, Y. Natalie Jeong1, Robert J. Rudy1 and Daniel K. Coleman1
(1)
Department of Periodontology, Tufts University School of Dental Medicine, Boston, MA, USA
1.1 Introduction
A healthy periodontium is essential for the long-term survival of the dentition and for successful restorative dentistry. To maintain periodontal health requires a recognition and understanding of the multiple factors that contribute to the etiology of periodontal disease progression. Most dental and dental implant diseases are plaque induced and, therefore, are infections. Plaque, or microbial biofilm, is a sticky secretion comprised of bacterial cells in a polysaccharide media, which is attached to the teeth and other non-shedding surfaces by a glycocalyx (Fig. 1.1). This biofilm can be toxic to the teeth and the surrounding soft and hard tissues. Intraorally, it is responsible for dental caries, gingivitis, periodontitis, peri-implant mucositis, and peri-implantitis (Fig. 1.1a–c). Additionally, host susceptibility (host response) to the toxins in dental plaque plays a significant role in the degree of periodontal inflammation and its progression. The body’s immune response mediates the inflammation and always must be taken into consideration when diagnosing and treating periodontal inflammation.
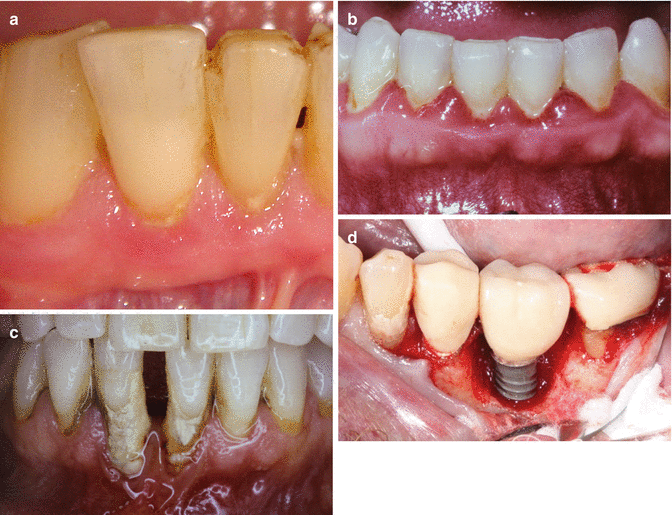

Fig. 1.1
(a) The presence of plaque is not easily identified by the patient. Note the soft tissue erythema associated with biofilm accumulation. (b) Generalized severe gingivitis. (c) Generalized severe periodontitis. Note attachment loss. (d) Peri-implant bone loss
Plaque/biofilm accumulates on teeth daily in quantities that have the potential for creating gingival inflammation. Dental plaque must be removed to ensure freedom from periodontal diseases, peri-implant diseases, and dental caries. Mechanical removal is especially necessary due to the protective interactions between the tooth surface and subjacent bacteria, which resist the effects of antimicrobial agents, such as mouthwashes. Without mechanical removal the bacteria’s secretions or toxins remain on the tooth and are responsible for the development of gingival inflammation and the acidic demineralization of teeth. For susceptible individuals, these toxins must be removed daily. For less susceptible individuals who are periodontally healthy, it has been shown that the removal of dental plaque every 24–48 h can successfully prevent clinical signs of gingivitis. From daily mechanical removal to more in-depth preventative care, the maintenance of periodontal health is the shared responsibility between the patient and the clinician.
1.2 Anatomy (Fig. 1.2a, b)
1.2.1 Gingival Anatomy with Respect to Periodontal Diseases or Deformation
(a)
The gingiva, which along with the soft tissue covering the hard palate is known as masticatory mucosa and is comprised of the marginal gingiva and the attached gingiva. The epithelial surface of the gingiva is keratinized on the facial or buccal surfaces from the crest of the marginal gingiva to the mucogingival junction. The sulcular surface of the gingiva is nonkeratinized. The keratinized epithelium helps to protect the gingiva from disruption of the cells, trauma, as a result of toothbrush bristles or during the mastication of abrasive foods.
(b)
Marginal gingiva or “free” gingiva is that portion of the gingiva, which is not attached to the tooth and comprises the boundary of the gingival sulcus/pocket. The measurement with a periodontal probe from the crest of the gingival margin to the most superior part of the epithelial attachment is known as the clinical probing depth (PD) and measures the marginal or free gingiva.
(c)
The attached gingiva is measured from the most coronal aspect of the epithelial attachment to the crest of the alveolar bone and is comprised of the epithelial attachment and the connective tissue attachment (Fig. 1.2a). This is also called the attachment apparatus. Structurally the epithelial attachment consists of the internal basal lamina, which is comprised of hemidesmosomes that connect the junctional epithelium to the tooth surface by way of a transudate of mucopolysaccharide glycocalyx (laminin and other glucoproteins). Thus, the actual attachment is the glycocalyx. The connective tissue attachment primarily consists of type I collagen fibers of which there are five types: dentogingival, alveologingival, dentoperiosteal, circular, and transseptal. It is the attached gingiva and specifically the connective tissue, which supports the gingiva and helps prevent attachment loss and recession from trauma during mastication and brushing. It is important to recognize that the dentogingival, the dentoperiosteal, and the transseptal fibers are embedded into the cementum. This attachment helps to provide resistance from mechanical stress, which can be caused by brushing or during mastication of abrasive foods. The cementum is comprised of acellular, located at the cementoenamel junction to the midportion of the root and cellular, located at the apical third of the root. The alveolar bone supports the tooth and also helps prevent recession due to trauma. It is comprised of cortical bone, cancellous bone, and alveolar bone proper, which lines the tooth socket (dental alveolus). This bone is also known as bundle bone, as the fibers from the periodontal ligament are embedded into it. The periodontal ligament, which is comprised of type I collagen fibers, blood vessels, and nerves serves to anchor the tooth to the alveolar bone proper, to transmit occlusal forces to the bone, and to supply cells for bone, fiber, and cementum remodeling and formation. Its innervation acts as a protective warning system for occlusal overload.
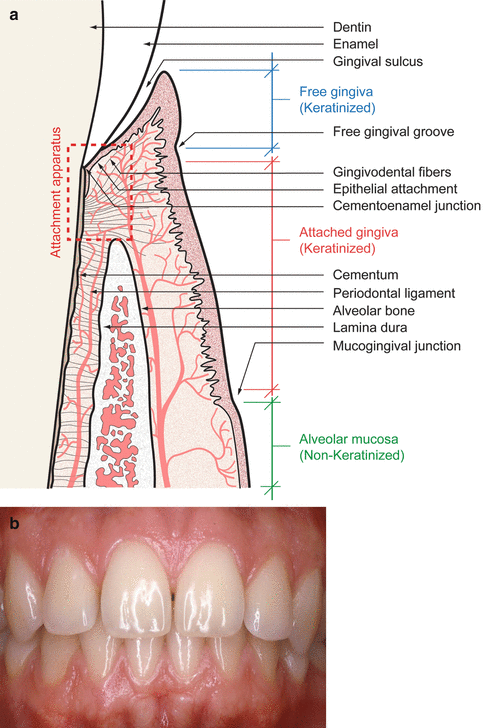

Fig. 1.2
(a) Diagram of gingival attachment anatomy. (b) Clinical periodontal health
(d)
The normal marginal gingival architecture is scalloped, which means that the interproximal gingiva fills or almost fills the interproximal space, and the cervical crest of the marginal gingiva is apical to the crest of the interproximal gingiva. This is called “positive architecture.” Interdentally from a buccal-lingual or facial-lingual perspective, the shape of the gingiva is described as a “col” or valley-like depression formed by the facial and lingual papillae. “Flat” architecture is when the most superior height of the interproximal gingiva is at the same level as the cervical gingiva. In this case, the papilla is often described as “blunted.” “Negative” architecture is when the cervical crest of the marginal gingiva is superior to the interproximal gingiva, which is often seen in conjunction with or following acute ulcerative necrotizing gingivitis/periodontitis (ANUG/NUP). The description of negative gingival architecture is often called “cratered.” Pronounced scalloped gingiva is sometimes seen normally with individuals with long papillae, which fill the embrasure space. Additionally, a pronounced scalloped gingiva may also be seen in the case of gingival recession. When there is an insufficient width of attached gingiva, even correct brushing techniques might cause recession (Fig. 1.3).
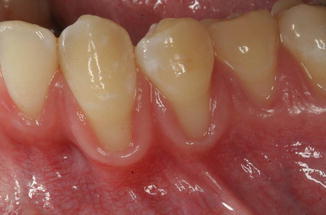

Fig. 1.3
Scalloped gingiva is often seen with a thin biotype
(e)
The width of attached gingiva may play a significant role in helping to prevent recession. The epithelial attachment acts as a seal to the oral fluids and bacteria. The connective tissue attachment is comprised of primarily type I collagen with some type III. Collectively they are known as the attachment apparatus. Their function is to hold the marginal gingiva against the tooth providing it with sufficient rigidity, which will withstand the forces of mastication and correct brushing techniques without distorting. Also it stabilizes the marginal gingiva by uniting it with both the tissue of the relatively rigid attached gingiva as well as the cementum layer of the tooth (Fig. 1.4).
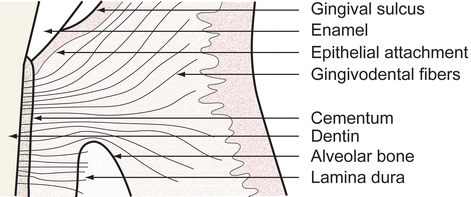

Fig. 1.4
The connective tissue fibers and the epithelial attachment hold the gingiva to the tooth
(f)
A patient with a thin periodontal biotype, which means a minimal zone of attached gingiva and thin facial alveolar bone often with fenestrations and dehiscences, is subject to gingival recession even with adequate brushing techniques and is very likely to show gingival recession with a scrub technique of brushing (Fig. 1.5a). A fenestration (window) is where the root protrudes through the thin bone; however, there is bone surrounding the protrusion, and a dehiscence is where the protrusion of the root through the bone is contiguous with more coronal aspect of the tooth (Fig. 1.5b).
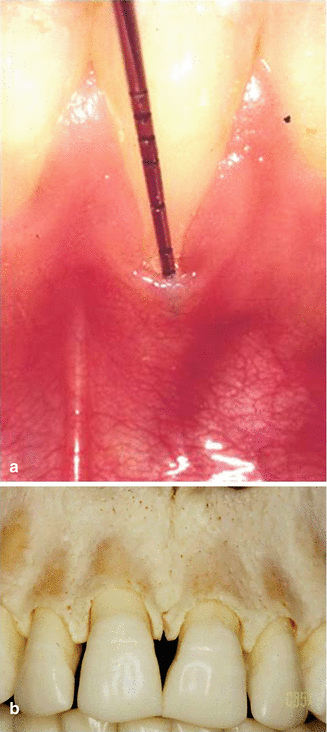

Fig. 1.5
(a) With a thin biotype, the gingiva can be entirely missing. (b) A thin biotype can show bony dehiscences and fenestrations
1.2.2 Gingival and Tooth Anatomy with Respect to Professional Hygiene Therapy
(a)
The therapeutic goal of professional hygiene therapy is for the clinician to completely remove accretions, plaque, calculus, and stain from the tooth surfaces. From this view point, the clinician assists the patient to achieve gingival and periodontal health. The clinician’s goal for mechanical root/tooth debridement is to achieve a plaque and calculus-free surface, which is smooth to the feel of an explorer. The depth of the gingival crevice often plays a significant role in the clinician’s ability to achieve this goal. There are pockets where the base is above the crest of the bone (suprabony)(Fig. 1.6) and pockets that extend below the crest of the bone (infrabony) (Fig. 1.7). Research has shown that with gingival crevices/pockets ≥5 mm, it is unpredictable that complete professional hygiene can be achieved subgingivally.
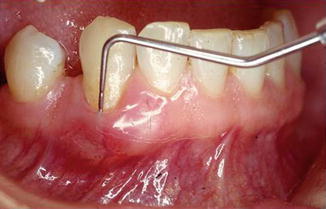
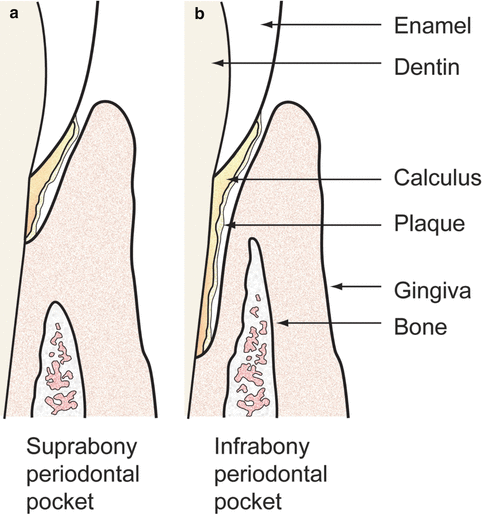

Fig. 1.6
Deep pockets on the facial of single-rooted teeth can indicate a dehiscence and a suprabony pocket

Fig. 1.7
Left diagram, suprabony pocket; right diagram, infrabony pocket
(b)
Gingival biotypes are classified as thick and thin. According to Dr. Arnold Weisgold, the thin biotype has a less wide zone of attached gingiva measured from the crest coronoapically than a thick biotype. Additionally, the bone underneath the gingiva in a thin biotype will also be thin measured faciolingually and many times exhibit dehiscences or fenestrations (Fig. 1.5b). The patient with a thin biotype will respond to gingival inflammation with recession, whereas gingival inflammation in the thick biotype patient tends to create periodontal pockets. Generally a person with a thin biotype will exhibit a triangular crown and a significantly tapered root, while an individual with a thick biotype will show a more square-shaped crown, and the root will not be as tapered as with a thin biotype. Biotypes can be created also by tooth position during tooth eruption especially in a crowded dentition or due to pathological migration. Also orthodontic tooth movement in a facial position can develop a thin biotype for a single tooth or group of teeth. Generally, the widest gingiva is found associated with the maxillary incisors, with the narrowest gingiva associated with the facial of the mandibular 1st premolars (Fig.1.8a–c).
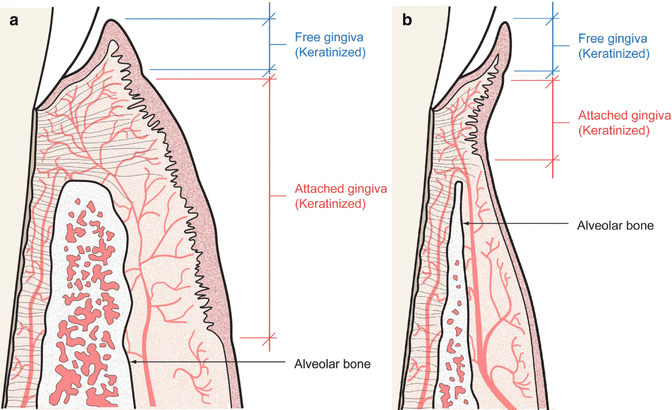
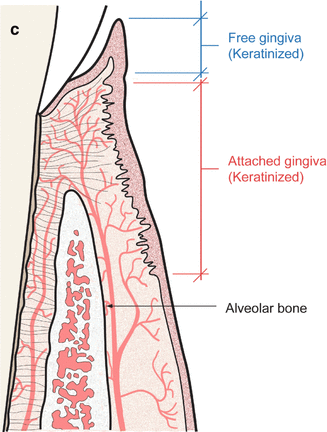


Fig. 1.8
(a) A thick biotype is often seen with square teeth, thick gingiva, and thick surrounding alveolar bone. (b) A thin biotype often shows triangular-shaped teeth and gingival recession as a result of insufficient attached gingiva. (c) Average biotype
(c)
The attachment apparatus consists of the epithelial attachment and the connective tissue attachment. The average coronoapical width of the attachment apparatus is 2.04 mm as described by Gargiulo. It has been shown to range between .75 and 4.3 mm, and thus a patient with rough root surfaces, which require subgingival root planing and a short or weak attachment apparatus, has a greater chance of additional attachment loss with scaling and root planing than a patient with a thick biotype and a normal width of attached gingiva (Fig. 1.9).
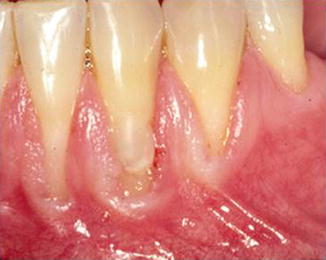

Fig. 1.9
Scaling and root planing with a thin biotype must be very precise to prevent creating further recession
(d)
Thorough root debridement for a patient with a thin biotype could cause additional attachment loss and increased recession by dislodging a weak connective tissue attachment if the attachment is from alveolar mucosa. In deep periodontal pockets of ≥4 mm with attachment loss and a wide zone of gingiva, the concern for permanent attachment loss with scaling and root planing is less than with a thin biotype, as the goal is to reduce the pocket to provide the patient access to clean the tooth subgingivally as well as to attempt reattachment, new attachment, or even perhaps regeneration, all of which might be achieved with comprehensive scaling and root planing. In a patient with shallow pockets, especially in the aesthetic zone, recession is undesirable and in some instances can be avoided. Thus, extreme care must be taken by the clinician to not disturb the connective tissue attachment, which means utilizing sharp, thin instruments and a solid dry finger rest to provide the greatest control of the blade of the curette possible when root planing.
(e)
Tooth anatomy also plays a major role in the completeness of subgingival professional hygiene therapy. Furcation attachment loss and root concavities including developmental grooves or enamel projections and pearls substantially reduce the operator’s ability to thoroughly clean the teeth and create smooth root surfaces (Fig. 1.10a–d).
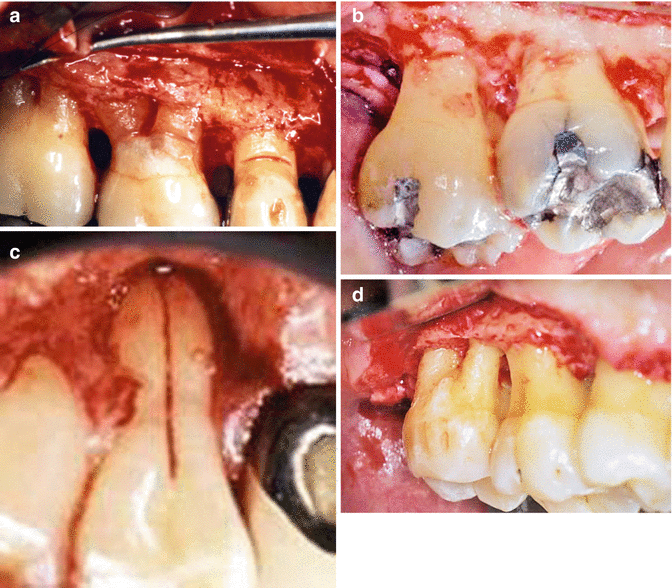

Fig. 1.10
(a) A narrow furcation involvement creates difficulty in root planing especially with hand curettes. (b) Root concavities and the interproximal concavity coronal to a furcation inhibit plaque removal with dental floss and allows for difficulty in calculus removal with hand and ultrasonic instrumentation. (c) Palatal grooves enhance plaque accumulation, provide a surface for calculus collection, and make it difficult to clean. (d) Enamel projections allow for pocketing into the furcation and are many times responsible for furcation involvements
1.2.3 Gingival and Tooth Anatomy with Respect to Patient Hygiene Therapy
(a)
The external surface of the gingiva is keratinized; however, just because of the keratinized surface, it is not more resistant to inflammation caused by the toxins of bacterial plaque than nonkeratinized epithelium. The keratinized surface of the gingival epithelium is generally less sensitive to the toothbrush bristles than is the alveolar mucosa, and thus a patient is more likely to remove biofilm from the tooth at the tooth-soft tissue interface with an intrasulcular technique of brushing with the presence of a wide dimension of gingiva than when the interface consists of is primarily nonkeratinized alveolar mucosa.
(b)
To help prevent gingivitis and periodontitis, the gingival crevice/sulcus must be accessible by dental floss or toothbrush bristles in order to dislodge the biofilm formed by bacterial cells and attached to the tooth. Thus, the deeper the probing depth, the less likely that a patient will be able to remove the biofilm and the more likely that they will exhibit gingival inflammation. Gingival hyperplasia or incomplete passive eruption, without attachment loss, can create pockets that are inaccessible for mechanical plaque removal by the patient (Fig. 1.11).
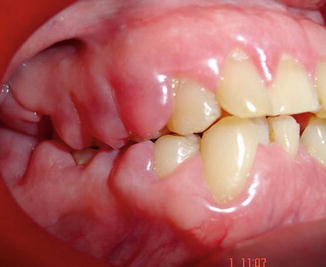

Fig. 1.11
Severe gingival overgrowth
(c)
In general, it is accepted that 3 mm or less gingival crevices are considered normal and cleansable; however, a 3 mm facial or lingual pocket is difficult or impossible to access by the toothbrush bristles and can lead to gingival inflammation (Fig. 1.12a). Access by toothbrush bristles or by dental floss/tape depends on the gingival architecture. Interproximal sulci of ≤3 mm might not be cleansable in the situation of flat or negative interproximal tissue architecture (Fig. 1.12b). Conversely interproximal sulci of ≥4 mm might be very accessible for plaque removal with dental floss in the anterior sextant for a patient with a thin biotype, triangular teeth, positive gingival architecture, and long papillae (Fig. 1.12c).
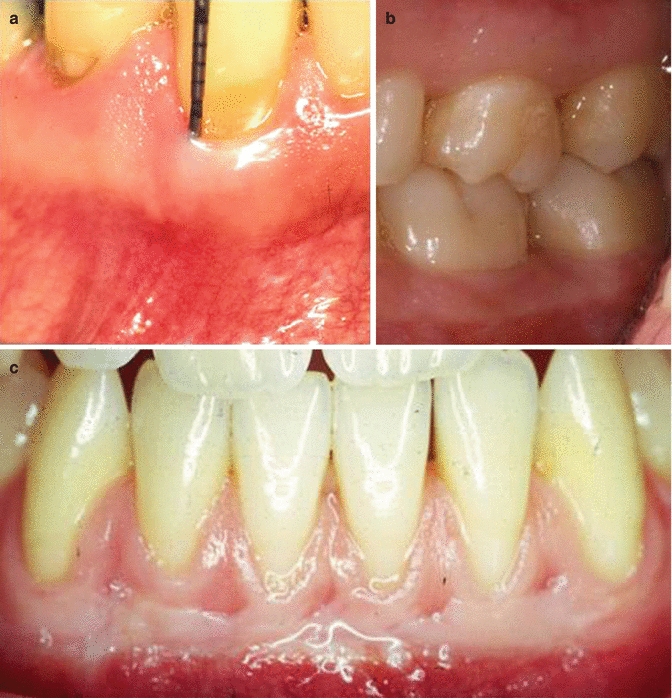

Fig. 1.12
(a) A 3 mm facial pocket can be difficult to access by toothbrush bristles. (b) Posterior teeth have short interproximal papilla or flat architecture, and a 3 mm interproximal gingival crevice can be difficult to clean. (c) Long papillae might have a 4 or 5 mm crevice, which can be accessed for plaque removal using dental floss/tape
(d)
The gingival biotype also plays a role in the technique that is taught to patients. An intrasulcular technique of brushing is generally advocated for the removal of biofilm at and to a degree beneath the gingival sulcus; however, in the case of a thin biotype with a minimal (≤1 mm zone of attached gingiva, a non-intrasulcular technique of brushing (Stillman’s) might be preferable to lessen the chance of gingival recession (see Chap. 3).
(e)
As the width of the attached gingiva varies within the mouth, it is sometimes necessary for a patient to use an intrasulcular technique of brushing in certain areas of their mouth and a non-intrasulcular technique in others.
1.2.4 Summary
The tooth, the periodontium, and the gingival anatomy play an essential role in periodontal disease control therapy by the patient and by the clinician. A clinician’s understanding of dental and periodontal anatomy and its function to support a tooth in health, and their understanding of how to help patients to prevent damage by bacterial plaque or physical trauma is of paramount importance in providing the patient with optimal therapy. Knowledge of the significance of the attachment apparatus and its physiologic function with respect to the tooth as a supportive mechanism helping to control the invasion of microorganisms and also serving to control gingival recession is of key importance. The clinician’s awareness of the gingival anatomy affords the opportunity to know the appropriate plaque control techniques to teach the patient and where to apply them. Additionally, the therapist must know gingival anatomy in order to apply the most effective mechanical techniques to use in order to thoroughly debride the teeth and roots. The following chapters will describe patient plaque control techniques and the techniques and instruments that the clinician can use for thorough tooth/root debridement.
1.3 Periodontal Examination
In order to have an in-depth understanding of the patient’s periodontal and dental anatomy and dental, soft tissue, and periodontal pathology, prior to arriving at a diagnosis and developing a plan of therapy, a comprehensive examination is essential. The integral parts of a periodontal examination include:
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


