Fig. 15.1
Average facial shape in adult patients with unilateral complete cleft lip and palate compared with a non-cleft sample (Courtesy of Dr. E. Dahl, University of Copenhagen)
The pattern of growth is different from that in non-cleft individuals. Semb (1991a) found only a small increase between 5 and 18 years of age in the length of the maxilla measured to the anterior outline of the alveolar process in a mixed longitudinal study of 257 subjects with complete UCLP. There was a concomitant reduction in maxillary prominence at the dentoalveolar level, as seen in Fig. 15.2. The excessive lower face angulation changed little over time in the UCLP sample (approximately 3° greater than the Bolton standards at age 5 years), whereas it was reduced by 5° in the non-cleft sample. The gradual reduction of maxillary prominence over time and increased lower face height has also been described in several long-term studies (Enemark et al. 1990; Paulin and Thilander 1991; Smahel et al. 1993; Friede and Enemark 2001; Brattström et al. 2005; Nollet et al. 2008; Meazzini et al. 2008; Friede et al. 2011).
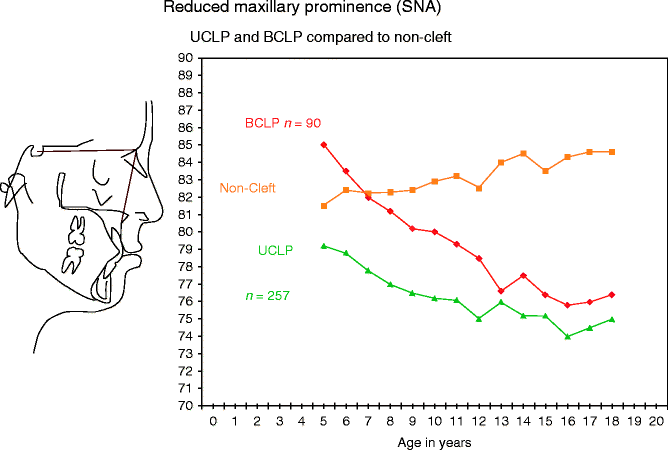

Fig. 15.2
Changes in maxillary prominence (SNA) for 257 patients with complete unilateral cleft lip and palate (UCLP) and 90 patients with complete bilateral cleft lip and palate (BCLP) compared with a non-cleft sample
15.1.2 BCLP
A mixed longitudinal study of 90 patients with complete BCLP from 5 to 18 years (Semb 1991b) found the maxilla in BCLP to be relatively prominent in early childhood (4° more prominent at 5 years), but it steadily receded so that by 7 years, it was similar to the value for non-cleft subjects (Broadbent et al. 1975) and by 18 years, it was 6° less (see Fig. 15.2). Throughout the period of observation, the mandible was less prominent (4° less at 5 years and 6° less at 18 years). Vertically, lower facial angulation remained higher in BCLP (2° at 5 years and 9° at 18 years). Similar findings have been reported (Heidbüchel et al. 1994; Gnoinski and Rutz 2009).
Thus, the growth pattern is different between UCLP and BCLP groups in one obvious respect. In comparison with UCLP patients, subjects with BCLP displayed greater maxillary prominence in early childhood (SNA was 5.3° larger at 5 years), but this difference reduced with time so that by 18 years, the maxilla was only slightly (1.4°) more prominent on average. In other respects, facial growth patterns were similar in both conditions, although the gonial angle was somewhat greater (3°) in BCLP throughout the period of observation.
15.1.3 Late Deterioration
Impairment of maxillary development continues into the late teens and early adulthood while mandibular growth continues (Enemark et al. 1990; Paulin and Thilander 1991; Semb 1991a, b; Friede and Enemark 2001; Brattström et al. 2005; Gnoinski and Rutz 2009; Myklebust et al. 2009; Friede et al. 2011; Semb et al. 2011). Thus, the anteroposterior jaw relationship worsens over time and with it the occlusion.
Since there are few publications of longitudinal follow-up beyond age 20, it is not possible to say when this growth differential ends. Enemark et al. (1990) followed 57 patients with UCLP from birth to 21 years of age. The cephalometric study showed that from 16 to 21 years, the maxillary prominence reduced by 1.1° while the mandibular prominence increased by 1.0°. The same was found in a longitudinal cephalometric study of 60 patients with UCLP from Oslo studied at 16, 18 and 21 years of age (Myklebust et al. 2009). Maxillary prominence (SNA) is reduced by 0.3° from 16 to 18 years and by 0.3° from 18 to 21 years; maxillary length (condylion to A-point) is increased by 0.6 mm from 16 to 18 years and by 0.5 mm from 18 to 21, while the mandibular length is increased by 2.3 mm from 16 to 18 years and with 1.1 mm from 18 to 21 years. A deterioration of the occlusion in the late teens/early adulthood has been reported by Lilja et al. (2006), Marcusson and Paulin (2004), and Semb et al. (2011).
15.2 Intrinsic Facial Differences Not Attributable to Surgery
It would be surprising if the catastrophic events leading to failed union of the facial processes were not associated with dysmorphology beyond the cleft site. Some indication of the extent to which the variations in facial form in UCLP and BCLP described above are intrinsic can be obtained by comparing individuals with unrepaired clefts and normal controls.
On anteroposterior cephalograms, increased width of various facial parts in unoperated infants with UCLP and BCLP has been found (Hermann et al. 2000, 2004). On lateral cephalograms, the maxilla in the UCLP group was smaller, though more protrusive at the alveolar level and at the level of the anterior nasal spine in the male subjects. The mandible was also smaller, the gonial angle was increased, the mandibular plane was steeper and the lower incisors were retroclined in the UCLP group. There was a reduced posterior height and a tendency towards increased anterior lower facial height. These differences in mandibular shape were more marked in females. The nose was less protruded, but as a result of the maxillary protrusion, there was an increase in profile convexity (Capelozza et al. 1993; Mars and Houston 1990). Differences likely to be intrinsic in nature also include abnormalities in the size and form of the cranial base (although the literature is contradictory on this point). One consistent finding is the smaller craniofacial dimensions (including size of the maxilla) found in both unoperated and operated individuals with UCLP and BCLP compared with non-cleft subjects, though this may relate to a smaller overall stature in individuals with clefts (Jensen et al. 1983).
Evidence that the prominence of the cleft maxilla is similar to that of the non-cleft is a key issue in the debate concerning surgical iatrogenesis. Therefore, it is noteworthy that the comparisons between individuals without cleft and individuals with unoperated cleft have revealed similar anterior projection of the basal maxilla on the greater segment (Capelozza et al. 1993; Mars and Houston 1990), and the same is true preoperatively for infants with complete clefts compared to infants with cleft lip and alveolus (Hermann et al. 2000, 2004).
A variety of reports including twin and fetal studies point to intrinsically reduced nasal airway volume in individuals with clefts, repaired or not. This in turn may contribute the mandibular abnormalities that are observed (Semb and Shaw 1996).
15.2.1 Individuality of Patients
Lastly, it must remembered that children, whether or not they have clefts, tend to resemble their parents and that inheritance, especially with regard to Class II or Class III predisposition, will be an influential background factor in post-surgical facial development. Furthermore, each child entering the operating room will have other inherited traits that may impact on healing and recovery and on a wide range of later development. This individuality is a key factor in explaining the wide variability of outcome demonstrated by any study cohort and the consequent need for adequate sample size in research. As Pruzansky observed, “Within certain defined limits, the success or failure of the surgical procedure depends more on the initial state than on the variables inherent in the manoeuvre. To put it another way, we expect that subtle differences among patients will be more prognostic of the subsequent state than differences between surgeons” Nordin (1957).
15.3 Surgical Iatrogenesis
Surgery has a great impact on maxillary growth that becomes progressively apparent as patients reach maturity with reduced prominence of the maxilla at the basal (anterior nasal spine) and dentoalveolar (A point) level (Liao and Mars 2005a, b). The mandibular growth pattern is unaffected by the surgical repair of complete clefts (da Silva et al. 1992).
It is conceivable that patients with a significant deficiency of tissue are most at risk for post-operative maxillary distortion and restraint. However, the specific cause of growth disturbance remains unclear, but lip closure as well as palate closure has been implicated (Ross and Johnston 1972; Mars and Houston 1990; Normando et al. 1992).
It is possible that the iatrogenic effects of lip closure may have been underestimated. Experimental animal studies have reported that increased pressure from the repaired cleft lip is the primary cause of maxillary growth restraint (Bardach et al. 1984a). Lip pressure in infants with UCLP has been measured after lip repair and until 2 years of age and found to be significantly higher than in a non-cleft control group. Furthermore, follow-up of partially operated human subjects with complete UCLP and BCLP where only the lip has been repaired, in comparison to individuals with both lip and palate repair, points to the significant role of lip closure. Indeed, increased lip pressure probably continues to mould the anterior dentoalveolar region and reduce the SNA angle into adulthood.
Two studies have focused on this question on relatively large samples of subjects with UCLP (Mars and Houston 1990; Capelozza et al. 1996). The length of the maxilla (Ar-ANS) was reduced after lip surgery by 6.3 and 4.0 mm, respectively, in the Sri Lankan and Brazilian lip-only samples, an effect that appears to be largely due to moulding of the anterior alveolus (Liao and Mars 2005b). In the samples where lip surgery and subsequent palate surgery were performed, palatal surgery appeared responsible for only a small additional amount of retrusion, 1.0 mm in the Sri Lankan sample and 0.7 mm in the Brazilian sample. The same effect was seen in the prominence of the anterior alveolar process. Dahl (1970) also found a substantial reduction in maxillary prominence in patients with UCLP who had undergone lip surgery only. However, because individuals with complete clefts who have undergone only palatal surgery are not available, this experiment cannot be considered complete. It is by no means certain that the effect of palatal repair alone would be limited to 1 or 2 mm (i.e. whichever operation is undertaken first could have the major restraining effect).
The transverse dimension of the basal maxilla does not seem to be affected by surgery, but the dental arches are highly affected. Palatal closure often includes incisions alongside the dental arches, and the scars produced may induce an inward deflection of the dentoalveolar processes, resulting in anterior and traverse crossbites (Ross and Johnston 1972; Bergland and Sidhu 1974; Dahl et al. 1981). It is therefore likely that different surgical techniques for closing the palate give rise to malocclusions of different extent without necessarily altering the neighbouring structures.
15.4 Clinical Uncertainty
Considerable ingenuity has been applied in the development and modification of primary surgical protocols for closing UCLP and BCLP. And if one takes the technique, timing and sequence of operations into account, the variations in practice between centres can be extreme. One survey funded by the European Union found that 201 cleft teams employed a total of 194 different protocols in the closure of UCLP (Shaw et al. 2001). The total number of primary operations to close the cleft varied from 1 to 4; a total of 17 possible sequences of operation for closing the cleft were practised; lip closure was performed at all possible points between birth and 12 months; the timing of hard palate closure ranged from birth to 13 years. Almost half the centres used presurgical orthopaedics. In fact, all of the 201 teams would have differed in their protocols had not seven of them previously agreed to participate in a randomised trial.
15.5 Theories That Have Influenced Surgical Management
In general, developments of new or modified surgical protocols have been founded on one or other theoretical premise, and disappointment with current results. Examples of these would include assumptions concerning the underlying mechanisms of maxillary growth, the presence and location of growth centres (to be avoided during surgery) or the role of muscular function in optimising growth potential. However, present understanding of the controlling mechanisms of facial growth is incomplete and derives from observational work and speculation in earlier decades.
However, this field of research no longer seems popular with craniofacial biologists, and understanding of the mechanisms of facial growth has not advanced in recent years. Current research mostly focuses on genetic causation, on gene environment interaction and on Hox genes, growth factors and signalling molecules that influence facial embryogenesis, providing, at this stage, few options for surgical manipulation.
Examples of theories that have influenced surgical management in a quest for better maxillary growth include:
-
Delaying closure of the hard palate.
-
“Later” lip repair may reduce early growth impairment.
-
Designing flaps to minimise denuded bone, for example, avoiding pushback techniques and using minimal lateral releasing incisions.
-
Avoiding use of the vomerine flap in order to safeguard septal and the vomero-premaxillary suture development and in turn growth.
-
Performing extensive facial muscle dissection to optimise function and, in turn, growth.
-
Reducing the extent of trauma at any one time by performance of surgical closure in small incremental stages, such as three or four operations rather than one or two.
-
Assuming early benefits of repairing the alveolar cleft by bone grafting or other osteogenic technique in infancy would not harm growth.
-
Assuming that presurgical orthopaedics/soft tissue moulding would facilitate surgery and improve the long-term result in better or equal growth.
-
Assuming that concentrating surgery on high-volume surgeons would achieve better growth.
As we shall see below, however, most of these theories and assumptions have proved unreliable in actual practice, except possibly in the case of the last. The following appraisal is based upon earlier reviews (Semb and Shaw 1996, 1998), three more recent comprehensive reviews (Liao and Mars 2006; Friede 2007; Yang and Liao 2010) and reports of additional studies that set out to make explicit intra- or intercentre comparisons of different surgical protocols using cephalometry and/or indices of dental arch relationship.
15.6 Clinical Evidence to Support or Refute Theories Concerning Surgery and Growth
15.6.1 Delayed Hard Palate Closure
Delayed hard palate closure is by no means a recent development having been proposed at least 90 years ago (Gillies and Fry 1921). It is still relatively popular; in the last survey, 16.5 % of European centres delayed closure till the child was older (range 3–13 years). But it has not been without critics. In their review of the rationale and supporting evidence for this procedure, Witzel and co-workers (1984) proposed that the beneficial effect on facial growth had not been proved (unless surgery is delayed until after 12 years of age) and deleterious effects on speech had been largely disregarded. Recent findings from a randomised trial confirm this risk (Willadsen 2011). By 3 years of age, the group where hard palate repair was delayed to 3 years had a more restricted phonological system and produced more cleft speech characteristics than the group repaired at 1 year.
Earlier data from single-centre studies indicate that maxillary prominence does not systematically differ between centres practicing early closure of the hard palate with a vomer flap or by different forms of one-stage palatoplasty, including pushback, and those who delay hard palate closure (Semb and Shaw 1996). Only the exceptional delay of hard palate closure in Marburg sample until mean age 13.2 years (range 8–22 years) confirmed a beneficial long-term effect on maxillary growth while assessment of speech development revealed significant speech impairment (Schweckendiek and Doz 1978; Bardach et al. 1984b).
However, earlier reports of very good maxillary growth with delayed closure (till age 8) were recently confirmed by Friede and co-workers (2011) in a cephalometric follow-up of 50 patients to age 19 and an assessment of dental arch relationship at age 19 (Lilja et al. 2006). Liao et al. (2010) also found better maxillary prominence at age 20 in a delayed closure group compared with an early closure group treated in different time periods at the same centre in Taiwan, though delayed closure was abandoned because of poor speech outcome. Noverraz et al. (1993) found no advantage for delayed closure in an intracentre comparison, while Gaggl et al. (2003) compared two groups from the same centre at 18 years, and found maxillary prominence to be worse in the delayed closure group, while another intracentre study, despite use of the original Schweckendiek protocol including obturation and hard palate closure at 7 years, reported very negatively on delayed closure as it led to severe speech problems, deleterious growth and a high rate of retrusion calling for orthognathic surgery (Holland et al. 2007). Negative speech and outcomes for delayed closure were also reported from yet another intracentre study (Rohrich et al. 2000).
Intercentre comparisons including at least one delayed hard palate closure group have been reported. Friede and Enemark (2001) compared growth outcome between Gothenburg and Aarhus samples of 30 patients. The first group had soft palate closure at 8 months and hard palate closure at 8.5 years (mean) while the second had anterior palate closure at 3 months (vomer flap) and soft palate closure at 22 months (pushback). Cephalometric values at three intervals from the early to mid-teens for maxillary prominence were better for the delayed closure group, though less so with age.
Swennen et al. (2002), however, found no differences in a comparison between a delayed closure and an early closure centre, nor did Stein et al. (2007) in a similar study. Comparison of delayed with early closure in the same centre revealed no difference in dental arch relationship (Noverraz et al. 1993). This was also the case in a subsequent Eurocleft comparison of records with another centre practising delayed closure (Nollet et al. 2005a). Nor did delayed closure surpass early closure in a small four-centre Scandinavian comparison (Friede et al. 1991).
Robertson and Jolleys (1974) conducted a randomised trial involving two groups of 20 patients where one group’s hard palate closure was delayed until 5 years of age. No benefit for dentofacial growth was found in delaying hard palate closure when the children reached 11 years of age.
One exception to this pattern is the report of a meta-analysis where regression analysis suggested delayed closure to be beneficial for growth (Nollet et al. 2005b). One explanation may be inclusion of a high proportion (65 %) of patients from the UK (where delayed closure is not practised), mainly drawn from a series of studies revealing historical deficiencies of cleft surgical services in general (Bearn et al. 2001).
An alternative approach to the timing question is presented by Berkowitz et al. (2005; see also Chap. 7). This multicentre three-dimensional analysis of study casts found that the velocity of growth decreases over the first 2 years and then plateaus. It was concluded that the optimal time for closure was when the ratio of the posterior cleft space to the total palatal surface area is 10 % or less, generally occurring between 18 and 24 months.
The present overview leads us to concur with the comprehensive reviews of Liao and Mars (2006) and Yang and Liao (2010) who noted that the great heterogeneity in reports precludes reliable conclusions at this time and makes the case that well-designed prospective studies are necessary to resolve this uncertainty; Friede (2007) also drew attention to the forthcoming findings of three randomised trials in the Scandcleft series (Semb 2001, described below).
15.6.2 Later Lip Closure
In truth, not much consideration has been given to the timing of lip closure, but we include it here for consideration as factor that may have been overlooked in interpreting outcomes. Bardach et al. (1984a) drew attention to the high lip pressure that follows repair, and lip surgery on its own is associated with considerable moulding of the anterior maxilla (Liao and Mars 2005a, b) and possibly restraint of the basal maxilla (Capelozza et al. 1996).
Almost one third of European centres perform lip repair at 6 months or later (Shaw et al. 2001). There are no comparative studies of early versus late lip repair that we are aware of, but it is interesting that several diverse protocols that include late lip repair have achieved good growth outcomes. These include “all-in-one repair” undertaken at 9 months (Fudalej et al. 2009), soft palate repair at 3 months followed by lip and hard palate repair at 6 months (Trotman and Ross 1993) and the Zurich protocol with lip repair at 6 months (Perko 1990). Another variation is the Gothenburg protocol where lip adhesion is done at 2 months and definitive repair is deferred to 18 months (Friede and Enemark 2001). Substantial postponement of lip closure of course may raise important sociological issues.
15.6.3 Efforts to Minimise Trauma and Scarring
It does seem probable that minimising trauma and scarring by delicate tissue handling and judicious flap design can only be beneficial and that suitable forms of tissue engineering or pharmaceutical modulation of scarring offer promise for the future (see Chap. 5). Much has been written about the harmful effect of palatal scars that form on areas of the palate denuded during primary surgery (Palmer et al. 1969; Blocksma et al. 1975), and it has been postulated especially that scar tissue located in the region of the maxillary/palatine and palatine/pterygoid sutures acts to prevent the maxilla’s normal downward and forward translation (Ross and Johnston 1972). Avoidance of the vomero-premaxillary suture has also been recommended (Friede and Morgan 1976).
Ross (1987) hypothesised that early soft tissue closure of the alveolus might also lead to some growth impairment compared to those who had had no alveolar repair.
Perko (1974) developed a mucosal split flap to avoid elevation of the periosteum. A modified version of this achieved more arch depth than the previously used Wardill-Kilner technique in a Japanese comparison (Leenstra et al. 1996). Jonsson et al. (1980) used a vomer flap covered with an autogenous skin graft in UCLP but without significant benefit. Also, no or minimal releasing incisions for closure of the palate (except in patients with very wide clefts) have been proposed (Brusati and Mannucci 1994; Sommerlad 2009).
15.6.4 Vomer Flap
Scott’s theories on the primacy of the nasal septum probably did much to underpin concerns about surgical harm to the vomer, and different opinions have been held regarding the disadvantages and benefits of the use of a single-layer vomer flap to close the hard palate (Friede and Johanson 1977; Jonsson et al. 1980; Bütow and Steinhauser 1984; Delaire and Precious 1985; Friede and Pruzansky 1985; Enemark et al. 1990; Semb 1991a, b; Hay and Sommerlad 2008). However, again, the available clinical evidence contradicts the theory. As noted above, and in an earlier review (Semb and Shaw 1996), single-centre cephalometric studies incorporating vomer flap show no systematic evidence of growth disturbance, and several have some of the highest values. Likewise, in a series of different intercentre comparisons involving analysis of dental arch relationship and/or cephalometry, alternative methods have equalled but not surpassed vomer flap (combined with modified von Langenbeck posterior palate closure) samples at statistically significant levels (Friede et al. 1991; Brattström et al. 1991; Mars et al. 1992; Mølsted et al. 1992, 2005; MacKay et al. 1994; Roberts-Harry et al. 1996; Gaukroger et al. 2002; Brattström et al. 2005; Nollet et al. 2005a; Flinn et al. 2006; Meazzini et al. 2008; Fudalej et al. 2009; Meazzini et al. 2010).
15.6.5 Extensive Orofacial Muscle Dissection
Anatomical study of the orofacial and oronasal musculature led Delaire to propose extensive “functional repair” of the musculature as a solution to midface growth inhibition (Joos 1995); however, although the theory was put into practice by Delaire and others for a time, little evidence for its validity has since emerged. One single-centre study reported UCLP outcomes at a mean age 6.5 years and found outcomes better than a historical control group treated by a different surgeon (Joos 1995). No conventional cephalometric data or study cast index was reported. Others have drawn attention to the possible paradox that more extensive surgery to achieve normal anatomy may incur the penalty of greater scarring and growth restraint (Kuijpers-Jagtman and Long 2000).
15.6.6 Single or Multiple Stages of Closure
In the European survey referred to above, the total number of operations taken to complete closure of complete unilateral clefts varied from one (5 %), two (71 %), three (22 %) and four (2 %) with multiple stages often part of a delayed hard palate program. The economy and reduction of the burden of care clearly favour the “all-in-one” approach, but that could be offset with a perceived greater challenge of post-operative management and worries about iatrogenic growth disturbance, as evidenced in animal studies (Bardach et al. 1993).
Interestingly, the evidence available from intercentre comparisons suggests that varying the number of stages may actually be neutral in terms of growth. In the Americleft study (Chap. 18), Centre C who performed three-stage closure (lip, then hard palate with vomer flap, then soft palate) ranked highest for growth (Daskalogiannakis et al. 2011; Hathaway et al. 2011). An “all-in-one” sample from Poland has also compared well with mainstream staging in intercentre comparisons (Fudalej et al. 2009). De Mey et al. (2009) reported a prospective cohort study in a single centre, where a two-stage Malek protocol was compared with an “all-in-one” Malek protocol. Entry to the latter group was limited to patients with a posterior palate width less than 10 mm. Both groups were followed till age 10 and 15 and had good cephalometric outcomes.
15.6.7 Primary Bone Grafting
Initial reports of successful bone grafting at the time of lip closure (Schmid 1955; Nordin 1957) led to its adoption in several centres. This was followed however by a steady process of abandonment in the subsequent decades and a series of reports mostly describing negative impact on maxillary growth (Rehrmann et al. 1970; Friede and Johanson 1974; Robertson and Jolleys 1983; Pfeifer 1986; Reichert and Manzari 1990; Lilja et al. 1996; Smahel et al. 1998) but with some exceptions (Rosenstein et al 2003; Dado and Rosentstein 2009). Intercentre comparisons also highlighted growth problems (Ross 1987; Brattström et al. 1991, 2005; Trotman et al. 1996), most recently within the Americleft study where the only centre performing primary bone grafting ranked poorest overall for maxillary growth (Hathaway et al. 2011).
15.6.8 Presurgical Infant Orthopaedics (PSIO)
This topic is the subject of another chapter, so will be referred to briefly here. Two sources provide comprehensive overview of the relevant literature (Kuijpers-Jagtman and Long 2000; Uzel and Alparslan 2011). Originating in the late 1940s, PSIO continues to be popular despite, rather than because of, the evidence. When reports about a particular technique provide no evidence of benefit, adherents are entitled to say that this does not amount to evidence of no benefit. However, in the case of PSIO, the Dutchcleft randomised trial of passive orthopaedics does provide good evidence of no benefit at 4 and 6 years in respect of maxillary development and dental arch relationship (Bongaarts et al. 2009), raising doubts about the ethical status of PSIO.
On the other hand, of the clinical reports of active orthopaedics with the Latham appliance listed by Uzel and Alparslan, five of six reports suggest actual harm in respect of facial growth (Roberts-Harry et al. 1996; Henkel and Gundlach 1997; Berkowitz et al. 2004; Matic and Power 2008; Power and Matic 2009). Only one report found no growth harm (Chan et al. 2003). Apart from the study of Roberts-Harry et al. (1996), the use of active orthopaedics and gingivoperiosteoplasty were combined (discussed below).
15.6.9 Nasoalveolar Moulding (NAM)
Though it has much in common with active PSIO in its intended reduction of the alveolar cleft gap to allow for gingivoperiosteoplasty (GPP) repair of the infant alveolar cleft, nasoalveolar moulding (NAM) also has explicit goals of alignment and correction of the deformity in the nasal cartilages and non-surgical elongation of the columella. If successful, it should obviate the need for secondary nose/lip revision and alveolar bone grafting (Grayson et al. 1999).
Beneficial short-term effects of NAM on nasolabial form and columella length have been demonstrated in technique papers and reports (Grayson et al. 1999; Grayson and Cutting 2001) and small retrospective case series (Wood et al. 1997; Grayson et al. 1999; Maull et al. 1999; Singh et al. 2007; Lee et al. 2008; Barillas et al. 2009). Most of these studies report improved nasolabial outcomes using a variety of assessment methods, though Liou et al. (2004) observed some lack of stability and Chang et al. (2010) considered further surgery necessary.
Unfortunately, in the two decades since its introduction, there have been no substantial reports of consecutive patients nor prospective studies of the influence on facial growth. Wood et al. (1997) compared 11 patients who received NAM and GPP with 9 who received NAM alone and found them not to differ in a cephalometric shape coordinate analysis. A subsequent follow-up of the same groups with 8–13 years old found reduced maxillary prominence (position of ANS) that did not reach statistical significance (Lee et al. 2004), while need for secondary bone grafting was estimated at 40 % in a sample of 20 sites with previous GPP (Santiago et al. 1998).
Preliminary intercentre comparisons in the Americleft project raise some doubts about the consistency of outcomes (Chap. 18).
15.6.10 Gingivoperiosteoplasty (GPP)
In 1965, Skoog introduced periosteoplasty as an alternative to bone grafting: by using double-layer periosteal flaps, bone formation across the cleft was induced without the need of a donor site. The periosteoplasty technique was adopted by a few teams, and in the 1990s, the technique was modified and popularised by Brusati and Mannucci (1992) and Cutting and Grayson (1993) as gingivoalveoloplasty. Normally accompanied by active presurgical orthopaedics or nasoalveolar moulding, the evidence required to validate it as a desirable routine intervention will have to confirm that it matches mixed dentition bone grafting in quality and reliability, that the additional burden imposed by the presurgical preparation offsets the burden of mixed dentition bone grafting and that the risk of requiring later orthognathic surgery is not increased.
Concerns about adequacy of the bone in the former cleft alveolus and subsequent maxillary growth have been reported. With respect to Skoog’s original procedure (Skoog 1965) and a free tibial periosteal graft variation, Hellquist and Svardström (1990) found good bone formation in only 47 % of patients, Rintala and Ranta (1989) found 72 % required secondary bone grafting and Renkielska et al. (2005) found 50 % of patients operated according to the Skoog protocol-required orthognathic surgery.
Millard adopted the active pin-retained or “Latham appliance” as a means of reducing the size of the cleft by aligning the alveolar segments prior to surgery (Millard and Latham 1990). However, this led to an increased level of anterior crossbite in unilateral and bilateral cases (Millard et al. 1999), and Berkowitz et al. (2004) reported a likely need for orthognathic surgery in the majority of patients. Similar conclusions were reached by Henkel and Gundlach (1997), who followed 60 Latham appliance/GPP patients with UCLP or BCLP and found substantial horizontal and vertical maxillary growth disturbance compared with a similar group treated without Latham appliance GPP. The success of grafting was not reported.
Two Canadian studies compared, respectively, 54 UCLP Latham appliance/GPP patients with 16 UCLP mixed dentition alveolar bone graft patients and 53 BCLP Latham appliance GPP patients with 10 BCLP secondary bone graft patients in their mid-teens (Matic and Power 2008; Power and Matic 2009). Both revealed considerably fewer successful grafts, more fistulae and disturbed growth in the Latham/GPP groups. Interestingly, no rebuttal of these critical reports was published by the originators of the protocol, and a subsequent report of BCLP patients treated by the Latham appliance and GPP confirmed the negative experience of others (Latham 2007). The author proposed an alternative method of palate closure and the postponement of definitive lip repair till 18 months to overcome this (Latham 2007).
It is of course difficult to distinguish between the Latham appliance and gingivoperiosteoplasty as the source of growth inhibition, and the advent of NAM was regarded by some authors as a superior preparation for GPP since it is “a passive process that directs the growth of the alveolar segments” (Hopper and Birgfield 2009). Hsieh et al. (2010) found maxillary growth at age 5 to be worse with GPP and NAM than with NAM alone. Long-term follow-up of a GPP variant postponed till the time of palate repair at 18–36 months indicated a higher need for orthognathic surgery in comparison with a sample from the same centre and a sample from another centre who received conventional mixed dentition bone grafting (Meazzini et al. 2010).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


