, Y. Natalie Jeong1, Robert J. Rudy1 and Daniel K. Coleman1
(1)
Department of Periodontology, Tufts University School of Dental Medicine, Boston, MA, USA
8.1 Introduction
The accumulation of bacterial plaque, food debris, and eventually calculus on the non-shedding surfaces of the human dentition has long been recognized, since the time of Pierre Fauchard in the eighteenth century, as the most fundamental factor responsible for the initiation of dental caries and periodontal diseases. This quintessential insight, recognized by so many astute clinicians, should not be ignored when treating patients with periodontal diseases. Whether the therapy is for gingivitis, periodontitis, pericoronitis, acute necrotizing ulcerative gingivitis (ANUG), peri-implant mucositis, or peri-implantitis, the individual patient’s level of cooperation in the therapy is crucial for achieving immediate and long-term successful results. Patients need to be empowered so they can reverse the ravages of neglect and move forward towards the new direction of clinical health and comfort. The decision for this change in direction must come from the individual patient, but dental health professionals must be willing to accept their responsibility to guide and motivate each patient.
“The known methods whereby dentists can prevent periodontal disease are more effective than those available for any other chronic affliction of the human body even more effective than caries preventive measures. But they are not widely used.For no other chronic disease are there such effective uncomplicated patient administered preventive procedures. But judging from the high incidence of periodontal disease they are hardly used. Either the public has not been sufficiently educated regarding what they can do for themselves or they are disinterested and satisfied to unnecessarily sacrifice their teeth to preventable disease.Neglect is a principal cause of gingival and periodontal disease; neglect of the healthy mouth permits disease to occur; neglect of early disease which permits the disease to destroy supporting tissues and neglect of the treated mouth which permits disease to occur.”—Irving Glickman (1967)
8.1.1 The Maintenance Therapy Program
After a period of healing, regardless of whether periodontal health is reestablished with phase I therapy services alone or with additional phase II surgical services as needed, all patients need to be assigned to a maintenance therapy program. The purpose of the maintenance therapy program is to provide a structured environment where patients’ oral health needs are addressed with appropriate therapeutic interventions.
The maintenance therapy program should be characterized by a proactive staff, dedicated to the following common goals:
(a)
Preventing the recurrence of dental diseases and mucosal lesions
(b)
Identifying new lesions in their incipient state
(c)
Ensuring a positive relationship between the specialist’s office and the referring general dentist’s office
(d)
Establishing clear communication channels between the patient and both offices
(e)
Advocating for the patient, when insurance carriers require further clarification as to why maintenance therapy services are necessary and justified
8.2 Getting Started
In general, the idea of risk assessment can be employed to help in determining the time interval between maintenance therapy visits. Immediately following phase I active therapy, all patients are considered to be at high risk for recurrence of disease; therefore, the interval should be short, between 2 and 3 months. This should continue for 1–2 years. Following 5–6 visits, the caries risk and periodontal disease risk can be reassessed, and a new interval can be established. The traditional 6-month interval should no longer be relied upon to address the needs of each individual patient. In addition, these visits should be scheduled in a mutually agreed-upon alternating pattern between the referring general dentist and the periodontist.
8.2.1 High-Risk Patients
Specific conditions that predispose the patient to periodontitis and increased risk of root caries require a shorter interval (8–10 weeks) and additional vigilance. Examples of high-risk patients might include the following:
-
Diabetic patients
-
Smokers
-
Pregnant patients
-
Sjogren’s patients
-
Head and neck cancer patients
-
Patients who take medications that compromise salivary flow
-
Patients who carry polymorphism of interleukin-1 genotype
8.3 Treatment Principles Regarding the Prevention of Gingivitis and Periodontitis
The two major responsibilities that must be addressed by patients:
1.
They must be willing to maintain excellent personal plaque control at home.
2.
They must be willing to cooperate and return to the dental office setting on a regular basis for maintenance therapy evaluation and preventive services.
The two major responsibilities that must be addressed by clinicians:
1.
They must remain involved in periodically motivating the patient in lifestyle changes that enhance oral hygiene standards.
2.
They must remain alert and diligent in their efforts to identify incipient disease and provide the necessary therapeutic interventions.
The three main etiologic factors responsible for gingivitis:
(a)
The patient’s inability to control the accumulation of bacterial plaque
(b)
The clinician’s deficiency in providing a meaningful educational experience for patients regarding plaque control measures, and therefore not empowering patients to prevent disease
(c)
Iatrogenic causes: loose or open contacts leading to food impaction, overhanging restorative margins, bulky restorative cervical contours, and violation of the biologic width
The three main principles regarding preventative dentistry:
(a)
Educate and empower patients.
(b)
Remove all etiologic factors that elicit inflammation.
(c)
Motivate patients to be cooperative and follow professional guidance and recommendations.
The three main reasons for treating gingivitis and periodontitis:
(a)
Reduce or eliminate symptoms of disease.
(b)
Reduce or eliminate risk of periodontitis and consequent attachment loss.
(c)
Reduce or eliminate bacterial and cytokine seeding into the general circulation and possible systemic consequences.
Success in treating gingivitis and periodontitis:
Success in treating gingivitis and periodontitis will be realized ONLY if the clinician strives to thoroughly manage or correct all of the etiologic factors:
(a)
Help improve plaque control by motivational counseling of the patient, which includes the review of brushing and flossing techniques.
(b)
Debride plaque and calculus from tooth surfaces.
(c)
Close all loose or open contacts if possible.
(d)
Remove all restorative overhangs and reduce bulky cervical contours.
(e)
Resolve all biologic width violation situations.
8.4 Basic Features of a Structured Maintenance Therapy Program
“Both maintenance therapy and primary active therapy must be introduced conceptually at the same time to the patient. All patients must be advised against the folly of relying on short-term gains (via active primary treatment and brief periods of improved plaque control) when long term retention of the teeth in function (via extended professional recall treatment and extended personal plaque control) is the only sensible goal.Successful long-term maintenance after treatment is more than anything else, an attitude of mind, both of the therapist and the patient. We all realize that a short-term therapeutic improvement, essential though it is, can be only a beginning. By itself, it means little. Ahead is the far more elusive goal of preserving the dentition in a state of health for the longest possible time. To attain this goal, the therapist must generate resolve within the patient, and this resolve must stem from an even firmer resolve within himself.”—Alfred L. Ogilvie, DDS, MSProfessor of Oral Medicine University of British Columbia, 1977
The maintenance therapy program is a proactive program that aims at preventing occurrence of new dental disease (caries and periodontal disease) and recurrence of previously treated dental disease. The objectives of the maintenance therapy appointment are essentially threefold in nature:
1.
Complete assessment of the present conditions and then compare with past records—does the new data suggest stability of attachment levels or not?
2.
Review motivational needs of each patient as they pertain to helping them sustain their dedication to high standards of plaque control.
3.
Make further recommendations that are essential to promoting dental and periodontal health.
8.4.1 Guidelines for Evaluation: What Are the Key Signs to Look for in Early Disease?
(a)
Are there gingival erythema and gingival enlargement?
(b)
Is there bleeding upon gentle probing?
(c)
Are there any new pocket (gingival or periodontal) depths?
(d)
Are older, previously noted, pocket depths becoming deeper?
(e)
Is there evidence of advancing attachment loss?
(f)
Is the advancing attachment loss generalized or localized?
(g)
Are root surfaces smooth and free of caries and calculus deposits?
(h)
Are tooth mobilities increasing?
Once the dental therapist is sensitized to the above signs of early disease, the actual maintenance therapy appointment should proceed smoothly and more expeditiously.
8.5 The Maintenance Therapy Appointment: The Basic Protocol
1.
Review medical history and update as necessary: for example, list all new medications, dosages, and reasons for taking such; list any recent hospitalizations and reasons for such; take a new blood pressure reading and record; determine level of diabetic control; determine status of smoking cessation efforts; and determine if any new medications are reducing salivary flow or if they have the potential to cause gingival enlargement.
2.
Complete the extraoral and intraoral examination for pathology of skin, lymph nodes, and oral mucosa.
3.
Perform periodontal examination and rechart findings.
(a)
Assess mobility, probing depths, bleeding upon gentle probing, color, size, consistency, and position of the gingival margin.
(b)
Evaluate occlusal relations; determine if there is fremitus or evidence of bruxism. Determine if there is evidence of increasing mobility patterns.
(c)
State the new periodontal diagnosis.
(d)
Assess stability of attachment levels.
(e)
Outline any new recommendations that will foster periodontal health, including a referral to a periodontal specialist.
4.
Perform a restorative examination and rechart findings.
(a)
Assess old restorations for breakage, open margins, open contacts, or biologic width violations.
(b)
Assess caries risk activity—use magnification and transillumination to detect new lesions.
(c)
Outline any new recommendations that will foster a zero caries rate (activity).
5.
Determine need for new radiographic imaging.
6.
Disclose the patient to determine plaque levels and use a plaque-free scoring system (Fig. 8.1).
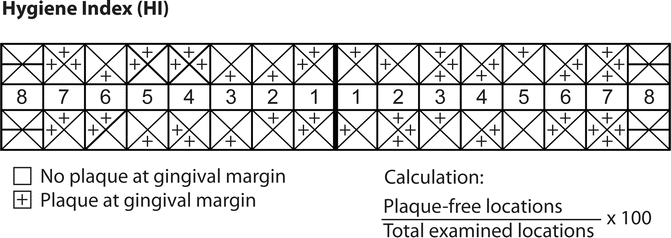

Fig. 8.1
Hygiene index
7.
Review oral hygiene methods—by allowing the patient to demonstrate their brushing and flossing techniques. Determine level of ability and actively re-instruct patient as necessary.
8.
Perform any necessary therapy such as: dental prophylaxis and root planing as needed, topical application of fluoride, or desensitizing agents and rescheduling patient for restorative procedures.
9.
Enter personal notes about patient that are deemed important or significant.
10.
Determine whether the interval length between maintenance therapy appointments is correct or requires adjustment.
Basic armamentarium for the maintenance therapy visit:
(a)
Examination instruments
(b)
Paper or digital copy of the maintenance therapy “Basic Protocol”
(c)
Preventive dentistry supplies for demonstration purposes (timing device, patient mirror, disclosing agents, brushes, interproximal aides, rubber tip)
(d)
Treatment instruments
(e)
Topical fluoride agents
(f)
Articulating paper or ribbon to evaluate the occlusion
8.6 Implant Maintenance
During maintenance therapy, dental providers are seeing an growing number of patients with implant-supported prostheses, and this trend is only going to increase because more dentists are offering implant therapies and more patients are keen to accept implant therapy rather than a conventional fixed partial denture or a removable partial denture. Routine maintenance therapy is crucial for preserving a patient’s peri-implant health.
8.6.1 Anatomy of a Dental Implant and its Supporting Prosthesis (Fig. 8.2)
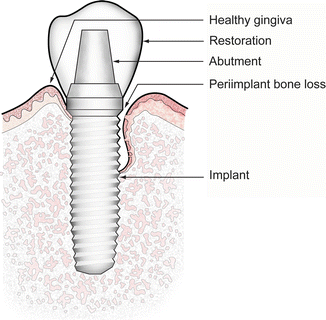
Fig. 8.2
Left side of figure represents implant health. Right side of figure depicts peri-implantitis
How does the attachment apparatus around implants differ from that of natural teeth?
-
Lack of a periodontal ligament
-
Circular gingival fibers around implants as opposed to perpendicular gingival fibers around teeth
-
Intimate contact between bone and implant surface
8.6.2 Evaluation of Implant Health
8.6.2.1 Parameters
-
Presence of plaque and/or calculus
-
Appearance of the peri-implant tissue; signs of inflammation such as bleeding or purulent exudate
-
Radiographic appearance
-
Probing depths
-
Patient comfort
-
Maintenance/re-care interval
The peri-implant soft tissue should be visually examined for signs of inflammation such as erythema, bleeding, swelling, and suppuration. If an infection or inflammation is present, the clinician will have to develop a treatment plan. The treatment plan may include nonsurgical therapy, antibiotics, shortening re-care intervals, or a referral for evaluation by a specialist.
The protocol for probing dental implants was in the past controversial; however, the consensus is that it is not only safe but is essential in order to evaluate peri-implant health.
The gingival attachment to implants is weaker than that of natural teeth, as there is no connective tissue attachment. The Junctional epithelium attaches to the implant surface via a glycocalyx secreted through hemidesmosomes, and the gingival fibers of the connective tissue, do not insert into the implant. Collagen fiber bundles originate from the bone and run vertically and parallel to the implant surfaces. Clinicians could inadvertently probe beyond this weak attachment and break the seal; hence, the probing depth reading may be exaggerated and subsequently interpreted as peri-implant disease. An experienced clinician should be able to probe dental implants without continual perforation of the epithelial attachment.
When interpreting a probing depth around an implant, implant positioning in the coronoapical dimension should be taken into consideration. To create an adequate emergence profile, implant fixtures are often placed slightly deeper than that of the location of the cementoenamel junction of a clinical crown, especially in the maxillary anterior region. Therefore, interproximal probing depth as deep as 6 mm may be observed if the proximal crestal bone levels of the adjacent teeth are more coronal than the implant platform.
This deeper probing depth reading does not indicate peri-implant tissue pathology unless:
1.
There is bleeding upon probing or suppuration.
2.
There is increased probing depth over time.
3.
There is radiographic evidence of bone loss compared to the baseline radiographic image.
Some have argued against using metallic probes, concerned that the metallic probes might scratch and damage the implant surface. However, the probe tip does not touch the implant surface—only the abutment surface in most cases. Thus, the surface alteration is minimal. A conventional metallic periodontal probe and a plastic periodontal probe are equally effective, though some practitioners prefer a plastic probe because it is more flexible (Fig. 8.3).


Fig. 8.3
Plastic and metal periodontal probes
Inflammation around an implant is a critical factor that determines whether intervention will be required. Although many etiological factors exist, one of the most common causes of inflammation around dental implants is excess cement that was not removed during crown cementation. Excessive subgingival cement remaining after cementation leads to a foreign body reaction that causes pathologic soft tissue inflammation and bone loss. In addition, the surface topography of the dental implant may provide a favorable environment for bacterial attachment. Accessing the subgingival space of the implant restoration nonsurgically because of implant positioning and subsequent suprastructure design could be challenging. Moreover, many commonly used types of dental cement are not detectable in radiographs. Meticulous attempts to remove excess cement must be practiced.
Another source of peri-implant inflammation is ill-fitting suprastructures. A loose abutment or screw may contribute to the accumulation of plaque, which may then lead to peri-implant inflammation.
8.6.2.2 Signs of a Healthy Implant
-
Surrounded by tissue that is firm and of normal color with no evidence of erythema, edema, bleeding, or suppuration.
-
The implant fixture should be non-movable.
-
No bone loss beyond crestal bone remodeling. Clinicians have established that most bone remodeling around healthy implants occurs during the early healing phase and is then followed by stabilization of the bone during the years in function. Documenting baseline bone levels after implant placement and after insertion of the prosthesis is important.
8.6.2.3 Diagnosis of Peri-implant Diseases
-
Peri-implant mucositis: a disease in which the presence of inflammation is confined to the soft tissue surrounding a dental implant with no signs of supporting bone loss following the initial bone remodeling that occurs during healing. Peri-implant mucositis may be identified clinically by erythema and bleeding upon probing and/or suppuration (Fig. 8.4).
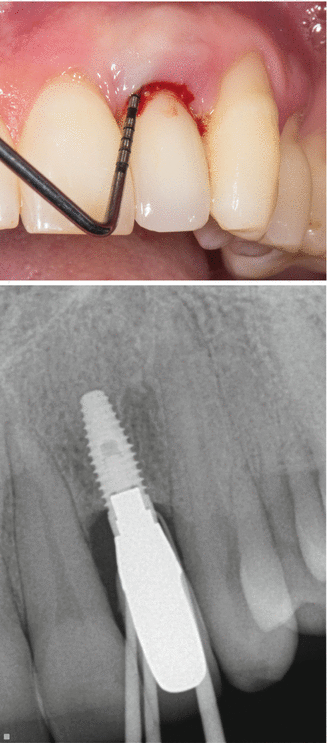 Fig. 8.4Peri-implant mucositis
Fig. 8.4Peri-implant mucositis -
Peri-implantitis: an inflammatory process around an implant that exhibits both soft tissue inflammation and progressive loss of bone beyond the initial bone remodeling (Fig. 8.5).
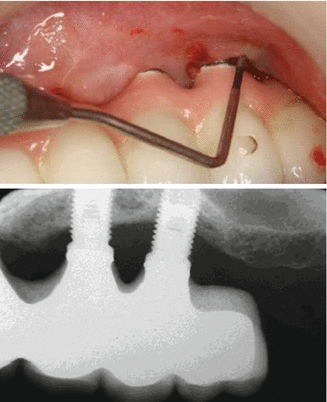 Fig. 8.5Peri-implantitis
Fig. 8.5Peri-implantitis
8.6.3 Instrumentation of Dental Implants
We are still in the early stages of investigating factors that could be responsible for peri-implant diseases. No one standardized method of implant maintenance has been identified. However, the importance of an adequate maintenance therapy for implant survival has not been disputed. The main objective when the clinician is instrumenting the dental implant prosthesis is to eliminate the bacterial microfilm by removing both hard and soft tissue deposits.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


