6
Medical Emergencies
- the incidence of medical emergencies in the dental workplace
- basic life support procedures and resuscitation techniques
- the use of emergency resuscitation equipment in the dental workplace
- the actions to take in the event of various medical emergency scenarios
Medical emergencies can occur anywhere, at any time, but some may be more likely to occur in the dental surgery setting due to the nature of dental treatment and the anxiety it evokes in some patients. The anxiety that some patients experience may have the following effects.
- Lowers the pain threshold so that ‘discomfort’ is experienced as ‘pain’, producing an agitated or even unco-operative patient.
- Perception of being about to feel pain, so that stress levels and anxiety are raised – this can then put a huge strain on the patient’s body, especially the heart and circulatory system.
- Fear and anxiety at the prospect of dental treatment may worry the patient enough to prevent them eating beforehand, for fear of vomiting – the patient will then have a low blood sugar and be more prone to fainting, and in those with diabetes the low blood sugar is likely to precipitate a hypoglycaemic attack.
In addition, the following points also have to be considered.
- Many dental treatments involve the injection of a local anaesthetic, and these drugs may interact with some common patient medications.
- Any of the dental materials, antibiotics or local anaesthetics used in dentistry have the potential to cause an allergic reaction in the patient, the worse-case scenario being a full anaphylactic reaction.
- Many dental treatments are carried out with the patient lying supine (flat) in the dental chair, and this leaves their airway potentially vulnerable to foreign object inhalation, choking and a full respiratory obstruction emergency.
The dental team can do much to reduce the anxiety levels of their patients merely by creating a friendly, welcoming and pleasant atmosphere within the workplace. Showing sympathy to an anxious patient helps to reduce their stress levels and alleviates their concerns over appearing ‘foolish’ to the staff and to other patients. For those patients whose anxiety is so great that it borders on phobia (an exaggerated and illogical fear), all methods of pain and anxiety control techniques should be considered by the dental team, and offered where appropriate. This ensures that these patients will still attend and undergo dental treatment routinely.
However, those patients who pose the greatest concern with regard to medical emergencies are those with diagnosed risk factors.
- Heart conditions – any abnormality or disorder of the heart may potentially allow unexpected problems to arise during stressful episodes, such as when undergoing dental treatment.
- Hypertension (high blood pressure) – anxiety often causes a raised systolic blood pressure, which can then put a considerable strain on an already malfunctioning heart.
- Liver or kidney disorders – both these organs are responsible for eliminating waste products and toxins from the body, and any amount of malfunction due to disease could result in drugs not being detoxified and removed adequately.
- Diabetes – uncontrolled diabetes or failure to take medications accurately may result in a hypoglycaemic attack. In addition, those with diabetes tend to heal poorly and be more prone to infections, including those involving the oral cavity.
- Allergies – these patients are often sensitive to, or even allergic to, more than one allergen, so great care must be taken to avoid the use of known potential allergens in the dental workplace, such as latex and penicillin-based antibiotics.
- Certain medications known to react with some local anaesthetics – these are drugs that can be potentiated by adrenaline-containing local anaesthetics, and include some types of antidepressants, thyroxine and any medication that may cause hypertension, such as some contraceptives and hormone replacement therapy.
- Previous history of complications during dental treatment – depending on the complication and its cause, it is possible for some to be a regular occurrence with the same patient.
- Long-term steroid treatment – this treatment tends to override the body’s own production of the hormones required to react to and survive stressful events, resulting in shock and a potentially fatal crash in the patient’s blood pressure when stressful events do occur.
These patients will be identified by the accurate completion and recording of a medical history before dental treatment begins. This medical history can then be stored with the patient records (computerised or paper, or both) and updated at the beginning of every course of treatment.
Nevertheless, medical emergencies can and do occur in the dental surgery environment and the dental team must be able to recognise them and support life where necessary until specialist help arrives (that is, paramedics). All members of the dental team are expected to hold a Basic Life Support (BLS) certificate if working with patients, and to undergo the necessary continuing professional development (CPD) requirements to update their medical emergencies knowledge as laid down in the General Dental Council (GDC)’s Standards Guidance documentation.
Casualty assessment
The correct recognition of the cause of any emergency is vital if the casualty is to be correctly treated and their life supported until the emergency services can attend. This is done by being able to recognise the ‘signs’ and ‘symptoms’ of an emergency.
The signs are what the rescuer can see.
- Skin colour – is it pink, grey, red, pale?
- Breathlessness – are they gasping, breathing quickly, struggling to inhale or exhale?
- Suddenness of any collapse – did the casualty fall straight to the ground or did they slowly slump down?
- Actions before collapse, such as clutching the chest.
- Condition of the pulse – is it fast, slow, weak, absent?
At the same time, the casualty will feel symptoms, which may be asked about if they are not unconscious.
- Any pain – is it sharp, dull, throbbing, made worse by anything?
- Location of pain – where is it felt exactly?
- Nausea – does the casualty feel sick or have they vomited?
- Drowsiness – do they feel sleepy, are they struggling to respond to verbal commands?
- Difficulty breathing – are they struggling to breathe in, out or both?
- Dizziness – does the person feel like they will fall over, is the room spinning?
By assessing the casualty and noting the signs and symptoms exhibited, the rescuer can determine their next course of action, and often this will be to reassure the conscious casualty and to summon more experienced help.
However, there are two signs that should prompt any rescuer to begin BLS immediately.
- Unconsciousness
- Abnormal breathing
These two signs indicate that the casualty’s life is at risk, as sudden unconsciousness may indicate that the heart has stopped beating (asystole) or is beating ineffectively (fibrillating), and abnormal breathing indicates a compromised airway and possible lack of oxygen to the brain (hypoxia). The presence of any of these signs may result in the death of the casualty if not dealt with quickly by the rescuer.
The aim of BLS is to maintain a flow of oxygenated blood to the casualty until one of the following happens.
- They recover and begin to circulate oxygenated blood by breathing unassisted.
- Their life support is handed over to specialists, usually paramedics.
- The rescuer is too physically exhausted to continue.
- Their death is confirmed by an authorised practitioner, such as a doctor, at the scene.
Oxygen is the atmospheric gas that is vital for life. It is breathed into the respiratory system through the nose and mouth, and then passes down the trachea to the two bronchi which enter the right or left lung. In the lungs, the oxygen passes out into the circulatory system during external respiration, and is transported around the body in the arterial bloodstream by the continual pumping action of the heart. Where required, the oxygen passes out of the blood vessel and into the body tissues during internal respiration, where it is used to provide energy for the cells to work.
The actions of the respiratory system in taking up oxygen from the atmosphere and absorbing it into the blood, and the circulatory system in transporting that oxygen around the body to the cells, are carefully controlled by the brain. If any one of these three vital organs fails, the other two will also fail shortly after.
Without oxygen, the cells, and therefore the body, cannot function and death will occur. After only 3–4 min without oxygen, the brain cells can suffer irreversible damage which, if not fatal, will lead to some degree of permanent brain damage. The quicker that the need for BLS is established and begun, the better the chances of survival for the casualty – and ideally this should be within seconds of their own life support system failing.
So, the fundamental aims of BLS are to maintain the life of the casualty by achieving the following.
- Provide oxygen to the lungs – by some form of rescue breathing.
- Circulate the oxygen to the body tissues – by external chest compressions to mimic the pumping action of the heart.
Death occurs when there is a permanent cessation of the function of the heart and lungs, and these are the criteria by which a medical doctor will diagnose and certify death. Other specialists, such as paramedics, are able to diagnose and determine that death has occurred by the absence of:
- spontaneous breathing
- heartbeat
- pupillary response to light (pupils of the eyes remain dilated when exposed to light).
The lack of pupil response to light indicates brain death.
However, only a medical doctor can certify that death has occurred and issue a death certificate, so all rescue attempts must continue until this has been established, or until any rescuers are too physically exhausted to continue in their efforts to resuscitate the individual.
If there is more than one rescuer able to provide BLS, it is important that the compression and ventilation roles are regularly swapped between them, as chest compressions are physically tiring to perform and the rescuer will soon become exhausted.
Current Basic Life Support guidelines
In the United Kingdom, the general guidelines to be used for BLS are issued by the Resuscitation Council (UK) and should be followed nationally. Local protocol amendments may exist in some areas or in some workplaces (especially hospitals), and readers should ensure that they are aware of these. However, the current Resuscitation Council advice is that rescuers need to apply 30 chest compressions for each two rescue breaths given, no matter how many rescuers are present. This gives the current compression:ventilation algorithm of 30:2.
The two important signs that should be looked for when determining the need to provide BLS to a casualty are:
- unconsciousness
- abnormal or absent breathing.
Unconsciousness indicates that the casualty is unresponsive to all stimuli, and that their heart may have stopped beating – they have gone into cardiac arrest. There is no instance where the heart can have stopped beating and a person remain conscious, as the body cells (especially the brain) will become starved of oxygen very quickly and will be unable to function.
Abnormal breathing, such as infrequent noisy gasps, indicates that there is a possible obstruction in the casualty’s respiratory system which is making normal breathing difficult. This will gradually reduce the oygen supply to the body cells, and once breathing ceases completely, the oxygen supply is cut off immediately. The casualty’s skin colour will change from pink, through pale to blue or grey as their body tissues become starved of oxygen. This is more difficult to determine in those with darker skin tones, so the lips, nailbeds and mucous membranes of the mouth may also be checked for signs indicating lack of oxygenation or hypoxia.
The actions that may be required to help the casualty cannot be determined until the rescuer has fully assessed the situation, and although swift action is necessary to avoid brain damage or death, the following questions must be quickly considered by the rescuer in an effort to realise the correct medical emergency.
- Why has the individual become unconscious? Are there any external causes such as trauma, electrocution, poisonous fumes, drowning?
- How is unconsciousness established? Are they alert or moving, are they responsive to noise or voices, are they responsive to pain, are they completely unresponsive?
- Is their breathing abnormal? Are they gasping, coughing or even clutching at their throat?
- Are there any breath sounds? How is this established?
- What does the rescuer do next? At what point should help be summoned, and what actions are required immediately?
The accepted order to follow when assessing an emergency situation and determining whether BLS is required can be summarised and easily remembered by the following code.
- D for Danger
- R for Response
- S for Shout for help
- A for Airway
- B for Breathing
- C for Circulation
This is best remembered as DRSABC (referred to as ‘doctors – a – b – c’).
Valuable time can be wasted during this assessment by attempting to open or remove clothing from the casualty while trying to establish their condition, which should not be attempted by the rescuer. The casualty may actually sustain further injury while clothing is being removed. In addition, many individuals would become very distressed at finding themselves partially clad and surrounded by strangers. The dignity and rights to decency and privacy of the casualty must be maintained at all times, by all rescuers.
DRSABC in detail
Danger
Check the immediate area for possible dangers, such as electric wires running through pooled water, punctured gas canisters, spilt chemicals giving off strong fumes, etc. If hazardous chemicals are suspected of being involved in the emergency situation, the workplace COSHH file must be consulted at some point for information on first aid actions that may be necessary. This action is best delegated to a spare rescuer, while BLS is being carried out by others.
If possible, any dangers should be made safe by the rescuer before approaching the casualty, but not at the risk of endangering themselves in the process. Ideally, this should not involve moving the individual except in extreme circumstances, such as rising water levels that may cause drowning. This is to prevent any further injury being caused.
Response
The level of responsiveness will determine whether the casualty is unconscious or not. Call loudly to them, asking if they can hear you or if they are all right, while gently shaking them. Their responsiveness can quickly be assessed and determined by a system referred to as the AVPU code.
- Alert – the casualty is fully conscious and able to communicate fully and spontaneously.
- Verbal – the casualty is not fully conscious but is able to respond to verbal commands and prompts.
- Painful – the casualty is semi-conscious at best, but able to respond to painful stimuli such as a gentle pinch.
- Unresponsive – the casualty shows no response to verbal prompts nor painful stimuli, they are unconscious and unable to be roused.
If the casualty shows no response whatsoever, then they are in need of help urgently. Wherever possible, the level of responsiveness should be determined without moving the individual from the position in which they were found, to avoid any further injury.
Shout
If the casualty is unresponsive and therefore unconscious, the rescuer will need help with any attempt at BLS if it is required, as well as to summon specialist help if necessary. If only one rescuer remains to aid the individual while help is being sought, they may need to continue BLS for a prolonged period of time, and ultimately this may result in their physical exhaustion. If attempts at BLS have to then be abandoned before specialist help arrives, the casualty is likely to die.
Shout very loudly to alert anyone else in the vicinity that an emergency situation has arisen. In the workplace, there may be internal communication systems in place for just such an event, such as intercoms, alarm bells or coded calls, and these must be known and used appropriately by the rescuer.
Airway
The airway needs to be checked for any obstruction, such as vomit or debris or the tongue itself, which may have fallen back and blocked it. Any loose obstruction should be removed by rolling the casualty’s head to the side to encourage it to drop out of the mouth. In the dental surgery there will also be electrically operated suction equipment available at the chairside or a manually operated suction device within the emergency kit that all dental workplaces have to have on the premises (Figure 6.1). However, these must only be used by those rescuers who have been trained to do so, as they can push debris further down the airway or cause soft tissue injury if not used correctly.
Figure 6.1 Portable suction unit.

Figure 6.2 Head tilt to open airway.
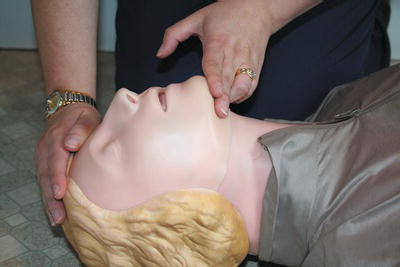
The casualty’s airway can then be opened to allow breathing to occur. This can be achieved by tilting the head back by placing the palm of one hand on the casualty’s forehead and lifting the chin with the fingers of the other hand at the same time (Figure 6.2). However, this technique must never be used when an individual has a suspected neck or spinal injury, as to do so would almost certainly cause further damage to the spinal cord. This could result in permanent paralysis. In these cases, the airway can be opened by thrusting the lower jaw forward with both hands, without any head tilting occurring (Figure 6.3). This should avoid any further neck or spinal injury.
Figure 6.3 Jaw thrust to open airway.
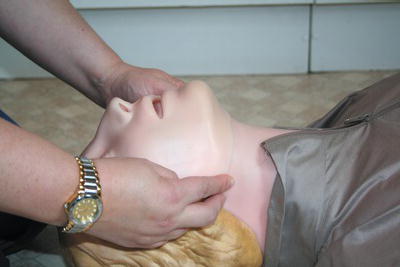
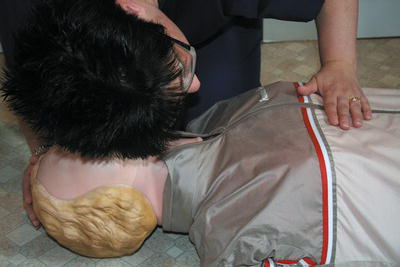
Figure 6.4 Look, listen, feel for signs of breathing.
Breathing
With the airway open, breathing is assessed quickly over a 10-sec period. The rescuer needs to determine if any spontaneous breathing attempts are being made, and their quality, by checking for the following (Figure 6.4).
- Look to see if the chest is rising and falling.
- Listen to any breathing sounds.
- Are they regular or infrequent?
- Are they quiet or noisy?
- Are they normal or gasping in nature?
- Feel for air flow by placing the cheek close to the casualty’s mouth.
If breathing is absent or abnormal, the emergency services must be called as specialist help is required. Ideally, a second person can be sent to do this but if necessary, the lone rescuer must leave the casualty and go to cal/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


