Fig. 6.1.
Differently pronounced attachments of the masseter muscle indicate a long history of unilateral function and asymmetrical skeletal relations
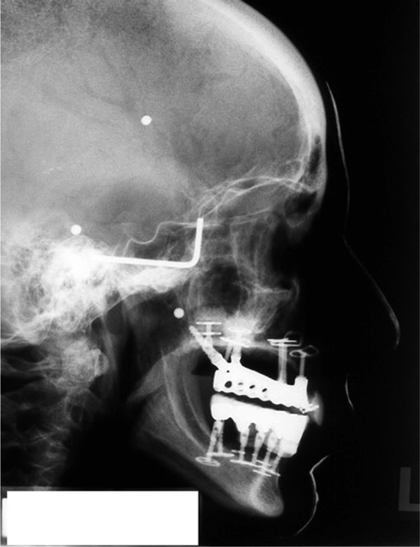
Fig. 6.2.
Lateral teleradiographs should be obtained before and after implant therapy to check the orientation of the bridge in relation to the relevant planes. In addition, the dentist may want to apply contrast medium (e.g. barium slurry), which in this example is used to visualize the facial profile
In the anterior segment of the mandible, pits of varying sizes must be expected, some of which may contain unpleasantly large vessels of the arterial anastomosis. It is therefore always necessary to palpate this area thoroughly, unless it is planned to dislodge the mucosa on the lingual side of the mandible during the procedure and protect the soft-tissue structures with a raspatory.
The conditions for palpatory examination are much less favourable in the maxilla where the palatal soft-tissue structures are thick and hard. The palatal artery, which tends to be concealed below a half-open bony canal, is virtually never palpable. Whenever the situation is unclear, the only way to explore the bone structures is by dislodging a flap. The implant site for the tuberopterygoid screw cannot be viewed either on a dental film or on an OPG. The only way to explore this area, should the need arise, is by tomography.
6.6 Functional Diagnosis and Restorative Alternatives
The first parameter to be established is whether the midlines of both jaws coincide. The labial frenum will usually suffice as reference point. It may be necessary to disregard this parameter if any teeth are missing unilaterally due to agenesis or extraction because any midline shifts associated with these situations cannot and must not be corrected by prosthetic means. The same applies if the OPG reveals that the horizontal branch of the mandible is not equally long on both sides of the jaw.
Deviations in the opening and closing movements of the mouth are the main diagnostic criterion indicating the presence of functional problems. This statement is true regardless of whether or not the dysfunction is symptomatic or asymptomatic. Pain is strictly confined to the working side.
Elongation of teeth can be observed on the non-working side where the intrusive effect of the masticatory function is less marked. Since the anterior segment (i.e. canine to canine) of the maxilla is always activated as a whole, it is mainly the central and lateral incisors of the non-working side that become elongated. Posterior teeth, by contrast, will always become elongated collectively. The occlusal plane will deviate from the horizontal line in these cases, taking a cranial course on the working side and a caudal course on the non-working side. From a frontal perspective, this type of occlusal plane will come across as an oblique line although it is really a winding line (see Chapter 10 for details).
Lateralization of the dentition can also be observed on the working side, due to the fact that the intrusive forces are unilaterally stronger. This development may cause prosthetic problems, since the former working side will be overly lateral relative to the mandibular teeth after the midline has been adjusted with a view to re-establishing a physiological function. In difficult situations, a correctly adjusted midline may even give rise to lateral non-occlusion. Potential treatment alternatives would include wide bridge elements, medialization of the bridge relative to the bone, or orthodontic pre-treatment. Readjusting the midline will always result in a unilateral increase of the vertical dimension if teeth are still present in the maxilla. The minimum requirement with regard to the vertical dimension is defined by the elongated side (i.e. the former non-working side). In most of these situations, new laterotrusion facets will need to be established with abrasive instruments.
Unilateral extractions on the non-working side will invariably give rise to tilting of the molars distal to the extraction socket, with the distal cusps gaining more vertical space. The premature contacts resulting from this development may cause the mandible to become decentralized in all spatial directions, thus creating locked bite situation. The teeth on the working side are, by contrast, more likely to undergo bodily movements in a lateral direction (i.e. translation movements).
The condylar angle is large on the working side because the movements taking place in this area are confined to rotation. The angle on the non-working side, by contrast, is very flat because the translation movements dominating this area counteract the development of a steep tubercle.
This situation results in different AFMP angles on both sides of the jaw. The angle is always larger on the non-working side due to the elongation and medialization of teeth. The effort required to chew on this side becomes even greater, and the tendency to retain the unilateral chewing pattern is further reinforced.
Age-related diastemas may form through periodontally induced protrusion and elongation in addition to physiological abrasion, which will cause the teeth to become narrower even in the absence of periodontal problems.
6.6.1 Non-correctable Dysfunctions
Any treatment plans involving the use of BOI implants should be reconsidered if a balanced function apparently cannot be restored by any means. Possible reasons include efferent or afferent nerve dysfunction, paralysis of muscles (e.g. after polyomyelitis),or dissection of muscles/jaw segments. All these factors can create situations in which a balanced masticatory function is either out of reach or cannot be properly controlled. Restorative therapy based on strategically positioned BOI implants is not indicated in these cases. Instead, an attempt should be made to maximize both the number of inserted implants and the number of disks per implant, thus creating a situation in which the sum total of these contact surfaces will still allow a favourable force distribution even in the presence of inappropriate loading patterns that would otherwise give rise to osteolysis around individual disks and loss of individual implants due to isolation-related overloading. It is still possible to use this multi-implant strategy with immediate loading. The larger number of implants and load-transmitting surfaces will increase the direct bone-preserving effect of the implant surfaces relative to the effect of macrotrajectories.
BOI-based treatment with strategic implant positioning only is contra-indicated in the presence of permanent dysfunction. Consider that a resting osseous system may be present at the outset of therapy in which the preoperative trajectorial bone orientation may no longer be wholly in line with the functional pattern. Any increase of the BMU frequency and artificial stimulation of remodelling in this situation as triggered by an implantation procedure would abruptly induce reorientation of the bone structures, particularly if the masticatory function is not bilaterally balanced, which give rise to substantial morphological alterations. In masticatory systems that are not bilaterally balanced, it is considerably harder to tell in advance which bone areas will remain stable and sufficiently mineralized over the years.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


