Supporting Structures
The Periodontium
• To understand the relationships within the gingival unit, a supporting structure of the teeth
• To understand the terminology of the gingival unit and to identify its various parts
• To understand how the gingival unit functions
• To understand how the attachment apparatus is related to the gingival unit
• To understand the relationship of cementum, periodontal ligament, and alveolar bone
• To understand how the fibers of the periodontal ligament function in tooth movement and shock absorption
GINGIVAL UNIT
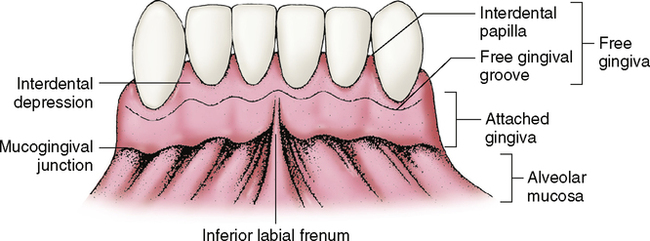
The gingiva is made up of free and attached gingiva (Fig. 8-1). Composed of very dense mucosa called masticatory mucosa, it has a thick epithelial covering and keratinized cells. The underlying mucosa is composed of dense collagen fibers (Table 8-1). This type of masticatory mucosa is also found on the hard palate. Masticatory mucosa is well designed to withstand the trauma to which it is subjected in grinding food.
Table 8-I
Characteristics of Gingiva and Alveolar Mucosa
| Tissue Characteristics | Free and Attached Gingiva | Alveolar Mucosa |
| Type of mucosa | Masticatory | Lining |
| Tone | Tightly bound | Movable and elastic |
| Epithelium | Thick epithelial layer | Thin epithelial layer |
| Keratinized | Nonkeratinized | |
| Rete peg formation | No rete peg formation | |
| Texture | Stippled surface (like an orange peel) | Smooth |
| Color | Light pink | Red to bright red |
| Fiber | Collagenous fibers | Collagenous fibers and elastic fibers |
Attached Gingiva
The gingiva is connected to the tooth by a meshwork of collagenous fibers. These fibers are formed by fibroblasts, which are the principal cells of connective tissue. All fibers embedded in the cementum are known as Sharpey’s fibers; they extend from the cementum to the papillary area of the gingiva. These fibers pass out from the cementum in small bundles (Fig. 8-2, A). Some of the fibers (A) curve toward the mucosa of the free gingiva and interlace with one another. Other fibers (B) pass directly across from the cementum to the gingiva. Still further apically, other fibers (C) pass from the cementum over the alveolar crest and turn apically between the outer periosteum of the alveolar process and the outer epithelial covering of the attached gingiva.
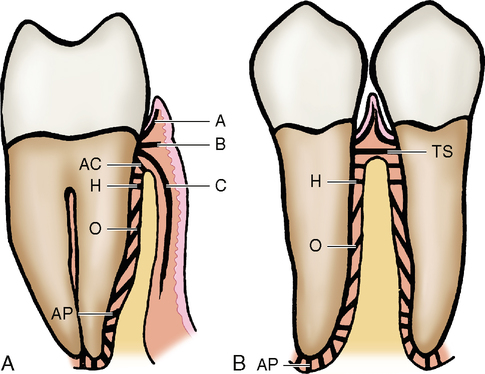
On the proximal side (Fig. 8-2, B), the connective tissue fibers arise from a higher level on the cementum because of the curvature of the CEJ on the interproximal surfaces of the teeth. This curvature allows more room for the cementum to attach to the gingiva. Attachment is made possible by/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses