Fig. 30.1
(a–d) Schematic illustrations of the postulated maxillary displacement during rapid maxillary expansion. (a) The maxilla before expansion: the semicircles represent the right and left maxillae; the rectangles represent the pterygoid plates. (b) Posterior displacement of the maxilla after expansion by a hyrax expander: each half of the maxilla rotates outward and backward around the posterior nasal spine (PNS), which entails bone resorption behind the maxillary tuberosities and results in posterior displacement of maxilla. (c) Anterior displacement of the maxilla after expansion by a hyrax expander: each half of the maxilla rotates outward and backward around the PNS, which entails the circumaxillary structures to displace the maxilla forward and results in anterior displacement of maxilla. (d) Anterior displacement of the maxilla after expansion by a double-hinged expander: each half of the maxilla rotates outward and forward around the maxillary tuberosities, which geometrically results in anterior displacement of maxilla without the possibility of entailing bone resorption behind the maxillary tuberosities
These two assumptions explain why some of the clinical studies on hyrax-type expanders reported anterior displacement of maxilla (Haas 1970; Wertz 1970; Akkaya et al. 1999), while some others reported no significant displacement (Da Silva Filho et al. 1991; Pangrazio-Kulbersh et al. 1998) or posterior displacement of maxilla (Sarver and Johnston 1989; Cozza et al. 2001). The posterior displacement of maxilla compromises the maxillary protraction in cleft patients.
The double-hinged rapid maxillary expander (US Patent No. 6334771 B1) is developed for a greater amount of anterior displacement of maxilla (Liou and Tsai 2005; Liou and Chen 2003). Its configuration is similar to a W-appliance and has two hinges of rotation. It consists of a jackscrew in the center, two bolts holding the screw, a body holding the bolts at anterior and two hinges of rotation at posterior (Fig. 30.2a, b). The rationale for its greater amount of anterior displacement of maxilla is it expands and rotates each half of the maxilla laterally and anteriorly through the two hinges of rotation located beside the molars bilaterally. This kind of expansion entails the circumaxillary structures to displace the maxilla anteriorly with less possibility of bone resorption behind the maxillary tuberosity (Fig. 30.1d).
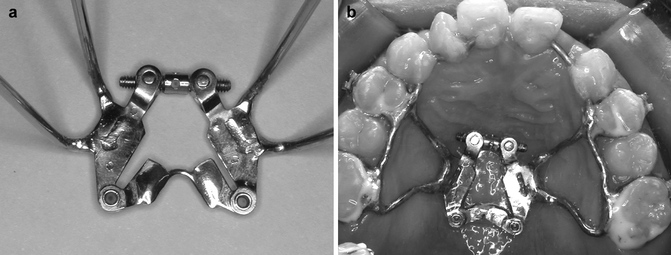

Fig. 30.2
(a, b) The configuration of the double-hinged rapid maxillary expander (a) and the assembly of the device in a clinical case (b)
Maxillary first premolars and molars are banded and maxillary impression is taken for the fabrication of the double-hinged expander. The expander is oriented perpendicular to the central incisors and is soldered to the molar and premolar bands. Two anterior extension arms (0.051-in. stainless steel wires) extend bilaterally from the premolar bands toward central incisors (Fig. 30.2b). The premolar and molar bands and the anterior extension arms are sandblasted before cementation. After cementation of the expander, the anterior extension arms are bonded to the anterior teeth with composite resin. One day after cementation, the double-hinged expander is activated according to the protocol of Alt-RAMEC.
30.2.1.2 Alternate Rapid Maxillary Expansions and Constrictions (Alt-RAMEC) of Maxilla
The Alt-RAMEC is a protocol of repetitive weekly alternate rapid maxillary expansions and constrictions (Liou and Tsai 2005; Liou and Chen 2003) (Table 30.1). It lasts for 7–9 weeks until the maxilla is loosened. The weekly (every 7 days) sequence is 7 mm of expansion, 7 mm of constriction, 7 mm of expansion, 7 mm of constriction, 7 mm of expansion, 7 mm of constriction, 7 mm of expansion, 7 mm of constriction, 7 mm of expansion, etc. Each day, the maxilla is expanded or constricted 1 mm/day (four turns in one activation). This protocol allows better disarticulation of circumaxillary sutures without overexpansion of maxilla. Its rationale is similar to simple tooth extraction in which we repeatedly rock the tooth buccally and lingually until the tooth is disarticulated out of the alveolar socket.
Table 30.1
Clinical protocol for alternate rapid maxillary expansions and constrictions
|
Alternate weekly sequence
|
Weekly amount of expansion/constriction (mm)
|
Daily amount of activation (mm)
|
|---|---|---|
|
Expansion
|
7
|
1
|
|
Constriction
|
7
|
1
|
|
Expansion
|
7
|
1
|
|
Constriction
|
7
|
1
|
|
Expansion
|
7
|
1
|
|
Constriction
|
7
|
1
|
|
Expansion
|
7
|
1
|
|
Constriction
|
7
|
1
|
|
Expansion
|
7
|
1
|
Patients are seen once a month. The maxilla is examined clinically for its loosening by holding the patient’s head with one hand and rocking the expander with maxilla up and down with another hand. The maxilla is ready for protraction only once loosening of the maxilla has been observed clinically.
30.2.1.3 Maxillary Protraction Springs for Effective Maxillary Orthopedic Protraction
The maxillary protraction device is a pair of noncompliant, tooth-borne, intraoral maxillary protraction spring (US patent 6273713 B1) (Liou and Tsai 2005; Liou and Chen 2003) (Fig. 30.3). It is a 0.036-in. b-nickel-titanium helix spring. Ball pins are used to mount the spring on the maxillary and mandibular headgear tubes. The spring is activated by the lower jaw movement. It is passive and in 180° when the mandible opens (Fig. 30.3a). While the mandible closes, it is compressed to 100–120° and generated 300–400 g of horizontal and upward force on the maxilla (Fig. 30.3b). A 0.036-in. b-nickel-titanium mandibular lingual holding arch with built-in lingual crown torque is used for splinting the mandibular dentition as an anchor unit for the protraction (Fig. 30.3c).
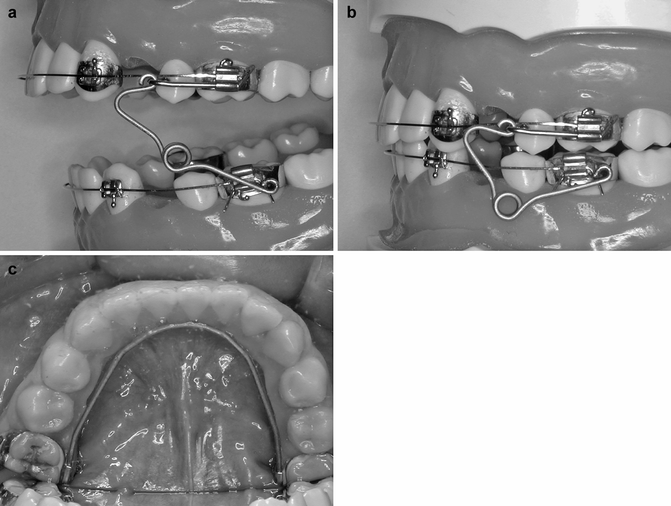

Fig. 30.3
(a–c) The intraoral maxillary protraction spring (a, b) and removable b-nickel-titanium mandibular lingual holding arch (c) for effective maxillary orthopedic protraction
30.2.1.4 Treatment Protocol for Effective Maxillary Orthopedic Protraction
The treatment protocol for effective maxillary orthopedic protraction includes 7–9 weeks of Alt-RAMEC and 4 months of maxillary protraction using intraoral maxillary protraction springs. The total treatment protocol is 6 months. The patients are seen every 4 weeks for adjusting or replacing the intraoral maxillary protraction springs when they are distorted or broken. The expander and protraction device are removed at the end of 6th month.
30.2.1.5 Treatment Results and Effects of Effective Maxillary Orthopedic Protraction
The differences between Alt-RAMEC and a single course of rapid maxillary expansion (RME) have been evaluated in a clinical cephalometric study (Liou and Tsai 2005). Twenty-six consecutive cases of unilateral cleft lip and palate patients with hypoplastic maxillae (SNA < 82) were included for maxillary protraction. Their ages ranged from 9 to 12 years old. The group of RME (7 days, 1 mm/day) was the first 16 consecutive cases. The group of Alt-RAMEC was the next ten consecutive cases. The expander used in both groups was the double-hinged expander, and the protraction appliance was the intraoral maxillary protraction springs.
The amount of maxillary anterior displacement by the double-hinged expander in the Alt-RAMEC group was 3.0 ± 0.9 mm at A point. This was significantly greater than the 1.6 ± 1.0 mm in the RME group. The amount of maxillary advancement with intraoral protraction springs in the Alt-RAMEC group was 2.9 ± 1.9 mm at A point and was significantly greater than the 0.9 ± 1.1 mm in the RME group. The overall amount of maxillary advancement in the Alt-RAMEC group was 5.8 ± 2.3 mm at A point. The clinical and cephalometric results are shown in Fig. 30.4. The protraction results remained stable without significant relapse after 2 years (5.8 ± 2.3 vs. 5.7 ± 3.0 mm).
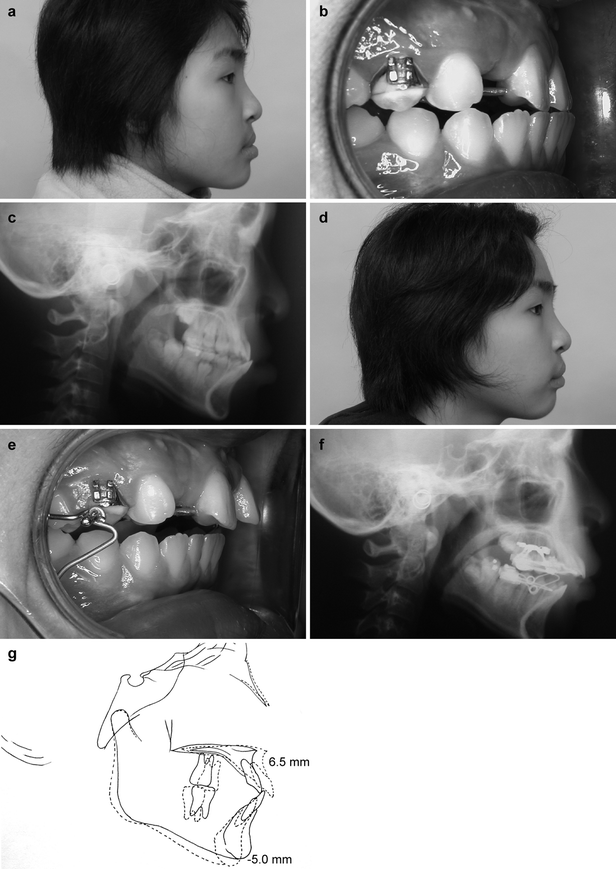

Fig. 30.4
(a–g) The clinical results of effective maxillary orthopedic protraction in a 12-year-old bilateral cleft patient. The treatment was 9 weeks of Alt-RAMEC, 1 month of active maxillary protraction, and 3 months of maintenance. The amount of maxillary protraction at A point was 6.5 mm and the mandible rotated downward and backward for 5 mm. (a–c) The lateral facial profile, occlusion, and cephalogram before treatment. (d–f) The lateral facial profile, occlusion, and cephalogram after treatment. (g) Cephalometric superimposition before and after treatment
The protocol of Alt-RAMEC displaces the maxilla anteriorly twice and facilitates maxillary protraction three times better than a single course of RME. This indirectly proves that the protocol of Alt-RAMEC disarticulates circumaxillary sutures better than a single course of rapid maxillary expansion. Because the circumaxillary sutures are protracted three times faster than usual, the protraction results could be an orthopedic process of “sutural protraction osteogenesis,” which is similar but less vigorous than sutural expansion distraction osteogenesis. The maxillary protraction by using the double-hinged expander, repetitive weekly protocol of Alt-RAMEC, and the intraoral protraction springs is effective with stable results at 2 year follow-up.
To obtain good stability, our clinical experience revealed that the timing for effective maxillary orthopedic protraction is around the onset of puberty (age 11–13). Early treatment is not recommended because of the unpredictable mandibular growth. The onset of puberty could be evaluated by using vertebral bone age on cephalogram (Mito et al. 2003; Franchi et al. 2000).
30.3 Orthopedic Management of a Downward Displaced Premaxilla in Bilateral Cleft Patients
In growing bilateral cleft patients, one of the most common premaxillary deformities is a prominent and downward displaced premaxilla with or without wide alveolar clefts (Fig. 30.5a). The vertical discrepancy between the premaxilla and buccal segments results in an unaesthetic “equine appearance,” anterior deep overbite, and also makes the alveolar bone grafting difficult or impossible (Hayward 1983).
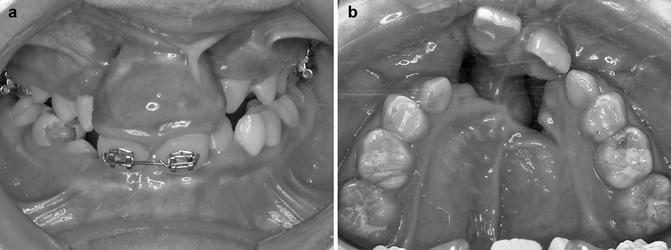

Fig. 30.5
(a, b) Two of the most common premaxillary deformities in bilateral cleft lip and palate. (a) A prominent and downward displaced premaxilla with or without wide alveolar clefts. (b) A laterally displaced premaxilla with a wide alveolar cleft on one side
In a cephalometric study, Liou et al. inferred that the downward displaced premaxilla is not because of overgrowth of the premaxilla or overeruption of the maxillary incisors (Liou et al. 2004). The premaxilla might have been downward distorted in the early age of life after the primary surgical repairs. Several studies indicated that the prominence of premaxilla becomes less pronounced during the growth period and gradually resolves into the adulthood (Pruzansky 1955; Harvold 1961; Narula and Ross 1970; Friede and Pruzansky 1972; Vargervik 1983; Trotman and Ross 1993). It is recommended that the premaxillary deformities be left untreated until adulthood (Friede and Pruzansky 1985). However, to leave the deformities unsolved until adulthood may complicate the alveolar bone grafting and impact the young patients psychosocially.
The contemporary surgical interventions of the downward displaced premaxilla in bilateral cleft patients include removal of the primary maxillary incisors in order to improve the appearance and temporarily reduce the dentoalveolar prominence (Vargervik 1983), and surgical reposition of the premaxilla in conjunction with alveolar bone grafting (Harvold 1961; Freihofer et al. 1991; Bardach et al. 1992; Heidbuchel et al. 1993; Iino et al. 1998). However, the premaxilla in the growing subjects having surgical repositioning grows at a very low rate and becomes retrusive progressively in the older age (Vargervik 1983; Smahel 1984).
30.3.1 Premaxillary Orthopedic Intrusion
A better treatment modality, therefore, is to reposition the premaxilla and approximate the alveolar cleft nonsurgically and orthopedically so that the growth of premaxilla would not be disturbed and the alveolar bone graft could be performed successfully. A new nonsurgical technique called premaxillary orthopedic intrusion has been developed for correcting the downward displaced premaxilla in growing patients with bilateral cleft (Liou and Chen 2003; Liou et al. 2004).
30.3.1.1 Orthodontic Preparation
Before initiating orthopedic intrusion of premaxilla, the maxillary incisors are well aligned orthodontically so that a segment of 0.016 by 0.022 stainless steel arch wire can be placed. The maxillary first permanent molars or the second primary molars are banded, and the band is welded with an orthodontic triple tube. The triple tubes are for holding the orthopedic intrusion device. A fan-type rapid maxillary expander, if necessary, could be placed for repositioning the collapsed buccal segments. A transpalatal arch and/or a segment of stainless steel arch wire (0.016 by 0.022) are placed on the buccal teeth for consolidating the buccal segments as an anchor unit for the orthopedic intrusion of premaxilla.
30.3.1.2 Device for Premaxillary Orthopedic Intrusion
No headgear, extraoral device, or surgery is used for the intrusion. The device for orthopedic intrusion of the downward displaced premaxilla is a pair of tooth-borne distraction devices (Fig. 30.6a). The device anchors on the maxillary buccal teeth and delivers an intermittent intrusion force to the premaxilla through the maxillary incisors. The U-shaped connector of the device is inserted into the headgear tube on the molar band and secured with a 0.012-in. ligature wire. The extension arm of the device is secured with 0.012-in. ligature wires onto the segmental arch wire on the central incisors (Fig. 30.6b–e).
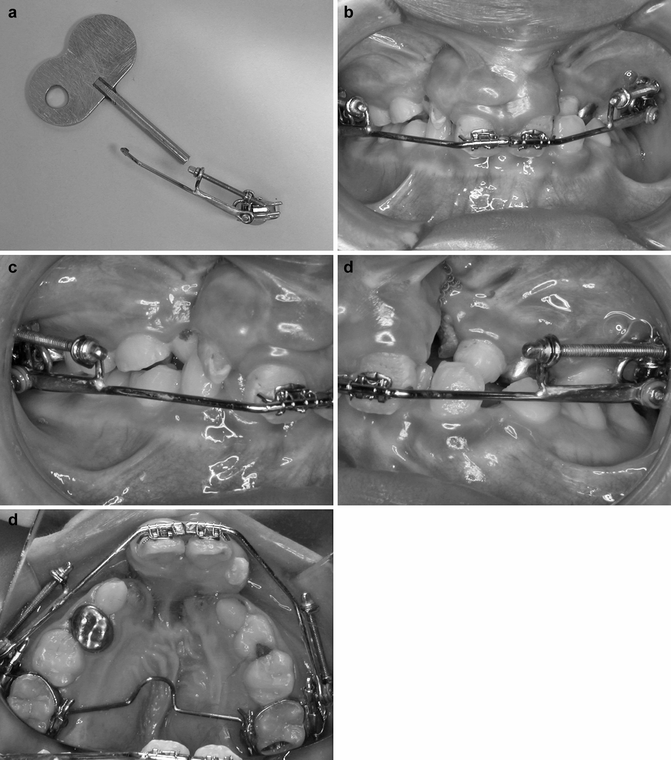

Fig. 30.6
(a–e) The device for premaxillary orthopedic intrusion (a) and the assembly of the device in a clinical case (b–e)
On both sides, the devices are activated 0.3 mm/day until the premaxilla has been upward repositioned to the desired position. The devices are then maintained for another 3 months before their removal. After removal of the intrusion devices, an orthodontic arch wire is placed for further maintenance, and alveolar bone grafting is then performed within 3 months.
30.3.1.3 Treatment Results of Premaxillary Orthopedic Intrusion
The treatment results have been evaluated in a cephalometric study on ten consecutive cases (Liou et al. 2004). The orthopedic intrusion of premaxilla was completed within 4 weeks in all the patients. After the intrusion, the occlusal planes and gingival lines of the premaxilla and buccal segments were leveled clinically. The facial appearance during resting and smiling improved and had no “equine appearance.” The clinical results are shown in Fig. 30.7.
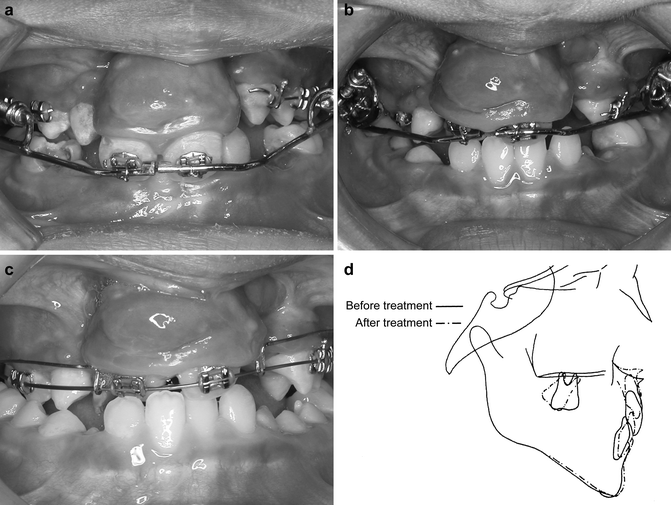

Fig. 30.7
(a–d) The premaxillary orthopedic intrusion. The equine appearance of the premaxilla prior treatment (a), after 1 month of orthopedic intrusion (b), 5 months after the orthopedic intrusion (c), and cephalometric superimposition before and after premaxillary orthopedic intrusion (d)
The cephalometric study revealed that there was no significant vertical movement of the maxillary buccal segments, and the premaxilla was significantly intruded (Fig. 30.7d). The nasal bone was also significantly brought forward and upward at the nasal tip, but its amount was significantly less than the orthopedic intrusion of the premaxilla.
The correction of the premaxillary deformity mainly came from three aspects: orthopedic intrusion of the premaxilla, dental intrusion of the maxillary incisors, and shortening of the premaxillary dentoalveolar height. The orthopedic intrusion of the premaxilla (3.0 mm) and dental intrusion of the maxillary incisors (3.5 mm) gave a total amount of 6.5 mm upward repositioning at the tip of the maxillary incisor. The shortening of the premaxillary dentoalveolar height (3.5 mm) could be due to the dental intrusion of the maxillary incisors, which was expected when a tooth-borne distraction device was used. The correction was 46 % (3.0/6.5) orthopedic effect and 54 % (3.0/6.5) dentoalveolar effect.
The orthopedic intrusion of the premaxilla remains relatively stable in the 1-year observation after treatment. However, the dental intrusion of maxillary incisors seems unstable. The dental relapse of the maxillary incisors tends to elongate the premaxillary dentoalveolar height and compromise the result of premaxillary orthopedic intrusion. For this reason, it is recommended to maintain the dental intrusion with an orthodontic arch wire and perform alveolar bone grafting shortly after removal of the intrusion devices (Fig. 30.7c).
30.3.1.4 Mechanisms of Premaxillary Orthopedic Intrusion
The possible events that may occur during orthopedic intrusion of premaxilla include mechanical upward displacement of the premaxilla and vomeronasal septum complex, sutural contraction osteogenesis (Castello et al. 2000) and/or osteolysis (Kawakami et al. 1996) in the vomero-premaxillary suture, or bending/remodeling of the vomeronasal septum complex:
1.
Mechanical upward displacement without bending/remodeling of the vomeronasal septum complex and no sutural contraction osteogenesis/osteolysis in the vomero-premaxillary suture
2.
Sutural contraction osteogenesis/osteolysis in the vomero-premaxillary suture without bending/remodeling/mechanical upward displacement of the vomeronasal septum complex
3.
Bending/remodeling without mechanical upward displacement of the vomeronasal septum complex and no sutural contraction osteogenesis/osteolysis in the vomero-premaxillary suture
4.
Any combinations of 1, 2, or 3
By the analysis on the lateral and posteroanterior cephalometric radiographs, it was implied what occurred during the orthopedic intrusion of premaxilla was mostly similar to the sutural contraction osteogenesis/osteolysis in the vomero-premaxillary suture combined with slightly mechanical upward displacement of the vomeronasal septum complex and nasal bones (Fig. 30.8).
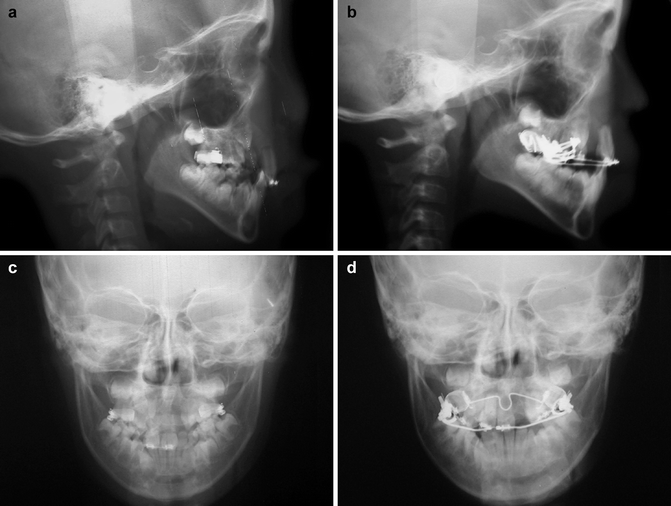

Fig. 30.8
(a–d) The cephalometric radiograms of the same patient in Fig. 30.7. (a, b) The lateral cephalogram before and after premaxillary orthopedic intrusion. (c, d) The posteroanterior cephalogram before and after premaxillary orthopedic intrusion. Note the premaxilla and incisors were intruded without further deviation of the vomer bone and nasal septum
30.4 Orthopedic Management of a Laterally Displaced Premaxilla in Bilateral Cleft Patients
In growing bilateral cleft patients, another common premaxillary deformity is a laterally displaced premaxilla with a wide alveolar cleft on one side (Fig. 30.5b). The laterally displaced premaxilla results in an unaesthetic appearance with a skewed premaxilla and dental midline and uneven width of the alveolar cleft beside the premaxilla.
The alveolar bone grafting and closure of oronasal fistula could be difficult without surgical repositioning the laterally displaced premaxilla. However, the premaxilla in growing subjects having surgical repositioning grows at a very low rate and becomes retrusive progressively as they age (Vargervik 1983; Smahel 1984).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


