6 Surgical endodontics
ASSUMED KNOWLEDGE
It is assumed at this stage that you will have knowledge/competencies in the following areas:
INTRODUCTION
Non-surgical endodontics attempts to eliminate the bacteria by cleaning and shaping the root canal to remove infected dentine, disinfecting the canal and sealing with a root filling. If non-surgical endodontics fails, it is usually because of the persistence of noxious substances (toxins and other by-products of bacteria) within the root canal system. If a root canal therapy fails and the tooth cannot be retreated, surgical endodontics may be indicated to eliminate the noxious substances from the root canal system. Where surgical endodontics is indicated, it is desirable that a root filling has been inserted first to improve the chances of success.
PRINCIPLES OF SURGICAL ENDODONTICS
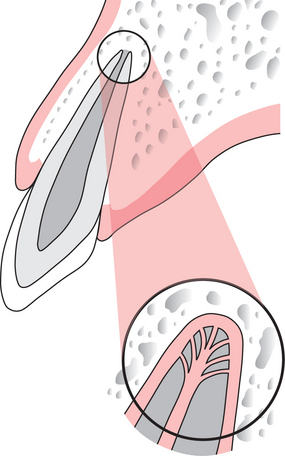
Apicectomy
The objectives of apicectomy are to:
Root-end (retrograde) filling
A root-end filling is a restoration placed into the cut surface of the root after apicectomy of the root apex to occlude the root canal apically. The root-end filling requires a small cavity to be prepared in the root surface with a bur or ultrasonic instrument, and a suitable restorative material is placed in the cavity. The objective of placing a root-end filling is to achieve a satisfactory seal of the root surface.
INDICATIONS FOR SURGICAL ENDODONTICS
Conventional endodontics is impracticable
Operator-induced (iatrogenic)
CONTRAINDICATIONS FOR SURGICAL ENDODONTICS
Factors influencing the decision to undertake surgical endodontics
Local contraindications
TREATMENT PLANNING FOR SURGICAL ENDODONTICS
Careful preoperative planning is the key to success.
Clinical examination
In the presence of an acute apical abscess, there may be erythema or swelling of the soft tissues at the apex of the affected tooth. The periapical soft tissues may be tender to palpate, and the tooth is likely to be tender to percussion. A sinus may be present on the buccal aspect of the affected tooth, although this is not always the case. Occasionally pus from a maxillary incisor may discharge through a pathological sinus into the floor of the nose. Pus from a maxillary premolar or molar may discharge into the maxillary antrum, or rarely, on to the face (see Ch. 7).
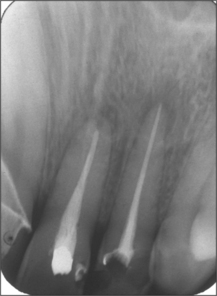
Radiographic examination
Radiographs demonstrate both anatomical and pathological features at the apex of the tooth (Fig. 6.4). A radiograph may demonstrate an incompletely sealed root canal, or bone loss around the apex of the tooth involved. If there is chronic apical disease, a lesion with the physical characteristics of a cyst may be identified at the apex of the tooth. Rarely, the cause of a failed root filling cannot be established through clinical or radiographic examination but it may become apparent when surgical endodontics is undertaken. For example, a root fracture not detectable clinically or radiographically may be identified on surgical exploration.
Advice to the patient before surgery
Complications
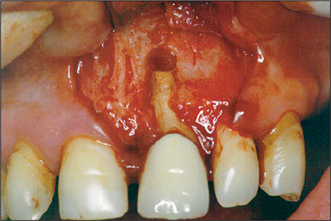
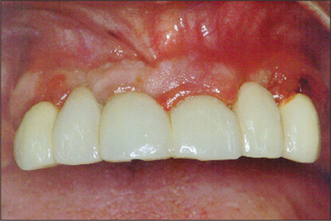
Patients should be informed of pain, swelling and bruising of the face arising after surgery. Damage to adjacent teeth may occur through carelessness or difficulty in locating the apex of the tooth to be treated. This latter complication should be anticipated preoperatively. Contraction of the mucoperiosteal flap may occur through scarring as it heals, leading to unsightly recession around the gingival margin (Fig. 6.5). A judicious approach to flap design, reflection, retraction and careful/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses