3
Corticotomy-facilitated orthodontics: Surgical considerations
Pushkar Mehra and Hasnain Shinwari
Department of Oral and Maxillofacial Surgery, Boston University Henry M. Goldman School of Dental Medicine, Boston, MA, USA
Introduction
Alveolar arch crowding is the most common manifestation of a dental malocclusion. Correction of dental malocclusions has been shown to improve periodontal health and psychosocial status (Rusanen et al., 2010). The conventional orthodontic approach for resolution of dental crowding involves either extraction of selected teeth (often bicuspids) or alternative mechanics like expansion, interproximal stripping, and/or angulation modifications using nonsurgical orthodontic treatment alone. Generally speaking, mild to moderate crowding in most cases can be managed without extraction of teeth, but moderate to severe cases are usually best treated with dental extractions. Adult orthodontics is becoming very popular, and an increasing number of adults in recent years are undergoing orthodontic treatment. Duration and cost of the treatment still remain the biggest challenges for the orthodontic field in the current era relative to treatment of adults. Typical orthodontic treatment ranges from 1 to 2 years, which requires continuous compliance and expense from the patient’s perspective for a considerable period of time. The duration and management of comprehensive orthodontic treatment for adults is significantly longer than for adolescents (Vig et al., 1990). Thus, it is only likely that many potential orthodontic patients either decline or discontinue the treatment due to their changing social and financial situations.
Decreasing the time for tooth movement has been the focus of many clinicians and researchers for a long time. For the last few decades, investigators have recommended many unique treatment modifications with an aim to reduce the overall treatment time. Introduction of newer minimally invasive, predictable surgical techniques (e.g., distraction osteogenesis, alveolar bone corticotomies) has been the main focus of many clinicians for the past century (Frost, 1983, 1989a,b). This chapter will discuss one such surgical technique: selective alveolar decortication (SAD) or corticotomy.
SAD is a relatively new technique in the dental literature. However, documentation of the original concept in orthopedics literature dates back to the early 19th century. SAD refers to intentional surgical disruption of alveolar cortical bone that aims to reduce the resistance that native bone can offer towards orthodontic dental movement, thereby making orthodontic treatment more rapid. Many modifications of this basic technique have evolved in the field of dentistry over the last few years, and different authors have changed the terminology as per their own preferences (e.g., corticotomy, Wilckodontics®, corticotomy-facilitated orthodontics, accelerated osteogenic orthodontics, and Piezocision® to name a few).
In the orthodontic literature, the term “corticotomy” is vaguely defined and is often confused with “osteotomy.” Strictly speaking, the corticotomy procedure refers to a surgical technique in which a cut is made into the buccal and/or lingual cortical plates that surround the tooth without completely going through both cortices; as a result, the teeth will be present in an alveolar bone segment connected to other adjacent teeth and structures only through the medullary bone. In contrast, an osteotomy is defined as complete cuts though the entire thicknesses of both buccal and lingual cortical plates and the interposed medullary bone, potentially creating a mobilized segment of bone and teeth. Osteotomies, theoretically, may have a higher incidence of complications, such as ischemic necrosis of the bone segment, wound dehiscences at the osteotomy site, and devitalization of the teeth adjacent to the osteotomy sites.
Historical background
The technique to accelerate tooth movement (alveolar corticotomy) was first introduced by Köle (1959). It was believed that, by creating blocks of bone with vertical buccal and lingual corticotomies and apical horizontal osteotomy connecting cuts, segments of bone with the embedded teeth could be moved rapidly. However, owing to the invasive nature of Köle’s technique, it was never widely accepted. In early 1990s, Suya (1991) revised Köle’s technique with the “substitution of a subapical horizontal corticotomy cuts in place of the horizontal osteotomy cut beyond the apices of the teeth” and published a clinical study that showed good results. The concept of “regional acceleratory phenomenon” (RAP) was introduced by an orthopedist, Dr Henry Frost who proposed that intentional injury to the cortical bone results in a modification of the bone metabolism, leading to a transient state of osteopenia described as RAP. The RAP mechanism potentiating tissue healing was shown to occur in the mandible as well (Yaffe et al., 1994).
The Wilcko brothers in 2000 reintroduced and later perfected this combined surgical–orthodontic therapy with an innovative technique of combining corticotomy surgery with alveolar grafting. They initially termed their technique Accelerated Osteogenic Orthodontics™ (AOO) and more recently changed the terminology to Periodontally Accelerated Osteogenic Orthodontics® (PAOO®) (Wilcko et al., 2001). This technique entails comprehensive fixed orthodontic appliances in conjunction with full-thickness flaps and labial and lingual corticotomies around teeth to be moved. In addition, particulate bone graft is also applied directly over the bone cuts and the flap sutured in place. Tooth movement is initiated at least 1 week before the surgery and every 2 weeks thereafter by activation of the orthodontic appliance. The Wilcko’s were the first to demonstrate that the movement does not result from repositioning of tooth–bone blocks, but rather from a cascade of transient localized reactions in the bony alveolar housing leading to bone healing. The earlier concept of the rapid tooth movement was based on bony block movement in corticotomy techniques including buccal and lingual vertical and sub-apical horizontal cuts circumscribing the roots of the teeth. Current research has proven that the rapid tooth movement after corticotomy is facilitated by RAP, described as accelerated bone turnover and decreased regional bone density (Wilcko et al., 2001).
Biophysiologic considerations
An injury of any type initiates healing by perturbing some of the surviving local cells, sensitizing them so that they can respond better to specific local and systemic messengers and stimuli. Injury also releases local biochemical and biophysical messengers that make cells respond and help to determine how they should respond. The bone remodeling basic multicellular unit (BMU) first produces osteoclasts that remove preexisting hard tissue and then produces osteoblasts that replace it with well-oriented lamellar bone in the stereotypical activation–resorption–formation sequence. Bone resorption and bone formation occur in tandem in the remodeling process. This coupling mechanism has been postulated as a means by which bone is neither lost nor gained during repair. At the end of healing, when the stimulus to RAP resolves, the BMU activation declines to normal, remodeling spaces fill back with new bone, and osteopenia disappears.
The initial response of bone to a traumatic injury is by a biologic state called RAP characterized by a transient increase in bone turnover and a decrease in trabecular bone density (Frost, 1983). This localized burst of tissue remodeling is also witnessed after a surgical osteotomy or a fracture (Shih and Norrdin, 1985). Alveolar corticotomy is a surgical intervention limited to cortical bone that is incorporated into orthodontic treatment plan to facilitate the treatment of complex occlusal problems (Köle, 1959). It generates the localized RAP at the site of injury (Wilcko et al., 2001) due to which bone regenerates faster than the normal regional regeneration process. This faster regeneration is due to the enhanced stages of bone healing which could be as fast as 2–10 times that of normal physiologic healing (Frost, 1983). A localized and reversible decrease in mineral bone density or osteopenia that begins with the initial stage of RAP and diminishes with the end of RAP is responsible for the faster tooth movement. Locally induced osteopenia weakens the trabeculae of the alveolar bone, and this lesser resistance subsequently leads to the rapid movement of teeth (Sebaoun et al., 2008). Once orthodontic tooth movement is completed, an environment is created that favors alveolar remineralization. The effect of RAP begins within 2–3 days of injury and reaches its peak at 1–2 months. This effect lasts usually for 4months, but may take 6–24 months to completely subside (Wilcko et al., 2003).
Indications
- Decreasing the duration of orthodontic treatment in patients who are undergoing conventional, nonsurgical orthodontic therapy (treatment of dental malocclusions with orthodontics alone) (see Chapters 4–6).
- Expanding the alveolar basis, therefore reducing the need for premolar extractions and strengthens the periodontium, lowering the risk for periodontal damage during and after treatment (see Chapter 7).
- Selectively altering the differential anchorage among groups of teeth, hastening and facilitating the movement of teeth that have to be moved and diminishing the countereffect in the teeth that should not be moved (see Chapter 6–8).
- As a tool in multidisciplinary treatment, including managing of partial edentulism in adult and growing patients (see Chapter 8).
- Modifying the lower third of the face (see Chapters 6 and 7).
- Adjunctive measure in facilitating treatment of impacted teeth (see Chapter 6).
- Decreasing the duration of pre-operative orthodontic treatment in patients undergoing conventional, combined surgical–orthodontic therapy (treatment of skeletal malocclusions with orthognathic surgery).
- Alternative to orthognathic surgery for combined surgical–orthodontic management of select dentoskeletal malocclusions.
- Salvage technique for the management of post-orthognathic, occlusion-related complications.
- Management of clinically refractory orthodontic dental conditions.
Contraindications
These are similar to those for any minor oral surgery or periodontal surgery procedures, especially when related to conditions affecting systemic health and illness (cardiac, endocrine, musculoskeletal, etc.). Additionally, SAD may be contraindicated in certain local disease states, such as active periodontitis or systemic conditions (e.g., uncontrolled osteoporosis). It may also have an increased complication rate in patients who have a history of use of certain medications (e.g., nonsteroidal anti-inflammatotory drugs, immunosuppressive medications, steroids, bisphosphonates) and radiation therapy to the maxillofacial region.
Advantages
- Minimally invasive surgery:
- Decreased post-operative discomfort (compared with orthognatic surgery such as surgically assisted rapid palatal expansion (SARPE)).
- Minimal complications.
- Eliminates the need for dental extractions in many patients.
- Improved post-surgical outcomes:
- Less root resorption during active orthodontic movement due to decreased resistance of cortical bone.
- Improved quantity and quality of periodontium; more bone support due to the addition of bone graft.
- Decreased duration of treatment:
- Orthodontic treatment;
- Total treatment time;
- Decrease of length-related side effects of orthodontics due to plaque accumulation, such as decay and periodontal disease.
- Ability to perform surgery in an office setting:
- Improved efficiency;
- Decreased costs;
- No requirement for hospitalization.
Surgical technique
Pre-operative considerations
Medical and surgical history should be obtained and considerations for surgery are similar to routine indications and clearance for intraoral dentoalveolar procedures. A panoramic radiograph is recommended to evaluate the maxillary sinus, nasal cavities, and other skeletal and dental structures from a general perspective. Full-mouth periapical X-rays are recommended to evaluate root proximity and other structures, such as periodontal health and status, lamina dura, and so on. Cone beam computed tomography scans are becoming widely popular and have the benefit of a precise evaluation of the thickness of buccal and lingual cortical plates and their intimate relationship to the roots of teeth, besides giving all the information that plain films would give.
Orthodontic appliances are placed approximately 1–2 weeks week prior to the surgery. Standard brackets, arch wires, and normal orthodontic force level can be used. Surgery is performed in an office setting with or without sedation, depending on patient and doctor preference. The surgical armamentarium required is similar to any intraoral, minor dentoalveolar surgical, or implant surgery procedure (hand instruments, rotary instrumentation, piezoelectric module, bone graft materials, sutures, etc.). Local anesthetic with vasoconstrictor should be infiltrated buccally/labially and palatally at least 7 min prior to incision to maintain optimal hemostasis. Use of appropriate antibiotics with adequate oral flora coverage (oral amoxicillin or clindamycin) and oral chlorhexidine rinse is recommended prior to surgery. These are usually started approximately 1 h prior to the procedure and continued for 1–2 weeks post-operatively.
Incision design
A no. 15 Bard–Parker surgical blade is used on a suitable scalpel handle and held at a slight angle to the teeth. For four quadrant cases, a smooth continuous stroke is made in the gingival sulcus from first molar to first molar crossing the midline in one arch. A vertical releasing incision can then be made behind the first molar. Vertical incisions are not recommended in the anterior region because of esthetic reasons. Although some cases can be performed with only sulcular incisions, vertical releases ensure increased access and ease of flap reflection, and may especially be indicated for those practitioners who are less experienced with surgical procedures. The authors also recommend that, in the anterior midline region, the incision be designed in a manner that avoids incising the triangular papilla on the labial mucosa between the central incisors (papilla-sparing incision) (Figure 3.1a). The above-mentioned incision design is indicated for conventional surgery; many other modifications have been proposed including vertical separate incisions for piezoelectric instrumentation (Figure 3.1b). These modifications are beyond the scope of this chapter and will be described in Chapter 5.
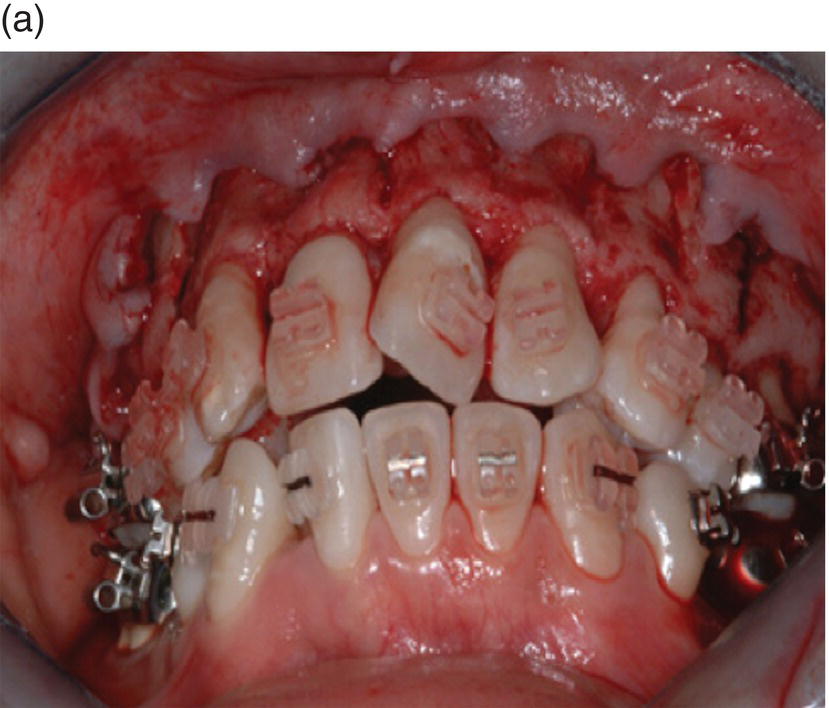
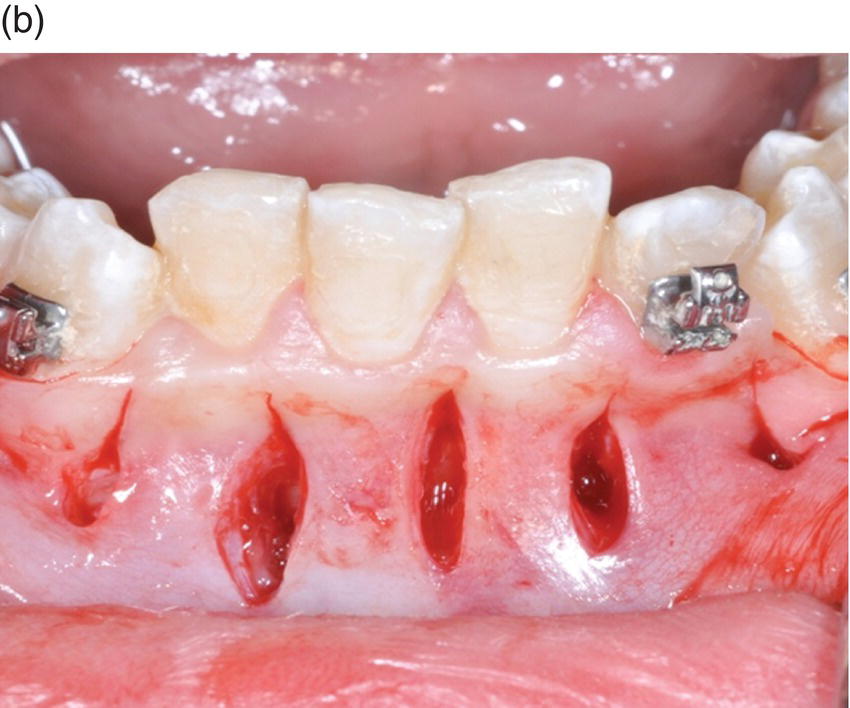
Figure 3.1 (a) A sulcular incision has been made around the necks of the individual teeth in the areas to be decorticated. The flap has been reflected apically to demonstrate bone exposure. (b) Modified incisions have been proposed by some authors, especially using piezoelectrical instrumentation. This photograph depicts five vertical incisions in the areas where piezoelectric instrumentation would be used to decorticate the bone in the interdental regions.
Flap reflection and exposure
The reflection of a full-thickness mucoperisoteal flap is carried out next. The sharp end of a no. 9 Molt’s periosteal elevator or Woodson is slipped underneath the papilla in the area of the incision and is turned laterally to reflect the papilla away from the underlying bone (Figure 3.2). This technique is then utilized for the remainder of the flap, extending laterally. Care should be exercised not to da/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


