18
Obstetric anaesthesia
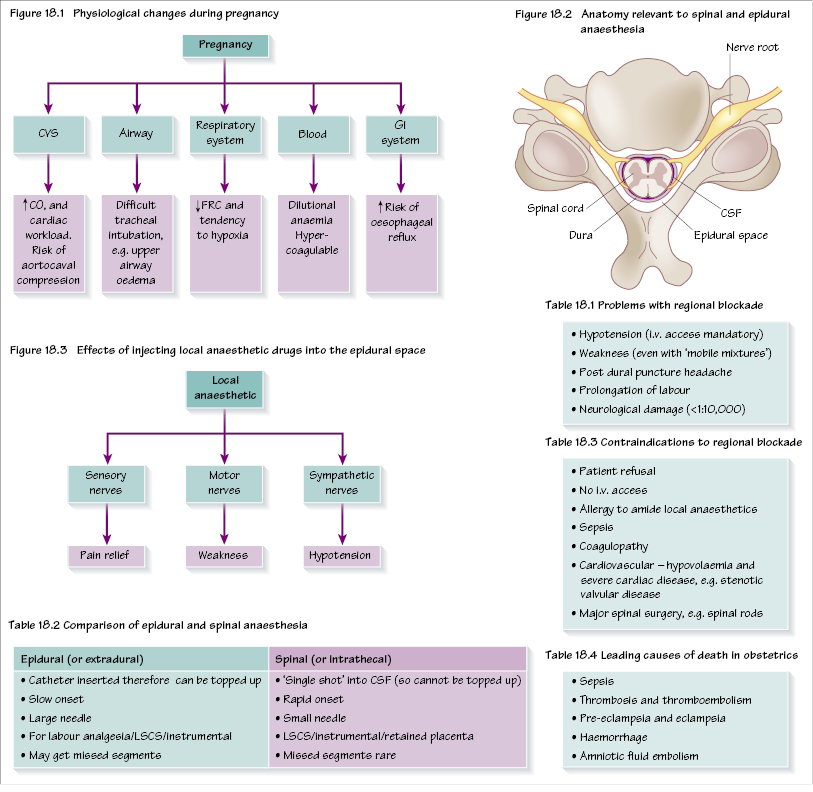
Many of the physiological changes that take place in pregnancy are of relevance to all obstetric anaesthesia (Figure 18.1). There are a variety of methods of pain relief in labour (e.g.TENS, entonox and pethidine) that are provided without anaesthetic input. Methods with anaesthetic input are described in this chapter.
Epidurals for pain relief in labour
Epidurals provide excellent segmental analgesia. The anatomy of the spinal and epidural spaces is shown in Figure 18.2.
What solution is used in the epidural?
Local anaesthetics (LA) were used on their own for many years. The effects of injecting local anaesthetic drugs in to the epidural space is shown in Figure 18.3. Bupivacaine is the only LA used as it is long acting and has low transfer to the fetus. Some of the side effects, particularly leg weakness, can be reduced by adding an opioid (commonly fentanyl) to the LA, which also enhances analgesia. This LA/opioid mixture was popularized as the mobile epidural.
What are the side effects/risks? (Table 18.1, Figure 18.3)
- Hypotension from sympathetic block.
- Weakness (much less with mobile mixtures).
- Urinary retention may occur.
- Headache from accidental dural puncture, which has an incidence of about 0.6%. The resultant CSF leak causes a severe headache, which will often require a blood patch – a repeat epidural injection at a later date in which blood is injected.
- Catheter misplacement so that the injectate goes not into the epidural space but into the CSF or intravenously. The former will cause a total spinal anaesthesia from head to toe, together with total paralysis and loss of consciousness. The latter will cause cardiac arrhythmias which are often refractory to treatment, although l-bupiviacaine is a safer isomer than the st/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


