Temporomandibular Disorders
Tomas Magnusson and Martti Helkimo
Definitions
Temporomandibular disorders (TMD) is a collective term embracing a number of clinical problems that involve the masticatory musculature, the temporomandibular joint (TMJ) and associated structures, or both [1]. The term is synonymous with the terms cranio‐mandibular disorders (CMD), functional disorders of the masticatory system, and mandibular dysfunction.
The most frequent reason for seeking treatment at a TMD clinic is pain, usually localized in the muscles of mastication and/or the TMJ. Typically the pain can be provoked and aggravated by chewing or by other jaw functions. TMD have been identified as a major cause of nondental pain in the orofacial region [1].
In addition to pain, limited or asymmetric mandibular movements, and TMJ sounds are commonly found in these patients. Common patient complaints also include jawache, earache, headache, and facial pain. Bruxism (jaw clenching and tooth grinding) and other oral parafunctions (e.g., nail‐biting and gum chewing) may be related problems.
Epidemiology
Signs and symptoms of TMD seem to be relatively common in the general population of adults. In cross‐sectional epidemiologic studies of adult populations, the prevalence rates range from about 40 to 75% having at least one sign and about 35% having at least one symptom of TMD.
It is almost impossible to get a clear picture as to occurrence of TMD in children and adolescents. Estimates of prevalence rates differ markedly from one study to another (Figure 22.1 and Table 22.1). This variation arises from a combination of factors such as inter‐ and intra‐individual variations among examiners, differences in the composition of the study populations, examination methods, choice of variables as well as a multitude of incomparable definitions and criteria for symptoms and signs.
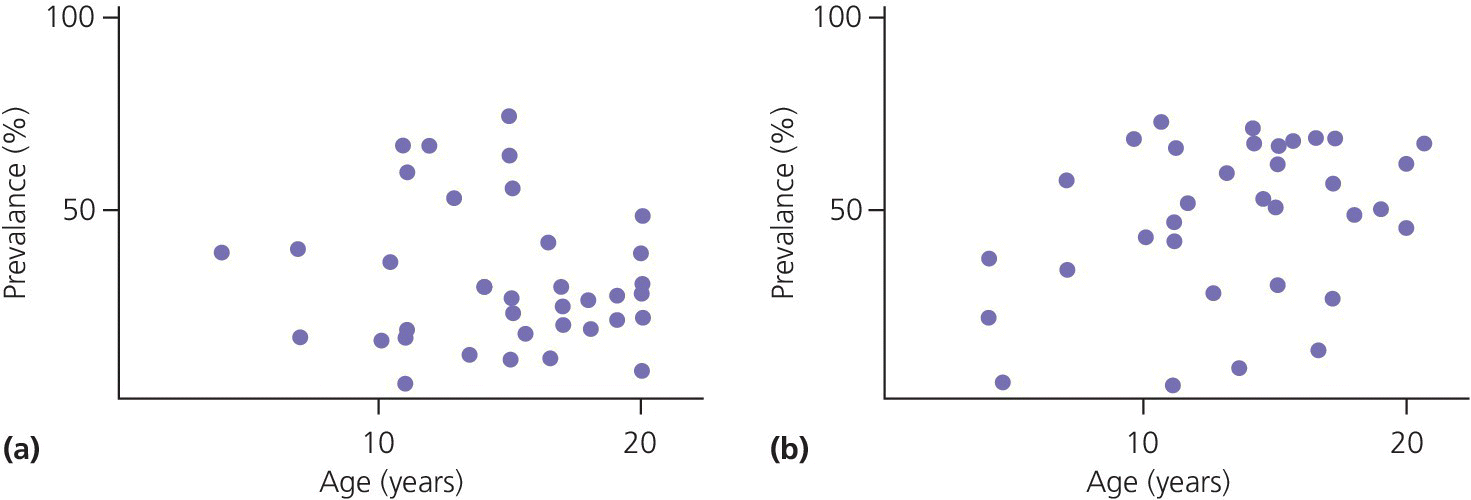
Figure 22.1 Diagrams showing prevalence of one or more (a) subjective symptoms and (b) clinical signs of TMD presented in different epidemiologic studies of children and adolescents. The single dots represent the prevalence figure found in different studies. Note the wide variations within the same age groups, ranging from single percent to more than 70%.
Adapted from Nydell et al. 1994 [2]. Reproduced with permission of the Swedish Dental Journal.
Table 22.1 Range and median values for the prevalences of (a) subjective symptoms and (b) clinical signs of TMD in different epidemiologic investigations
Adapted from Nydell et al. 1994 [2].
| All reported data | ||
| Range (%) | Median (%) | |
| (a) Subjective symptoms | ||
| Tiredness or stiffness in the jaws | 0–59 | 5.0 |
| TMJ sounds | 0–32 | 13.0 |
| Pain on opening the mouth or other jaw movements | 0.4–59 | 4.0 |
| Pain in the face or jaws | 0–19 | 3.0 |
| Headache | 1–88 | 13.2 |
| Difficulties in opening the mouth | 0–9 | 1.8 |
| Locking or luxation | 0.4–7 | 3.0 |
| One or more subjective symptoms | 3–74 | 26.2 |
| (b) Clinical signs | ||
| Impaired opening capacity | 0–29 | 1.8 |
| TMJ sounds | 0–50 | 19.2 |
| Deviation upon opening and closing the jaw | 0–78 | 6.5 |
| Locking or luxation | 0–1 | 0.5 |
| Tenderness on palpation of the TMJ | 0–44 | 4.0 |
| Tenderness on palpation of the masticatory muscles | 1–68 | 21.2 |
| Pain upon movement | 0–18 | 2.5 |
| One or more clinical signs | 2–78 | 51.2 |
Another plausible, and often overlooked, reason for the great variation in the reported frequencies of signs and symptoms of TMD is that examination methods designed for adults have been applied uncritically on children without taking the age and cognitive development of the child into consideration [2].
In spite of the large volume of data from recent literature on the epidemiology of TMD, it is still not possible to make a conclusive statement as to the “true” prevalence of TMD signs and symptoms in children and adolescents, nor can we even say if these phenomena change with age. In recent years, a change has been taking place in how we look upon the condition. In earlier years, research was focused on functional disturbances in the masticatory system, and thereto associated pain. Today, focus has shifted—in many quarters—to research, diagnosis, and treatment of pain occurring in the orofacial area irrespective of its etiology. TMD is, by some authors, regarded as a chronic pain condition. This implies that it is difficult, or even impossible, to compare results from epidemiologic studies from later years with early ones, especially if symptom criteria are ambiguously defined in the studies. Despite these shortcomings, it is obvious from longitudinal studies that symptoms and signs show great fluctuation with time [3,4]. Most signs and symptoms seem to come and go in an unpredictable way [5,6]. In a 20‐year longitudinal study, no significant progression of signs and symptoms of TMD from childhood, through adolescence, to adulthood have been found [7]. In addition, cross‐sectional epidemiologic studies covering a 20‐year period have shown that the estimated TMD treatment need in 10‐ and 15‐year‐olds was 3–4% and 2–5%, respectively [8].
From the many epidemiologic studies performed in this field, it can be concluded that signs and symptoms of TMD in children and adolescents are in most cases occasional and mild, except for some rare conditions and diseases such as juvenile idiopathic arthritis (Still’s disease), which can be progressive and develop into severe functional limitation and pain in some few individuals.
Bruxism
Oral parafunctions include bruxism, lip‐biting, thumb‐sucking, and abnormal posturing of the jaw. In contrast to normal functional behaviors, such as chewing and swallowing, these parafunctional behaviors seem to have no obvious functional purpose.
Parafunctional activities are very common in all age groups, and only occasionally have significant negative effects on the structures of the masticatory system. As in adults, muscular pain, headache, and TMJ overloading may result also in children. In those cases, a protective bite splint may be indicated.
Nail‐biting and excessive chewing on chewing gum are fairly common habits in children and adolescents, and can be as important etiologic factors for TMD as tooth grinding and tooth clenching. Unphysiologic sleeping posture, e.g., belly sleeping, can also result in unfavorable loading of the TMJs and be a contributory factor to dysfunction of the joints.
In most cases, nocturnal bruxism in children does no harm. The patients and parents should be informed that, although very loud sounds may occur, there is little evidence that permanent damage results from bruxism in childhood. On the contrary, it has been shown that tooth wear of primary teeth has a low predictive value for tooth wear of permanent teeth [9]. The child will in most cases outgrow the behavior in time. It has even been suggested that bruxism in small children is a physiologic phenomenon necessary for a normal eruption of the permanent teeth. However, tooth wear at 14 years of age, when the “mature” dentition is established, is a good predictor for further wear [9].
TMD and orthodontics
The possibility that orthodontic treatment in childhood might be a risk factor for the development of TMD later in life has been an issue of great controversy in the dental literature for a long time. Several comprehensive review articles and meta‐analyses have focused on this question [10–13]. The conclusion from these studies is that there is no scientific evidence that orthodontic treatment increases the risk for development of TMD. On the contrary, there is some support for the conclusion that properly performed orthodontic treatment in childhood might have a positive effect on the functional status of the masticatory system later in life [14–16].
Taking the history in children and adolescents with suspected TMD
Taking the history in children entails several difficulties. For instance, many children try to please the questioner by giving the answer they believe is the desired one [17]. Because of this, care must be taken to avoid leading questions as far as possible when reviewing the history [18]. Another problem is that younger children cannot use language to express pain. Not until about the age of 12 years, at the end of the cognitive development and when the ability to think abstractly has developed, are children able to describe their pain verbally [19].
Bearing these limitations in mind, taking the history can be an important key to a correct diagnosis and a subsequent successful treatment. The history should be taken in a calm and confident atmosphere. The questions should be relevant and kept as simple as possible. Some examples of questions that should be included in the history are presented in Box 22.1.

VIDEdental - Online dental courses


