50 Outcomes of Endodontic Treatment
A patient will assess the success of an endodontic procedure by the resolution of any pain or swelling, but the clinician needs a more objective set of criteria to establish success. Strindberg (1956) published the first of the “modern” studies on the outcome of treatment, and he stated the necessary criteria to be:
• absence of pain or swelling;
• no loss of function;
• absence or resolution of a fistulous tract;
• resolution of an area of radiolucency associated with the treated tooth, based on examination of the radiograph.
These criteria are still used today, although to complete resolution of an area of radiolucency, partial resolution or “incomplete healing” is commonly added.
Failure is obviously the absence of some or all of these criteria, although Friedman (2002) has recently argued that the terms “healed” and “failure to heal,” or “persistence of disease,” are more accurate.
Numerous studies have been published since Strindberg’s on the outcome of endodontic treatment, although the majority would today be considered to have fairly low levels of evidence. There are many factors that influenced these studies, for example: the sample size; whether the work was carried out by a single operator or a number of operators; the observation period; the follow-up interval; whether the observers were distinct from the clinicians and whether they had been trained and their degree of interexaminer agreement appraised; the lighting conditions for viewing radiographs; the reexamination of a proportion of the radiographs for consistency of reporting; the strictness of the criteria themselves (i.e., did success or healing mean only complete resolution of areas of radiolucency, or did it include partial resolution as well); and finally, was the study prospective in design or retrospective?
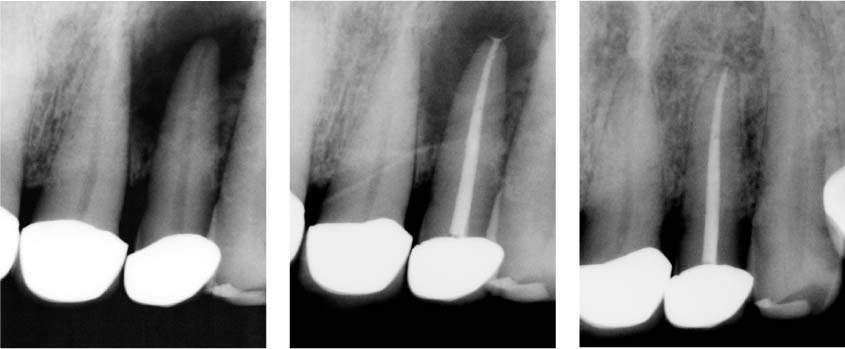
50.1 Primary endodontic therapy I
Left: Tooth 22 exhibits an extensive apical radiolucency.
Middle: Completed root canal filling.
Right: Follow-up radiograph 1 year later. Complete healing, with regeneration of a normal periodontal ligament space.
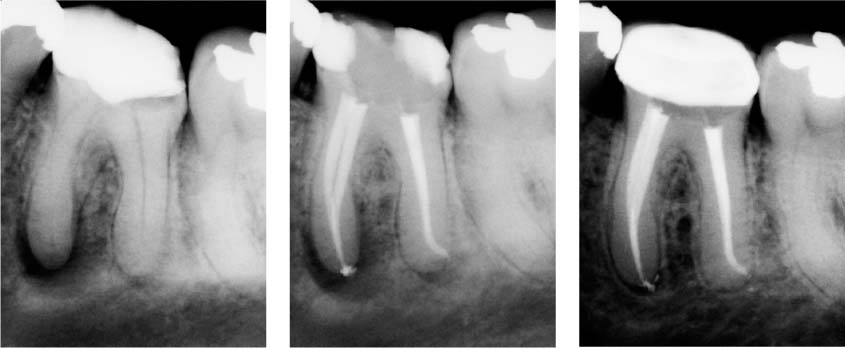
50.2 Primary endodontic therapy II
Left: Extensive lesion in the region of the mesial root of tooth 36.
Middle: Completed root canal filling.
Right: Follow-up radiograph 1 year later. Significant, but yet incomplete healing. The periodontal ligament space appears to be widened. The tooth was symptom-free.
Over the past decade or more, there have been many cross-sectional studies examining full mouth periapical or panoramic radiographs to assess the presence of apical periodontitis in untreated teeth and those that have received root canal therapy. Although the papers derive from many different countries, the results have been surprisingly similar and reveal a much higher percentage of affected areas associated with root filled teeth, with an overall mean in the region of 35%.
It is apparent that the rate of healing for treatment carried out in general dental practice throughout the world is significantly lower than when treatment is provided by specialists or students, undergraduate and postgraduate, when under close supervision. One can presume that most, if not all, of the latter treatment was carried out under rubber dam, whereas it is generally accepted that this simple device is used by a lower proportion of general dental practitioners.
In addition to the standard of care provided, the other significant factors influencing healing, reported consistently in some of the studies in Fig. 50.3, are the presence of an existing area of radiolucency on the pr/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses