Categories
Characteristics
Crown-originating fracture (COF)
Spontaneous fracture originating in the crown and may progress into the root in an apical direction
Vertical root fracture (VRF)
A root-originating fracture that may originate anywhere in the root and occur primarily in endodontically treated teeth
Trauma-related fractures
Tooth fractures of acute nature may involve the crown or the root or both
Dental Fractures
The following is a scheme of categorization based on what can be observed with respect to the various dental fracture situations.
Crown-Originating Fractures (COFs)
These types of fractures typically originate in the tooth crown and are not related to root canal treatment. The fractures progress toward the root; after reaching the coronal area of the root, the fracture lines continue in an apical direction. If not treated, teeth with such fractures will eventually split vertically, or if the fracture line progresses diagonally below a cusp, that cusp may fracture off the tooth. If the cusp fracture does not create a serious periodontal problem, usually this entity can be treated with good prognosis.
Craze lines are fractures limited to the enamel only and may extend over the marginal ridges (Fig. 2.1) in molars and occur in the anterior segments as well (Fig. 2.2) [3]. They are considered benign and require no treatment except occasionally for esthetic reasons.
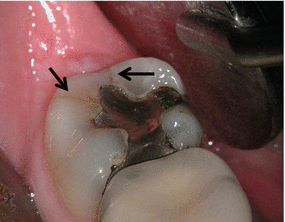
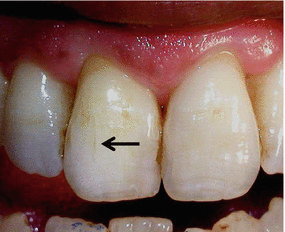

Fig. 2.1
Two craze lines in a mandibular molar. The two black arrows point at the craze lines extending from the amalgam filling to the external distal surface of the crown (Courtesy Dr R. Paul)

Fig. 2.2
A black arrow pointing at a craze line in a maxillary incisor
Some crown-originating fractures (COFs) have been identified as cracked teeth [1]; they are found in maxillary and mandibular molars and maxillary premolars. These fractures occur mostly in teeth with vital pulps and have a mesiodistal pattern. They can be observed in intact crowns or may be seen next to a carious lesion or adjacent to a small restoration. The fracture in the crown can at times extend apically to eventually separate the tooth into two parts (split tooth) [3] (Figs. 2.3, 2.4, 2.5, 2.6, 2.7, 2.8, and 2.9).
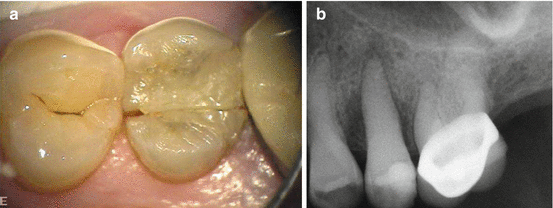
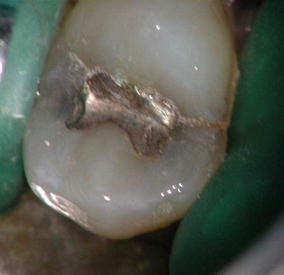
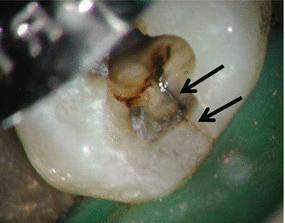
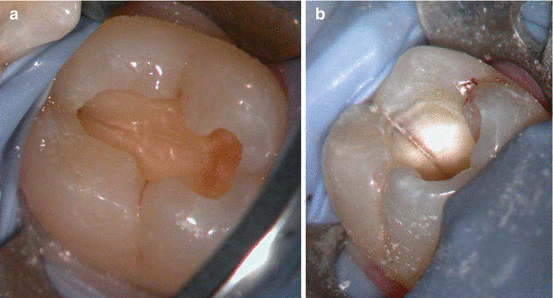
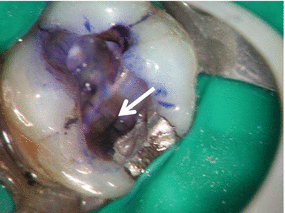

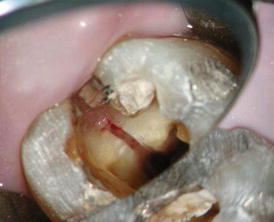

Fig. 2.3
(a, b) A mesiodistal fracture in a maxillary premolar crown. The crown was previously treated with an esthetic white restoration. The patient’s chief complaint was of “problems in brushing the teeth in this area.” (a) The pulp was diagnosed as necrotic with asymptomatic apical periodontitis. The fracture extends apically creating pockets of 6 mm in the proximal areas. Bone resorption due to the periodontal destruction can be seen mesially and distally (b) (Courtesy Dr N. Chivian)

Fig. 2.4
A diagnosis of symptomatic irreversible pulpitis was done in a patient with a class I amalgam restoration in a maxillary premolar. With the use of magnification and illumination, two fractures can be seen extending mesially and distally from the amalgam restoration

Fig. 2.5
Following local anesthetics and tooth isolation, the fracture is seen clearly (two black arrows) after removal of the restoration extending beyond the marginal ridge to the external surface (Courtesy Dr R. Paul)

Fig. 2.6
(a, b) Mesiodistal fracture in a mandibular crown seen in the roof of the pulp chamber after removal of the coronal restoration (a). At the pulp chamber level, the fracture can be seen extending to the orifices of the root canal (b) (Courtesy Dr R. Paul)

Fig. 2.7
Mesiodistal fracture can be seen at the floor of the chamber (white arrow) in mesial distal direction in a mandibular molar using methylene blue dye (Courtesy Dr R. Paul)

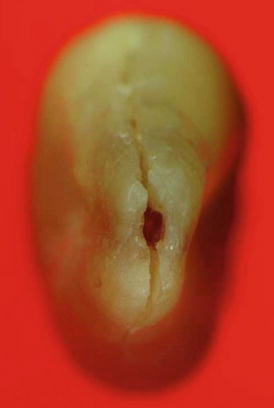
Fig. 2.8
An extracted maxillary premolar showing a VRF that originated in the crown and propagated apically (Black arrow)

Fig. 2.9
A fracture in the crown that extended apically to bifurcation area to separate a mandibular molar into two parts (Courtesy Dr. R. Paul)
Crown-originating fractures typically extend to either or both of the marginal ridges through to the proximal surfaces [3]. Very few of these crown fractures have a bucolingual direction. The fractures progress from the marginal ridges through the pulp chambers and eventually may result in a split tooth.
Fractures may be visualized in the tooth crown with transillumination or with the use of dyes absorbed into the fracture lines. The patient’s history and symptomatology may include pain in the tooth or pain referred to other oral regions increasing the diagnostic difficulty [6]. Many patients experience a vague discomfort during mastication, often with elevated sensitivity to cold.
Contributing to the diagnostic difficulty may be lack of notable caries or other reasons for pulpal disease. The patient’s symptoms may also resemble those in patients with ear aches, TMJ dysfunction, sinusitis and neurological problems [7]. The longer the symptoms are present, the more diffuse they become, and the more difficult the diagnosis becomes [6]. It may be prudent to consider the presence of COF whenever the usual suspects (caries, etc.) are absent. Correct diagnosis and identification of the actual type of fracture involved will help in developing treatment options.
Some patients do present with existing pulp necrosis with or without periapical disease as a result of long-term COF. The term fracture necrosis has been suggested for such an entity [8] (Figs. 2.10 and 2.11).
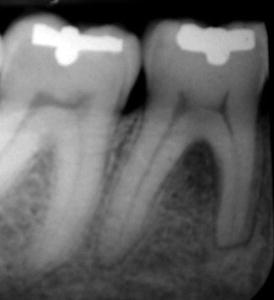
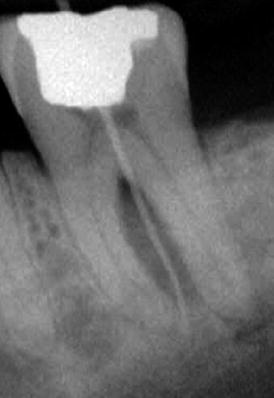

Fig. 2.10
This radiograph was taken during routine patient examination. The tooth was asymptomatic. A shallow cl I intact amalgam restoration was noted in the crown. A small fracture was seen in the occlusal surface of the crown. The pulp tested nonvital. It caused necrosis of the pulp and as a result damage to the hard tissues. External apical resorption can be seen in the mesial root and bifurcation radiolucency (Fracture Necrosis) (Courtesy Dr R. Paul)

Fig. 2.11
A patient presented to the dental office with a complaint of “suppuration of pus from the gum.” Clinical examination presented with a deep cl 1 amalgam restoration. The pulp tested nonvital, and a sinus tract was presented at the level of the apical part of the attached gingivae. A gutta-percha tracing can be seen in the radiograph all the way to the tip of the mesial root. Radiolucency between the roots can also be noted (Fracture Necrosis)
Vertical Root Fractures (VRFs)
Vertical root fracture (VRF) is a frustrating complication associated with root canal treatment in teeth and leads to their extraction [9, 10]. With a few exceptions of VRF in vital teeth [11], they primarily involve endodontically treated and restored teeth [12]; they are longitudinally oriented, thus having an apicocoronal direction. There is an overall prevalence of up to 11 % in endodontically treated teeth [13, 14]. In an incidence study done in a hospital clinic over 1 year [15], a total of 87 new cases of teeth had various types of crown and root fractures with 13 % of them VRFs in endodontically treated teeth.
A VRF can originate at any level in the root [3] although it appears that they commonly begin in the apical part. If they originate away from the apex, such as in the middle of the root, they can propagate in either direction, either apical or coronal. From the horizontal aspect, the fractures originate in the root canal wall and extend to the root surface over time and may involve either one side—buccal or lingual (incomplete)—or both sides (complete fracture) (Figs. 2.12, 2.13, and 2.14). Both in the incomplete and complete fractures, for the most part the fractures have a buccolingual pattern. Very rarely does a VRF have a mesiodistal orientation (Fig. 2.15).
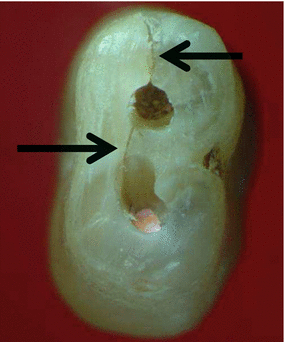
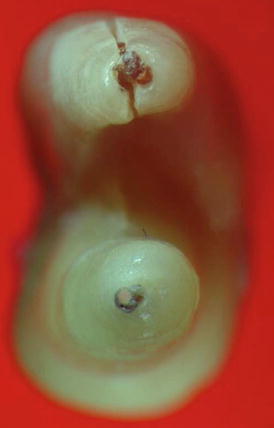

Fig. 2.12
Two black arrows are pointing at an incomplete VRF in double-canal single-rooted maxillary premolar. The fracture is not extending to the other root surface

Fig. 2.13
A complete VRF in a buccal root of a bifurcated maxillary premolar
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses