7
Temperature regulation
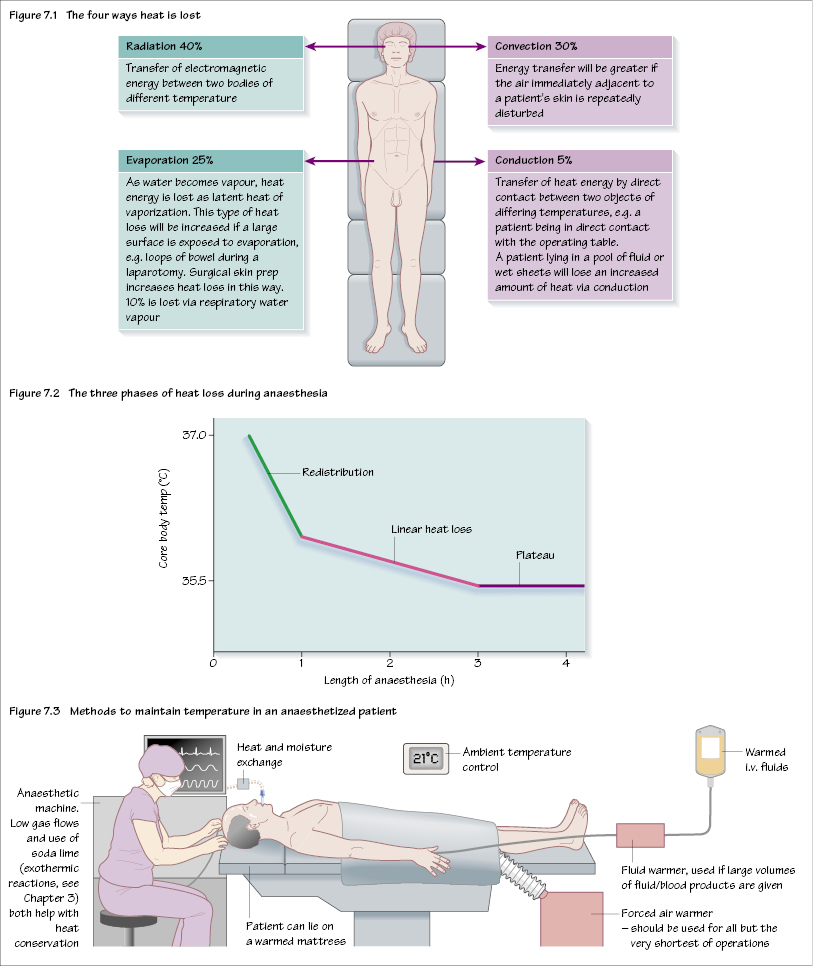
Patients lose heat during the perioperative period. Heat loss can start on the ward or during transfer to the theatre suite, especially if wearing only a thin theatre gown. It is more common in children, especially babies, as they have a larger surface area to body mass ratio.
Hypothermia in this setting is defined as a core temperature <36.0°C. If a patient’s preoperative temperature is <36°C then active warming measures should be instituted. Anaesthesia should be delayed for elective cases until the temperature is >36°C.
The body loses heat in four ways: radiation, convection, evaporation and conduction (Figure 7.1).
Afferent information is conducted from the skin’s thermoreceptors (hot and cold) to the anterior hypothalamus. Efferent responses are relayed via the posterior hypothalamus.
Autonomic control of temperature is mediated by:
- shivering;
- non-shivering thermogenesis, which occurs in brown adipose tissue (sympathetic); a large amount exists in neonates but only a small amount in adults, where it contributes <10–15% of heat production;
- sweating;
- changes in peripheral vascular smooth muscle tone.
Factors contributing to heat loss during anaesthesia are:
- alteration of autonomic control;
- peripheral vasodilatation, e.g. by volatile anaesthetics;
- use of surgical skin prep;
- exposed surgical site (e.g. laparotomy);
- removal of behavioural responses, e.g. clothes etc.;
- poor nutritional status/thin patients with a paucity of insulating fat.
Effect of anaesthesia on temperature control
Central control within the hypothalamus is altered so that heat-conserving measures are triggered at a lower temperature and heat-losing processes are initiated at a higher temperature. Impairment of thermoregulatory responses causes three phases of heat loss during anaesthesia (Figure 7.2):
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


