Chapter 6
Problem Solving in the Diagnosis of Nonodontogenic Pain
Problem-solving challenges and dilemmas in the diagnosis of nonodontogenic pain addressed in this chapter are:
“The condition (tic douloureux) frequently results from chronic irritation of the fifth cranial nerve. The pain is very acute, and occurs in distinct paroxysms, gradually increasing in severity, until it reaches a climax, when it quickly subsides. The attack may occur at any time and is provided by speech, laughing, talking, the movement of a muscle, etc., and even slight noise or light touch, as placing the hat on the head, may cause a paroxysm. The patient lives in constant dread of an attack.”< ?xml:namespace prefix = "mbp" />
In the course of clinical practice, it is typical that pain is the reason many patients seek a consultation. Some symptoms are virtually diagnostic for pulpal and periapical pathosis. When a patient reports protracted pain that results from thermal stimulation, for example, there is a high likelihood it is of pulpal etiology; only the dental pulp is capable of such painful responses. The main diagnostic task is to find out which tooth is the problem.
In other cases, the history of symptoms is not so specific for pulpal or periapical pathosis. Through diagnostic procedures and radiographic interpretation described in
It is not the goal of this chapter to be encyclopedic. Other sources in the endodontic and dental literature have already described an extensive array of medical conditions from which oral and facial pain symptoms have occasionally been observed.
If a case of oral-facial pain is encountered for which no dental etiology can be found, the patient should be referred to an oral surgeon or physician for further evaluation. It is not the responsibility of the dentist to make the diagnosis or manage the treatment of such a case. It is the responsibility of the dentist to rule out a dental etiology and assist the patient in resolving the problem through an appropriate referral. To facilitate this problem-solving endeavor, various nonodontogenic pain scenarios will be presented in the manner they are most commonly encountered: thorough analysis of clinical cases.
Occlusal Discrepancies
Occlusal discrepancies are a common source of patient discomfort. Many are not tooth related, but with data gathering and problem-solving techniques, the source of the patient’s distress can usually be identified and eliminated rapidly.

PROBLEM SOLVING
Problem
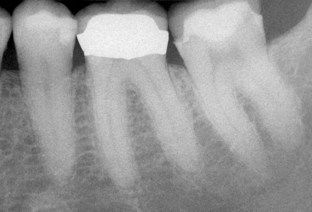
A 31-year-old female was referred for root canal treatment on her mandibular left first molar. She stated that she could not chew comfortably on the tooth. She had no thermal sensitivity and was not experiencing any spontaneous pain. A radiograph gave no evidence of dental caries, periapical pathosis, or periodontal disease (
Discussion
An examination should always begin with an accurate and detailed history of symptoms. Occasionally the patient may not recall all pertinent details, or the clinician may follow a line of inquiry that initially does not reveal important clues. It is appropriate to treat the case as having a potential problem and perform usual tests to confirm or rule out a pulpal diagnosis that requires treatment. In this case, having performed tests, it was clear that the pulp was normal in all three teeth, and the pain was from another source. Since the only symptom has been sensitivity to occlusal pressure, it was logical to assess the occlusion, which proved to be the problem. A simple occlusal adjustment of the prematurity was the only treatment required.


PROBLEM SOLVING
Problem
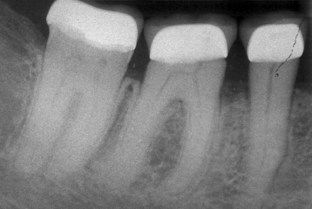
A 53-year-old male was seen on referral. For several weeks, he had been unable to chew comfortably on the mandibular right first molar. When he awoke, there was usually a particular soreness in the tooth. He had not had recent dental treatment, and there was no history of thermal sensitivity. A radiograph indicated no caries, periapical pathosis, or periodontal disease (
Discussion
This case differs from the first case in the fact that the presence of pulpal pathosis can neither be confirmed nor ruled out. It is inappropriate to proceed with root canal treatment, because there is no confirmation of pathosis. In this case, the occlusal adjustment is both a diagnostic procedure and a potential final treatment.

As for the prematurity found in the first case, occlusal adjustment may be the only treatment required. On the other hand, if sensitivity to percussion is of pulpal origin, (degenerative or irreversible pulpitis), an occlusal adjustment will improve but not eliminate the problem. In time, more definitive signs or symptoms of pulpal pathosis will become apparent, with the potential for radiographic changes at the end of the root (increase in the width of the periodontal ligament space and loss of the lamina dura; see
The appropriate course of action at this point is to wait and watch. The patient is now informed of the possible outcomes and should be encouraged to return if the symptoms become worse at any point in the future. It is impossible to predict when a true pulp problem and its sequelae may evolve. It may occur in a relatively short period of time, such as a gradual increase in symptoms over a span of days, or it may not become apparent for months.

CLINICAL PROBLEM
Problem
The patient was a 35-year-old female with a 17-month history of continuing pain following root canal treatment of the mandibular left first molar. A postoperative radiograph of treatment was provided by the referring dentist (
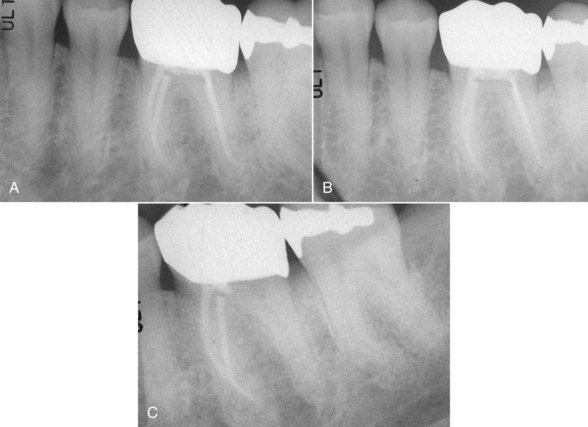
FIGURE 6-4 A, Immediate posttreatment radiograph of mandibular left first molar supplied by referring dentist. The chief complaint is continuing pain. B, Same tooth 10 months later. C, After 16 months, gutta-percha was removed from distal canal. There was no improvement in symptoms.
Referring clinician notes: Root canal treatment was completed on the mandibular left first molar for “local swelling and the feeling of warmth” over the area of the apices. Following treatment, the symptoms persisted to the present time despite antibiotics, one complete retreatment/revision, and a third reopening to remove the filling material in the distal canal. This is the status of the tooth at present.
Patient-related information: Subsequent to the initial treatment, the symptoms resolved for a time then returned. The pain had been continuous in the area of initial treatment and was the same pain felt prior to treatment. At no time were there symptoms specific to the tooth (i.e., cold, hot, or percussion sensitivity). Ten months following treatment, a feeling of external swelling developed on the inferior border of the left mandible, which prompted a return to the dentist.
A radiograph was made on return to the treating dentist 10 months post treatment (see
At this point, the dentist chose to remove the gutta-percha root filling from the distal canal, which was done on a subsequent visit 2 weeks later (see
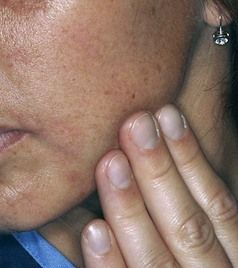
Clinical examination on referral appointment: The patient stated that the swelling had always been felt externally in the area along the inferior border of the mandible (
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses