Fig. 8.1
(a–c) A patient was scheduled for periodontal surgery in the maxillary left quadrant. The periapical radiograph revealed endodontically treated bifurcated premolar with a dowel in the palatal root (b). A 5 mm probing defect was noted in midbuccal area and the probing was between normal limits in all the other aspects. Upon reflecting the periodontal flap (c), a typical dehiscence for a vertical root fracture in an endodontically treated tooth was seen. The dehiscence was limited to mainly the coronal area of the root which corresponds with the graphic illustration (a).The fracture and the dehiscence were noted early enough so there is still interproximal bone that will enhance the prognosis of the future implant
Class Ib: including bony dehiscence in which the defect involves the coronal and middle third of the root without affecting the apical third (Fig. 8.2a–c)
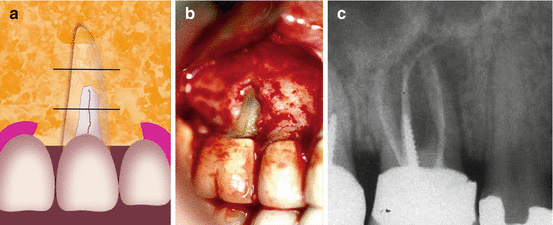

Fig. 8.2
(a–c) A graphic illustration of class 1b of which the defect involves the coronal and middle part of the root not involving the apical third (a). (b) Shows a dehiscence along a mesiobuccal root of a maxillary molar. The periapical radiograph (c) shows a large radiolucency around the palatal and the mesiobuccal root of the maxillary molar with a gutta-percha tracing cone in the area from a draining sinus tract
Subclasses (a-c) represent the evolution from an incomplete fracture affecting only the coronal portion of the root (Class Ia) to a fracture extending to the middle portion (Class Ib) and finally encompassing the apical third of the root (Class Ic) (Fig. 8.3a–c).
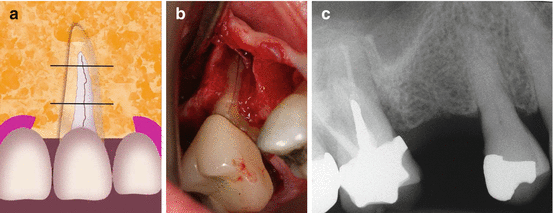

Fig. 8.3
(a–c) A large dehiscence of bone facing a vertical root fracture in a maxillary molar. The schematic illustration shows that the fracture line and the dehiscence include all three thirds of the root (a). A VRF extending to the full length of the mesiobuccal root of a maxillary molar (b). The radiographic image (c) shows bone loss adjacent to the MB root (Courtesy Dr. D. Greenfield)
Class II: Vertical Bone Defects
Class II defects include bony dehiscence (V- or U-shaped) involving both buccal and interdental bone.
This type of defects has three subcategories depending on the vertical dimension: Class IIa involves the most coronal third of the bone socket, Class IIb involves also the middle third, and Class IIc extends to the apical portion.
Defects affecting interdental bone may cause the complete loss of one bone peak (mesial and/or distal) (Fig. 8.4a–c).
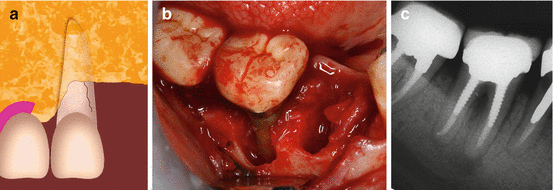

Fig. 8.4
(a–c) A graphic illustration of an interproximal defect causing bone loss of the crest on either mesial or distal aspects of a tooth or both (a). A typical angular–mesial and distal bone loss due to a root fracture in a mesial root of a mandibular molar (b). The periapical radiograph (c) show both mesial and interproximal radiolucencies around the mesial root (Courtesy Dr. E. Venezia)
The absence of one of the bone peaks creates a defect in which only a single residual wall remains after tooth extraction.
The involvement of interdental bone could be an evolution of defects (Class II) over time. The complete loss of one interdental bone peak leads to a one-wall defect.
Class III: Sites with Fenestrations
Class III defects are fenestrations, bone defects characterized by the presence of a bridge of intact bone coronal to the defect and usually located at the apical third of the postextraction socket (Fig. 8.5a–c).
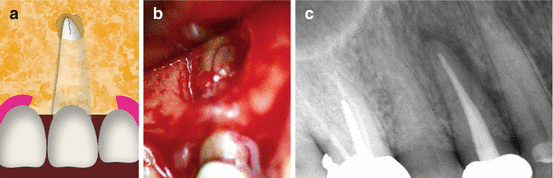

Fig. 8.5
(a–c) The graphic illustration (a) and the clinical VRF case in a maxillary premolar (b) are demonstrating a typical fenestration in the bone. The periapical radiograph (c) shows a typical “halo” (“J”)-type radiolucency around the apical part of an endodontically treated maxillary premolar
These defects may be due to the presence of an inflammatory or infective focus due to an incomplete VRF at the apical portion of the root [14].
Class III could be caused by incomplete fractures developing from the apex in a coronal direction.
It has been suggested that vertical root fractures insidiously can evolve over a period of time, from a marginal crack to a complete fracture involving the whole length of the root [24].
Implant Treatment Choice After Extraction of VRF Tooth in Consideration to Classification of VRF Alveolar Bone Defects
VRF Class Discussion and Clinical Guidance
Class I: Narrow and Wide Buccal Dehiscences
The use of resorbable (mainly collagen) and nonresorbable (mainly ePTFE) membranes for treatment of bone dehiscence both with or without the use of bone grafting material has been widely reported [25–37].
A number of studies described the use of autogenous bone [26, 28–30, 32, 33, 36, 37], deproteinized bovine bone mineral [27, 32–34], allogeneic graft [31], or no graft [25] in association with nonresorbable membranes.
The 5-year survival rate of maxillary implants placed together with ePTFE membranes varied from 76.8 % [26] to 100 % [32, 36]. Percentage of defect fill with this technique ranged between 70 and 100 % [25, 28–30, 34, 35], while in one study the bone fill was higher than 70 % [28]. The most frequently described complication was membrane exposure (up to 41.2 % of cases [35]).
Resorbable membranes have also been successfully applied for the treatment of dehiscence-like defects associated with implant placement [27, 28, 32, 33, 35, 37–48].
Bioresorbable barriers may be used alone [28, 35, 38, 39] or in combination with deproteinized bovine bone mineral (DBBM) [25, 32, 33, 37, 41–44, 46, 47] or other grafting materials, such as allograft or autogenous bone [28, 32, 33, 36, 45, 48]. High implant survival rates have been described also with this type of membrane alone [28] or combined with DBBM [41–44, 46, 47] and autologous bone or other bone substitutes [28, 36, 45, 49]. The incidence of reported complications (mainly membrane exposures) reached up to 39 % [35]. In one single study, the use of titanium meshes and autogenous bone was described, reporting 93.5 % bone defect fill [50].
Our review of the literature indicates that in Class I defects, the dehiscence could be successfully resolved with either nonresorbable or resorbable barriers. Moreover, no differences could be evaluated in bone regeneration in relation to the height of the defect [36]. An important clinical consideration here is the ability to achieve an adequate primary stability of the implant and complete soft tissue closure during the healing phase [51, 52].
Class II: Vertical Bone Defects
A number of studies reported techniques for the regeneration of vertical bone defects simultaneously with implant placement [53–63].
No statistically significant differences in implant survival were reported between nonresorbable and resorbable barrier membranes among studies where this type of comparison was performed [58–60].
Implant survival rates were generally high [54–57]. Postsurgical complications were frequent ranging from 9 to 45.5 % [58, 59]. Membrane exposure was the most frequent but the only complication reported [59].
Studies describing the treatment of vertical defects, with loss of interdental bone only on one side, categorized here as Class II cases, are relatively scarce. A previous systematic review [64] suggested, based on clinical and histological data, the potential use of vertical bone regeneration techniques in such situations. High survival rates for implants placed simultaneously with vertical ridge augmentation have been reported [53–63]. The frequency of complications in such cases appears to be high and should be carefully considered in the overall treatment plan. In these cases, the stabilization of the barrier (both resorbable and nonresorbable) is often challenging due to the characteristics of the bone defect, while the experience of the operator is also a factor that determines success [59]. Due to these reasons, a two-stage rather than a single-visit surgical protocol appears to yield more success in Class II defects [64].
Class III: Sites with Fenestrations
Several studies have reported on the management of fenestrations by guided bone regeneration (GBR) with membranes at the time of implant placement [26–29, 38–40, 49, 50].
Reported survival rates are high [26]. Apparently, bioresorbable membranes lead to a higher implant survival rate than the nonresorbable ones. Membrane exposures were reported only in the use of nonresorbable membranes.
There are a relatively few studies related to the Class III classification with bony fenestrations [26–29, 38–40, 49, 50]. In two studies, the use of ePTFE membranes showed a relatively low percentage of complete bone defect filling (above 85 %) [25, 26], and this could be a reasonable basis to avoid their application [26].
Final Considerations
Immediate implant placement following the extraction of a vertically fractured tooth may be a challenging treatment alternative due to the presence of bone defects as well as infection and inflammation in the surgical area [65]. Accurate debridement of the extraction socket is mandatory as one of the fundamental prerequisites for obtaining long-term implant survival rates [66]. Following improper lesion debridement, bacteria could be isolated even from specimens taken from fully healed bone [67].
Spread of infection into subjacent niches from the fracture site may also be a serious concern when planning implant placement [12–14].
It has been proposed, in particular in anterior esthetic zones, that immediate and, even more, early postextraction implants may be helpful in maintaining the stability of the soft tissues to achieve better esthetic outcome [68–71]. Implants can be placed in infected sites without the occurrence of severe complications, when an adequate debridement of the socket is performed [17, 72, 73]. Primary soft tissue closure is mandatory for the success of any bone regenerative procedure, especially when barrier membranes are applied. Delaying implant placement and bone regeneration for a few weeks could present a viable treatment alternative to lower complication rate due to spontaneous membrane exposure [41].
The scientific literature has validated the use of guided bone regeneration to treat peri-implant bone defects at the time of implant placement [74, 75].
The fact that wider defects are more clinically challenging implies that careful diagnostic evaluations are needed to detect the fracture at an earlier stage. While only invasive procedures, as open flap, can confirm the exact extent of VRF [4], the use of advanced imaging techniques such as cone beam computed tomography can be of help for early diagnosis [76]. Finally, whenever cases of VRF are detected during explorative surgery [4, 77, 78], a sound knowledge of the bone defect anatomy can help in the decision concerning the best bone augmentation alternative.
Detailed studies documenting the dimensions and anatomy of bony defects connected to VRF are necessary to base the present classification on evidence.
References
1.
2.
3.
4.
5.
6.
7.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


