, Y. Natalie Jeong1, Robert J. Rudy1 and Daniel K. Coleman1
(1)
Department of Periodontology, Tufts University School of Dental Medicine, Boston, MA, USA
7.1 Pharmacotherapeutics
7.1.1 Introduction
The first line of treatment for periodontal disease is the removal of pathogenic bacteria and plaque, which is done by mechanical scaling and root planning along with a meticulous home-care regimen. However, adding adjunctive systemic or locally delivered antimicrobial therapy should be considered. Pharmacotherapeutics should be used as an adjunctive therapy to conventional periodontal treatment, not as a substitute to conventional mechanical debridement.
7.1.2 Systemic Antibiotics
7.1.2.1 When Are Antibiotics Employed?
In 2004, the American Academy of Periodontology published a position paper regarding the use of systemic antimicrobial therapy in the management of chronic and aggressive periodontal disease. This position paper suggested that systemic antimicrobial therapy might be prescribed as an adjunct to both surgical and nonsurgical therapy to those patients who do not respond adequately to mechanical therapy or manifest acute periodontal infections. Systemic antibiotic therapy may be utilized as a prophylaxis for medically compromised patients as well.
7.1.2.2 What Antibiotics Are Commonly Used?
It is prudent to choose an antibiotic that demonstrates a broad spectrum of activity because a variety of potential pathogens (Gram-negative anaerobes, facultative anaerobes, Gram-positive anaerobic cocci and rods) are associated with periodontal disease. Patients’ medical conditions and potential drug interactions need to be reviewed carefully prior to making choices about appropriate medications, doses, and duration of administration. A consultation with the patients’ medical providers might be necessary.
The most common systemic antibiotics prescribed in the treatment of periodontal disease include the following:
-
Amoxicillin
-
Metronidazole
-
Clindamycin
-
Tetracycline
-
Azithromycin
-
Ciprofloxacin
Amoxicillin/Metronidazole
-
250 mg/tid/8 days of each drug
Amoxicillin is a broad-spectrum semisynthetic antibiotic that has a bactericidal activity against many Gram-positive and Gram-negative microorganisms. Metronidazole is a nitroimidazole antibiotic medication used particularly for anaerobic bacteria and protozoans.
An effective clinical result is often achieved by using a combination of amoxicillin and metronidazole. The combined mechanical and systemic antibiotic therapy is more effective than mechanical therapy alone in terms of improvement of clinical and microbiological features of periodontal disease.
Clindamycin
-
300 mg/tid/8 days
Clindamycin is a lincosamide antibiotic used to treat infections with anaerobic bacteria. It is utilized as an alternative antibiotic when a patient presents with a penicillin allergy. The most severe common adverse effect of clindamycin is Clostridium difficile-associated pseudomembranous colitis. Although this side effect occurs with several other antibiotics such as beta-lactam antibiotics, it is classically linked to clindamycin use.
Tetracycline/Minocycline/Doxycycline
-
Tetracycline 250 mg/tid or qid/21 days
-
Doxycycline 100–200 mg/qd/21 days
-
Minocycline 100–200 mg/qd/21 days
Tetracyclines incorporate a family of medications that are broad-spectrum antibiotics that act by inhibiting protein synthesis. Photosensitivity is a known side effect of this antibiotic. Tetracyclines achieve a much higher concentration in crevicular fluid relative to their serum levels.
Azithromycin
-
500 mg/qd/4–7 days
Azithromycin is a subclass of macrolide antibiotics. It prevents bacteria from growing by interfering with protein synthesis.
Ciprofloxacin
-
500 mg/bid/8 days
Ciprofloxacin is a second-generation fluoroquinolone antibiotic. This broad-spectrum antibiotic works through the disruption of DNA synthesis.
7.1.3 Local Delivery Antibiotic Therapy
7.1.3.1 What Are the Indications?
-
Local sites with inflammation that have not responded to conventional therapy
-
Local sites with recurrent signs of inflammation at a periodontal maintenance appointment
7.1.3.2 Available Local Delivery Antibiotics (Fig. 7.1)
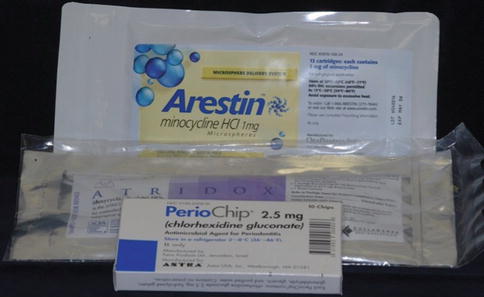
Fig. 7.1
Local delivery antibiotics
-
Arestin ™—Minocycline in a resorbable bead vehicle
-
Atridox ™—Doxycycline in a resorbable polylactide gel
-
PerioChip ®—Chlorhexidine in a resorbable gelatin wafer
7.1.3.3 Subantimicrobial Dose Doxycycline (SDD)
-
Periostat ®—20 mg doxycycline, bid x 9 months
Collagenases are a subgroup of the matrix metalloproteinase family of enzymes. Periostat® is a systemically delivered collagenase inhibitor consisting of subantimicrobial dose (20 mg) of doxycycline. This drug has been approved by the FDA for host modulation as an adjunct to scaling and root planing in the treatment of periodontitis.
7.1.3.4 Oral Rinses
A mouth rinse must not only reduce plaque but also have a therapeutic effect. Currently, long-term, 6-month studies support only the use of mouth rinses containing 0.12 chlorhexidine gluconate or certain essential oils including the phenolic compounds thymol, menthol, eucalyptol, and methyl salicylate to reduce plaque and gingivitis.
Chlorhexidine 0.12% Oral Rinse
0.12% chlorhexidine gluconate is used as a mouth rinse ½ oz twice daily for 30 seconds. In the United States it is obtained by a prescription.
Chlorhexidine-containing mouth rinses can cause extrinsic staining of the teeth with prolonged use. Patients should be informed that any stain may be removed through prophylaxis (Fig. 7.2).


Fig. 7.2
Chlorhexidine gluconate mouth rinse
Nonprescription-Based Oral Rinses
A number of essential oils including the phenolic compounds thymol, menthol, eucalyptol, or methyl salicylate-containing oral rinses are also available for over-the-counter use (Fig. 7.3).


Fig. 7.3
Essential oil mouthwash
7.1.4 Conclusions
Clinicians should consider many factors when they contemplate the use of adjunctive antimicrobial therapies in the management of periodontal disease. The development of resistant bacteria from repeated exposure to antibiotics, the side effects from antibiotics, and the interactions between antibiotics and other medications all should be carefully reviewed. When employed appropriately, adjunctive therapy can enhance the outcome of conventional mechanical therapy in treating periodontal diseases. It is the responsibility of the clinicians to determine the indications for use and to select the appropriate antibiotic for each patient.
7.2 The Importance of Smoking Cessation
7.2.1 Introduction
Given that 52 % of the patients with periodontitis are current or past cigarette smokers and that 90 % of refractory periodontitis is seen in habitual smokers, it behooves the dental profession to address smoking cessation in any treatment plan that is presented to this patient population.
Tobacco was initially used in Ecuador and Peru by the shaman doctor/priests as an analgesic and antiseptic and was placed on teeth to help relieve toothaches. In the 1500s, European physicians Jean Nicot and Nicolas Monardes incorporated the use of tobacco into their medical practices and claimed to cure bad breath, toothaches, and cancer. Ironically, most of these ailments were caused by tobacco use, but the use of tobacco for medicinal purposes spread across Europe as did its recreational use.
With the introduction of mass-produced cigarettes, the prevalence of cigarette use has soared, and in 2014, one billion people smoked worldwide, and this use was responsible for six million deaths, 600,000 of which were related to second-hand smoke exposure. In addition to cigarette smoking, there has been an increase in cigar use by children and young adults who have been attracted to inexpensive, small, flavored products. Despite the decline in pipe usage, the use of hookahs has increased. Other smokeless products, such as SNUS (moist powdered tobacco developed in Sweden), and chewing tobacco, Orbs, Strips, and Sticks (compressed tobacco) are also contributing to nicotine addiction. All of these products are harmful and increase the risks of diseases, so dental health-care providers must be diligent in addressing this problem.
7.2.2 The Systemic Impact of Tobacco Use
As dental professionals review the medical and dental histories of their patients, it becomes apparent that their tobacco-addicted patients have a host of acute and/or chronic diseases that are related to tobacco usage. It is imperative that the clinician understand the nature of these illnesses as they will impact their treatment plans. It is also crucial that they maintain a dialog with their patients’ physicians as to understanding their present medical status, as well as be part of a health-care team that can coordinate an effective tobacco cessation approach to their nicotine-addicted patients.
As discussed, there are many chronic diseases that patients present with due to their smoking tobacco products. These include:
1.
Stroke
2.
Diabetes
3.
Blindness and cataracts
4.
Periodontitis
5.
Aortic aneurysm
6.
Coronary heart disease
7.
Pneumonia
8.
Atheroslerotic peripheral vascular disease
9.
Chronic obstructive pulmonary disease
10.
Asthma and other respiratory ailments
11.
Hip fractures
12.
Reproductive effects in women
Most people assume that smoking can cause lung and bronchus cancer, but many other cancers are associated with smoking as well.
Cancers include:
1.
Oropharynx and oral cavity are seen in smoking but also in the use of smokeless tobacco as well.
2.
Larynx.
3.
Esophagus.
4.
Stomach.
5.
Pancreas.
6.
Kidney and ureter.
7.
Cervix and bladder.
The gravest oral consequence of smoking use is oral cancer, and it has been shown that 75 % of oral cancer patients smoke and have a heavy alcohol intake. Given that oral health is primarily the responsibility of dental professionals, counseling patients in smoking cessation is an important part of their treatment plan.
As disconcerting as second-hand smokes’ impact on adults is, its impact on infants and children is even more so. Second-hand smoke increases the frequency and severity of asthmatic attacks, respiratory infections, ear infections, and sudden infant death syndrome. In addition, women smoking while they are pregnant results in tens of thousands of infant deaths annually worldwide.
7.2.3 The Dental Implications of Tobacco Use
Tobacco use has been implicated in:
1.
Dental caries
2.
Periodontal diseases
3.
Leukoplakia
4.
Oral and pharyngeal cancer
5.
Cleft lip and palate formation
6.
Nicotinic stomatitis
7.
Dental implant failure
Some of the oral effects of smoking are in part related to:
1.
Decreased salivary flow and decreased pH of saliva.
2.
Reduced salivary buffering capacity affecting the microbiota.
3.
Favorable environment for the growth of periodontal pathogens.
4.
Reduced the IgG2 antibodies lowering the immune system.
5.
Reduced phagocytosis affecting wound healing.
6.
Altered the functionality of the gingival microvasculature masking inflammation.
7.
Nicotine causes an abnormal growth of fibroblasts needed for collagen synthesis.
8.
Suppressed proliferation of osteoblasts.
Fifty-two percent of patients with periodontitis are current or past cigarette smokers and 90 % of recurrent periodontitis is seen in habitual smokers. It has been shown that patients who currently use tobacco products show decreased pocket reduction, less gain in clinical attachment, reduced bone regeneration, and lower percentages of root coverage as compared to control subjects. Smoking also negatively affects the short and long-term success of dental implants.
Given the negative implications of tobacco use and wound healing, this should give pause to the periodontist recommending phase II surgical therapy. In other words nonsurgical therapy may be the most prudent course of action, while the patient is working their way thru the smoking cessation program that is described later.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


