13 Maxillofacial trauma
ASSUMED KNOWLEDGE
It is assumed that at this stage you will have knowledge/competencies in the following areas:
INTENDED LEARNING OUTCOMES
At the end of this chapter you should be able to:
THE CAUSES AND PREVENTION OF MAXILLOFACIAL INJURY
The causes of maxillofacial injury reflect the culture in which it is sustained. The most frequent cause of serious maxillofacial injury in the developed world in the past century has been the motor vehicle, the only exception being epidemics of injury sustained in two world wars. Overall, incidence of maxillofacial injuries has reflected death rates on the roads such that, for example in the UK, incidence reached a peak in the 1960s and the 1970s and has been falling since. Violence has become a more common cause of maxillofacial fracture, on both sides of the Atlantic, since the late 1960s.
THE MANAGEMENT OF MAXILLOFACIAL TRAUMA
History of injury
Dental surgeons are often asked to see the injured person after their general condition has been stabilized. Occasionally this is not the case, however, and a dental practitioner may be the first to the scene of a serious accident or assault. If injuries are life-threatening, the history should be dispensed with until airway, cervical spine, breathing and circulation have been stabilized.
The Glasgow Coma Scale
First described by two Glasgow neuroscientists, the Glasgow Coma Scale (GCS) is an internationally recognized method for measuring coma. It cannot discriminate between causes of coma, such as brain injury or alcohol intoxication, but it provides an excellent means of assessing the need for hospital admission and recovery (Table 13.1).
| Score | |
|---|---|
| Eyes open: | |
| Spontaneously | 4 |
| To speech | 3 |
| To pain | 2 |
| Never | 1 |
| Best motor response: | |
| Obeys commands | 6 |
| Localizes pain | 5 |
| Flexion withdrawal | 4 |
| Decerebrate flexion | 3 |
| Decerebrate extension | 2 |
| No response | 1 |
| Best verbal response: | |
| Orientated | 5 |
| Confused | 4 |
| Inappropriate words | 3 |
| Incomprehensible sounds | 2 |
| Silent | 1 |
Scores for the three components can be added together (< 8 is defined as coma; maximum score = 15) or listed separately.
Examination
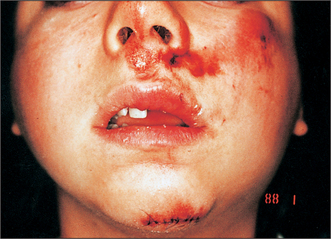
Pay particular attention to signs of bleeding or other discharge from the ears, eyes, nose and mouth. In seriously injured patients there may be leakage of cerebrospinal fluid from the ears or nose. Look for signs of impact, including on the scalp. Abrasions (Fig. 13.1) or haematomas often signal the sites of underlying bone injury. There is often little swelling in the immediate aftermath of injury. However, within 6 hours mandibular angle fractures, for example, are often associated with swelling over the angle (Fig. 13.1) and subcondylar fractures with preauricular swelling.
An examination may follow this order:
Mobility of the middle third of the face, such as that brought about by Le Fort I, Le Fort II and Le Fort III pattern fractures (Fig. 13.2) is best assessed by placing the patient’s head securely against a head rest, grasping the upper teeth and alveolus and moving them gently, but purposefully, laterally, superiorly and anteriorly. Simultaneous palpation of the nasal bones has often been advocated but this can give rise to false-positive findings because of the mobility of the scalp and skin in this region. A ‘cracked cup’ sound when the upper teeth are percussed can be diagnostic of a Le Fort pattern fracture.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses