Preparation of the Periodontium for Restorative Dentistry
Periodontal health is the “sine qua non,” a prerequisite, of successful comprehensive dentistry.23 To achieve the long-term therapeutic targets of comfort, good function, treatment predictability, longevity, and ease of restorative and maintenance care, active periodontal infection must be treated and controlled before the initiation of restorative, esthetic, and implant dentistry. In addition, the residual effects of periodontal disease or anatomic aberrations inconsistent with realizing and maintaining long-term stability must be addressed. More recently, this phase of treatment includes techniques performed in anticipation of esthetic or implant dentistry, such as clinical crown lengthening, covering denuded roots, alveolar ridge retention or augmentation, and implant site development (see Video 66-1: Effects of Single Tooth Loss).![]()
Rationale for Therapy
The many reasons for establishing periodontal health before performing restorative dentistry include the following45:
1. Periodontal treatment is undertaken to ensure the establishment of stable gingival margins before tooth preparation. Noninflamed, healthy tissues are less likely to change (e.g., shrink) as a result of subgingival restorative treatment or postrestoration periodontal care.26,27 In addition, tissues that do not bleed during restorative manipulation allow for a more predictable restorative and esthetic result.20,21
2. Certain periodontal procedures are designed to provide for adequate tooth length for retention, access for tooth preparation, impression making, tooth preparation, and finishing of restorative margins in anticipation of restorative dentistry.20,41 Failure to complete these procedures before restorative care can add to the complexity of treatment and introduce unnecessary risk of failure.20
3. Periodontal therapy should antecede restorative care because the resolution of inflammation may result in the repositioning of teeth40 or in soft tissue and mucosal changes. Failure to anticipate these changes may interfere with prosthetic designs planned or constructed before periodontal treatment.
4. Traumatic forces placed on teeth with ongoing periodontitis may increase tooth mobility, discomfort, and possibly the rate of attachment loss.8 Restorations constructed on teeth free of periodontal inflammation, synchronous with a functionally appropriate occlusion, are more compatible with long-term periodontal stability and comfort (see Chapters 15 and 50).
5. Quality, quantity, and topography of the periodontium may play important roles as structural defense factors in maintaining periodontal health. Orthodontic tooth movement and restorations completed without the benefit of periodontal treatment designed for this purpose may be subject to negative changes that complicate construction and future maintenance.47
6. Successful esthetic and implant procedures may be difficult or impossible without the specialized periodontal procedures developed for this purpose.
Control of Active Disease
Periodontal therapy is intended to control active disease (see Chapters 42 to 49). In addition to the removal of root surface accretions that are primary etiologic agents, secondary local factors, such as plaque-retentive overhanging margins and untreated caries, must be addressed.13,18
Extraction of Hopeless Teeth
Extraction of hopeless teeth is followed by provisionalization with fixed or removable prosthetics. Retention of hopeless teeth without periodontal treatment may result in bone loss on adjacent teeth.30 Restorative margins are refined and provisional restorations refitted after the completion of active periodontal therapy.
Oral Hygiene Measures
Oral hygiene measures, when properly applied, have been shown to reduce plaque scores and gingival inflammation28,44 (see Chapter 45). However, in patients with deep periodontal pockets (>5 mm), plaque control measures alone are insufficient in resolving subgingival infection and inflammation.5,28
Scaling and Root Planing
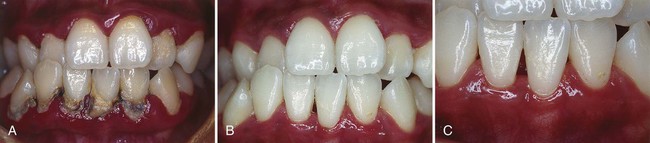
Scaling and root planing combined with oral hygiene measures have been demonstrated to significantly reduce gingival inflammation and the rate of progression of periodontitis3,4,29 (see Chapter 45). This applies even to patients with deep periodontal pockets5,14 (Figure 66-1).
Reevaluation
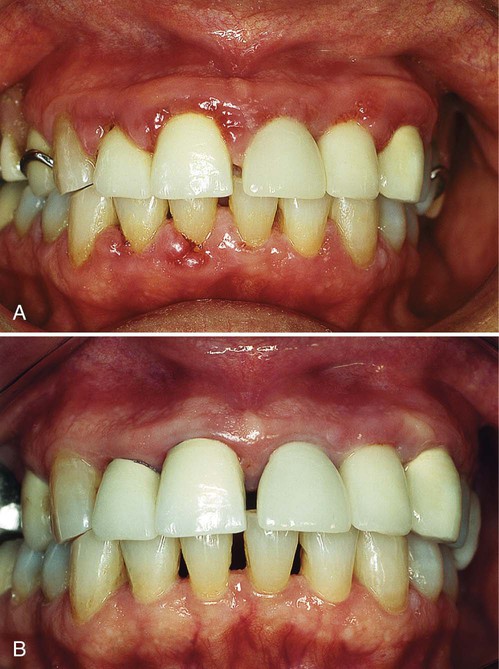
After 4 weeks the gingival tissues are evaluated to determine oral hygiene adequacy, soft tissue response, and pocket depth (see Chapter 44). This permits sufficient time for healing, reduction in inflammation and pocket depths, and gain in clinical attachment levels. In deeper pockets (>5 mm); however, plaque and calculus removal is often incomplete,42,46 with risk of future breakdown7 (Figure 66-2). As a result, periodontal surgery to access the root surfaces for instrumentation and to reduce periodontal pocket depths must be considered before restorative care may proceed.
Periodontal Surgery
Periodontal surgery may be required for some patients (see Chapters 64 and 65). This should be undertaken with future restorative and implant dentistry in mind. Some procedures are intended to treat active disease successfully,11,34 and some are aimed at the preparation of the mouth for restorative or prosthetic care.47
Adjunctive Orthodontic Therapy
Orthodontic treatment has been shown to be a useful adjunctive to periodontal therapy6,16,17,22 (see Chapter 51). It should be undertaken only after active periodontal disease has been controlled. If nonsurgical treatment is sufficient, definitive periodontal pocket therapy may be postponed until after the completion of orthodontic tooth movement. This allows for the advantage of the positive bone changes that orthodontic therapy can provide. However, deep pockets and furcation invasions may require surgical access for root instrumentation in advance of orthodontic tooth movement. Failure to control active periodontitis can result in acute exacerbations and bone loss during tooth movement.9 As long as they are periodontally healthy, teeth with preexisting bone loss may be moved orthodontically without incurring additional attachment loss.36,37
Soft tissue–grafting procedures are often indicated in anticipation of orthodontic therapy to increase the dimension of attached tissue.47
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses