7
Orthodontically driven corticotomy: Tissue engineering to expand the basal bone, modify the periodontal biotype and lowering the risks of orthodontic damage to the periodontium
Federico Brugnami1 and Alfonso Caiazzo2,3
1 Private Practice Limited to Periodontics, Oral Implants and Adult Orthodontics, Piazza dei Prati degli Strozzi 21, Rome, Italy
2 Department of Oral and Maxillofacial Surgery, Boston University Henry M. Goldman School of Dental Medicine, Boston, MA, USA
3 Centro Odontoiatrico Salernitano, Via Bottiglieri 13, Salerno, Italy
Introduction
Orthodontic movements and gingival recession have always been a clinical concern. Wennstrom et al. (1996), in talking about tooth movement within the arch, stated that “a more lingual positioning of the tooth results in an increase of the gingival height on the facial aspect with a coronal migration of the soft tissue margin. The opposite will occur when changing to a more facial position in the alveolar process.” When the tissue is apical to the cemento-enamel junction (CEJ) it is called gingival recession. Some unpublished data suggests that there is a higher incidence of gingival recession in patients orthodontically treated for transverse discrepancy (Graber et al., 2005). On the other hand, other studies failed to correlate expanding movement and vestibular recessions. Bassarelli et al. (2005) studied stone models before and after treatment and found no higher incidence of increased length of clinical crown. One other study from the same group concluded that even in case of proclination of mandibular incisors there was no correlation between orthodontic treatment and development of vestibular recession. Anyway, they included a thin biotype as a predictor of gingival recession in proclination of mandibular incisors (Melsen and Allais, 2005). In both studies the analysis was performed right at the end of orthodontic treatment, thus limiting the possibility to intercept a late manifestation of apical migration of the gingival margin. One possible theory is that orthodontics per se is not creating a recession but it may create a marginal bone resorption if the tooth is moved outside the bony envelope of the alveolar process (Wennstrom, 1996). This may be observed, for example, in untreated patients with crowding. In these cases the discrepancy between the mesio-distal teeth’s size and the space available may force some of the teeth outside the bony alveolar housing. Staufer and Landmeser (2004) showed that, in cases of more than 5 mm of crowding, gingival recession of more than 3.5 mm was 12 times more likely to occur. This may not be irreversible as previously thought. In a recent case report, a non-surgical correction of multiple recession “was accomplished by orthodontically moving teeth more into alveolar bone and by taking more careful oral hygiene measures” (Northway, 2013) (Figures 7.1–7.5).
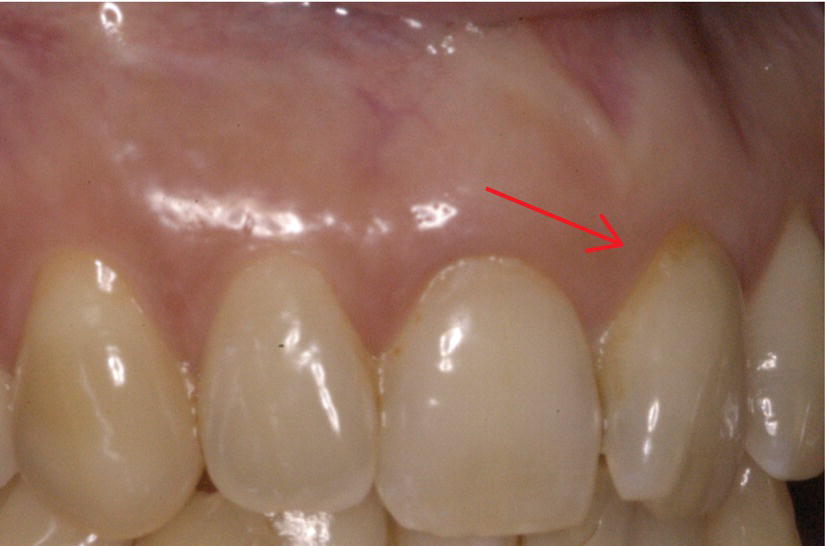
Figure 7.1 Upper left central incisor showing gingival recession. Although the recession may look small, its surgical treatment may give unpredictable results. Owing to the lack of inter-proximal mesial bone support caused by the rotation of the tooth, this defect falls in class III according to the Miller classification.
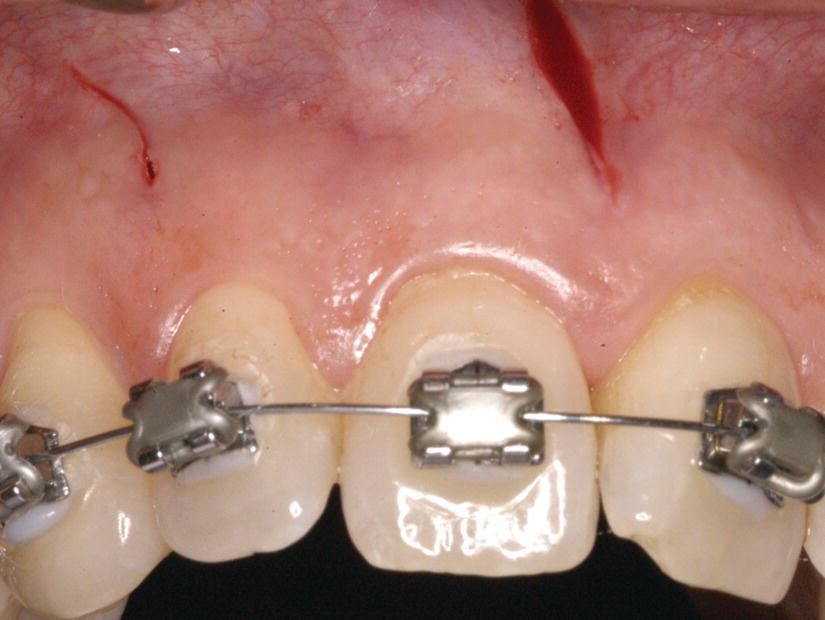
Figure 7.2 The patient was treated with the principle of Piezocision® (Chapter 5), with no bone graft.
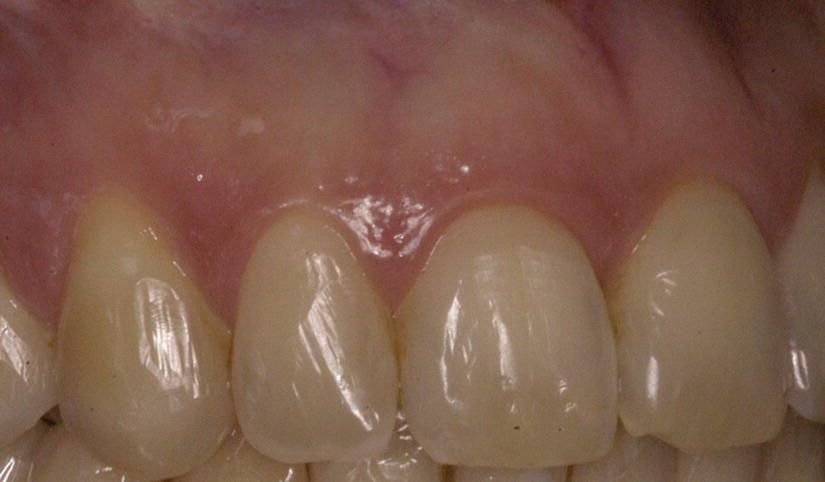
Figure 7.3 De-rotation of the tooth and spontaneous resolution of the muco-gingival defect, at the end of treatment.
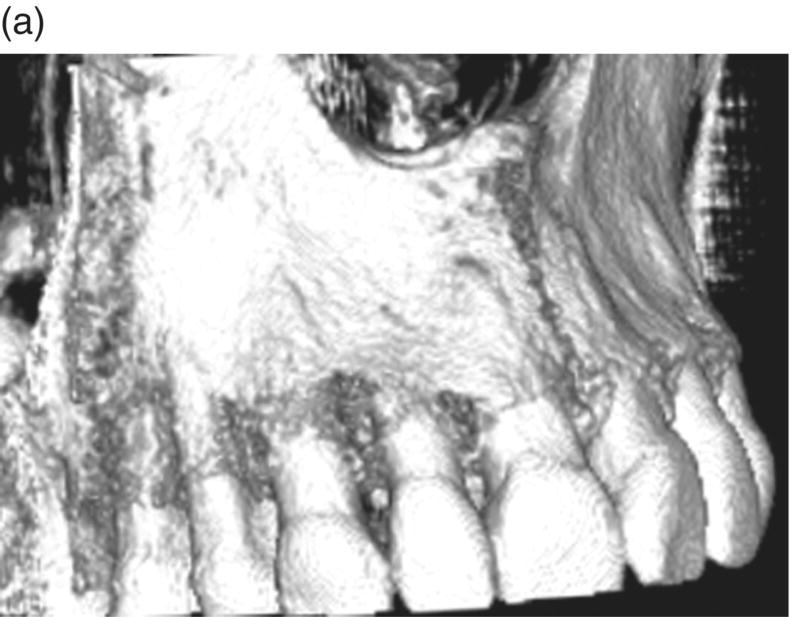
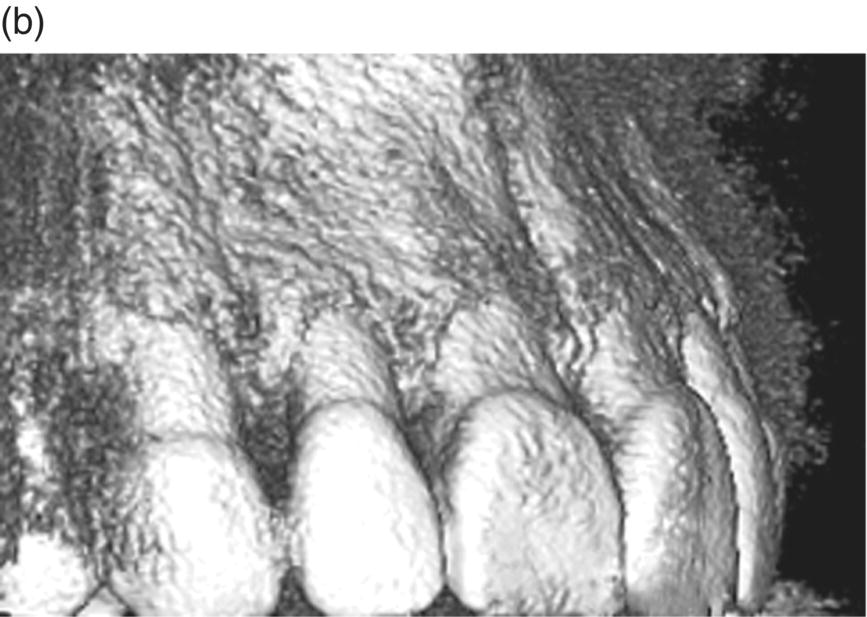
Figure 7.4 (a) 3D reconstruction area:The pre-treatment cone-beam computed tomography (CBCT) confirms the lack of bone support at the mesial line angle of the upper left central incisor. It also shows a very thin buccal plate in all the pre-maxilla, and some dehiscences. (b) The post-treatment CBCT shows the presence of bone support at the mesial line angle of the incisor, after his de-rotation and more proper 3D positioning of the root in the alveolar bony housing.
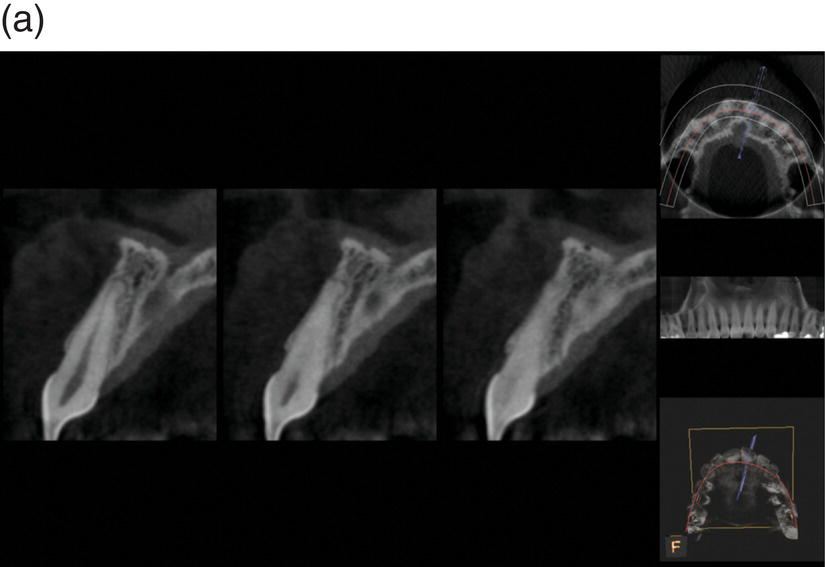
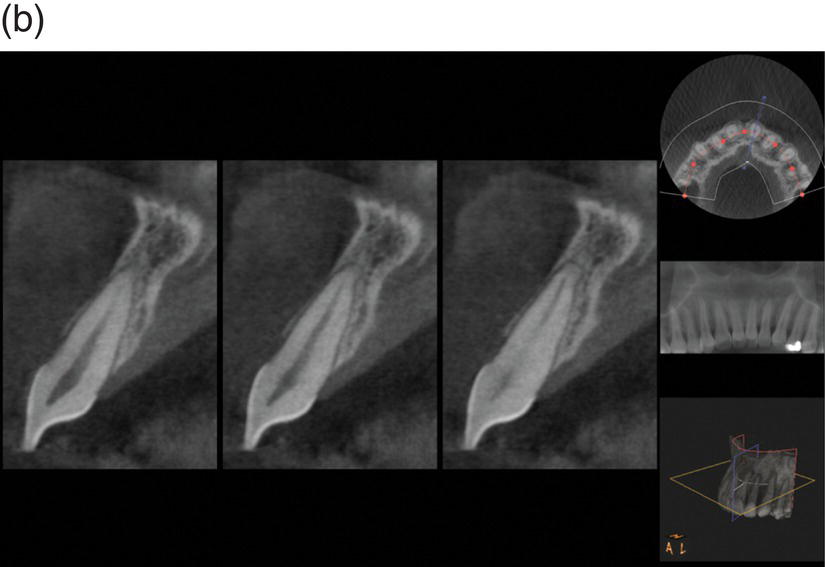
Figure 7.5 (a) Bidimensional axial view of the incisor. The pre-treatment shows a very thin buccal plate and the presence of a dehiscence. (b) The post-treatment showed a resolution of the dehiscence, due to a more centered 3D position of the root in the alveolar bony housing.
This confirms the importance of achieving proper tridimensional positioning of the roots inside the bony alveolar housing after orthodontic treatment. Gingival recession may eventually become evident only if an inflammatory process (traumatic and/or infective) starts the disruption of the gingival attachment. Therefore, we may expect to visualize the incidence of recessions only some time after treatment (Figure 7.6).
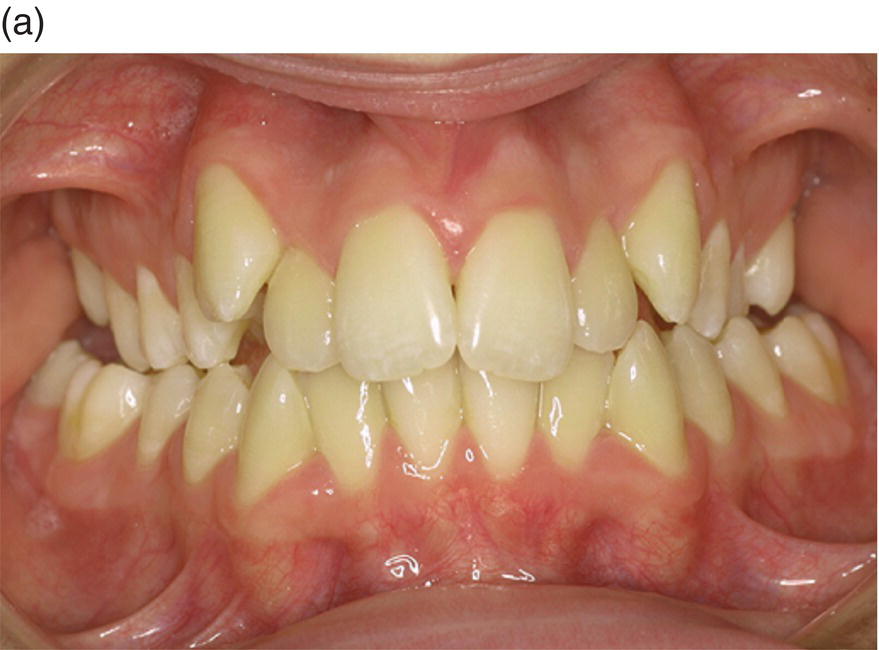
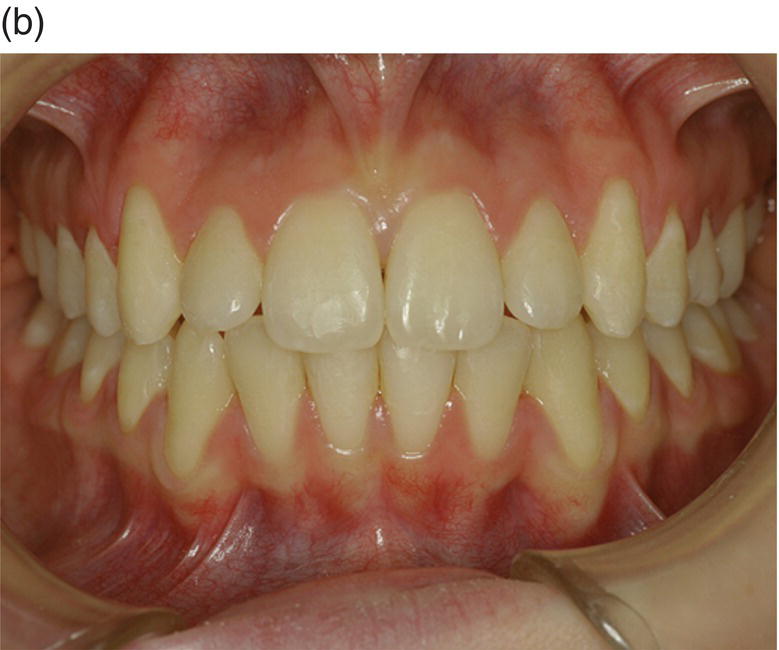
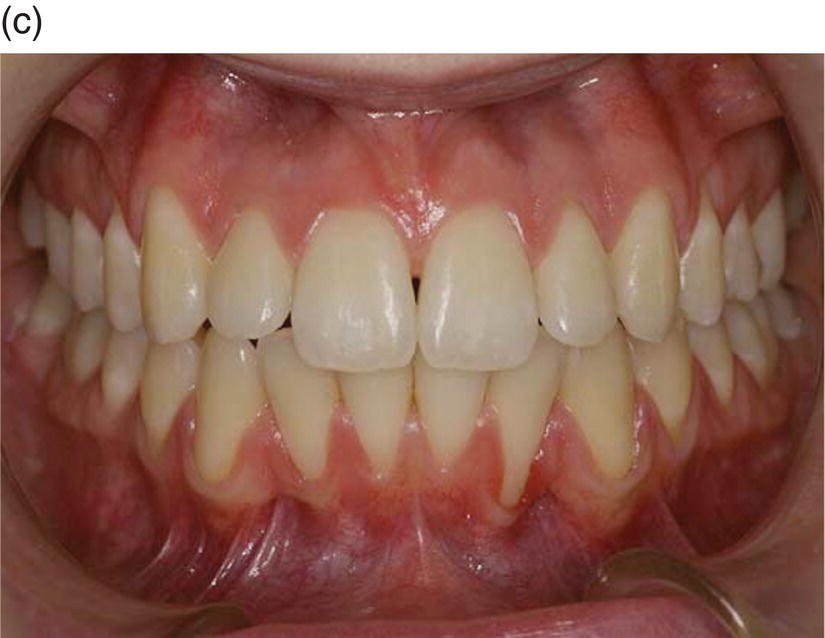
Figure 7.6 (a) A 14-year-old female presented with a sleletal class I, dental class II, with increased overjet, crowding and a transverse deficiency as seen in the frontal initial photograph. She was treated with rapid palatal expansion follow by low-friction attachment to expand the upper maxilla and solve the crowding. Owing to her flat profile and thin upper lip, it was decided to avoid extractions and over-proincline the incisors to solve the overjet. (b) At the end of treatment (26 months) a proper occlusion was achieved. The overjet went from −5 mm to −2 mm. Although the inclination of the lower incisors passed from a 1 inf − GoGn value of 90° to 102°, the periodontal tissue looked very thin, but no signs of gingival recession were yet visible. The periodontal situation remained stable at the 1 year follow-up. (c) At the 2 year follow-up, although the overjet rebounded to −2.5 mm and 1 inf − GoGn to 92°, gingival recession started to become evident.
(Courtesy of Dr Roberto Ferro, Clinical Director “Unità Operativa Autonoma di Odontoiatria AULSS n 15 Regione Veneto” – Cittadella (Pd), Italy.)
A more recent study by Renkema et al. (2013) evaluated the long-term development of labial gingival recession during orthodontic treatment and retention phase. In this retrospective case–control study on stone models the percentage of subjects with recession was consistently higher in cases than in controls. The presence of gingival recession was scored (Yes or No) on plaster models of 100 orthodontic patients (cases) and 120 controls at the age of 12 (T12), 15 (T15), 18 (T18), and 21 (T21) years. In the treated group, T12 reflected the start of orthodontic treatment and T15 the end of active treatment and the start of retention phase with bonded retainers. Overall, the odds ratio to have recessions for orthodontic patients compared with controls is 4.48 (p < 0.001; 95% confidence interval: 2.61–7.70). In particular, the lower incisors seem to be more at risk:
“Our results suggest that lower incisors are particularly vulnerable to the development of recessions in orthodontic patients. For example, 31% of the cases and 16.7% of the controls demonstrated at least 1 recession site at T21 (in all the teeth except lower incisors, ratio – 2:1), whereas 13% cases and 1.7% controls had at least 1 lower incisor with a recession at T21 (ratio – 8:1)”.
They concluded that “orthodontic treatment and/or the retention phase may be risk factors for the development of labial gingival recessions,” while “mandibular incisors seem to be the most vulnerable to the development of gingival recessions.”
Radiographic evaluation of orthodontic side effects
Most studies on alveolar bone changes in patients who have undergone orthodontic treatment have used bitewing and/or periapical radiography, thus restricting the assessments to proximal bone surfaces (Hollender et al., 1980; Bondemark,1998; Janson et al., 2003). Low-dose, high-quality CBCT is now becoming readily available, offering the possibility of evaluating bone changes in every dimension (Fuhrmann, 1996). During orthodontic tooth movement, teeth may be repositioned beyond the bony alveolar housing with resultant dehiscence and fenestration formation (Sarikaya et al., 2002).
Lund et al. (2012), using CBCT, investigated in 152 patients the distance between the CEJ and the marginal bone crest (MBC) at buccal, lingual, mesial, and distal surfaces from central incisors to first molars in adolescents before (baseline) and after extractive orthodontic treatment (study end point). Patients with class I malocclusion, crowding, and an overjet of 5 mm were examined with a CBCT unit using a 60 mm × 60 mm field of view and a 0.125 mm voxel size. Lingual surfaces, followed by buccal surfaces, showed the largest changes. Eighty-four percent of lingual surfaces of mandibular central incisors exhibited a bone-height decrease of >2 mm (Figure 7.7).
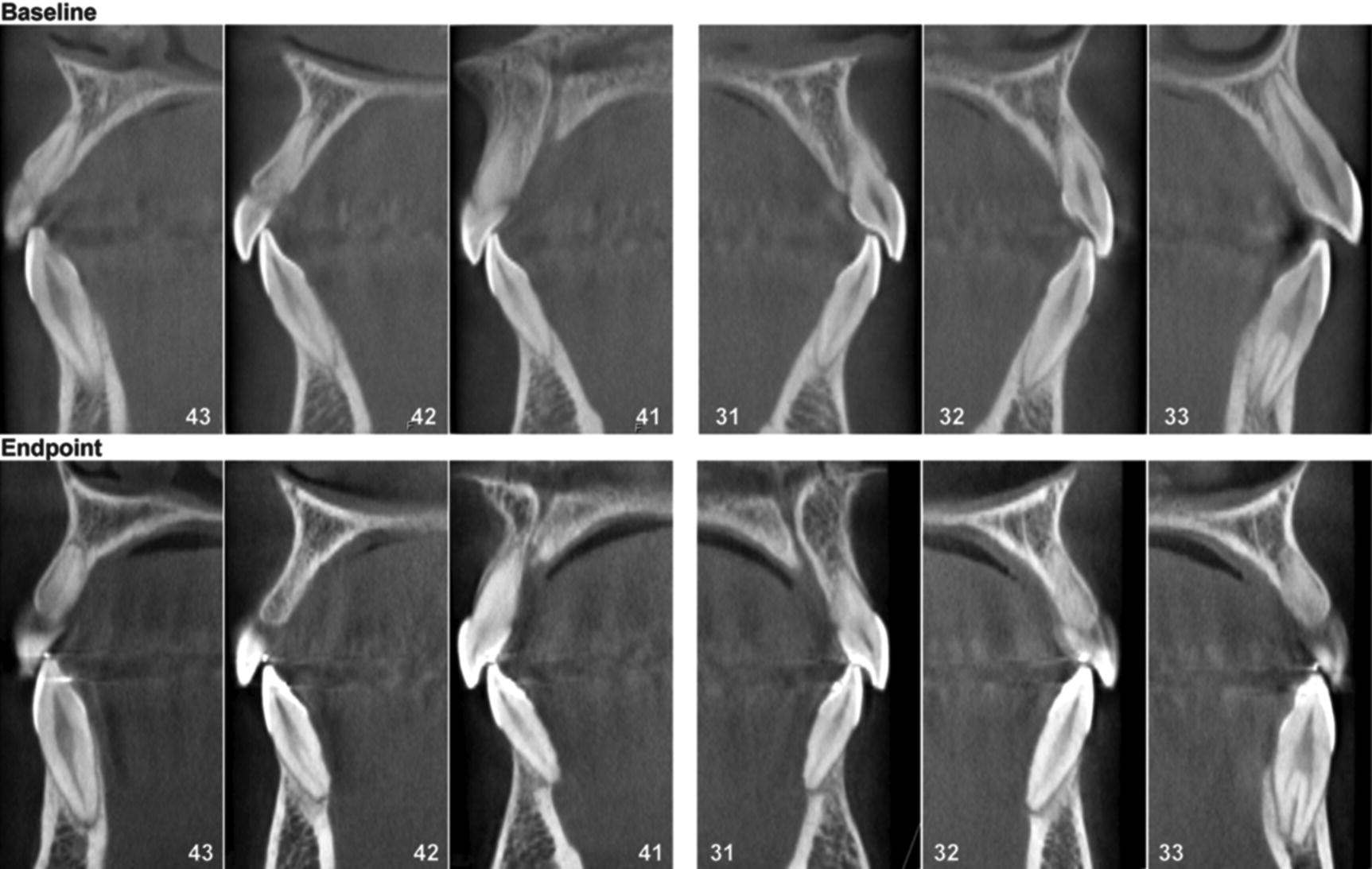
Figure 7.7 Sagittal images of mandibular frontal teeth (43–33) from a patient showing a large increase in the distance from the CEJ to the MBC between baseline and the study end point. Teeth numbered according to Federation Dentaire Internationale (FDI).
(Reprinted from Lund et al. (2012), with permission from Wiley.)
They concluded that “while some differences may be explained by reasons other than the orthodontic treatment per se, it seems likely that loss of marginal bone height, at least in the short-term, can be a side effect of extractive orthodontic treatment for a specific type of malocclusion, where retraction of teeth in anterior jaw regions causes remodeling of the alveolar bone.” Garib et al. (2006) also showed a correlation between rapid palatal expansion and thinning of the vestibular plate up to almost 1 mm. This confirmed what was already stated before the advent of Periodontally Accelerated Osteogenic Orthodontics® (PAOO®): the buccal plate of the alveolus may be considered inviolable and any movement beyond that line might cause bony dehiscence and eventually a gingival recession (Engelking and Zachrisson, 1982). The revolutionary PAOO modifies this vision and the concept can be stretched to the point that, according to Williams and Murphy (2008), “the alveolar ‘envelope’ or limits of alveolar housing may be more malleable than previously believed and can be virtually defined by the position of the roots,” as will be outlined by the following case (Figure 7.8).
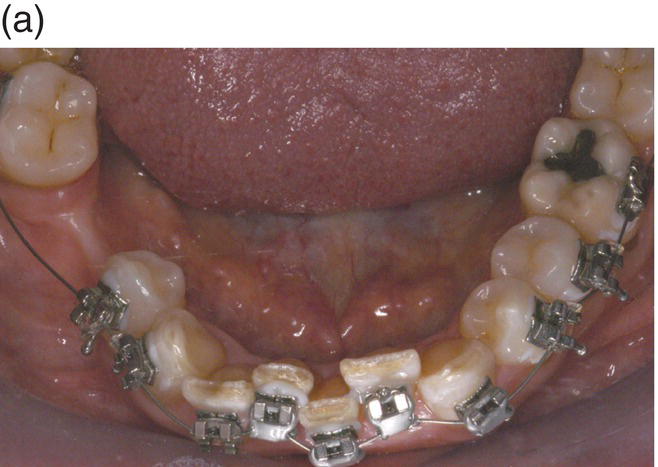
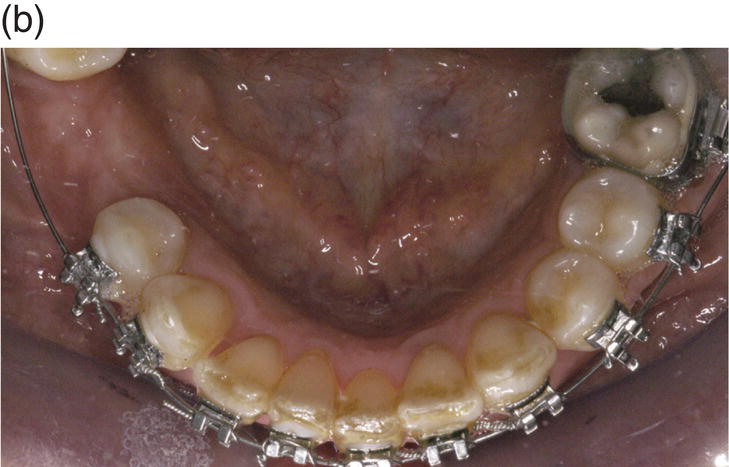
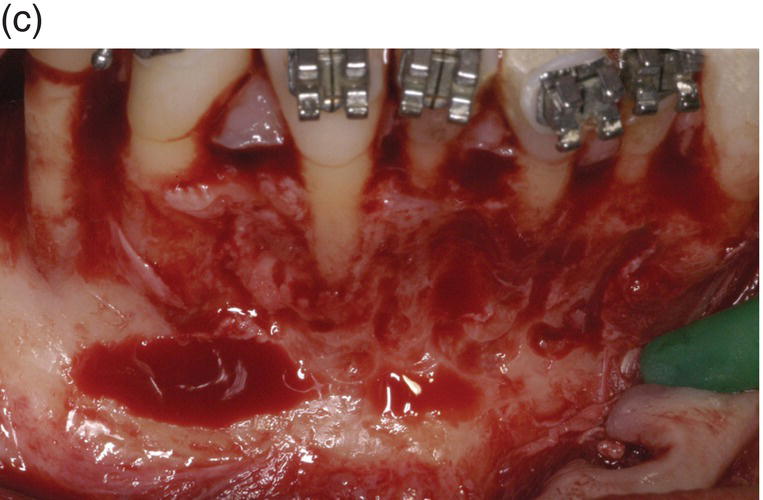
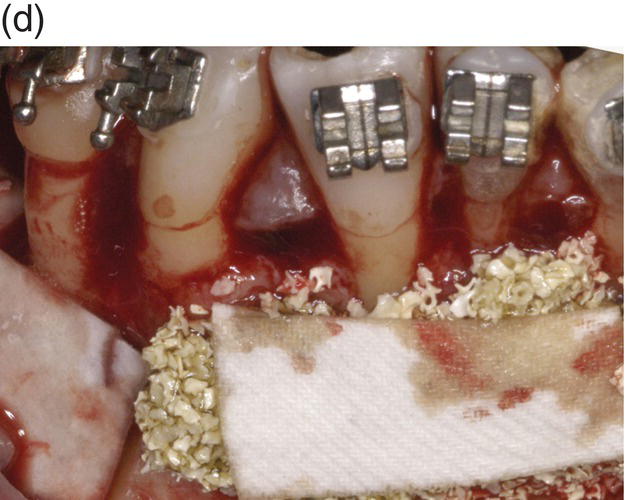
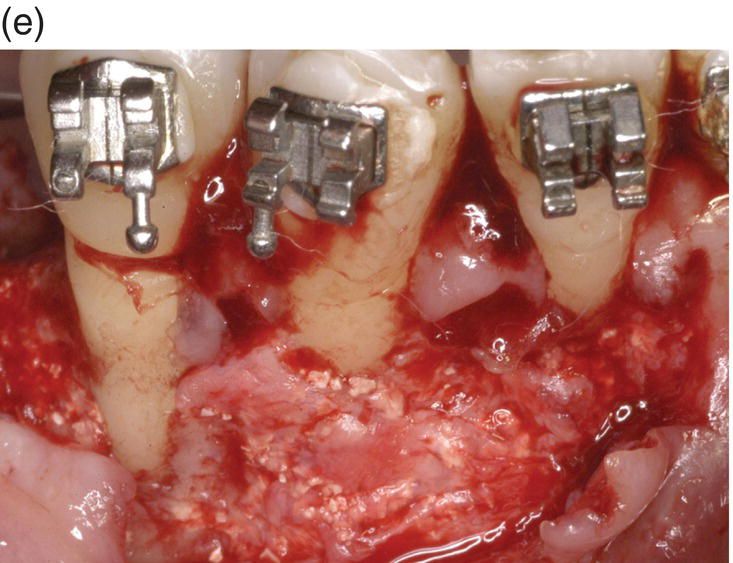
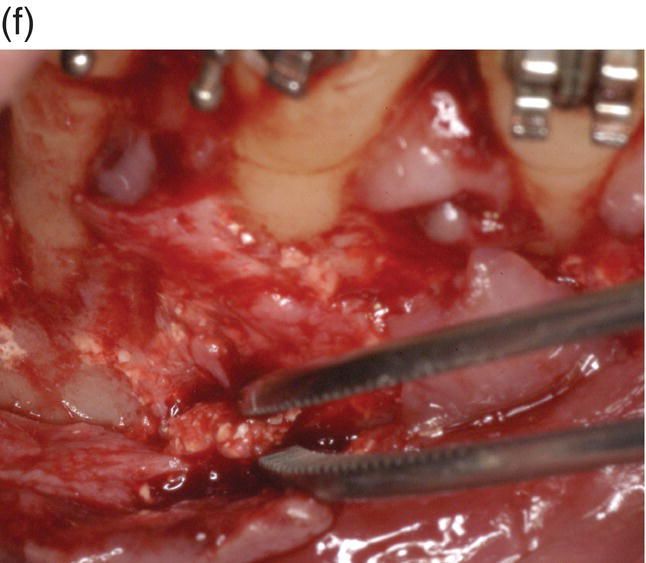
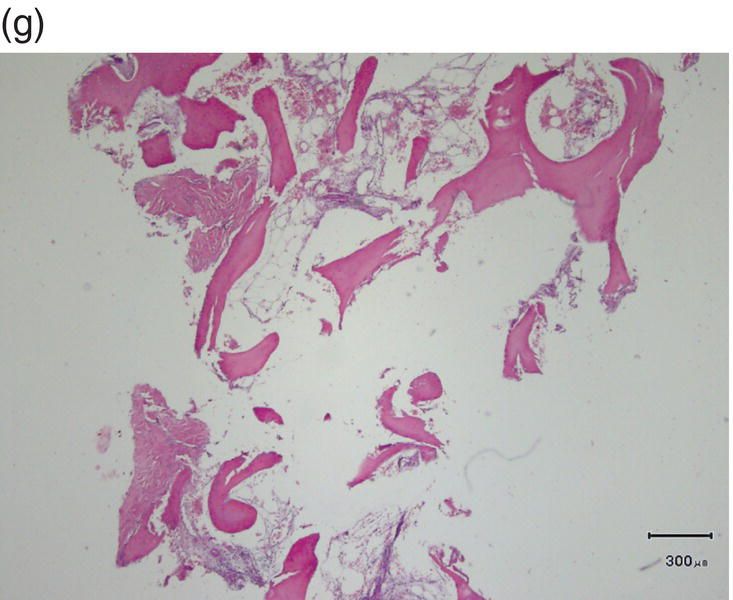
Figure 7.8 (a) Occlusal view at the beginning of treatment. (b) Decrowding 28 days after surgery. (c) Flap elevation and bone exposure recessions on several teeth should be noted. (d) Grafting material and membrane insertion. (e) At 6 months re-entry a coverage of the dehiscence treated with graft and membrane can be noted. (f) Biopsy of the site. (g) Histology showing a prominent bone marrow portion with some fibrous connective tissue and mature bone for 35% of the core area.
A 42-year-old white female presented with a class II division I malocclusion, deep bite, and severe crowding in the lower jaw. Clinical examination revealed an edentulous and severely atrophic mandibular alveolar ridge and missing teeth nos. 24 and 25.
As the patient desired rehabilitation of the edentulous areas with implant-supported restorations, she was informed that bucco-lingual ridge augmentation would be required. It was possible to perform the ridge augmentation, including the harvesting of autologous bone, and the corticotomy in one combined surgical procedure. The exposure of the alveolar bone level showed an unexpected, although not unusual, situation: large fenestrations (hidden recession) on teeth nos. 26 (lower right lateral) and 28 (first lower right premolar). A very thin buccal plate on the lower right canine (no. 27) and a smaller fenestration of the lower central left incisor (no. 24) were also noted. In the anticipated resolution of the crowding, teeth nos. 26 and 24 were expected to remain in the same position or slightly move buccally, tooth 27 to move buccally and tooth 28 to move mainly distally and slightly buccally.
Corticotomy was performed with a surgical round bur under copious irrigation, with a scalloped design around the roots of the teeth, until bleeding from the marrow was noticed. Bone thinning was refined with a manual bone-scraping instrument that also acted as collector of autologous bone graft needed to be placed over the deficient contiguous ridge. The autologous graft in the edentulous area was covered with a layer of xenogeneic bone (Endobone, Biomet Palm Beach Gardens, FL, USA) and with a resorbable membrane (Osseoguard, Biomet Palm Beach Gardens, FL, USA). The xenogeneic bone was also placed over the buccal plate in the anterior sextant where corticotomy was performed, with particular care to ensure coverage of the areas with dehiscence of the roots. In the region of tooth no. 26, a resorbable membrane was used to cover the osseous defect following the principles of conventional guided tissue regeneration (GTR) technique, while the recession over no. 28 was left uncovered by both graft and membrane to act as a control.
Six months after surgery, an endosseous implant was placed into the augmented edentulous area. The design of the flap was extended mesially, offering a chance to visually control the right quadrant where corticotomy was performed: regeneration of the bony dehiscence overlying tooth no. 26 (lower right lateral) was evident, while the control (tooth no. 28, first lower right premolar) remained unchanged, confirming the importance of combination of the corticotomy with a regenerative procedure (guided bone regeneration (GBR) and/or GTR). The buccal plate on tooth no. 27 also appeared augmented in thickness despite a movement outside the original bony envelope.
In the area of tooth no. 27 a fragment of tissue was harvested with a blade. The result showed a prominent bone marrow portion with some fibrous connective tissue and mature bone for 35% of the core area.
Research experience
Aim of the study
Bone resorption occurs in the direction of tooth movement. The reduced volume of the alveolar bone, sometimes with minimal thickness and sometimes non-existent, is a complicating factor for orthodontic treatment. Previous 3D CBCT studies have shown a great incidence of bone marginal resorption in those areas where the movement was carried out toward the cortical plate (Lund et al., 2010). Corticotomy has shown the ability to expand the alveolar basis (Wilcko et al., 2008), potentially minimizing the risk of bone dehiscence and fenestrations as side effects of orthodontic movement outside the original bony envelope.
Material and methods
This retrospective evaluation included 20 adult patients (age 13–58 years, mean 45 years) treated in two private offices, with a combination of orthodontics and corticotomy, with or without bone graft. For the nature of their malocclusion, the treatment plan included a movement of one or more teeth, toward the cortical plate on the buccal (i.e., expansion of upper arch or proclination of the lower inferior) or lingual (i.e., extraction cases with anterior retraction) surfaces for a total of 142 teeth. In one case a 6-month re-entry was possible, allowing a visual comparison of treated and untreated areas, regeneration of previously missing buccal plate (dehiscence), and harvesting of a bone biopsy for histologic analysis (Figure 7.8f and g). In two cases a 5-year CBCT follow-up was available (Figure 7.9).
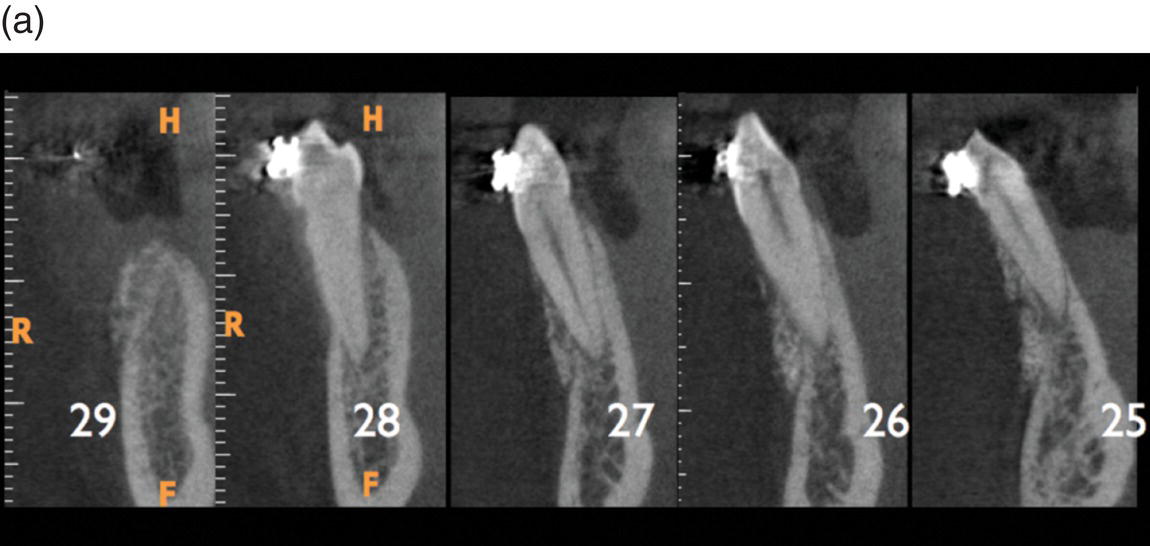
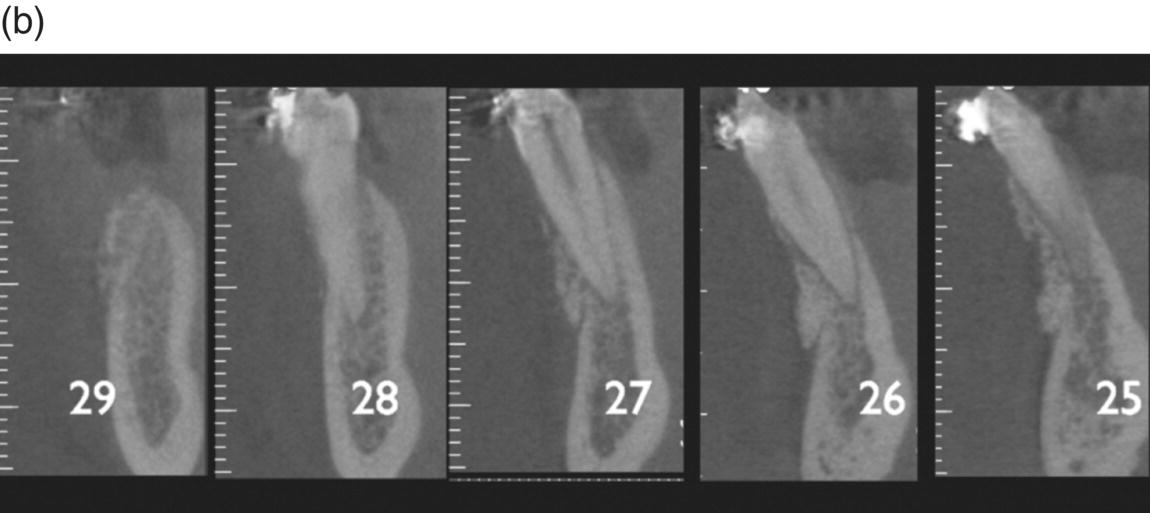
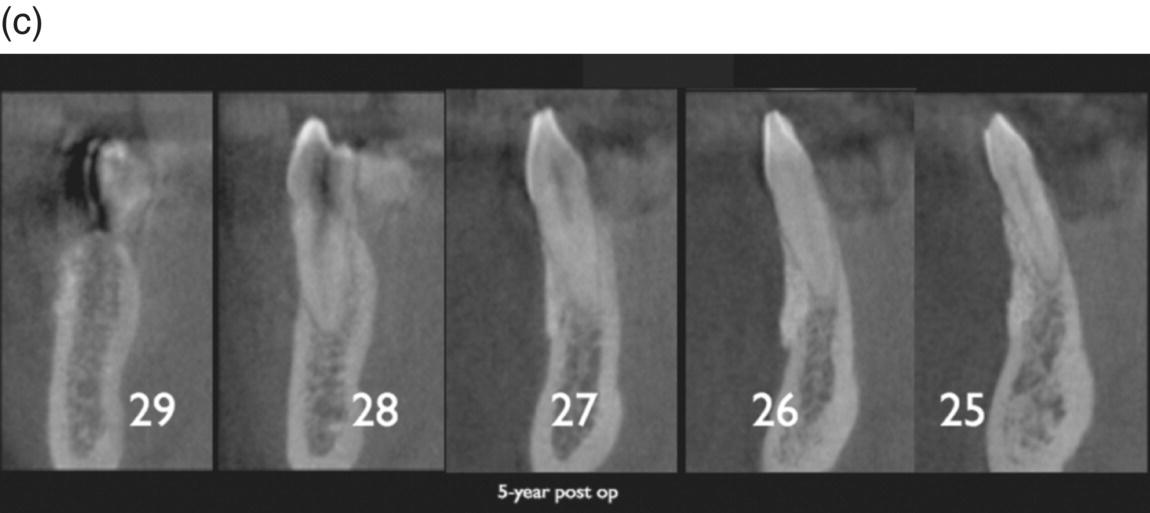
Figure 7.9 Axial views of a 5-year follow-up CBCT. (a) Inferior anterior group. Note the presence of the grafting material. (b) Grafting still covering most of the buccal cortex. Teeth numbered according to the American Dental association (ADA). (c) Without the grafting material a fenestration would be present, highly increasing the risk of recession.
Radiographic examination
The CBCT examinations were performed not later than starting the active treatment and at the end of treatment. All examinations were made using a 9000 3D CBCT (Carestream Health, Inc., USA) unit equipped with a flat-panel detector. The exposed volume was 50 mm by 30 mm (voxel size 0.679 μm to 0.2 mm, depending on whether a “stitching” of three consecutive volumes were performed to represent the entire jaw), encompassing the teeth in the jaw where corticotomy had to be performed. Exposure parameters were: 70 kV, 8–10 mA (based on subject size), and a single 360° 24 to 72 s exposure time comprising a range of 235 to 468 projections. CBCT was performed to evaluate the thickness of bone and the 3D positioning of the roots in the alveolar ridge before treatment. Primary data reconstructions were made using the acquisition software (CS3D Imaging, Carestream Health, Inc., USA), resulting in perpendicular slices in axial, coronal, and sagittal planes of the image volume. Subsequently, a second reconstruction was made to obtain contiguous 0.5 mm thickness slices. The workstation consisted of an ASUS Computer, Intel® i5 CPU, with a graphics card (NVIDIA GeForce 9500 GT Series GPU 32-bit – NVIDIA Corporation, Santa Clara, CA, USA). Reformatting and measurements were made on 19-inch flat-panel monitor (resolution 1600 pixels × 1200 pixels).
Assessment of marginal bone level and buccal/lingual plate thickness
Reconstructions were made so that, for each individual tooth/root, that was inclined lingually or labially the axial slices became perpendicular to its long axis. This can be done irrespective of the angulation of the tooth relative to the alveolar process or the presence of crowding. Image slices, perpendicular to the axial slices, are automatically reconstructed. This results in optimal visualization of the MBC in relation to the CEJ in axial, coronal, and sagittal views, as described by Lund et al. (2010).
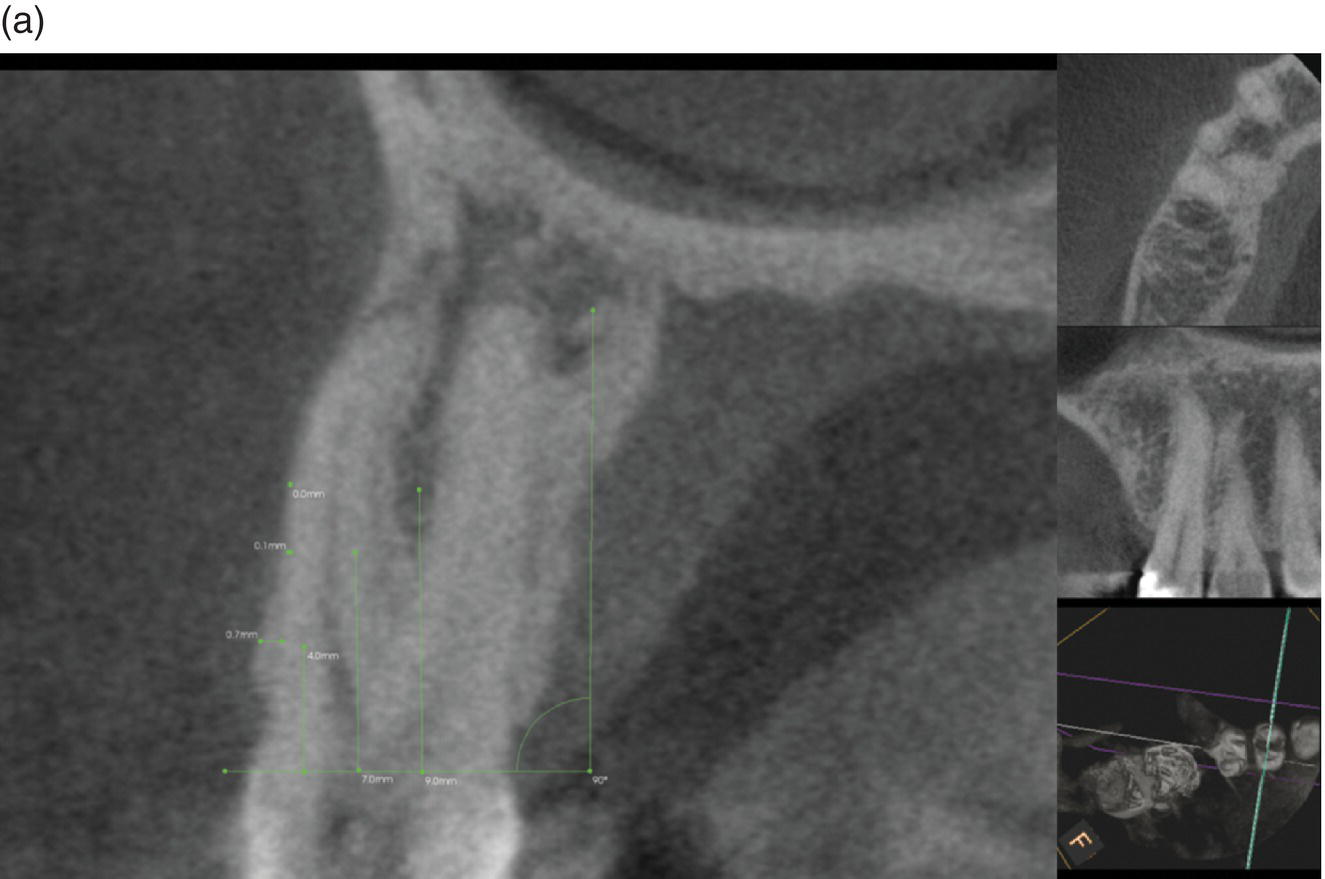
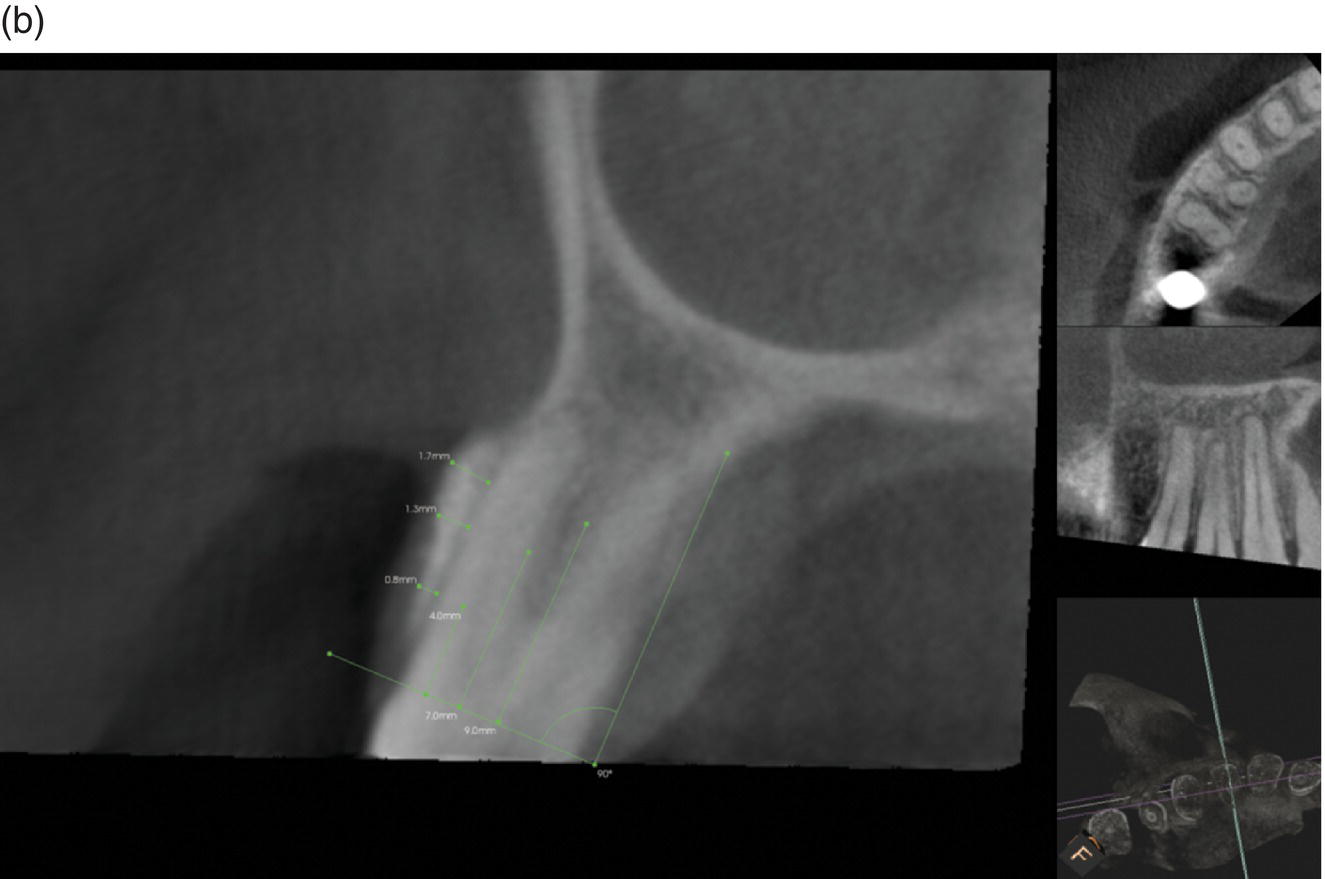
Using the axial view, one reference line was placed between the CEJs at the buccal and palatal/lingual surfaces. Parallel to that, three lines were placed at 4, 7, and 9 mm distance; one of the authors (FB) measured the thickness of the plate (to the nearest 0.1 mm). Only the teeth where the movement was carried out outside the original bony envelope were considered (Figure 7.10).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


