CASE REPORT-1
Bone grafting of osseous defect of extraction socket simultaneous with implant placement (Courtesy: Dr Peter Randelzhofer and Dr Gert de Lange)
1. Compensation of buccal bone wall resorption after tooth extraction by bone augmentation with Geistlich Bio-Oss® and Geistlich Bio-Gide®
2. Immediate implant placement to reduce overall treatment time in the aesthetic area
3. Preservation of the papillae (< ?xml:namespace prefix = "mbp" />
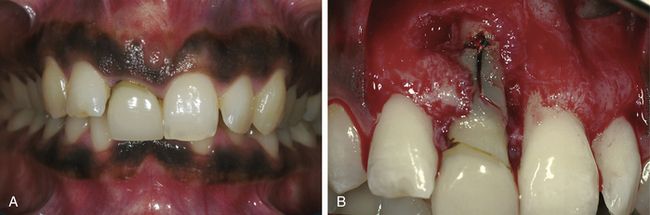
Fig 14.1 The patient presented with a thick, medium scalloped, gingival morphology. Tooth 11 presented with poor prognosis due to vertical root fracture. The tooth had slightly extruded resulting in a vertical gain of soft tissue. (A) The pigmented gingiva presented an extra challenge. (B) After careful flap elevation, a clear fracture of the root was visible. The vertical bone defect affected two-thirds of the buccal bone plate.
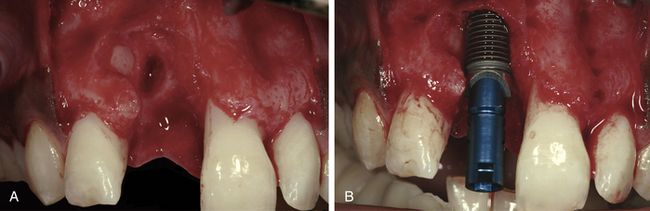
Fig 14.2 An extensive bone deficit became visible after tooth extraction. (A) It was accompanied by extensive attachment loss on tooth 21, which caused a high aesthetic risk due to possible loss of papillae after surgery. Inserted implant showed good primary stability. (B) Due to the pronounced bone defect, a closed healing approach was chosen.
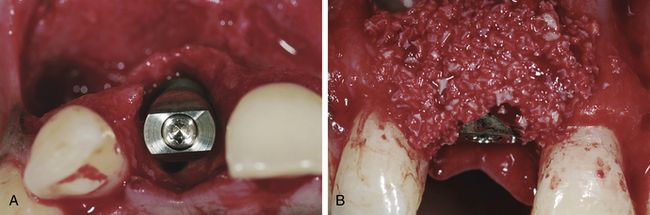
Fig 14.3 The implant was placed within the bordering sidewalls of the defect (within the osseous envelope) to maintain adequate space for the graft. (A) The gap distance from the implant surface to the buccal bone plate should be at least 2 mm. Autologous bone chips were harvested using a trephine drill from the retromolar area and were placed onto the implant surface. Geistlich Bio-Oss® was mixed with blood and applied onto the bone chips to prevent primary resorption of the autologous bone. (B) The regenerated hard tissue provided the basis for stable soft tissue architecture.
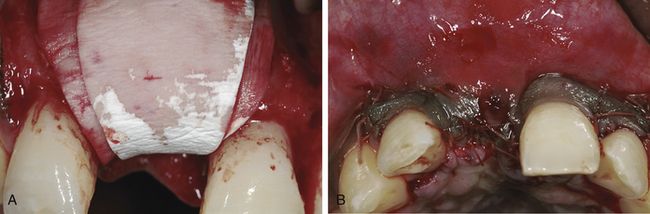
Fig 14.4 The augmented area was covered with the Geistlich Bio-Gide® membrane. (A) The membrane was placed in the double layer technique to provide stable protection for bone regeneration. For additional soft tissue augmentation, a connective tissue graft from the palate was sutured under the flap. In order to guarantee a tension-free closure the flap was mobilized by a split-flap technique. (B) Primary wound closure was achieved with resorbable vicryl sutures 6.0/5.0. During a second stage surgery, 4 months later, the pigmented gingiva was repositioned coronally by a split-flap technique to restore its natural shape (not shown).
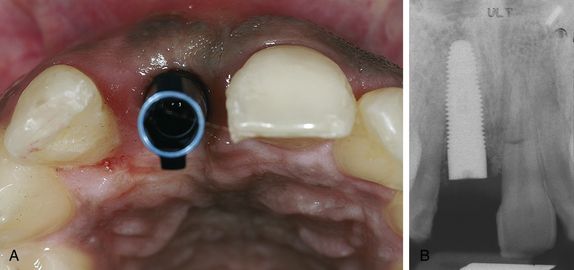
Fig 14.5 (A) Five months after implant placement: the distance from the implant to the buccal aspect of the alveolar ridge was still more than 2 mm, which was important for a stable long-term aesthetic result. (B) Control radiograph on reopening.
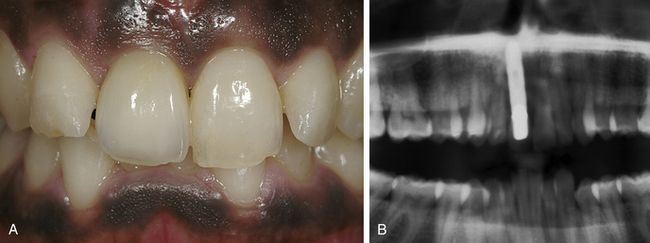
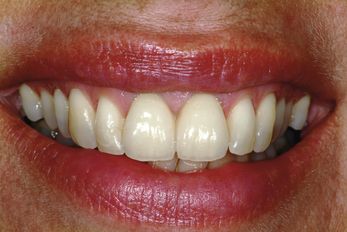
Fig 14.6 Clinical situation 1 month after crown placement: the gingiva showed a natural appearance, was nicely scalloped, and displayed no scar tissues. (A) The pigmented part could be maintained in shape and colour. (B) Control radiograph 1 year after implantation.

The technique presented in

CASE REPORT-2
Bone grafting simultaneous with immediate implant with open (transmucosal) healing (Courtesy: Dr Peter Randelzhofer and Dr Gert de Lange) (
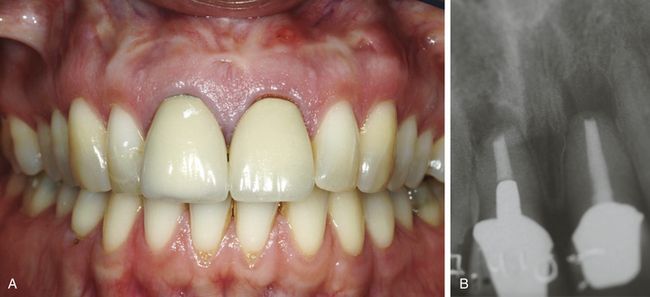
Fig 14.7 (A) Patient presented with a high smile line and thin biotype with two rather large central incisors with fistulae and poor prognosis. (B) Radiograph showed endodontic infections of both central incisors with expected osseous defect apical to the post-extraction socket.
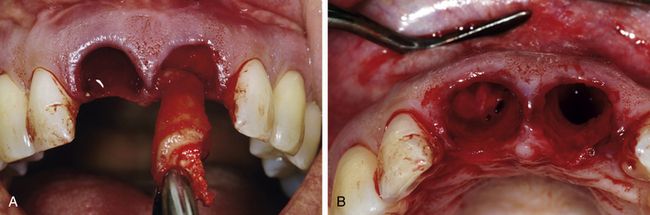
Fig 14.8 (A) Careful extraction of both central incisors was done, preserving marginal gingiva and papillae. (B) Palpation of the buccal wall showed bone defects connected with a granuloma in the socket.
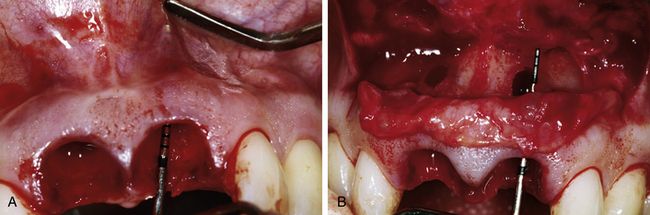
Fig 14.9 Inspection of the left socket showed apical soft tissue and hard tissue defects. (A) Note the thin central papilla. (B) After a vestibular half circle incision was made, the flap was deflected downwards and the buccal bone defects became visible for the right and left sockets.
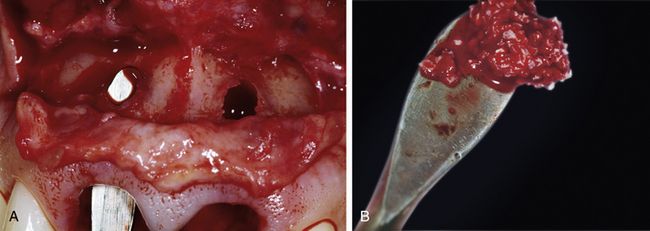
Fig 14.10 After removal of granuloma tissue and endodontic material, thorough cleaning of the bone was done using antibiotics. (A) There were large remaining bony defects of the buccal wall of both sockets. The buccal bone plate was restored using autologous bone particles collected from lower retromolar site and covered with Geistlich Bio-Oss®. (B) Geistlich Bio-Oss® particles were also used to fill the remaining buccal space between healing abutment and marginal gingiva for maximum soft tissue support.
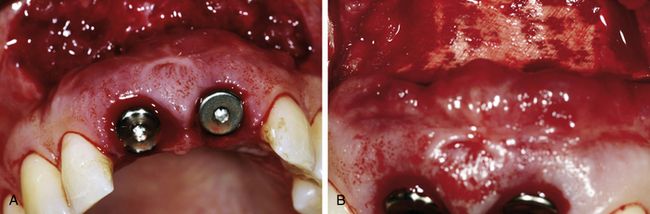
Fig 14.11 Two Camlog Screw Line implants were placed with primary stability of 35 Ncm. (A) Adequate supports of the marginal soft tissues was obtained by immediately placing a wide body healing abutment intended to prevent tissue collapse and to preserve the contour of the gingival margin. (B) For undisturbed bone regeneration, the augmented area was covered with Geistlich Bio-Gide® barrier membrane.
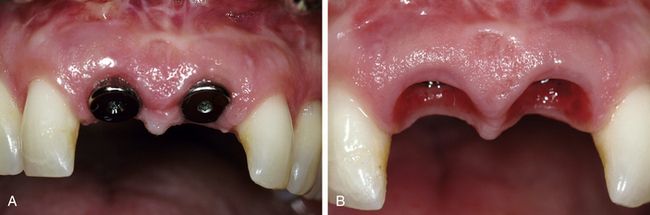
Fig 14.12 (A) One week after open healing, the soft tissues had adapted well. (B) Healing abutments which preserved the soft tissue well were removed 2 months after implant placement and replaced with provisional crowns of anatomical shape, which created nicely scalloped marginal gingiva and papillae.
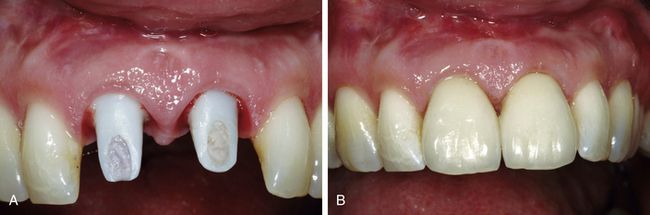
Fig 14.13 (A) Ceramic abutments were placed. Final zirconium crowns, which were smaller in the cervical region, were fixed on the abutments. (B) Note the total absence of tissue loss and gingival recession.

The open healing procedure in

CASE REPORT-3
Bone defects are difficult to evaluate using only the radiograph, and often, surprisingly, are seen after the site is exposed to insert the implant (
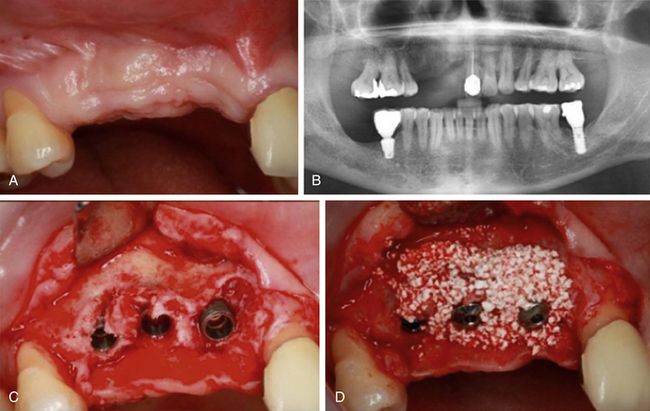
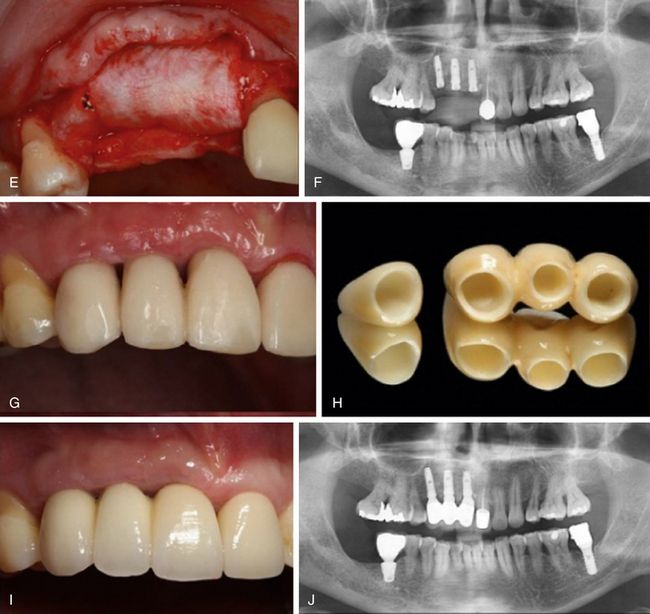
Fig 14.15 (A and B) Missing teeth numbers 11, 12, and 13. (C) The small bone defects are visible around the inserted implants, which need to be grafted. (D) The particulated (HA + β-TCP) bone graft (osteon) is used to graft the Peri-implant defectsand (E) a collagen barrier membrane is used to cover the grafted site. Flaps are sutured back. (F) Post implantation radiograph. (G) Implants are uncovered and temporized after 4 months (H and I) the implants are finally restored using metal-free zirconium prosthesis. (J) Post loading radiograph.


CASE REPORT-4
Grafting of small osseous defects simultaneous with implants placement (Courtesy: Dentium Co. and Well Dental Clinic, Soul, Korea) (
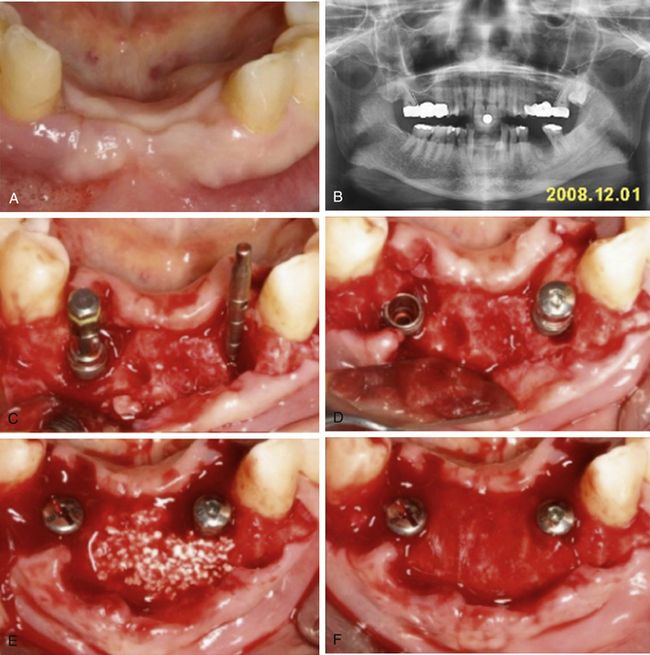
Fig 14.16 (A and B) Missing mandibular incisors. (C and D) Small osseous defects are visible after insertion of the implants, which were grafted using (E and F) osteon bone substitute and covered with collagen barrier membrane.
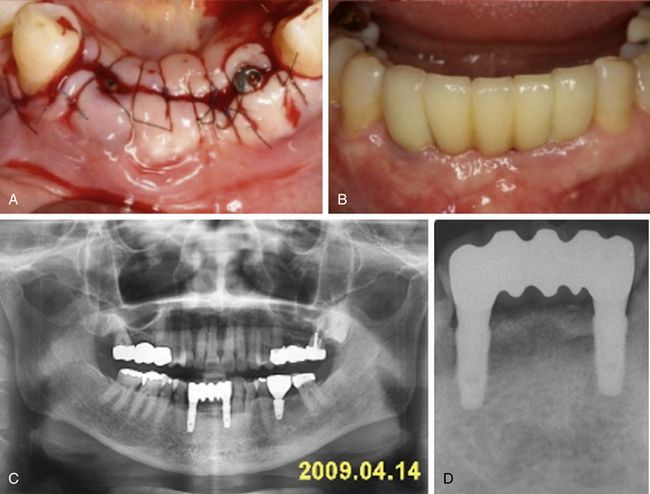
Fig 14.17 (A) Flap is sutured back. (B and C) Implants are uncovered and restored after 4 months. (D) Radiograph 1 year after implant restoration shows stable crestal bone level.


CASE REPORT-5
A 57-year-old healthy female with history of trauma to the face 8 years earlier, presented to the Oral Surgery and Implantology Center of Dr Len Tolstunov, San Francisco, CA, USA. The patient was referred by the general dentist for evaluation of a failing upper left canine. On presentation, the patient complained of cuspid mobility and periodic discharge from a wound high in the vestibule.
The patient’s history of the present condition was significant for the trauma that happened 8 years ago, when she was hit with a fist to the left anterior maxilla. The upper left canine was affected by the blow, the patient felt it was loose but she did not go to a dentist and let it heal on its own. The patient felt a bump deep in the vestibule next to the tooth for many years and there was occasional discharge. The patient finally decided to see a dentist and an oral surgeon, due to recent increased swelling and pain in the area of the traumatized tooth.
The patient’s aesthetic profile consisted of a low smile line, oval teeth and a thick, flat gingival biotype. There was an open gingival flap exposing the necrotic apical two-thirds of the root of the canine, which was probed deep in the vestibule with no discharge from the wound (
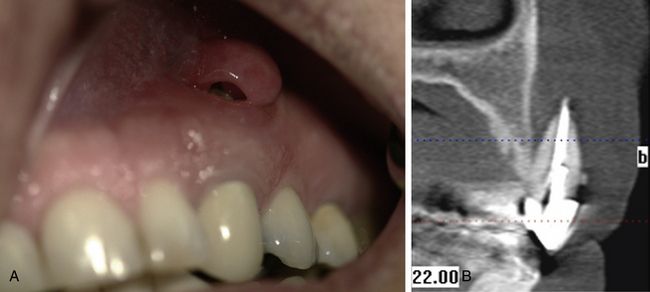
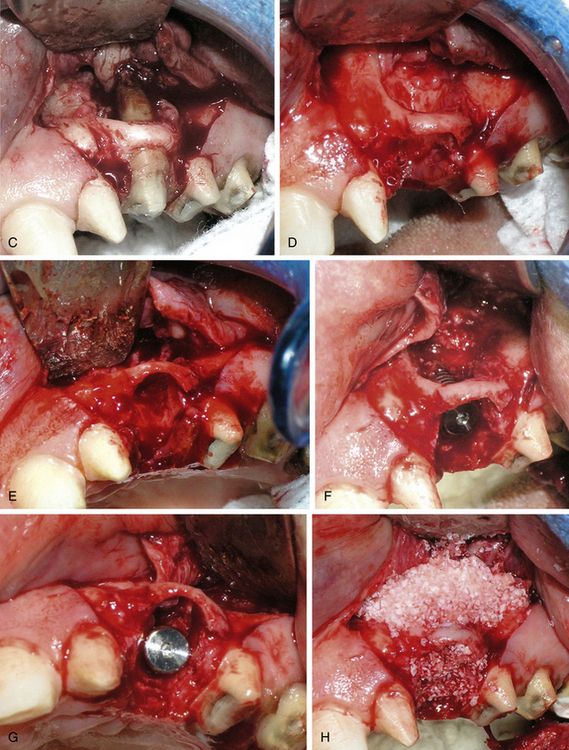
Fig 14.18 (A and B) Maxillary left canine with the large hard and soft tissue defect.(C–E) A large osseous defect is visible after careful flap elevation and tooth extraction. All the granulation tissue was curetted out and site was disinfected using tetracycline powder. (F and G) The osteotomy was prepared and the implant was placed within the bony envelope and at the correct prosthetic position. (H) The facial wall defect as well as the Peri-implant socket spaces were grafted using Bio-Oss (Osteohealth Co.), 0.5 g and Puros (Zimmer), 0.5 ml.
Radiographic examination consisted of the periapical, panoramic, and cone beam computed tomography (CBCT) scans that demonstrated (old) mid root fracture, previous root canal treatment, and severe apical bone loss around the tooth with just a small amount of structural bone support left on the palatal and buccal crestal area (
The recommendations for the patient’s condition included a staged approach with an extraction of the cuspid, a bone graft followed by the placement of an endosseous implant 4–6 months later, followed by a restorative phase with a ceramic restoration. The patient also needed a provisional appliance.
The patient rejected a staged treatment due to her busy schedule and asked that the practitioner should attempt to do both surgical stages in one. The patient’s consent was taken and she was scheduled for surgery.
The surgery consisted of extraction of the affected tooth, bone grafting and implant placement at the same time under intravenous (IV) sedation. After the IV sedation was started and local anaesthesia was given, the crestal full-thickness flap with a distal releasing incision was reflected. Severe buccal bone loss and exposure of the unsupported and fractured canine tooth were visualized (
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses