuity defects, and/or infection ( Figure 65-2 ).
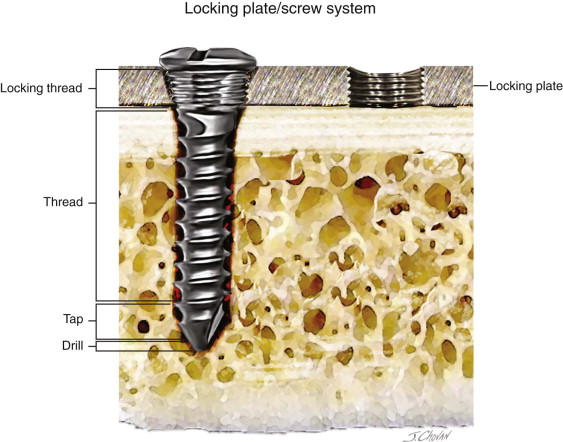
Locking Versus Nonlocking Plates
Locking plate/screw systems offer several advantages over the conventional type:
- 1.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


