Dental Fear and Behavior Management Problems
Gunilla Klingberg and Kristina Arnrup
The prevention and treatment of oral diseases in childhood and adolescence as the basis for good oral health throughout life is the aim of pediatric dentistry. There are two main, equally important, issues within this goal: (a) to keep the oral environment healthy, and (b) to keep the patient capable of using and willing to use the dental service. This chapter deals with the second of these issues, including how to help children to cope with dental treatment and how to prevent development of dental anxiety and odontophobia.
Children and adolescents show tremendous variation in maturity, personality, temperament, and emotions, leading to a corresponding variation in vulnerability and ability to cope with the dental treatment situation. As a consequence of this, the pediatric dentist needs a repertoire of strategies, in addition to the dental treatment techniques, to prevent behavior management problems and to manage children who display such problems. This repertoire should involve both psychological and pharmacological techniques.
Definitions and prevalence of dental fear and anxiety
Many children perceive a visit to the dentist as stressful. This can be expected since an appointment includes several stress‐evoking components, such as meeting unfamiliar adults and authority figures, strange sounds and tastes, having to lie down, discomfort, and even pain. Uncooperative behavior and fear reactions are, therefore, common encounters in the daily dental clinical situation. The reported prevalence of dental fear/anxiety and behavior management problems varies in different populations, but have both been estimated to affect 9% of children and adolescents [1].
Fear may be described as a natural emotion based on the perception of a real threat, while anxiety is associated with fear reactions towards a situation of an anticipated, but not realistic, threat. Anxiety may therefore be looked on as a more disorder‐like type of fear among those who have not been able to adapt to specific fearful situations. Phobia is a disorder that is diagnosed according to clinical criteria (Box 6.1). Based on these descriptions it is likely that dental fear as well as dental behavior management problems have their peaks at a young age followed by rather drastic decline, while dental anxiety starts during early school age and then shows moderate increase. Dental phobia will probably affect fewer individuals, and show a more moderate increase as the young individual grows older (Figure 6.1). It is difficult to differentiate fear from anxiety in the clinical situation, and the terms dental fear and dental anxiety frequently are used interchangeably, as in this chapter.
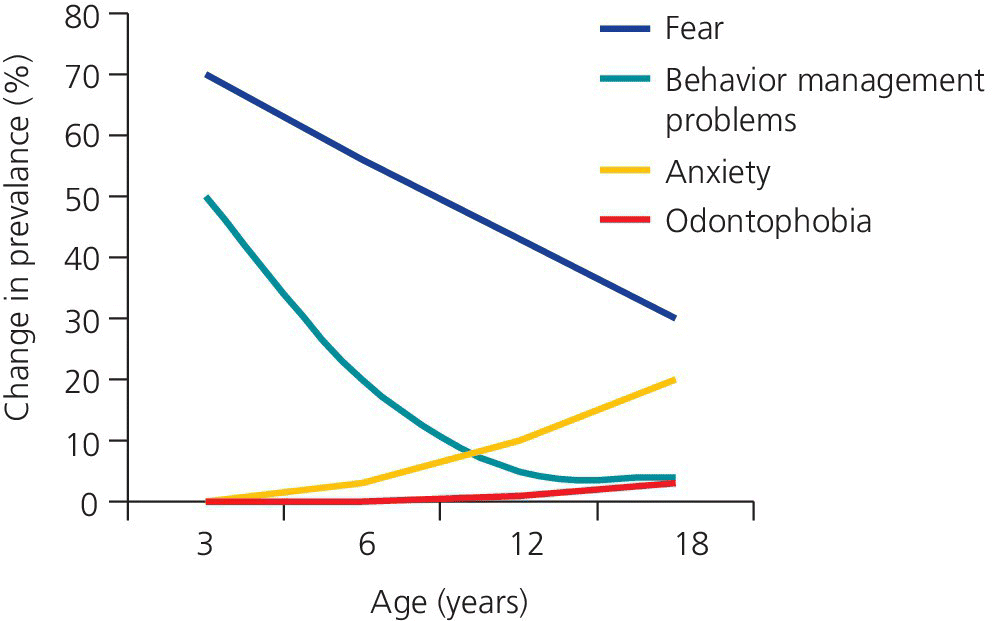
Figure 6.1 Estimated changes in prevalence of dental fear, dental anxiety, dental phobia and behavior management problems in children and adolescents
Expressions of dental fear and behavior management problems
A very relevant question to ask is: “Is it possible to distinguish between dental fear and behavior management problems in the clinical situation?” (Box 6.2). There is no simple answer to this. In the clinical situation the dentist is not likely to miss a child presenting with behavior management problems. Clinicians may empirically recognize the child with inadequate understanding, maturity, or ability to cooperate. A child who is acting out by crying or physically resisting may be contrasted to a child whispering to his or her mother, making no eye contact with the dentist and distancing himself or herself from interaction. Children with dental fear and anxiety can be outgoing in their general behavior, but are sometimes more passive and silent during treatment. Thus, there is the risk of overlooking that a patient is anxious, which may increase the risk for unintentionally harming him or her. It is important not to take cooperative behaviors alone as a sign of the child feeling comfortable. With increased knowledge about signs and causes of dental anxiety and behavior management problems, the dentist will become more attentive to these problems.
Etiology
Dental anxiety and behavior management problems in children are phenomena of multifactorial and complex origins. Three main domains of etiologic factors can be identified (Figure 6.2). As the different components in each of the domains or groups vary in importance over time, the patient’s apprehension of anxiety as well as the behavior during dental treatments may vary. New aspects may be added leading to an increase in problems or, conversely, the child may learn to handle some of the anxiety‐provoking components, leading to a decrease in problems. Thus, time is an important variable. The child patient we see today will grow to be an adult patient of tomorrow. From research about dental anxiety and odontophobia in adults we know that they often identify the origin of their problems as negative experiences during dental treatment in childhood and adolescence. In cases where the initial fear and behavior management problems lead to avoidance of dental treatment, there is a great risk of entering a vicious circle, leading to dental anxiety and odontophobia and deterioration of dental health over time. Prevention of this negative development is a major task for pediatric dentists.
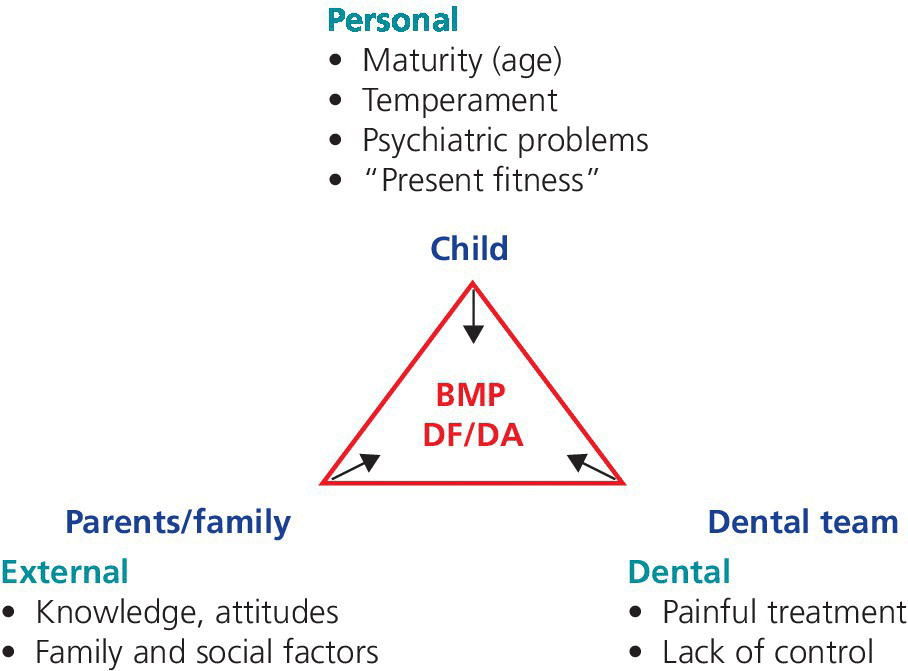
Figure 6.2 The reasons for dental fear/anxiety (DF/DA) and dental behavior management problems (BMP) are multifactorial and complex. Three groups of factors have been identified: personal, external, and dental factors. The impact and relative importance of the different factors vary between children and individually over time. If DF/DA and/or BMP lead to avoidance of dental treatment, there is a risk of entering and maintaining a vicious circle which may lead to odontophobia.
Personal factors
One of the most important factors in explaining the occurrence of dental anxiety and behavior management problems is the age of the child. Both dental fear and behavior management problems are more common in young children, reflecting the influence of a child’s psychological development on his or her ability to cope with dental treatment [1]. A young child may experience and understand the dental situation differently than older children. One major reason for this is that the process of understanding and having the motivation to comply with dental treatment differs depending on psychological development. The latter is also dependent on communication skills in the dental teams. After all, dental treatment requires a great deal from a child: to lie down without moving; to tolerate discomfort; strange tastes; maybe even pain; and all this in an unfamiliar environment with strange people, etc.
All children go through developmental periods of obstinacy often coinciding with the crisis that the child is dealing with during the different phases in his or her socioemotional development. These normal, but trying, periods are sometimes revealed as behavior management problems in the dental treatment situation. When talking to the parents they often describe a sudden change in the mood of their child, from compliant and easy‐going to showing and testing behavior and stubbornness. This is a transient period that will pass in a couple of weeks or maybe a month or two.
Symptoms of fear and anxiety are normal developmental phenomena in children, and many children display a relatively high number of anxiety symptoms without having anxiety disorders. Young children show fear of more and of different stimuli than older children. Several studies have shown a clear and positive relationship between high general fear level, emotional disorders, or general anxiety on the one hand and dental fear and anxiety, or behavior management problems on the other [1]. Associations between fear problems such as medical fears, fear of the unknown, and fear of injury on the one hand and dental fear and anxiety on the other have been reported.
In this context it is important to bear in mind the difficulties of distinguishing between dental fear and dental anxiety in children. The visit to the dentist could well be fearful to many children without giving rise to anxiety. Fearful reactions in young children are natural and this may explain the high prevalence in these age groups. Persisting dental fear, dental anxiety, and phobia developing later in childhood should be regarded as pathologic phenomena.
Fear/anxiety/phobia of blood, injections, and injuries is a special type of anxiety that frequently seems to interact negatively with dental treatment, since most of these children are fearful of dental injections (blood–injection–injury phobia: BII phobia) [2]. There is a strong tendency to faint or nearly faint when exposed to the fearful stimuli, which is unique to this type of phobia. The age of onset is thought to be early, which means that the prevalence is highest among young children. Positive relationships between BII phobia and dental anxiety and dental avoidance have been shown, indicating that BII phobia is a contributing factor.
Temperament is a personal emotional quality that is moderately stable over time and appears early in life. It is also believed to be under some genetic influence. Difficulties approaching novel situations and unfamiliar people have been reported to characterize children with dental fear and/or behavior management problems. Associations have also been reported with characteristics described as “negative mood,” “unhappy child,” “easily distressed,” or “impulsiveness.” Thus, dental fear and/or behavior management problems have been associated with aspects of children’s temperament (Box 6.3) [1]. One dimension of temperament is shyness, which is found in about 10% of children. Shy children need extra time to feel at ease with the situation. Another temperamental dimension, associated with dental fear as well as behavior management problems, is negative emotionality. Children with behavior management problems have also been reported to score higher on activity and impulsivity.
Looking at fear, temperament, and behavior together, different subgroups have been identified among children with dental behavior management problems. Among these subgroups are children with high dental and general fear, children with fear combined with inhibited temperamental profile (shyness, negative emotionality, and internalizing behavior), and children with less pronounced fear combined with impulsiveness and externalizing/outgoing behavior [3].
In the group of children with dental anxiety without uncooperative behaviors it seems likely to find children with pronounced shyness or an inhibited temperamental profile. These children are well aware of how they should behave during a dental visit and therefore cope well with the treatment despite their anxiety. These children require special awareness on the part of the dental team during treatment in order not to be forced beyond their coping abilities. As inhibited children do not have an outgoing behavior, the lack of uncooperativeness could be misinterpreted for agreeing with the treatment situation if the dentist is not aware of this temperamental trait.
Uncooperative behavior in dental care situations may also be related to neuropsychiatric disorders such as attention deficit hyperactivity disorder (ADHD), autism spectrum disorders, or to intellectual disability. Dental anxiety and behavior management problems have been reported to occur more frequently in children with ADHD [4]. Approximately 5% of children are expected to have some kind of neuropsychiatric disorder [5]. ADHD represents a significant proportion with prevalence figures reported to vary from 3 to 7% [6].
External factors
It is well known that parental dental anxiety affects dental anxiety in children [7]. Children may also acquire dental fear through social learning from siblings, other relatives, and friends. Apart from transmitting subtle feelings of fear and anxiety to their children, fearful parents sometimes also interfere with the dental treatment of their child, for example by questioning the need for injections or restorative treatments, or may give accounts from their own negative experiences. On these occasions they may serve as live and powerful negative models of dental anxiety for their children. Studies among adult odontophobic patients by Berggren and Meynert [8] and Moore et al. [9] have reported that negative family attitudes towards dental care and dental fear in the family were common reasons for the development of odontophobia. For many of these adult patients the problems with dental fear and anxiety started in childhood, often even before their first dental visit.
The social situation of the child is likely to be of importance. Children live under different circumstances in modern society, sometimes also on the margins of society in one aspect or another. Dental fear problems have been reported to be more frequent in subpopulations such as immigrants. Groups with lower socioeconomic standards have also been reported to exhibit a higher prevalence of dental anxiety and behavior management problems. It is possible that these differences can be leveled out to some extent in countries where organized free dental care for children is provided. Hence, some studies from Sweden and Norway have failed to establish a relationship between socioeconomic variables and dental fear. One explanation might be that oral health is less affected by socioeconomic standards in these populations. A child who has good oral health runs a smaller risk of caries and filling therapy and thereby a smaller risk of encountering discomfort and pain in the dental situation. Family risk factors (for example, parents not living together and low socioeconomic status) per se are not presumed to influence children’s fear and behavior, but rather to influence parents’ attitudes and behavior, and thereby their ability to guide and support their children during dental treatment. A Swedish study among patients referred for specialized pediatric dental care because of dental behavior management problems reports that the referred children and adolescents more frequently have a “burdensome” life and family situation, including low socioeconomic status, and parents not living together [10].
Children in refugee families are in a vulnerable situation since the children and their parents generally bear traumatic memories and many have post‐traumatic stress syndrome. The numbers of refugee families have increased over the years and it is important to remember that some of them have been involved in war, or have even been subjected to torture, etc. Traumatized parents can have problems supporting their children in oral health behavior as well as in coping with dental care. A dental care situation, with its ingredients of intense lights from the operatory lamp, dental instruments in the mouth, strange tastes, and smells, can lead to flashbacks. For children in such circumstances, the risk of developing dental anxiety is obvious.
Child rearing may also have an impact on how the child will comply with dental treatments. Dental teams often identify factors related to family or upbringing as a cause of problems. The situation for both children and parents has changed over the past few decades and continues to do so. In many countries this has led to an alteration of the role children play in society. Previously, the distinctions between childhood and adulthood were clearer. The adult, a parent, a schoolteacher, or dentist was more clearly the one setting the rules and leading the way. Today, children frequently question adult people’s authority and this certainly affects the dental treatment situation. However, the cultural context of the child can imply great variation on this theme.
Dental factors
One of the most commonly mentioned causes of dental fear/anxiety and behavior management problems is painful dental treatments. Pain is defined by the International Association for the Study of Pain [11] as an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. It is important to acknowledge that the sensation is not necessarily dependent on tissue damage; it may also be generated by conditioned stimuli such as the sound of the drill or a gentle touch of the needle. Since painful stimuli normally bring about physiological and psychological reactions to protect the body from tissue damage, uncooperative behavior is a logical and relevant reaction when a child experiences pain or discomfort. Unfortunately, experiences of pain are not uncommon in child dental care, since it has been shown that many children have, for instance, restorative treatments carried out without local anesthesia [12,13].
Children’s understanding of (and vulnerability to) pain varies considerably depending on cognitive abilities, and the reactions and thoughts concerning painful stimuli vary according to age and maturity [14]. In addition to this, factors such as the child’s socioemotional development, family and social situation, parental support, kind of rapport with the dental team, etc., affect how the child will cope with stress, pain, and discomfort. There is also a growing body of evidence showing that children who have been subjected to painful procedures without adequate anesthesia develop increased perception of pain about future procedures, despite adequate pain control [15]. One strong painful dental stimulus could be enough to cause dental fear and anxiety in a vulnerable child patient. However, repeated exposure to dental treatments that are only somewhat discomforting or a little painful, or are perceived as such by the child, can have the same result. It is, therefore, not acceptable from an ethical point of view to withhold local anesthesia from children, especially as this is a documented way to reduce or even prevent pain.
Perceived lack of control has been shown to be another major triggering factor for behavior management problems and dental fear/anxiety [16]. This may imply that the child patients have not been properly informed about the treatment (informational control), or that they have deprived influence of their own behavior (behavioral control), or even that they are not given sufficient information after the treatment (retrospective control). Painful dental treatment in situations when the child feels lack of control has been shown to be particularly harmful [17].
Discomfort goes hand in hand with pain and children frequently have problems distinguishing between the two. Discomfort can represent a psychological comprehension of a stressful situation. This is often experienced in novel situations, if the child is frightened about what will happen, or feels lack of control, etc.
It seems possible to assume that a large proportion of the behavior management problems and refusal to go along with treatment reflects the fact that children are fearful, particularly when they perceive pain, discomfort, or stress. These are normal and fully adequate reactions, especially in young children lacking experience of their own coping ability. However, it is still an important task for the dental team to prevent these adverse reactions and, if they occur, to handle them properly in order to prevent further development of dental anxiety.
The dental team has a delicate task when treating child patients. They represent authority and can, if perceived in this way, imply a threat or something frightening to some children. The attitudes towards children among dentists and other members of the team are important as to how they behave and interact when treating children. As attitudes also include cognition it is important that dental personnel working with children have a good knowledge not only of dentistry, but also of children, child development, and child psychology. Child competency is a concept grounded in the United Nations (UN) Convention on the Rights of the Child. It encompasses the knowledge and competencies we need to have in order to fulfill the requirements that the convention states regarding personnel within the health sector. In order to provide high‐quality comprehensive care including communication with the child patient and his or her family we as dentists need to ensure that we acquire and maintain child competency.
Principles of management
This section deals with the use of psychological techniques for the prevention of behavior management problems and dental fear/anxiety/phobia, as well as how to manage children displaying such problems. Knowledge of the multiple and interacting etiologic factors of fear, anxiety, and behavior management problems is necessary in order to be successful in these tasks. As already explained, etiologic factors can be described within three domains:
- personal factors
- external factors
- dental factors.
The first two of these determine how vulnerable the child is when entering the dental clinic. Irrespective of age, some children are very robust and tolerate a lot, while others are vulnerable and respond negatively even to minor stress stimuli. The dental staff has no influence on this, but they must be sensitive and adapt their behavior and treatment strategy to it. Dental factors are those that the dental staff are able to control. The prevention of pain and discomfort combined with the establishment of a good psychological relationship with the child and his or her parents on the one hand, and the dental team on the other, are the major issues.
A complex network of interactions arises between the child, parent, dentist, and dental assistant when uncooperative or fearful children are treated. Each attempt to treat must be preceded by diagnosis and planning, which, for children, also involves the parent to a varying degree. The concept of informed consent, parental permission, and assent from the child has been adopted from pediatric care, and the parent’s involvement during treatment has become standard. Thus, in addition to being a source of information, the parent is participating in a shared decision‐making and treatment‐planning process and is more likely to comply and adequately support their child when actively involved and informed. A relationship built on trust, empathy, and mutual respect gains patient cooperation.
The suggested treatment techniques are based on the principles of cognitive behavioral therapy (CBT) [18] and allow implications for prevention as well as treatment of dental fear/anxiety and/or behavior management problems. The cognitive component in CBT seeks to identify the beliefs that generate fear and avoidance in the clinical situation, and to produce a cognitive change in these beliefs. This is combined with behavioral exercises in which the child is helped to test his or her threat beliefs.
The practice of CBT in pediatric dentistry involves two basic issues:
- creating a safe environment
- graded exposure to feared stimuli.
Creating a safe environment
When a child is accompanied by his or her parents, it is necessary to establish an equally good and respectful communication with both the child and the adult (Box 6.4). This is an absolute prerequisite for founding the platform on which the diagnosing, treatment planning, and shared decision‐making have to take place. Time used for rapport building at the beginning of a treatment should be seen as a necessary investment in the relationship, which can be assumed to “repay” itself many times over during a child’s dental care career. If for some reason it is difficult to establish a good rapport and relationship with the child and/or parents, it is usually a good idea to have another dentist involved.

VIDEdental - Online dental courses


