Eruption and shedding of the teeth
Learning objectives
Key terms
Diphyodont
Eruption pathway
Extracellular phase
Fibroblast
Functional eruptive phase
Gubernaculum dentis or gubernacular cord
Intracellular phase
Intraoral occlusal/incisal movement
Mixed dentition period
Movement
Osteoblasts
Osteoclasts
Penetration
Preeruptive phase
Prefunctional eruptive phase
Root formation
Ruffled border
Shedding
Tissues: overlying, surrounding, underlying
Overview
Tooth eruption is the process by which developing teeth emerge through the soft tissue of the jaws and the overlying mucosa to enter the oral cavity, contact the teeth of the opposing arch, and function in mastication. The movements related to tooth eruption begin during crown formation and require adjustments relative to the forming bony crypt. This is the preeruptive phase. Tooth eruption is also involved in the initiation of root development and continues until the tooth’s emergence into the oral cavity, which is the prefunctional eruptive phase. The teeth continue to erupt until they reach incisal or occlusal contact. Then, they undergo functional eruptive movements, which include compensation for jaw growth and occlusal wear of the enamel. This stage is the functional eruptive phase. Eruption is actually a continuous process that ends only with the loss of the tooth. Each dentition, primary and permanent, has various problems during eruption and in the sequencing of eruption in the oral cavity. Teeth differ extensively in their eruptive schedules as well. This chapter describes these events. Finally, the process of tooth shedding or exfoliation of the primary dentition is discussed (Boxes 6-1 and 6-2). Primary tooth loss results from three fundamental causes: root resorption, bone resorption, and size of crown too small to withstand mastication.
Preeruptive phase
The preeruptive phase includes all movements of primary and permanent tooth crowns from the time of their early initiation and formation to the time of crown completion. Therefore this phase is finished with early initiation of root formation. The developing crowns move constantly in the jaws during the preeruptive phase. They respond to positional changes of the neighboring crowns and to changes in the mandible and maxilla as the face develops outward, forward, and downward away from the brain in its maturing growth path. During the lengthening of the jaws, primary and permanent teeth make mesial and distal movements. Eventually the permanent tooth crowns move within the jaws, adjusting their position to the resorptive roots of the primary dentition and the remodeling alveolar processes, especially during the mixed dentition period from 8 to 12 years of age.
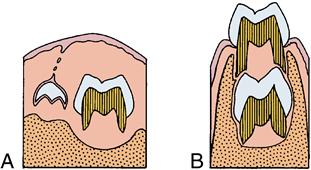
Early in the preeruptive period, the permanent anterior teeth begin developing lingual to the incisal level of the primary teeth (Figs. 6-1 and 6-2). Later, however, as the primary teeth erupt, the permanent successors are positioned lingual to the apical third of their roots. The permanent premolars shift from a location near the occlusal area of the primary molars to a location enclosed within the roots of the primary molars (see Fig. 6-2). This change in relative position is the result of the eruption of the primary teeth and an increase in height of the supporting structures. On the other hand, the permanent molars, which have no primary predecessors, develop without this type of relationship (Fig. 6-3). Maxillary molars develop within the tuberosities of the maxilla with their occlusal surfaces slanted distally. Mandibular molars develop in the mandibular rami with their occlusal surfaces slanting mesially (see Fig. 6-3). This slant is the result of the angle of eruption as the molars arise from the curvature of the condyle of the posterior mandible. All movements in the preeruptive phase occur within the crypts of the developing and growing crown before root formation begins.
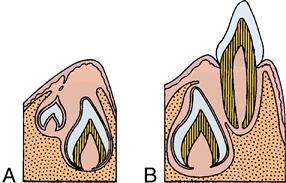
A, Preeruptive period. B, Prefunctional eruptive period.
Prefunctional eruptive phase
The prefunctional eruptive phase starts with the initiation of root formation and ends when the teeth reach occlusal contact. Four major events occur during this phase:
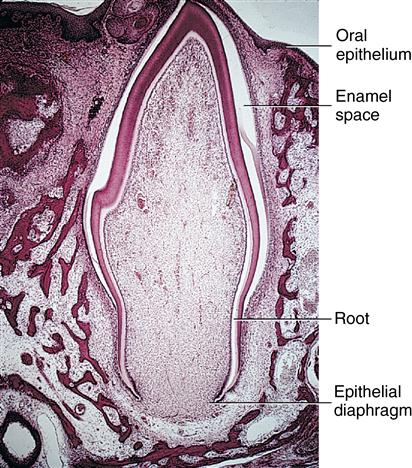
1. Root formation requires space for the elongation of the roots. The first step in root formation is proliferation of the epithelial root sheath, which in time causes initiation of root dentin and formation of the pulp tissues of the forming root. Root formation also causes an increase in the fibrous tissue of the surrounding dental follicle (Fig. 6-4).
2. Movement occurs incisally or occlusally through the bony crypt of the jaws to reach the oral mucosa. The movement is the result of a need for space in which the enlarging roots can form. The reduced enamel epithelium next contacts and fuses with the oral epithelium (Fig. 6-5). Both of these epithelial layers proliferate toward each other, their cells intermingle, and fusion occurs. A reduced epithelial layer overlying the erupting crown arises from the reduced enamel epithelium (Fig. 6-6).
3. Penetration of the tooth’s crown tip through the fused epithelial layers allows entrance of the crown enamel into the oral cavity. Only the organic developmental cuticle (primary), secreted earlier by the ameloblasts, covers the enamel (Fig. 6-7).
4. Intraoral occlusal or incisal movement of the erupting tooth continues until clinical contact with the opposing crown occurs. The crown continues to move through the mucosa, causing gradual exposure of the crown surface, with an increasingly apical shift of the gingival attachment (see Fig. 6-7). The exposed crown is the clinical crown, extending from the cusp tip to the area of the gingival attachment. In contrast, the anatomic crown is the entire crown, extending from the cusp tip to the cementoenamel junction.
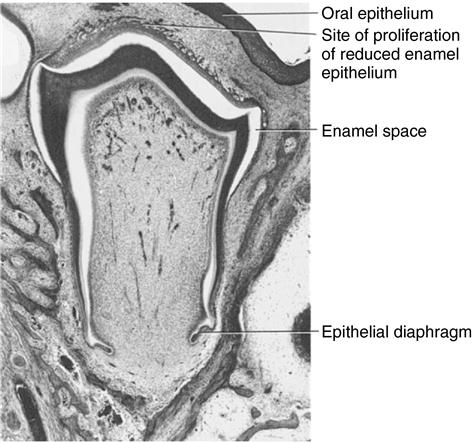
The root develops, and reduced epithelium overlying the crown approaches oral mucosa. Reduced enamel epithelium proliferates, anticipating fusion.
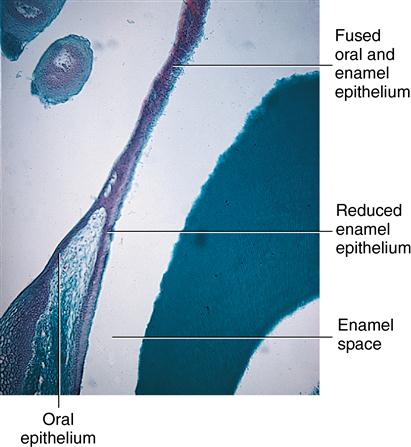
Enamel space occurs as enamel is dissolved in preparation of slide.

The permanent tooth’s position is shown on the left. The dashed line indicates cuticle overlying the enamel surface of the erupting tooth.
Changes in tissues
The prefunctional eruptive phase is characterized by significant changes in the tissues overlying, surrounding, and underlying the erupting teeth.
Overlying the teeth
The dental follicle changes and forms a pathway for the erupting teeth. A zone of degenerating connective tissue fibers and cells immediately overlying the teeth appears first (Figs. 6-8 and 6-9). During the process, the blood vessels decrease in number, and nerve fibers break up into pieces and degenerate. The altered tissue area overlying the teeth becomes visible as an inverted triangular area known as the eruption pathway. In the periphery of this zone, the follicular fibers, regarded as the gubernaculum dentis or gubernacular cord (Fig. 6-10), are directed toward the mucosa. Some scientists believe that these fibers guide the teeth in their movements to ensure complete tooth eruption.
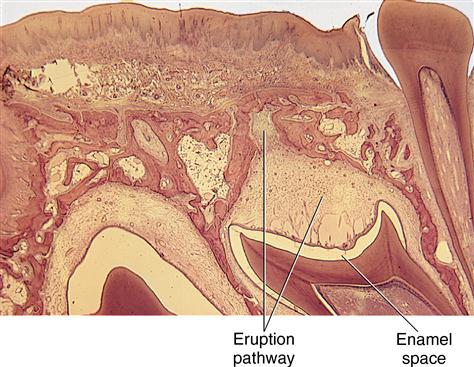
Observe the appearance of the eruption pathway developed overlying the crown.
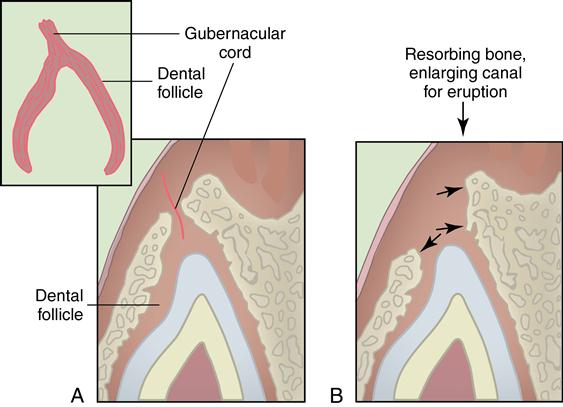
A, Early developing eruption pathway. B, Resorption of bone in eruption pathway.
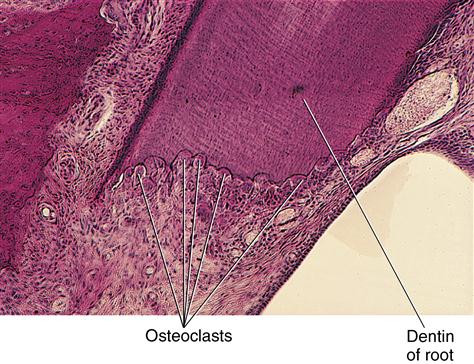
Macrophages appear in the eruption pathway tissue. These cells cause the release of hydrolytic enzymes that aid in the destruction of the cells and fibers in this area with the loss of blood vessels and nerves. Osteoclasts are found along the borders of the resorptive bone overlying the teeth. This bone loss adjacent to the teeth keeps pace with the eruptive movements of the teeth (see Fig. 6-9). Osteoclasts and osteoblasts constantly remodel the alveolar bone as the teeth enlarge and move forward in the direction of the growing face.
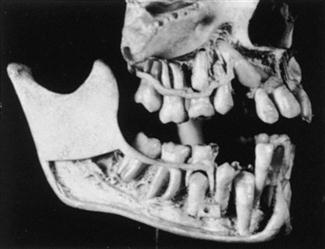
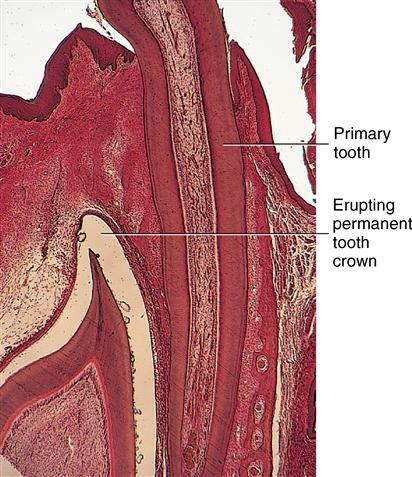
Although the process of eruption for permanent teeth is similar to that of the primary teeth, the presence of roots from primary teeth poses a problem. The resorption of their roots is similar to the process of bone resorption for the emergence of primary teeth. Permanent teeth establish an eruptive path lingual to the primary anterior teeth and the premolars under the primary molars. Permanent molars erupt into the alveolar free space behind primary teeth (see Fig. 6-9). Small foramina just posterior to the primary tooth row are evidence of the eruption sites of the anterior permanent teeth (Fig. 6-11). As the roots resorb, the primary crowns are lost or shed (Fig. 6-12). Dentin resorption is similar to bone resorption (see Fig. 6-10).
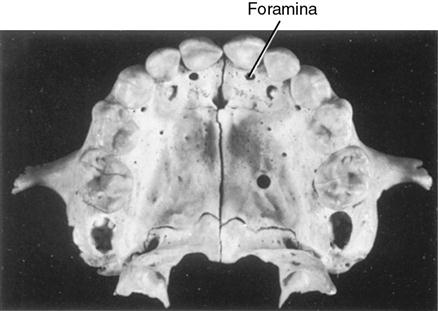
These are sites of eruption for permanent incisors.
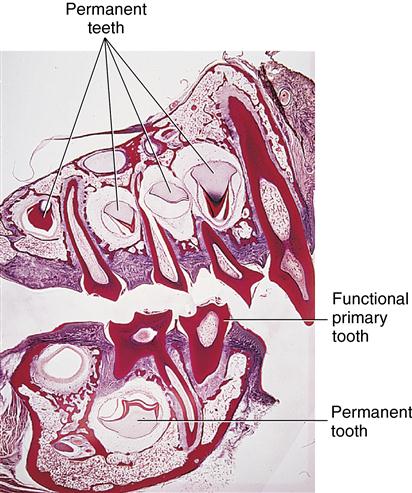
Roots of erupted primary teeth are undergoing resorption. Crowns of developing permanent teeth appear below primary teeth.
The resorptive process of primary and permanent teeth results from action of osteoclasts that arise from monocytes of the circulating bloodstream. These monocytes appear and fuse with others to form the multinucleated osteoclasts. Their function is to resorb the hard tissue. They do so by first separating the mineral from the collagen matrix through the action of the hydrolytic enzymes secreted by the osteoclasts. This enzymatic action is believed to occur within lacunae, which are developed by the osteoclasts. The osteoclast’s cell membrane is in contact with the bone and becomes modified by an enfolding process termed the ruffled border (Figs. 6-13 and 6-14). This border greatly increases the surface area of the osteoclast and allows the cell to function maximally in bone resorption (Fig. 6-15).
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses