10
Anterior open-bite treatment through orthodontically driven corticotomy
Nagwa Helmy El-Mangoury,1 Helmy Y. Mostafa,2,3 and Raweya Y. Mostafa3,4
1 Department of Orthodontics & Dentofacial Orthopedics, Cairo University Faculty of Dentistry, Cairo, Egypt
2 Private Practice of Orthodontics, Binghamton & Endicott, New York, USA
3 Mangoury & Mostafa Research Group
4 Private Practice of Orthodontics, Cairo, Egypt
Introduction
Astute orthodontists are always on a quest for implementing innovative techniques that enable them to serve their patients and deliver the expected services in an impeccable manner. During the last decade, new treatment modalities have been introduced into the orthodontic profession. Some of these modalities satisfied the efficiency parameters as far as speeding up the treatment; for example, via orthodontically driven corticotomy (ODC). In this chapter, our conceptual framework is tri-dimensional in nature: safe acceleration of tooth movements, efficient solving of clinical problems, and proficient expansion of orthodontic capabilities (Figure 10.1). Every effort was made to discuss anterior open-bite (AOB) treatment through evidence-based ODC. As shown in Figure 10.2, evidence-based orthodontics means to translate valid (El-Mangoury, 1981) research into judicious clinical orthodontics (Mostafa, 2005). In other words (Figure 10.2), decode the established reality into the practiced actuality (Mostafa, 2005).
Figure 10.1 Conceptual framework: above and beyond safe acceleration of tooth movements.
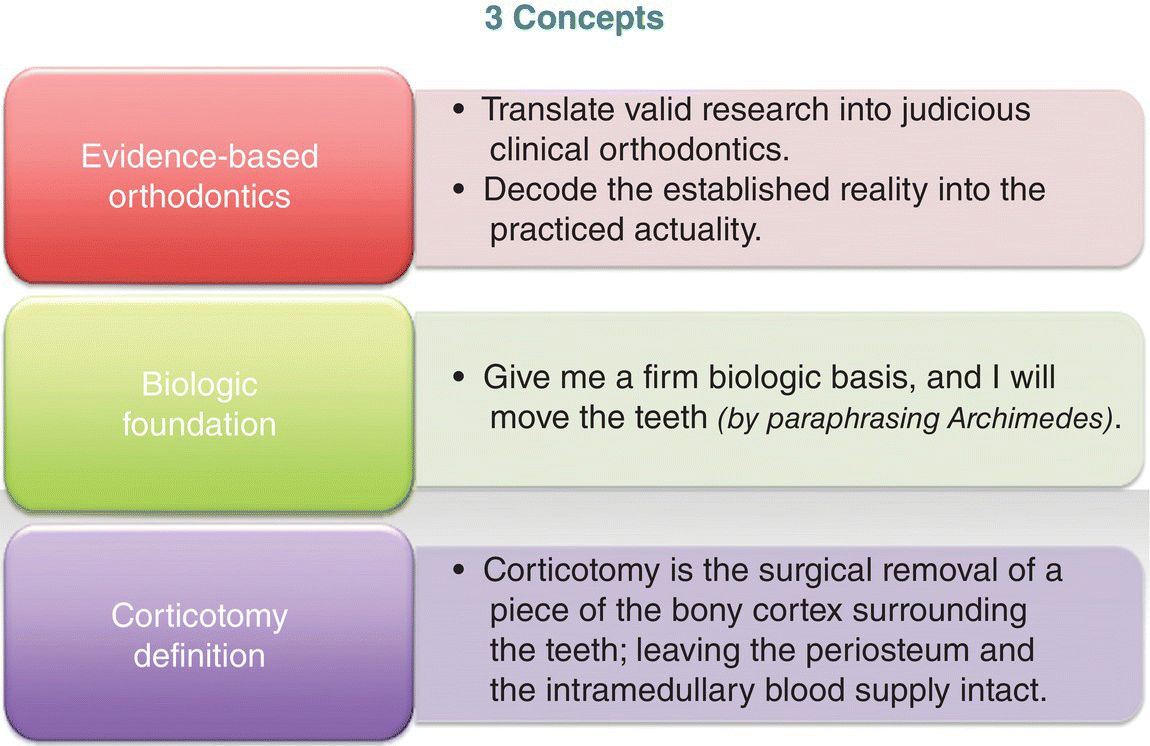
Figure 10.2 Three concepts: evidence-based orthodontics, biologic foundation, and corticotomy definition.
Further, a firm biologic foundation (Figure 10.2) is necessary for any type of tooth movements. Mostafa et al. (1991) pointed out that: “Archimedes, the Greek mathematician and inventor, stated: ‘Give me a firm place to stand, and I will move the earth.’ To paraphrase Archimedes, the contemporary orthodontist would say, ‘Give me a firm biologic basis, and I will move the teeth.’”
Open-bite
If the overbite is negative, it is called open-bite (El-Mangoury et al., 2014). Specifically, when the dentition is in centric occlusion, the anterior open-bite manifests itself through a lack of vertical contacts between the maxillary and the mandibular incisors (Figure 10.3). According to Proffit et al. (2007), the open-bite prevalence in the USA is 3.3%. The open-bite could be moderate (0–2 mm), severe (3–4 mm), or extremely severe (more than 4 mm) as shown by Proffit et al. (2007). The open-bite could be either anterior or posterior, unilateral or bilateral, acquired or hereditary, as well as dental or skeletal (El-Mangoury et al., 2014).
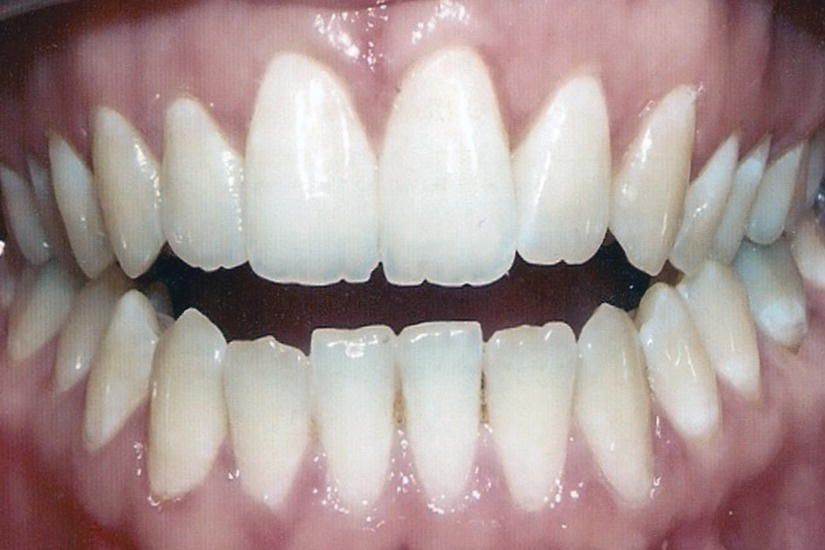
Figure 10.3 Anterior open-bite. When the dentition is in centric occlusion, the anterior open-bite manifests itself through a lack of vertical contacts between the maxillary and the mandibular incisors.
Dental open-bites are generally more responsive to treatment with orthodontics alone, whereas severe skeletal open-bites often require a combination of orthodontics and orthognathic surgery. Beane (1999) discussed the treatment principles for nonsurgical open-bites, and reviewed various treatment methods for skeletal open-bites.
Open-bites are challenging malocclusions; with a multifactorial etiology, varying clinical severity, and questionable stability (Mostafa et al., 2009a). They should not be approached as a single disease entity; rather, they should be viewed as clinical manifestations of underlying dental and skeletal discrepancies.
Specific open-bite treatment plans should be based upon the underlying etiology. Early intervention might be necessary to resolve any developing open-bite skeletal deformity. Altering the mandibular plane may be recommended through either dentofacial orthopedic growth modifications or orthognathic surgery in cases of downward and backward mandibular rotations. The reverse curve of Spee and the proclination of the maxillary incisors must be corrected. Extraction mechanotherapies in the treatment of open-bite might be beneficial to level the curve of Spee together with normalizing the proclined maxillary incisors.
Interventions for accelerating orthodontic tooth movement
In a systematic review about the interventions for accelerating tooth movement, Long et al. (2013) made the following four important conclusions:
- Corticotomy is effective and safe to accelerate orthodontic tooth movement.
- Low-level laser therapy was unable to accelerate orthodontic tooth movement.
- The current evidence does not reveal whether electrical current and pulsed electromagnetic fields are effective in accelerating orthodontic tooth movement.
- Dentoalveolar or periodontal distraction is promising in accelerating orthodontic tooth movement but lacks convincing evidence.
Brief definition of corticotomy
As indicated in the introduction and previous chapters, osteotomy is often confused with corticotomy. By definition, corticotomy is the surgical removal of a piece of the bony cortex surrounding the teeth, leaving the periosteum and the intramedullary blood supply intact (Figure 10.2).
Corticotomy baker’s dozen synonyms
The baker’s dozen phrase originated from the practice of medieval English bakers giving one or two extra loafs of bread when selling a dozen in order to avoid being penalized for selling short weight. Thus, 1 baker’s dozen equals 13 or 14. There are at least 14 corticotomy synonyms.
These synonyms are alphabetically organized in Figure 10.4. Chronologically arranged, these synonyms are: selective alveolar decortication (Mostafa et al., 1985; Fischer, 2007; Baloul et al., 2011; Hwang et al., 2011), corticotomy-facilitated orthodontics (CFO) (Kerdvongbundit, 1990; Iino et al., 2006; Fayed et al., 2009; Mostafa et al., 2009b; Aboul-Ela et al., 2011; Shoreibah et al., 2012a,b), rapid orthodontic decrowding (Wilcko et al., 2003), modified corticotomy (Germeç et al., 2006), alveolar corticotomy (Iino et al., 2007; Sanjideh et al., 2010), selective alveolar corticotomy (Oliveira et al., 2008; Baloul et al., 2011), speedy surgical-orthodontics (Chung et al. 2009a,b; Choo et al., 2011), Accelerated Osteogenic Orthodontics® (AOO®) as indicated by (Wilcko et al., 2009), decortication and osteoclastogenesis (Baloul et al., 2011), Wilckodontics (Einy et al., 2011), corticotomy-assisted decompensation (Kim et al., 2011), augmented corticotomy (Ahn et al., 2012), surgically facilitated orthodontic therapy (SFOT) as introduced by (Murphy et al., 2012), and corticotomy-enhanced intrusion (Grenga and Bovi, 2013).
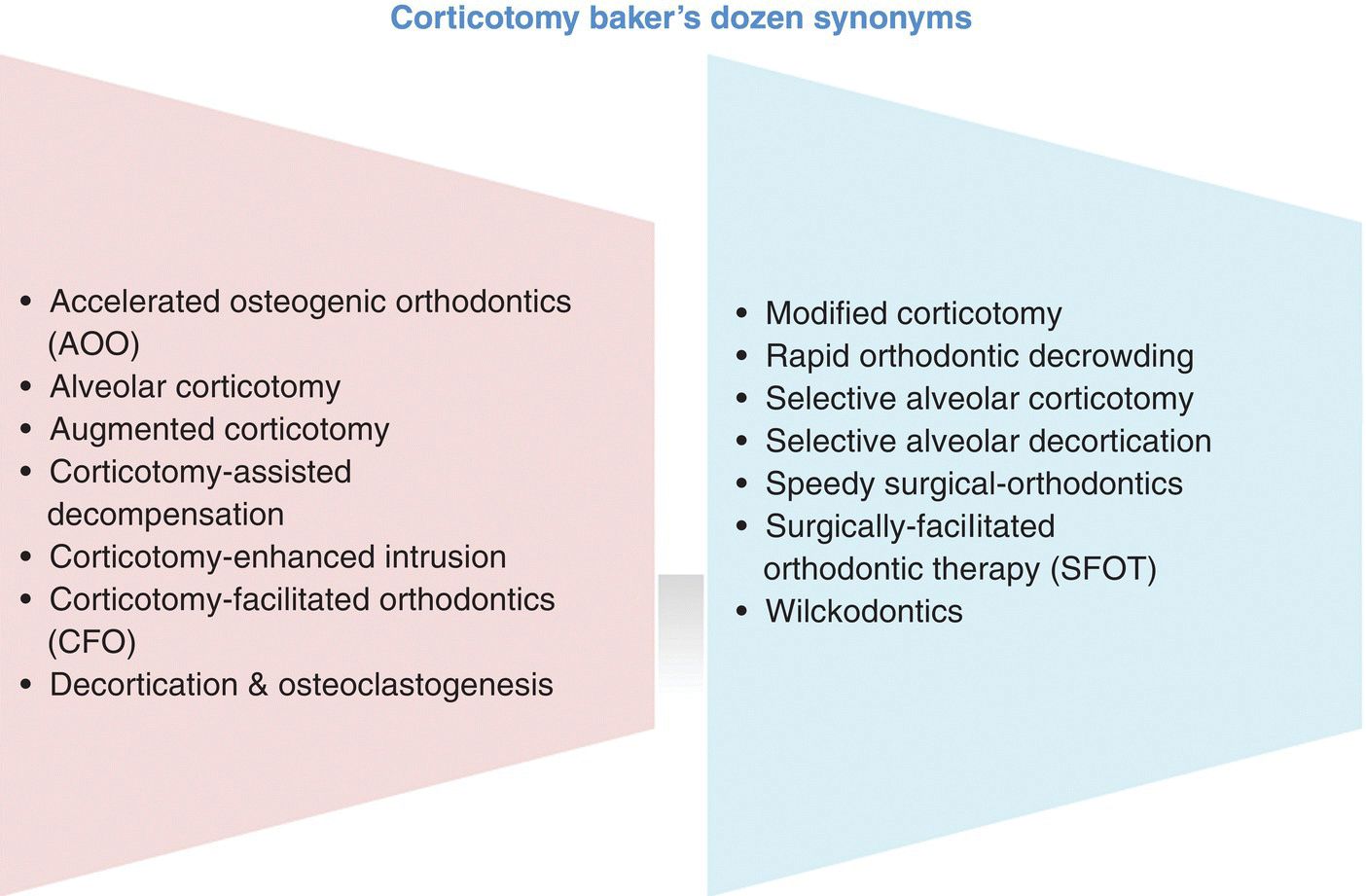
Figure 10.4 Corticotomy baker’s dozen synonyms. One baker’s dozen equals 13 or 14.
Most of these synonyms may directly be related to the concept of corticotomy (PAOO®) presented in detail throughout this book. The only technique that substantially differs from PAOO is speedy orthodontics (Chung et al., 2009a,b; Choo et al., 2011), because of the use orthopedic forces as opposed to the orthodontic ones. This is mainly due to the fact that the authors of speedy orthodontics espoused the bony-block movement, and therefore needed to use a stronger force to “bend” the medullary bone and move the bony block.
Chung et al. (2009a) described speedy orthodontics for treating severe protrusion in adults and concluded that this type of treatment mechanics can be an effective alternative to orthognathic surgery in adults. Later, Chung et al. (2009b) redescribed speedy orthodontics, which allows faster movements of the dental segments using skeletal anchorage. To minimize the risk of necrosis, two procedures were completed (Chung et al., 2009b). During the initial surgery, bilateral and horizontal corticotomies were performed in the palatal area (Chung et al., 2009b).
After 2–3 weeks, a second buccal corticotomy was done, and 500–900 g of force per side was immediately applied to the corticotomized segment (Chung et al., 2009b). Successful alveolar bone bending could be obtained in cases of adult protrusion or open-bite (Chung et al., 2009b). Speedy orthodontics allowed for more precise control of anterior segment retraction in adult protrusion patients and can be used for posterior segment intrusion (Chung et al., 2009b). Additionally, Choo et al. (2011) pointed out that speedy surgical orthodontics can be an effective modality for adults with severe maxillary protrusion.
Corticotomy and tissue engineering for orthodontists
About 30 years ago, Mostafa et al. (1985) were able to intrude overerupted maxillary molars through safe decortications and extremely simple biomechanics. Fischer (2007) was capable of reducing the orthodontic treatment duration for palatally impacted canines through selective alveolar decortication.
Iino et al. (2006) performed CFO on the lingual and buccal sides in the maxillary anterior as well as the mandibular anterior and posterior regions. Further, Mostafa et al. (2009b) studied six mongrel dogs, aged 6–9 months. Extraction of the maxillary second premolars and miniscrews placement were done bilaterally in the maxilla (Mostafa et al., 2009b). The corticotomy was performed on the right side (Mostafa et al., 2009b). The first premolars were distalized against the miniscrews with nickel–titanium coil springs on both sides (Mostafa et al., 2009b).
The first premolar on the CFO side moved significantly more rapidly (Mostafa et al., 2009b). Histologic findings showed more active and extensive bone remodeling on both the compressive and tension sides in the CFO group (Mostafa et al., 2009b). Actually, the CFO technique (Figure 10.5) doubled the rate of orthodontic tooth movement (Mostafa et al., 2009b). Mostafa et al. (2009b) pointed out that the more active and extensive bone remodeling in the CFO group as well as the acceleration of tooth movement associated with corticotomy might be due to increased bone turnover based on regional acceleratory phenomena.
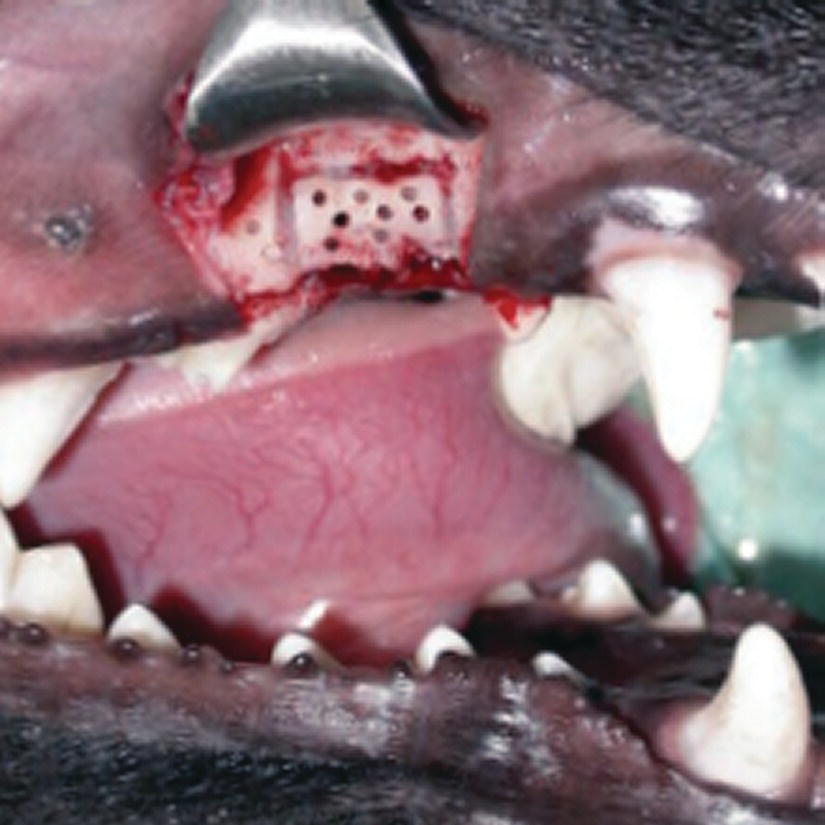
Figure 10.5 Corticotomy in a mongrel dog. Observe the horizontal and vertical cortical cuts, the cortical perforations, and the miniscrew.
Source: Mostafa et al. (2009b). Reproduced with permission of Elsevier.
Moreover, Fayed et al. (2009) concluded that the CFO technique delayed the osseous bone formation around the miniscrews in comparison with the standard technique. During the first 2 months after corticotomy, Aboul-Ela et al. (2011) found that the average daily rate of canine retraction was significantly twice as high on the corticotomy side (Figure 10.6) than on the control side. This rate of tooth movement declined to only 1.6 times higher in the third month, and 1.06 times higher by the end of the fourth month (Aboul-Ela et al., 2011). Thus, CFO can be a feasible treatment modality for adults seeking orthodontic treatment with reduced treatment durations (Aboul-Ela et al., 2011).
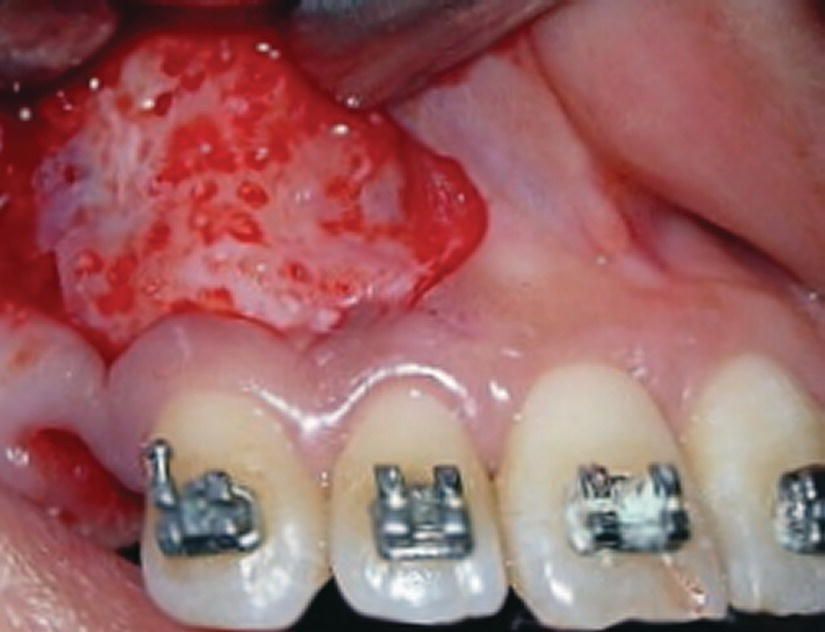
Figure 10.6 Corticotomy in the />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


