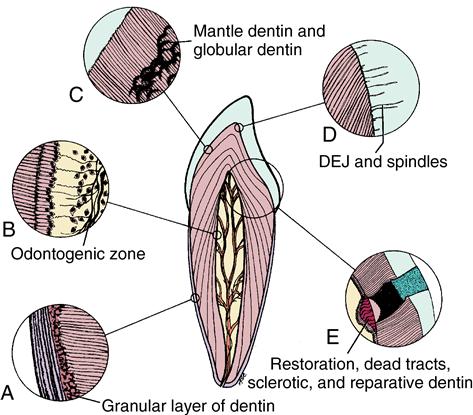
Dentin
Learning objectives
■ Describe the various types of dentin and the structures they contain.
■ Describe the dental process that lies in the dental tubules.
■ Discuss the relationship of the enamel to the dentin at their junction.
Key terms
Canaliculi
Dead tracts
Dentin: circumpulpal, globular, granular, interglobular, intratubular, mantle, peritubular, primary, reactionary/response, reparative, response, sclerotic, secondary, tertiary, transparent
Granular layer, granular layer of Tomes
Imbrication lines
Incremental lines
Interglobular spaces
Lines of von Ebner
Neonatal line
Osteodentin
Predentin
S curve
Smear layer
Overview
This chapter focuses on dentin, the hard tissue that constitutes the body of the tooth. Dentin is a living, sensitive tissue not normally exposed to the oral environment. Root dentin is covered by cementum, and crown dentin is covered by enamel. Dentin, like bone, is composed primarily of an organic matrix of collagen fibers and the mineral hydroxyapatite. It is classified as primary, secondary, or tertiary on the basis of the time of its development and the histologic characteristics of the tissue. Primary dentin is the major component of the crown and root and consists of mantle dentin, globular dentin, and circumpulpal dentin. Mantle dentin is deposited first, along the dentinoenamel junction, in a band about 150 μm wide and is mineralized by matrix vesicles and not a mineralization front. Mantle dentin does not contain dentin sialoprotein (DSP) or dentin phosphoprotein (DPP) in the mineralizing extracellular matrix. It is thought that mantle dentin is secreted by immature odontoblasts. The collagen fibers of this dentin are larger than those of the circumpulpal dentin, which forms later. Mantle dentin is separated from the circumpulpal dentin by a zone of disturbed dentin formation called globular dentin, which is noted because of the spaces between the globules, termed interglobular spaces. Globular dentin is believed to be a result of deficient mineralization caused during the final maturation of the odontoblast. Dentin continues to form, although the collagen fibers are smaller, until the teeth erupt and reach occlusion. As the teeth begin to function, the dentin is termed secondary dentin and is normal circumpulpal dentin. Dentin is responsive to the environment. When caries or mechanical trauma affects the pulp, dentin is deposited underlying that area and is termed reactionary/response, reparative, or tertiary dentin. This dentin is deposited to protect the pulp. Bordering the pulp is predentin, which is newly formed dentin before calcification and maturation. Predentin is composed of 90% type I collagen fibers and 10% noncollagenous proteins, which calcify within 24 hours as the odontoblasts deposit a new band of collagen fibers (Box 8-2).
In addition to classifying dentin, this chapter describes properties and characteristics of dentin. Like osteoblasts that form bone, the odontoblasts that form dentin lie on the surface of the forming hard tissue. Unlike bone, the odontoblastic processes exist in tubules and penetrate the dentin from the pulp to the dentinoenamel junction. Dentin, like bone, is deposited by appositional growth and produces incremental lines, but unlike bone, dentin does not remodel. In addition, a granular dentin anomaly appears along the root surface. This anomaly may also be caused by the cementum that forms adjacent to the root dentin during development. The odontoblasts may die because of trauma or old age, and dead tracts then develop in dentin. The tubules may later calcify as they fill with mineral. When this occurs, the dentin is termed sclerotic or transparent dentin.
Physical properties
Dentin, which forms the bulk of the tooth, is yellowish in contrast to the whiter enamel. It appears darker if a root canal procedure has been performed. Dentin is composed of 70% inorganic hydroxyapatite crystals, 20% organic collagen fibers with small amounts of other proteins, and 10% water by weight. With 20% less mineral than enamel, dentin is softer, although it is slightly harder than bone or cementum. Therefore it is more radiolucent than enamel but much more dense or radiopaque than pulp. Dentin is resilient or slightly elastic, and this allows the impact of mastication to occur without fracturing the brittle overlying enamel. This resilience is partly the result of the presence throughout the matrix of tubules, which extend from the dentinoenamel junction to the pulp.
Dentin classification
Dentin includes primary, secondary, and tertiary dentin. Based on structure, primary dentin is composed of mantle and circumpulpal dentin. Examples of these classifications are given in Fig. 8-1, A. Fig. 8-1, B, shows the S curve of the dentinal tubules through primary and secondary dentin. Primary dentin forms the body of the tooth; secondary dentin forms only after tooth eruption and is a narrow band that borders the pulp. Tertiary or reparative dentin is formed only in response to trauma to the pulp (Box 8-1).
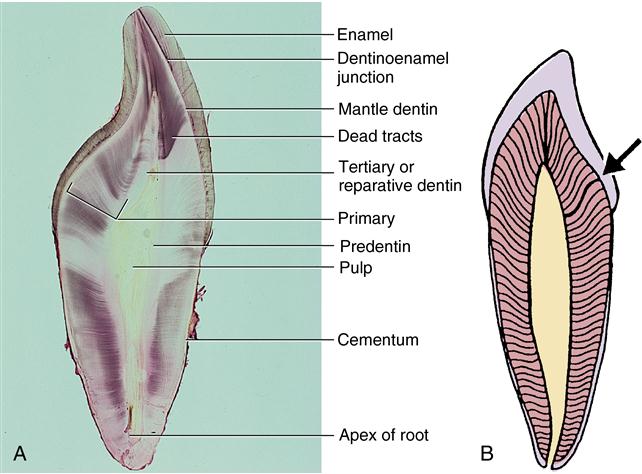
A, Incisor tooth section illustrating structures in enamel, dentin, and cementum. B, Diagram of dentin showing S curvature of the dentinal tubules, especially at the arrow. (Modified from Avery JK: Oral development and histology, ed 3, Stuttgart, 2002, Thieme Medical.)
Primary dentin
Mantle dentin is the first primary dentin formed. It is deposited first at the dentinoenamel junction (Fig. 8-2) and extends approximately 150 μm from the junction pulpward to the zone of interglobular or globular dentin. Mantle dentin is so named because it serves as a covering or mantle over the rest of the dentin. Normal circumpulpal dentin directly underlies mantle and globular dentin and comprises the bulk of the tooth’s primary dentin. Circumpulpal dentin may be 6 to 8 mm thick in the crown and a little thinner in the roots.

Area bounded by dentinoenamel junction above and interglobular dentin below.
Zones of dentin have structural differences. Mantle dentin is composed of large collagen fibers, some of which are 0.1 to 0.2 μm in diameter, in contrast to the circumpulpal dentinal matrix, which is 50 to 200 nanometers (nm). Thus the fibers in circumpulpal dentin are 10 times smaller than those in mantle dentin. Mantle dentin is also slightly less mineralized and contains fewer defects than circumpulpal dentin. Mantle dentin is nearly free of developmental defects. It interdigitates with enamel at the scalloped dentinoenamel junction peripherally and in the zone of globular dentin centrally. The area of globular dentin usually exists only in the crown but may extend into the root. Such a zone of dentinal matrix is not completely mineralized, and the area of globular calcospherites has not fused correctly (see Fig. 8-2 and Fig. 8-3, C).
Globular dentin contains hypomineralized areas between the globules, termed interglobular spaces. Fig. 8-3 shows examples of various structures in dentin. Interglobular spaces are not true spaces but are less mineralized areas between the calcified globules. The dentinal tubules run without interruption through this zone, indicating a defect in mineralization, not a defect in matrix formation (see Fig. 8-2). Interglobular dentin is especially noticeable with vitamin D deficiency, which affects mineralization of teeth and bones. Primary dentin constitutes the bulk of dentin in crowns and roots of teeth. It is characterized by the continuity of tubules from pulp to dentinoenamel junction and by incremental lines that indicate a daily rhythmic deposition pattern of approximately 4 μm of dentin.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses