Technologic Advances in Implant Surgery
Piezoelectric Bone Surgery
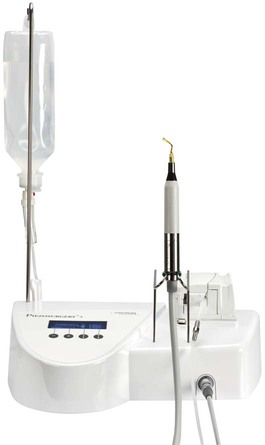
A new surgical technique, known as piezosurgery, was invented by Vercellotti and developed by Mectron Medical Technology. The piezosurgery device (Figure 80-1) consists of a piezoelectric ultrasonic transducer powered by an ultrasonic generator, capable of driving a range of specially designed cutting inserts (Figure 80-2).17,22 Box 80-1 describes the main cutting properties of piezosurgery by Mectron, and Box 80-2 describes piezosurgery inserts. Piezoelectric bone surgery techniques have been developed for clinical applications in dentistry and are becoming state of the art for a variety of procedures.18–20,22,28,29 Recently, Piezosurgery Medical expanded development of clinical applications to other fields of medicine. The extraordinary cutting properties of piezoelectric bone surgery have been introduced and applied in maxillofacial surgery, cranial and spinal neurosurgery, and hand-foot surgery.3–13





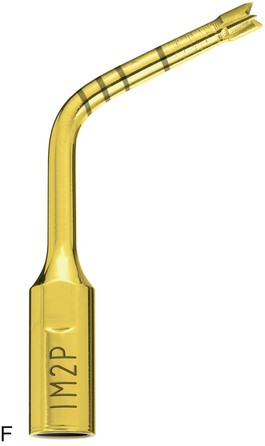
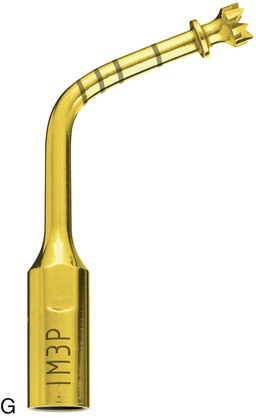


A, Piezosurgery osteotomy 7 insert: OT7 (0.5 mm thick). B, Piezosurgery osteotomy 7 special insert: OT7S (0.35 mm thick). C, Piezosurgery osteoplasty 1 insert: OP1. D, Piezosurgery osteoplasty 3 insert: OP3. E, Piezosurgery implant site preparation 1 insert: IM1. F, Piezosurgery implant site preparation 2 insert: IM2. G, Piezosurgery implant site preparation 3 insert: IM3. H, Piezosurgery periodontal surgery 2 insert: PS2. I, Piezosurgery elevation (of schneiderian membrane) 1 insert: EL1.
The most compelling characteristics of piezoelectric bone surgery are low surgical trauma, exceptional control during surgery, and a fast healing response of tissues. Clinical studies demonstrate that the specificity of operation and the techniques employed with piezoelectric bone surgery make it possible to advantageously exploit differences in hard- and soft-tissue anatomy.3,23,25,26 This not only increases treatment effectiveness but it also improves postoperative recovery and healing. Experimental studies on animals have shown faster tissue healing when compared to traditional cutting instruments.3
Clinical Characteristics of Ultrasonic Cutting
Excellent Healing
Clinical studies comparing use of piezoelectric bone surgery with traditional rotary instruments for third molar extractions14 and periodontal surgery25 have reported better recovery and fewer postoperative symptoms in those treated with piezosurgery. Postoperative healing after piezoelectric bone surgery is characterized by minimal swelling and little bleeding and postoperative morbidity is lower compared to traditional techniques.24 Gingival tissue is typically light in color when compared to the appearance of autogenous gel of platelet-rich plasma.
Clinical Applications
Periodontal Surgery
The use of piezosurgery in periodontal surgery simplifies and improves handling of soft and hard tissues.30 In resective periodontal surgery, for example, after raising the primary flap with a traditional technique, using a scaler-shaped insert (PS2) (Figure 80-3, A) or an insert in the shape of a rounded scalpel (OP3) makes it easier to detach the secondary flap and remove inflammatory granulation tissue. This phase has little bleeding as the result of the cavitation of the saline solution (coolant). With the right inserts and power mode, the ultrasound device facilitates effective scaling, debridement, and root planing (Figure 80-3, B and C). In particular, debridement with a special diamond-coated insert enables thorough cleaning even for interproximal bone defects (Figure 80-3, D). The mechanical action of ultrasonic microvibrations, together with cavitation of the irrigation fluid (pH neutral; isotonic saline solution) eliminates bacteria, toxins, dead cells, and debris, which creates a clean physiology for healing. Healing is improved by applying ultrasound to produce micropits at the base of the defect to activate cellular response of healing mechanisms. Autogenous bone-grafting material consists of bone chips that are collected during the piezoelectric osteoplasty operation for recontouring bone irregularities (Figure 80-3, E). The result is that this technology reduces the invasiveness of traditional surgery by making surgery faster and by ensuring thorough cleaning of the periodontium. It also favors tissue healing by using bone removed in the osteoplasty procedure to graft osseous defects.
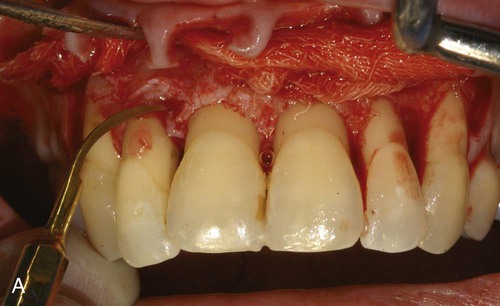
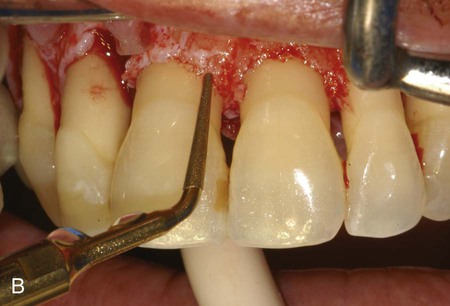
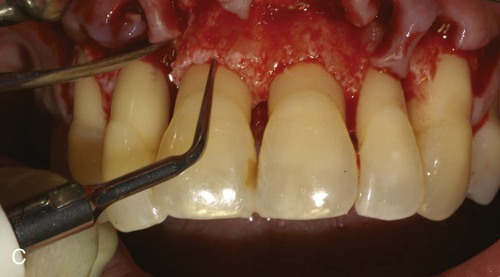
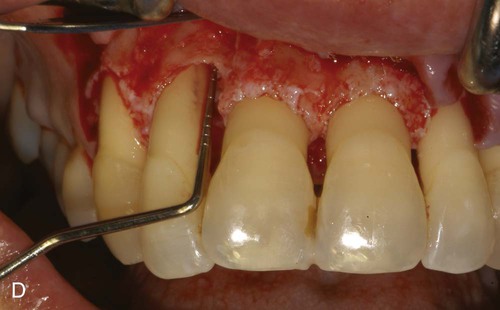
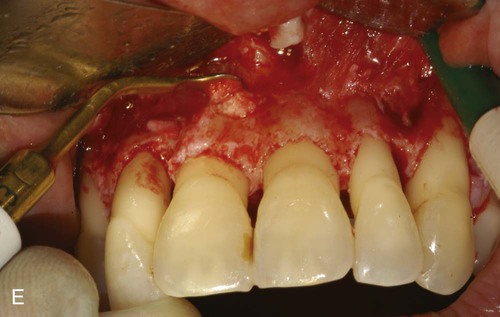
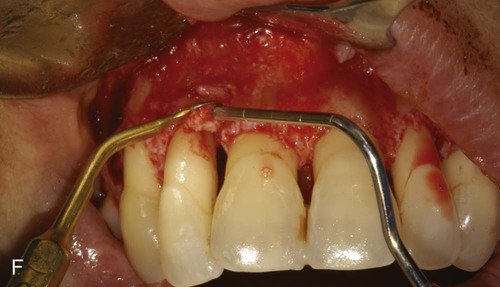
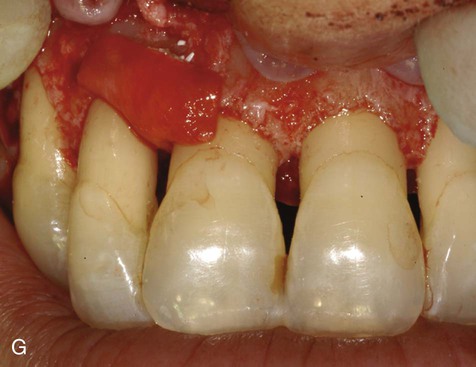
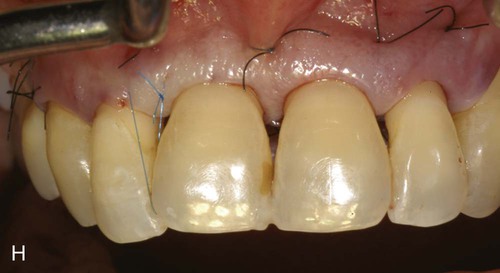
A, Ultrasonic scaling using piezosurgery PS2 insert. B, Root surface debridement using piezosurgery diamond-coated OP5 insert. C, Ultrasonic root planing using piezosurgery blunt insert: PP1. D, Interproximal infrabony defect with probe. E, Autogenous bone chip–harvesting technique using piezosurgery osteoplasty insert: OP3. F, Autogenous bone grafting technique. G, Collagen membrane stabilizing microbone grafting. H, Flap repositioned and sutured.
The ability to work on the bone defect with magnifying systems makes it possible to exploit the benefits of piezosurgery microprecision in preparing the recipient site and stabilizing micrografts (Figure 80-3, F to H).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses