Fig. 7.1
Root amputation of a vertically fractured mesiobuccal root of an upper molar. (a) An upper molar was diagnosed with pulp necrosis and asymptomatic apical periodontitis. (b) A root canal treatment was performed. (c) One-year latter the patient presented with a sinus tract, and the tooth was diagnosed with chronic apical abscess. The patient was scheduled to endodontic surgery. (d) During endodontic surgery, a vertical root fracture was diagnosed in the mesiobuccal root. The root was amputated just apically to the epithelial attachment. (e) One-year postsurgery follow-up: the tooth was asymptomatic and was diagnosed with normal apical issues
The periodontal status of the VRF tooth and especially the presence of a predisposing periodontal disease are important confounders for the ability to successfully treat and preserve the tooth [31]. The periodontium serves as the supporting apparatus for the teeth and is consisted from the alveolar mucosa, gingiva, cementum, periodontal ligament, and alveolar bone [32]. Periodontal diseases are infections and are caused by microorganisms that colonize the tooth surface at the gingival margin and may sometimes lead to a destruction of the periodontium [33].
A severe periodontal disease may compromise the ability to preserve the natural tooth, and interpretation of commonly used clinical parameters to determine the periodontal disease severity is therefore indicated [31]. In general, deep periodontal probing depth with an associated bleeding are indicators of periodontal disease activity as well as predictors of future attachment loss [31]. And severe periodontal disease with significant mobility, especially vertical mobility, significantly reduces the tooth prognosis [26].
Failure to maintain the natural tooth may lead to esthetic complications [34]. With modern dental practice, osseointegration of implants is readily attainable with high long-term survival rates [35–38]. However, dental implant success should be judged not only by osseointegration but also by esthetic results, and aesthetic predictability can often be difficult to attain. In addition, when esthetic implant failures occur, it may be impossible to be fully corrected [35–38].
On the other hand, periodontal defects such as gingival recession may be caused by surgical manipulations during attempts to preserve the VRF tooth [32, 39–44]. And periodontal bone loss with ensuing esthetic complications is more extensive in patients presented with thin periodontal biotype [34]. Therefore, a comprehensive periodontal and esthetic evaluation should be an integral part of the treatment planning of a VRF tooth [31, 35–38].
Although early diagnosis of VRF is important, the VRF may be diagnosed only after all endodontic and prosthetic procedures have been completed [8] due to lack of specific signs, symptoms, or radiographic features and because several etiologic factors may be involved [3, 11, 45–51]. Therefore, the timing of VRF diagnosis, either before or after the restorative procedures have been completed, and also the type of prosthetic restoration (e.g., a tooth that is a part of a bridge or a stand-alone restoration) may affect the decision whether to make additional efforts to preserve the vertically fractured tooth [31].
Many prosthetic and periodontal parameters affect the long-term prognosis of endodontically treated teeth, such as the amount of remaining tooth structure, the crown–root ratio, presence of tooth mobility, ferrule effect, and many more [28]. In addition, an appropriate postendodontic treatment restoration is extremely important for the long-term prognosis of the tooth [52].
Therefore, the decision to perform an additional treatment to preserve a VRF tooth should not be based only on the technical ability to endodontically treat the fracture line but on a broader spectrum of prosthetic, periodontal, and esthetic considerations that determine the long-term prognosis of the tooth and the risk of complications.
Treatment Options
In cases of strategically important teeth, an attempt can be made to preserve the tooth by treating the VRF. Several treatment options may be considered, including root amputation or root extraction, apical surgery with root shaving coronally to the fracture line, and sealing/cementation of the fracture following flap elevation approach or by extraction and replantation.
Various attempts to treat VRF teeth have been reported. While in most cases the treatments eventually resulted in tooth extraction, certain advances have been achieved in recent years, enabling the preservation of VRF teeth [7, 13, 14, 53–57]. The specific treatment alternative should be selected based on the tooth type, fracture type and location, prosthetic and esthetic considerations, and periodontal considerations.
Root Amputation and Root Extraction
When a VRF is diagnosed in single roots of a multirooted tooth, the most straightforward option is to surgically remove the fractured root only. More than 100 years ago, Farrar [58] described a surgical technique that included root resection with a filling of the remaining part with an ordinary filling material, such as amalgam. Farrar proposed resection at various levels, even leaving a short root stamp in the gingival tissue [58].
In some cases, a portion of the crown can be resected together with the involved root. In other cases, a tooth can be extruded orthodontically for easier management of the remaining tooth structure [7].
Root amputation may be recommended for maxillary molars with one fractured root (Fig. 7.1). Depending on the level of the fracture line and periodontal status of the patient, the resection can be performed at different levels of the root, and the most coronal part of the root can be retained following a root-end management and retrograde filling. A careful presurgical evaluation should be performed to exclude the possibility of fused roots rendering the amputation impossible. For fractured fused roots, a proper technique was described by Matusow [59] as “root stripping.” He presented a case of a second mandibular moral that served as a bridge abutment with fused medial root with VRF. The fused root was surgically “stripped,” leaving the distal root segment intact. This technique may be attempted for management of maxillary premolars with fractured buccal root where apically positioned furcation prevents a conventional root resection. For mandibular molars, while a root amputation is sometimes performed, hemisection and extraction of the fractured root or root resection is a more reliable option.
Techniques for the Preservation of a Fractured Root
The actual treatment for the VRF may be divided into two main categories: a treatment modality that includes extraction and replantation of the involved root or tooth following extraoral repair of the fracture; and repair of the fracture using flap elevation procedure while the tooth remains attached in the periodontium.
Tooth Extraction, Cementation of the Root Fracture, and Replantation
Extraction of the fractured tooth, cementation of the root fracture, and replantation as an attempt to preserve VRF teeth was reported in several case reports and in a case series [14–16].
Hayashi Kinomoto et al. [16] reported on treatments of 26 vertically fractured roots using replantation and reconstruction with dentin-bonded resin. They found that 18 cases were functional and retained, with 6 fully successful, after 4–76 months. They found that teeth with longitudinal fractures extending more than 2/3 from the cervical portion toward the apex and posterior teeth showed significantly lower success rates [16].
Arikan et al. [14] presented a successful treatment after 18 months follow-up of a central incisor with complete VRF that was extracted and root segment bonded and replanted. Kawai et al. [15] attempted a modification of this approach by replanting two VRF teeth with resin-bonded segments at 180° rotation into the original socket in order to bring the fracture line under healthy bony coverage and sound periodontal ligaments on the tooth surface face the destroyed boneless area. Hadrossek et al. [55] treated a central incisor by filling the fracture line and the retrograde preparation with a calcium silicate cement (Biodentine).
Another case of bonding the fracture line with adhesive resin cement was reported by Moradi Majd Akhtari et al. [60]: vertically fractured maxillary incisor was extracted, the fracture line was treated with adhesive resin cement, and the tooth was replanted. After 12 months, the tooth was asymptomatic [60].
In addition to doubtful prognosis of the fracture repair, the main disadvantage of this treatment modality is the risk of complications related to the extraction, such as inability to extract the tooth in one piece, lack of periodontal healing or bone resorption following replantation, and root resorption due to the damaged PDL. Therefore, the contraindications for tooth extraction and replantation are teeth which probably cannot be extracted and repositioned due to a complicated root anatomy, teeth with severe periodontitis, teeth without adjacent teeth, a noncompliant patient, and patients with critical general medical conditions [55].
Flap Elevation and Cementation of the Root Fracture
Several attempts to treat VRF by a flap procedure to gain access to the fracture line and enable its management were described. Selden [61] reported on a conservative treatment of six teeth with incomplete VRF using silver glass ionomer cement with bone graft, but all cases presented in that study failed in the long term [61].
Modern endodontics presents a possibility to treat fractured teeth by employing magnification and illumination devices that allow better visualization of the surgical field, thus increasing the accuracy of the treatment.
MTA was proposed as a sealing material to repair VRF [21], by preparing a groove along the entire vertical fracture, placing MTA in the groove and covering it with a absorbable membrane. Floratos et al. prepared the fracture line using a rotary or ultrasonic instrument with ensuing sealing of the defect with MTA and coverage with absorbable collagen membrane or calcium sulfate using microsurgical techniques and the microscope-assisted regenerative procedures [13].
Taschieri et al. [4] reported on 10 maxillary anterior teeth with incomplete VRF treated by a modern surgical endodontic technique (Fig. 7.2). Strict inclusion criteria were applied—teeth with probing depths of more than 4 mm or cases with halo-like periradicular radiolucency or interproximal angular radiolucency on one side of the root were excluded from that study. Following flap elevation, a groove following the fracture line was prepared using ultrasonic devices and sealed with MTA, and then filling of the bone defect with calcium sulfate. At 12 months follow-up, all cases were successful. After 33 months from seven patients available for follow-up, five cases remained healed [4].
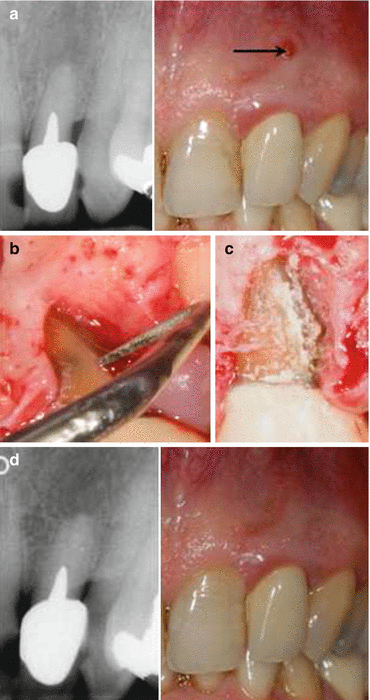

Fig. 7.2
Flap elevation procedure to repair incomplete vertical root fracture. Maxillary left lateral incisor. (a) Preoperative radiograph and clinical evidence of a sinus tract (arrow); (b) a groove was made on the root surface using a zirconium nitride retrotip along the fracture line; (c) the groove was filled with MTA as sealing material; (d) clinical and radiographic evidence of complete healing at 33 months follow-up (Reprinted from Taschieri et al. [4], Copyright (2010), with permission from Elsevier)
Dederich et al. [62] in a case report of a mandibular premolar sealed a hairline vertical fracture associated with a vertical bone defect using a CO2 laser with subsequent placement of collagen matrix barrier over the defect. After 12 months, no evidence of inflammation was detected; however, gingival recession was present [62].
Floratos and Kratchman [13] treated four cases in which endodontically treated maxillary or mandibular molars had an incomplete VRF involving one of the roots. Unlike in the study by Taschieri et al. [4], in this study, a similar technique was used successfully in anterior teeth with vertical fracture lines deriving from the apical part of the root. The fracture line was eliminated by resecting the root in a beveled manner, after which root-end preparation and root-end filling were performed by using MTA. The osteotomy was covered with an absorbable collagen membrane. After 8–24 months, cases demonstrated clinical success [13].
The flap procedure may have several disadvantages: a possible scar may form in the esthetic area of the gingiva, an additional osteotomy may be needed which generates extra loss of healthy bone structure, and a gingival recession may be expected. Therefore, in some cases this procedure is not indicated because of esthetic considerations [55].
Conclusions
The dilemma of whether to extract a VRF tooth and replace it with an implant or to adopt a more conservative treatment planning of an additional endodontic treatment aimed to preserve the natural tooth is complex and requires a multifactorial clinical decision-making process. Extraction of the VRF tooth or root is still the treatment of choice. However, in certain cases, modern endodontics provides new treatment alternatives to treat and maintain certain VRF teeth. Additional clinical studies are indicated to shed light on the prognosis of these new treatments.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


