7
Gastrointestinal disorders
Introduction
Diseases of the gastrointestinal (GI) system can be relevant to the dental surgeon for several reasons. The mouth may display signs of the disease itself, e.g. the cobblestone mucosa, facial or labial swelling of Crohn’s disease, or the osteomata of Gardner’s syndrome. These are well covered elsewhere and not discussed further here. The sequelae of GI disease, e.g. gastric reflux producing dental erosion, iron deficiency anaemia and treatment such as corticosteroid therapy may all impact on management and choice of anaesthesia.
Relevant points in the history
Lethargy, dyspnoea and angina may all occur secondary to anaemia from a GI cause, but cardiorespiratory conditions should also be borne in mind. The cause of an anaemia should always be investigated. The possibility of blood loss from the GI tract should be considered. Weight loss may be the result of reduced nutritional intake secondary to anorexia, nausea or vomiting. There may be loss of protein from diseased bowel, e.g. in ulcerative colitis. Cancer of the GI tract is the most significant potential cause of weight loss. The quantity and time course of the weight loss are both important. Enquiry with regard to appetite and any changes in bowel habit should also be made.
‘Heartburn’ or ‘indigestion’ are vague terms often used by patients and may be used to describe upper abdominal pain, gastro-oesophageal regurgitation, anorexia, nausea and vomiting. Oesophageal reflux or ‘heartburn’ causes epigastric pain, i.e. abdominal pain around the lower end of the sternum, which radiates to the back and is worse on stooping and drinking hot drinks. It can have implications for general anaesthesia (see below) and can be a cause of dental erosion especially on the palatal/lingual surfaces of the teeth as a result of the acidity of the gastric fluid. Factors promoting gastro-oesophageal reflux are shown in Table 7.1.
Dysphagia, or difficulty in swallowing, is a symptom that should always be taken seriously. Plummer–Vinson syndrome is the name given to dysphagia asso-ciated with webs of tissue in the pharynx and upper oesophagus. Other components of the syndrome include glossitis, iron deficiency anaemia and koilonychia (spoon-shaped fingernails suggesting iron deficiency but may also occur in ischaemic heart disease). Some other causes of dysphagia are listed in Table 7.2.
Vomiting may be due to extraintestinal causes such as meningitis, migraine or as a result of drug therapy (e.g. morphine). In children, vomiting can be a sign of infection of various body systems. Nausea or vomiting in the morning may be seen in pregnancy, alcoholism and anxiety. Haematemesis, or vomiting of blood, may arise from bleeding oesophageal varices. The relevance to dentistry is mainly related to the fact that these varices may occur secondary to chronic liver disease with its attendant implications for blood clotting and drug metabolism as a result of hepatic impairment.
Gastric bleeding may present as haematemesis, in which case the vomit is described as resembling coffee grounds. Blood altered by gastric acid appearing in the stool is described as melaena and is black and resembles tar.
A current or past history of peptic ulcer may be of relevance, particularly when NSAIDs are being considered. These ulcers are common, affecting around 10% of the world population. Men are affected twice as much as women. The incidence is declining in developed countries and this may be due to dietary changes. Peptic ulcers may affect the lower oesophagus, stomach and duodenum. The pendulum has swung away from surgery for these conditions since the advent of effective drug therapy. Helicobacter pylori (a microaerophilic Gram-negative bacterium) can be identified in the gastric antral mucosa in 90% of cases of duodenal ulcers and in the body or antral mucosa of about 60% of cases of gastric ulcer. It is a common aetiological factor in peptic ulcer disease. Triple therapy regimens are used for treatment when Helicobacter pylori is involved, e.g. a proton pump inhibitor such as omeprazole, a broad-spectrum antibiotic such as amoxicillin, and metronidazole.
Table 7.1 Factors promoting gastro-oesophageal reflux
|
|
|
|
|
|
Table 7.2 Possible causes of dysphagia
| Oral causes |
|
|
|
|
|
|
|
|
| Obstruction in oesophageal wall |
|
|
|
|
| External compression of oesophagus |
|
|
| Disorders of neuromuscular function |
|
|
|
|
| Other |
|
|
|
|
The term inflammatory bowel disease includes ulcerative colitis, Crohn’s disease (Fig. 7.1) and an indeterminate type. Factors that impact on dental practice include the possibility of anaemia secondary to chronic bleeding and corticosteroid therapy in these patients. Extraintestinal manifestations of inflammatory bowel disease may occur and are listed in Table 7.3.
Table 7.3 Extraintestinal manifestations of inflammatory bowel disease
| Aphthous stomatitis | |
| Hepatic | Fatty change |
| Amyloidosis | |
| Gallstones | |
| Skin | Erythema nodosum (see text) |
| Pyoderma gangrenosum (see text) | |
| Arthritis | |
| Finger clubbing | |
| Eye lesions, e.g. conjunctivitis | |
| Vasculitis | |
| Cardiovascular disease | |
| Bronchopulmonary disease |
Figure 7.1 A granulomatous inflammation of the lips in a patient with Crohn’s disease.
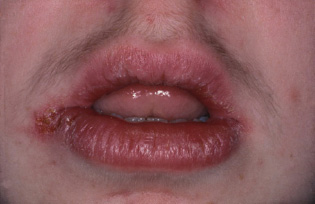
Crohn’s disease is a chronic inflammatory disorder characterised by transmural inflammation, which is granulomatous. Any part of the gut can be affected, but most commonly it affects the terminal ileum and proximal colon. There may be unaffected areas, and the active areas are described as skip lesions.
Ulcerative colitis is an inflammatory disorder of the colonic mucosa. It may just affect the rectum or extend to involve all or part of the colon. It is characterised by relapses and remissions.
Irritable bowel syndrome (IBS) is a term used to describe a group of heterogeneous abdominal symptoms for which no organic cause can be found.
A history of GI surgery may give clues to nutritional deficiencies that may be present, e.g. iron, vitamin B12 or folate deficiency post-gastric surgery. Recurrent oral ulceration and glossitis may ensue.
Pancreatic disease is of relevance in a thorough history since consequent malabsorption of vitamin K may lead to a bleeding tendency. There is also a possibility of diabetes mellitus or a diabetic tendency. Excessive alcohol intake can be a cause of acute pancreatitis, and a thorough social history may uncover this information. Other causes of acute pancreatitis include gallstones and some viral infections, e.g. HIV and mumps. Chronic pancreatitis is of a similar aetiology to acute pancreatitis. Endocrine and exocrine function both deteriorate. In both types of pancreatitis, abdominal pain is severe. Pancreatic cancer frequently involves the head of the pancreas, and local invasion leads to biliary obstruction, diabetes mellitus and pancreatitis. Thrombophlebitis migrans (peripheral vein thrombosis) is a common complication. Pancreatic cancer has the worst prognosis of any cancer in general terms, and treatment is usually surgical and palliative. The patient may give a history of jaundice or may actually be jaundiced. Jaundice is discussed later in the chapter.
Figure 7.2 A patient with Peutz–Jeghers syndrome.
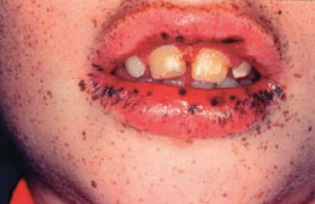
Congenital disorders of relevance can occur. Familial polyposis has an incidence of 1 in 24 000 and is transmitted as autosomal dominant. People with the condition have rectal and colonic polyps. A variant is Gardner’s syndrome, which also includes bony osteomata and soft tissue tumours, e.g. epidermal cysts. The colonic polyps are pre-malignant. and careful follow-up of these patients is needed. Subtotal colectomy with fulguration of rectal polyps may be carried out in order to prevent malignancy.
Peutz–Jeghers syndrome is an autosomal dominant condition comprising intestinal polyps and pigmented freckles periorally extending on to the oral mucosa (Fig. 7.2). The gastric and duodenal polyps have a predisposition to becoming malignant.
Table 7.4 Relevant points in the history
|
|
|
|
|
|
|
|
|
|
Some skin disorders may occur as part of a wider picture of GI disease. Erythema nodosum and pyoderma gangrenosum can occur in inflammatory bowel disease. The skin lesions are painful, erythematous nodular lesions on the anterior shin in erythema nodosum. Bluish edged ulcers occur on the back, thigh and buttocks in pyoderma gangrenosum. The skin disease associated with coeliac disease is dermatitis herpetiformis and comprises an itchy papulovesicular rash mainly on the trunk and upper limbs. IgA deposits at the epithelium basement membrane zone help to establish the diagnosis. There may also be papillary tip microabscess formation. There may be intraoral lesions which may be erosive or vesicular and resemble pemphigoid. Treatment is usually with dapsone. Aphthous ulcers may occur.
Coeliac disease is a permanent intolerance to gluten leading to intestinal villous atrophy and GI malabsorption. The villous atrophy reverses when taking a glutenfree diet. The disease may be complicated by anaemia and GI lymphoma.
Pseudomembranous colitis can be caused by many antibiotics, particularly clindamycin and lincomycin, and results from proliferation of toxigenic Clostridium difficile. It is characterised by painful diarrhoea with mucus passage, and is treated with oral vancomycin or metronidazole.
A summary of relevant points in the history is given in Table 7.4.
Examination
Oral lesions as a manifestation of GI disease are well discussed elsewhere and are not considered further here. It is worth remembering that cervical lymph node enlargement is an important sign not to be ignored. Possible causes include infection and neoplasia (primary or secondary).
Pallor can be a very subjective way of trying to assess for anaemia. The mucosa at the reflection in the inferior fornix of the eye is the best site for examination. The patient may readily become dyspnoeic secondary to anaemia, but this should be considered with an open mind because, as mentioned earlier, cardiorespiratory conditions are more likely to present in this manner.
A patient may be jaundiced for ‘extrahepatic’ reasons such as gallstones, cancer of the bile ducts or cancer of the head of pancreas. The sclera is a good site for examining for the yellow tint of jaundice (
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


