Arthrocentesis is a safe and rapid procedure used to treat a multitude of disorders affecting the temporomandibular joint (TMJ). The popularity of this procedure followed the success of arthroscopic surgical procedures with initial application for the treatment of disk displacement without reduction. Since that time, arthrocentesis has been described for other clinical indications; however, it is not indicated for all joint disorders. The procedure does not change the shape or position of the disk or the structure of the mandibular condyle and glenoid fossa. Pathology involving bony degeneration, osteophytes and bone spicules, disk perforation, or fibro-osseous ankylosis is not amendable to arthrocentesis. Treatment is generally indicated when other non-surgical and pharmacologic methods have failed.
The etiology of pain associated with the TMJ is multifaceted. Possible sources of pain include impingement, compression, and inflammatory changes in the retrodiscal tissues; inflammatory changes in the synovial membrane with joint effusion; and capsulitis. Biochemical investigations of TMJ synovial fluid obtained through arthroscopic lavage and arthrocentesis have yielded information regarding the pathophysiology of pain in the TMJ. Lavage and lysis of the joint space allows for removal and dilution of inflammatory mediators, which may contribute to reduction of pain. Elevated protein levels in synovial fluid parallel the degree of inflammation because of increased permeability of the synovial membrane to plasma proteins. Joint effusion detected on T 2 -weighted magnetic resonance images reflects hypertrophic synovial lining and exudation from inflamed tissues. Joint effusion is observed in joints at a more advanced degree of internal derangement.
Before arthrocentesis is performed, patients must undergo appropriate diagnosis and treatment planning. This is based upon medical history, visual analogue pain scales (if indicated), and clinical and radiographic findings. Clinical examination should include interincisal opening, lateral excursions, deviation on opening, and documentation of any occlusal discrepancies. Auscultation of the joint may be performed to ascertain any clicks or crepitus, which may indicate disk displacement or degenerative joint disease, respectively. Radiographic imaging would initially include a panoramic screening film followed by other appropriately indicated imaging modalities including tomographs, computed tomography, magnetic resonance imaging, or nuclear medicine studies.
Conservative management for TMJ disorders may include participating in physical therapy, avoiding traumatic behaviors such as clenching or gum chewing, changing the patient’s diet, administering nonsteroidal anti-inflammatory drugs or muscle relaxants, and wearing occlusal appliances. Patients who fail conservative measures are candidates for arthrocentesis. Non-surgical management for internal derangement without reduction improves symptoms comparably to surgical intervention; however, improvement takes a longer time. Patients with TMJ internal derangements without reduction who do not respond to non-surgical management benefit from arthrocentesis and/or arthroscopic lysis and lavage.
TMJ internal derangements have been described to progress through clinical stages, initially presenting as clicking with normal interincisal opening and progressing to limited opening lacking translatory movement where clicking ceases because of a nonreducible disk. Excessive loading on the joint with a nonreducible, anteriorly displaced disk, which restricts the ability of the condyle to translate on the articular surfaces, is treated effectively with arthrocentesis of the superior joint space. The major indications for arthrocentesis are as follows:
- 1.
Acute and chronic limitation of opening because of anteriorly displaced disk without reduction
- 2.
Chronic pain with good range of motion and anterior disk displacement with reduction
- 3.
Degenerative osteoarthritis
Nitzan has also described a condition of TMJ open lock where the condyle is entrapped anterior to a lagging disk. This has been reported to be effectively treated with arthrocentesis and should be distinguished from TMJ condylar dislocation where the condylar head is locked anterior to the articular eminence. Contraindications to TMJ arthrocentesis would be those patients who have not undergone appropriate conservative/non-surgical and pharmacologic treatment, demonstrate bony or fibrous ankylosis, or have extracapsular sources of pain.
PATHOPHYSIOLOGY OF TMJ DYSFUNCTION
There are several theories regarding the development of pain and dysfunction within the TMJ including the musculature, bony structures, synovium, and discal tissues. Past interest has been directed at the changes observed in the shape and position of the articular disk. More recent research has focused on the biomechanical and biochemical processes involved in TMJ dysfunction. The anchored disk phenomenon, as described by Nitzan, is a sudden onset of limited mouth opening with deviation of the mandible towards the affected side. Forced opening of the mouth may provoke pain. The disk will appear to be stuck to the fossa with the condyle sliding underneath the disk on magnetic resonance imaging (MRI) studies. This is in distinction to disk displacement without reduction, where the patient tends to evolve through stages with intermittent popping and clicking, leading to internal derangement with reduction, and eventual development of limitation of opening with internal derangement without reduction.
The suction cup effect is one of the forces that possibly can maintain the articular disk adherent to the fossa in the anchored disk phenomenon. In an earlier study, greater negative pressures were measured in the upper joint space of patients with anchored disk phenomenon compared to normal joints. The negative pressure was thought to be significantly strong enough to keep the disk from sliding in a normal manner. Insertion of a needle into the superior joint space would reduce the negative pressure; however, other factors may contribute to this condition. Joint overloading may cause collapse of the lubrication system through increased intra-articular pressure and hypoxia that is compensated by reoxygenation on termination of overloading. The hypoxia-reperfusion cycle can lead to the release and production of reactive oxygen species, which can lead to the degradation of hyaluronic acid (HA) and a marked reduction in synovial fluid viscosity. Within the TMJ, surface-active phospholipids function as boundary lubricants and protectors of the articular surfaces. Lysis of these surface-active phospholipids by phospholipase A 2 can result in a significant increase in friction and adhesion between articular surfaces. HA plays a role in joint lubrication through its protection of the surface-active phospholipids from lysis by phospholipase A 2 . Injection of hyaluronic acid after arthrocentesis/arthroscopy has been postulated to contribute to a boundary layer of lubrication initially after surgery so patients may begin their physical therapy postoperatively.
Temporomandibular joints with internal derangements may be painful as well as demonstrate restricted mobility. Proinflammatory cytokines, which are induced by inflammatory stimuli, may be involved in the pathogenesis of internal derangements. Interleukin-1-beta (IL-1-β) and tumor necrosis factor-alpha (TNF-α) are responsible for destruction of cartilage through degradation of proteoglycans. Interleukin-6 may act to protect cartilage through promotion of the production of tissue inhibitors. It has been suggested that IL-1-β and IL-6 in synovial fluid may be associated with the development of osteoarthritis and the presence of IL-6 may be an index of synovitis. Patients with internal derangements treated with arthrocentesis underwent analysis of synovial fluid aspirates for the assessment of proinflammatory cytokines. It was determined that the detection of IL-6 and IL-1-β in synovial fluid may be an indicator for possible unsuccessful treatment after arthrocentesis for internal derangement of the TMJ.
TECHNIQUE OF TEMPOROMANDIBULAR JOINT ARTHROCENTESIS
Symptomatic temporomandibular joint disease is often accompanied by accumulation of inflammatory mediators within the synovial fluid as previously described. The accumulation of these inflammatory mediators may persist for some time within the joint space because of the relatively avascular nature of this space. The mechanism of arthrocentesis to lavage and lyse the joint space may remove these inflammatory mediators as well as alter the intra-articular pressure through the addition of more fluid. It is logical, therefore, to combine arthrocentesis with nonsteroidal anti-inflammatory medications and possible splint therapy to treated an inflamed synovial joint. Since one of the goals of arthrocentesis is to wash out the inflammatory mediators responsible for inflammation within the joint, it would be necessary to adequately irrigate the joint space. Repeatedly injecting solution into the joint will increase pressure to release adhesions, but not necessarily eliminate the inflammatory mediators. It was observed that 200 mL of perfusate was sufficient to observe a statistically significant reduction in protein, bradykinin, and IL-6 concentrations. An ideal lavage volume between 300 and 400 mL perfusate resulted in no detectable level of protein and bradykinin. Previous recommendations were for 100 mL of perfusate to effectively decrease the concentration of protein in synovial fluid and provide therapeutic lavage. Recommendations should probably be for a minimum of 100 mL of total arthrocentesis volume to achieve therapeutic lavage of the superior joint space of the human TMJ.
Arthrocentesis of the TMJ under low pressure with an elevated infusion bag or syringe has been reported to be effective in treating patients with acute closed lock of the TMJ. Irrigation and lavage under sufficiently high hydraulic pressure could widen the joint space and potentially remove adhesions to improve mandibular mobility. This can be an effective procedure for treating patients with chronic closed lock and adhesions in the superior joint space. High-pressure infusion with a maximum pressure of 40 kilopascals (kPa) may offer wider application of arthrocentesis for patients other than those with acute closed lock. Arthroscopic correlation of joints undergoing arthrocentesis revealed the release of adhesions in those patients undergoing high-pressure irrigation, but not those having received low-pressure therapy. The results suggest that arthrocentesis with sufficient pressure could be effective for treatment of patients with closed lock with adhesions in the upper joint space.
Arthrocentesis of the TMJ may be performed with the patient receiving a local anesthetic, IV conscious sedation, or a general anesthetic, depending on surgeon and patient preferences. It is most conveniently performed with the patient in the office suite in a semi-reclined position. The hair is pulled from the surgical field and retracted using a combination of sterile surgical towels and antibiotic ointment. The external auditory canal should be protected from fluid and blood accumulation using an antibiotic-impregnated cotton pledget. A canthal-tragal line is drawn from the midpoint of the tragus to the lateral canthus of the ipsilateral eye. A point is made 10 mm forward from the tragus and 2 mm inferior to the line. This 10-2 point approximates the posterior extent of the articular fossa. This should be confirmed by palpation with the patient opening and closing the mouth. A second point corresponding to the height of the articular eminence can be marked at 20 mm anterior to the midtragal point and 10 mm below the tragal-canthal plane. This can function as a landmark for the placement of the second portal for the outflow of irrigant ( Figure 48-1 ).
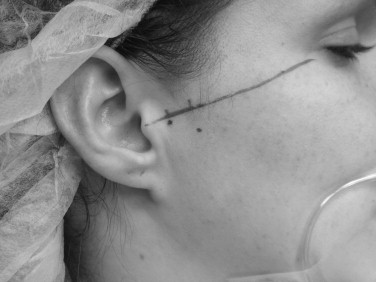
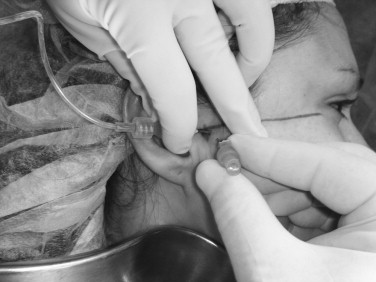
An auriculotemporal block and infiltration to the areas for joint penetration are completed using a local anesthetic. The superior joint is entered with an 18-gauge needle directed in an anterior-medial-inferior direction at the 10-2 entry point, aiming for the posterior aspect of the articular eminence or anterior recess. Alternatively, some surgeons prefer to gently touch the zygomatic arch and gently walk the needle into the superior joint space. Once the joint space is entered, it may be insufflated with saline or lactated Ringer’s solution. Several milliliters of solution can be injected rather passively into the joint space to the end point, where there is rebound of the syringe pressure with jaw movement. With the needle in place, the syringe is removed and either a larger syringe can be attached for irrigation or connection to an intravenous fluid bag may be performed. A second needle must be inserted for the outflow portal slightly anterior to the initial needle placement ( Figure 48-2 ). The lavage is performed by the surgeon using approximately 100 mL of fluid either manually or with intravenous fluid set-up. After completion of the lavage, the joint can be manipulated by the assistant, who is not part of the sterile field and has his or her gloved hand in the patient’s mouth, moving the patient’s mouth through opening, protrusive, and excursive movements. A goal of 30 to 40 mm interincisal opening should be achieved at the completion of arthrocentesis. Alternatively, there are commercially available Y-shaped needles available for arthrocentesis that require a single puncture into the superior joint space and contain inflow and outflow channels within the single needle ( Figure 48-3 ).

At the completion of the arthrocentesis procedure, some surgeons elect to inject steroids for their anti-inflammatory effects on the synovial tissue. Sodium hyaluronate has been proposed as a therapeutic agent for the treatment of TMJ disorders after arthrocentesis. It is a glycosaminoglycan produced by synovial cells and present in high concentrations in the joint cartilage and synovial fluid. This viscous, high molecular weight substance plays an important role in joint lubrication and protection of the cartilage. It has been demonstrated that arthrocentesis with the injection of sodium hyaluronate (a process called viscosupplementation) is an effective treatment for patients with degenerative TMJ disease. Patients with disk displacement with and without reduction may also benefit from the injection of sodium hyaluronate after arthrocentesis. These patients injected with sodium hyaluronate were observed to have a faster and longer-lasting period of pain relief. Jaw function and maximal opening increased earlier and were maintained longer in those patients receiving sodium hyaluronate in addition to arthrocentesis compared to those patients who only underwent the arthrocentesis procedure. Sodium hyaluronate contributes to joint function by maintaining lubrication, minimizing mechanical wear, and playing a role in the nutritional support of the avascular portion of the disk and condylar cartilage.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


