HISTORY
The technique of lengthening bone by gradual distraction has been used in a variety of specialties sporadically over the past century. Its application to the craniofacial skeleton is relatively recent, and its indications have been expanding over the past decade. Distraction osteogenesis (DO) was used by orthopedic surgeons during the first half of the 20th century. The concept of DO was formally introduced in 1969 by Gavriel A. Ilizarov, who together with Dr. L. M. Sojbelman published his first case series of distraction epiphysiolysis in the journal Eksperimentalnaja Khirurgia Anestesia . After he graduated from medical school in 1943, the Russian government sent Ilizarov to work in the Kurgan district of western Siberia. In post–World War II Russia, thousands of wounded veterans were in need of multiple surgical procedures, many of which involved conditions such as fracture, pseudoarthrosis, and osteomyelitis. Ilizarov had been applying this method for multiple surgical applications for years before his case reports were published. After hearing of the “miracles” accomplished with his revolutionary surgical procedures in orthopedic surgery, people in Russia referred to him as the “magician from Kurgan.” In 1951, Ilizarov started to use metal rings with transosseous wires to align and manipulate bone segments of complicated fractures in long bones, subsequently achieving bone healing after stabilizing the segments for a time. Early in the 1960s, Ilizarov distracted a short tibial stump with the intention of subsequently grafting the gap he had created. He was surprised to discover 1 month later on post-operative x-ray that he could not see a gap at all. At this point, he was able to identify technical aspects of the procedure that led to gradual successful lengthening of the tibia. The early concepts that he proved are still seminal today and are important in justifying these early concepts. Early postulates included (1) that corticotomy was safe with continued bone marrow viability, and (2) that combining corticotomy with slow distraction bone lengthening was possible. Ultimately, Ilizarov is recognized as one of the most important surgeons in the establishment of DO as a procedure with a large number of applications.
From a maxillofacial perspective, dentofacial traction is a procedure that has been used since the 18th century. Fauchard in 1728 had started to practice dental arch expansion in the presence of dental crowding; this was done at the expense of tooth movement with little change in bone morphology. Westcott in 1859 reported correction of crossbite in a 15-year-old patient after a slow and tedious process that had lasted several months. Angell in 1860 achieved rapid palatal expansion over the course of 2 weeks at the expense of midpalatal suture separation. Thirty-three years later, in 1893, Goddard standardized the procedure by recognizing the need for a 3-week period of stabilization to allow for “osseous material” formation at the “created gap.” In 1937, Kazanjian achieved mandibular advancement by gradually applying traction rather than acute movement of an osteotomized mandible. The device used consisted of a wire hook attached to the symphysis, which was advanced with traction with the use of an elastic band. Anchorage was achieved with the aid of a facial appliance anchored to the maxillary teeth and stabilized against the patient’s forehead, much like a phase I orthodontic appliance. Activation was started 3 days post-operatively when forward movement of the osteotomized mandibular segment was attained. Seventeen days later, traction was ended, and intermaxillary fixation was instituted for 11 weeks with the aid of occlusal splints. At this point, DO lacked recognition as a reliable method, in part because of lack of bone segment manipulation control, difficulty manipulating the custom appliances, and inadequate skeletal fixation methods used for stabilization after distraction.
In 1973, Snyder reported the first successful mandibular DO in a canine model following the distraction principles previously established by Ilizarov for limb lengthening. Guerrero (1990) and McCarthy (1992) were among the first to report on the clinical feasibility of mandibular lengthening by gradual distraction in patients with craniofacial anomalies. Since the first reports, DO has been widely used in the treatment of patients with various craniomaxillofacial deformities. Recently, there has been an explosion of reports in the literature regarding the use of DO on the craniomaxillofacial skeleton, and much has been learned about the indications and usefulness of this technique. Techniques and outcome expectations continue to be refined.
BIOLOGIC BASIS OF DISTRACTION OSTEOGENESIS
During the 1997 International Congress of Cranial and Facial Distraction Osteogenesis in Paris, France, Dr. Paul Tessier referred to DO as the “end of facial osteotomies as we know them.” A decade has passed, and traditional osteotomies still are used much more frequently, but distraction has provided solutions to some very difficult problems that were challenging or impossible to address prior to its development. As with many new technologies, much excitement was generated early in the development of distraction devices and techniques. As more experience and data become available, the best indications and the limitations are becoming clearer. Distraction techniques appear to have great potential in addressing a number of difficult problems such as exceptionally large advancements and advancements required in very young patients.
DO offers several purported advantages to the clinician who is managing craniofacial anomalies. Its major advantage is that it provides the opportunity for lengthening of craniofacial bones to a degree not typically possible with traditional techniques. DO also eliminates donor site morbidity in cases in which bone grafting typically is used in combination with traditional advancement techniques. In addition, DO provides a method of lengthening the craniofacial skeleton while at the same time distracting the surrounding soft tissue matrix. Consequently, DO has gained popularity as a treatment modality and has opened new therapeutic opportunities for the treatment of patients with numerous congenital and acquired craniofacial skeletal anomalies.
Established treatment parameters for DO as initially described by Ilizarov are important for a successful result and include the following :
- •
Cortical osteotomy with minimal periosteal stripping
- •
Latency period ranging from 3 to 7 days, depending on the surgical site, and a potentially shorter duration for younger children
- •
Distraction rate of 0.5 to 2.0 mm per day depending on the surgical site, usually 1.0 mm per day. Faster rates in children, especially neonates
- •
Distraction with application of continuous force is ideal but activation of the device twice per day or three times per day is effective and practical for the patient.
- •
Consolidation period should be approximately 6 weeks or should last until cortical outlines are visible on radiograph.
The procedure entails performing an osteotomy of the cortical bone at the site of anticipated lengthening. Preservation of the periosteum and the surrounding vascular supply is an important factor in the success of DO. The objective of DO will be to slowly separate the edges of the osteotomy to create a regenerative chamber that will give rise to bone. Depending on the distraction site, great variation is expected in the size and conformation of the osteotomy, and a regenerative chamber is possible (i.e., maxillary osteotomy, mandibular ramus osteotomy, fronto-orbital and midface osteotomy, or alveolar ridge osteotomy).
Once the corticotomies have been completed and the distractor device is in place, the latency period begins. The latency period ranges from 0 to 10 days, with the most common durations of 1 to 2 days in children and 5 days in adults. This allows for resolution of the inflammation resulting from the corticotomy and surgical placement of the device. The first phase of healing involves organization of the hematoma and induction of mesenchymal cells, as well as endosteal and periosteal cells, into osteoblasts and fibroblasts. Type I collagen is deposited and osteoid production takes place.
Once the distraction phase begins, this healing tissue is exploited by lengthening of the regenerate. Distraction of the regenerate tissue then can occur at a rate of approximately 1 mm per day. Although this process of regenerate lengthening is directed at providing bone, the surrounding soft tissue also is stretched during the lengthening procedure. This phenomenon of soft tissue expansion is referred to by some as distraction histogenesis . Skin, muscle, nerves, and vascular tissue purportedly have been generated, not stretched, but observation of many cases and conflicting literature make these concepts controversial.
In the young child, larger bones with a larger regenerate chamber site may be able to tolerate quicker distraction rates. Decreasing the rate is recommended for small areas such as the dentoalveolar ridge segments. The initial process of bone formation involves a regenerate chamber that is filled with a fibrous matrix that will ossify at the periphery and then centrally over time. The regenerate area consolidates into bone once the distraction process is consolidated and the segments are rigidly fixed in place. Distraction that moves too quickly will result in non-union, and distraction that occurs too slowly will result in early healing without the potential to lengthen the segments.
The consolidation time in adults should be at least 3 months and can be as long as 6 months, depending on the magnitude of distraction, the type of deformity, and the patient’s age. How the length of consolidation affects stability is unclear at this point, but it is clear that bone stability is very important during the consolidation phase. Once consolidation has been confirmed, removal of the hardware can be performed with basic radiography or other imaging modalities such as computed tomography (CT) scan.
In some cases, distraction osteogenesis offers several advantages over other techniques such as the following:
- •
Ability to accomplish large advancements
- •
Ability to expand soft tissue surrounding matrix
- •
Minimizes or eliminates the need for bone grafting
- •
Potentially less relapse than with traditional methods
However, when compared with traditional techniques, DO may have a number of disadvantages in certain situations, including those listed here:
- •
Higher post-operative infection rate at the osteotomy site
- •
Greater risk of hardware failure
- •
Difficulty with vector control with less precise positioning of segments when compared
- •
Risk of premature bone formation or non-union
Relative contraindications to DO include the following :
- •
Patient/Family non-compliance regarding activation of distraction device
- •
Lack of adequate bone (Class III hemifacial microsomia)
- •
Radiation therapy
- •
Bisphosphonate use
BIOLOGIC BASIS OF DISTRACTION OSTEOGENESIS
During the 1997 International Congress of Cranial and Facial Distraction Osteogenesis in Paris, France, Dr. Paul Tessier referred to DO as the “end of facial osteotomies as we know them.” A decade has passed, and traditional osteotomies still are used much more frequently, but distraction has provided solutions to some very difficult problems that were challenging or impossible to address prior to its development. As with many new technologies, much excitement was generated early in the development of distraction devices and techniques. As more experience and data become available, the best indications and the limitations are becoming clearer. Distraction techniques appear to have great potential in addressing a number of difficult problems such as exceptionally large advancements and advancements required in very young patients.
DO offers several purported advantages to the clinician who is managing craniofacial anomalies. Its major advantage is that it provides the opportunity for lengthening of craniofacial bones to a degree not typically possible with traditional techniques. DO also eliminates donor site morbidity in cases in which bone grafting typically is used in combination with traditional advancement techniques. In addition, DO provides a method of lengthening the craniofacial skeleton while at the same time distracting the surrounding soft tissue matrix. Consequently, DO has gained popularity as a treatment modality and has opened new therapeutic opportunities for the treatment of patients with numerous congenital and acquired craniofacial skeletal anomalies.
Established treatment parameters for DO as initially described by Ilizarov are important for a successful result and include the following :
- •
Cortical osteotomy with minimal periosteal stripping
- •
Latency period ranging from 3 to 7 days, depending on the surgical site, and a potentially shorter duration for younger children
- •
Distraction rate of 0.5 to 2.0 mm per day depending on the surgical site, usually 1.0 mm per day. Faster rates in children, especially neonates
- •
Distraction with application of continuous force is ideal but activation of the device twice per day or three times per day is effective and practical for the patient.
- •
Consolidation period should be approximately 6 weeks or should last until cortical outlines are visible on radiograph.
The procedure entails performing an osteotomy of the cortical bone at the site of anticipated lengthening. Preservation of the periosteum and the surrounding vascular supply is an important factor in the success of DO. The objective of DO will be to slowly separate the edges of the osteotomy to create a regenerative chamber that will give rise to bone. Depending on the distraction site, great variation is expected in the size and conformation of the osteotomy, and a regenerative chamber is possible (i.e., maxillary osteotomy, mandibular ramus osteotomy, fronto-orbital and midface osteotomy, or alveolar ridge osteotomy).
Once the corticotomies have been completed and the distractor device is in place, the latency period begins. The latency period ranges from 0 to 10 days, with the most common durations of 1 to 2 days in children and 5 days in adults. This allows for resolution of the inflammation resulting from the corticotomy and surgical placement of the device. The first phase of healing involves organization of the hematoma and induction of mesenchymal cells, as well as endosteal and periosteal cells, into osteoblasts and fibroblasts. Type I collagen is deposited and osteoid production takes place.
Once the distraction phase begins, this healing tissue is exploited by lengthening of the regenerate. Distraction of the regenerate tissue then can occur at a rate of approximately 1 mm per day. Although this process of regenerate lengthening is directed at providing bone, the surrounding soft tissue also is stretched during the lengthening procedure. This phenomenon of soft tissue expansion is referred to by some as distraction histogenesis . Skin, muscle, nerves, and vascular tissue purportedly have been generated, not stretched, but observation of many cases and conflicting literature make these concepts controversial.
In the young child, larger bones with a larger regenerate chamber site may be able to tolerate quicker distraction rates. Decreasing the rate is recommended for small areas such as the dentoalveolar ridge segments. The initial process of bone formation involves a regenerate chamber that is filled with a fibrous matrix that will ossify at the periphery and then centrally over time. The regenerate area consolidates into bone once the distraction process is consolidated and the segments are rigidly fixed in place. Distraction that moves too quickly will result in non-union, and distraction that occurs too slowly will result in early healing without the potential to lengthen the segments.
The consolidation time in adults should be at least 3 months and can be as long as 6 months, depending on the magnitude of distraction, the type of deformity, and the patient’s age. How the length of consolidation affects stability is unclear at this point, but it is clear that bone stability is very important during the consolidation phase. Once consolidation has been confirmed, removal of the hardware can be performed with basic radiography or other imaging modalities such as computed tomography (CT) scan.
In some cases, distraction osteogenesis offers several advantages over other techniques such as the following:
- •
Ability to accomplish large advancements
- •
Ability to expand soft tissue surrounding matrix
- •
Minimizes or eliminates the need for bone grafting
- •
Potentially less relapse than with traditional methods
However, when compared with traditional techniques, DO may have a number of disadvantages in certain situations, including those listed here:
- •
Higher post-operative infection rate at the osteotomy site
- •
Greater risk of hardware failure
- •
Difficulty with vector control with less precise positioning of segments when compared
- •
Risk of premature bone formation or non-union
Relative contraindications to DO include the following :
- •
Patient/Family non-compliance regarding activation of distraction device
- •
Lack of adequate bone (Class III hemifacial microsomia)
- •
Radiation therapy
- •
Bisphosphonate use
MANDIBULAR DISTRACTION OSTEOGENESIS
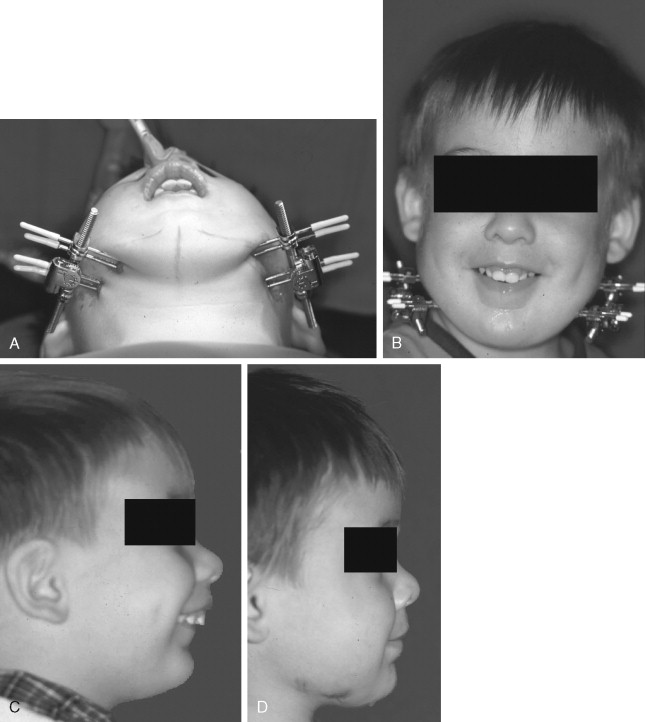
Mandibular retrognathia is a congenital or acquired condition that can represent functional and esthetic problems. Congenital abnormalities that may exhibit severe mandibular retrognathia include craniofacial anomalies such as hemifacial microsomia, Pierre-Robin sequence, Treacher-Collins syndrome, Nager syndrome, and a number of others. Acquired sources of origin include post-traumatic and iatrogenic post-surgical scar formation that may induce growth disturbances ( Figure 49-1 ). Mandibular growth may be adversely affected by condylar fractures that occur at an early age with formation of ankylosis at the temporomandibular joint and/or deficient mandibular growth.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


