CHAPTER 50 Oral Complications of Cancer Therapy
These various advances in cancer therapy are lifesaving, but often have significant morbidity and complications. Considerable attention is now being paid to the medical significance of complications of cancer therapy and the effects these complications have on quality of life. Studies have shown that the oral complications of cancer therapy can significantly interfere with the course of cancer therapy, adversely affect general quality of life, and increase the cost of care.78 In addition, a number of chronic orofacial complications can significantly affect long-term quality of life and oral function after cancer therapy. Successful prevention and treatment of the oral complications of cancer therapy can reduce pain, suffering, and disability while decreasing the risk of complications that may interfere with ongoing cancer therapy or result in lifelong functional compromise.
ORAL COMPLICATIONS OF CHEMOTHERAPY
In general, the therapeutic effects and toxicities of cancer chemotherapy arise from damage to rapidly dividing cancer and normal cells. Only a few anticancer agents can specifically target cancer cells. Consequently, most cancer chemotherapeutic agents inadvertently damage normal tissues of the body. Because the growth fraction for cancer is usually much higher than most normal tissue compartments, there is a quantitative difference in damage to the cancer cells compared with normal cells. Although systemic toxic effects of cancer chemotherapy usually result from damage to rapidly dividing cells, some toxicities result from damage that is not specifically related to cell division (Box 50-1).
Oral complications of cancer therapy may result directly from the cytotoxic effects (direct toxic effects) of the drugs on oral tissues (including salivary glands) or result from therapy involving distant tissues (indirect toxic effects). The clinical presentation of complications generally represents the results of complex interactions among multiple factors. These oral complications are listed in Box 50-2.
A number of factors affect the clinical expression of oral toxic effects of chemotherapy, the most prominent being which chemotherapeutic agent is administered along with its dose and schedule. The high turnover rate of oral mucosal tissues puts them at risk for the cytotoxic effects of many antineoplastic agents. Direct mucosal damage may be accentuated by many factors, including (1) salivary gland dysfunction, which compromises the barrier and lubricating functions provided by saliva; (2) mucosal trauma or irritation (e.g., from normal oral function, medications, and mouth breathing); and (3) infections caused by indigenous oral flora (especially opportunistic oral pathogens), acquired pathogens, and the reactivation of latent herpesviruses that cause local and systemic complications in patients who become immunosuppressed.62
Direct Oral Toxic Effects
Oral mucositis
The terms oral mucositis and stomatitis were often used interchangeably in the past, but they do not reflect identical processes. Stomatitis is a more general term and is applied to any inflammatory condition of the oral tissues, regardless of cause, including infections and autoimmune disorders. The term oral mucositis is increasingly being applied to inflammation and breakdown of the oral mucosa resulting from damage caused by chemotherapeutic agents or radiation therapy.64 Oral mucositis is the preferred term to represent the direct mucosal toxicity of cancer therapies on oral mucosal tissues.
Epidemiology
Oral mucositis is a significant problem in patients receiving chemotherapy for solid tumors. In one study, 303 of 599 (51%) patients receiving chemotherapy for solid tumors or lymphoma developed oral or gastrointestinal (GI) mucositis, or both.17 Oral mucositis developed in 22% of 1236 cycles of chemotherapy, GI mucositis developed in 7% of cycles, and oral and GI mucositis developed in 8% of cycles. Among patients who receive high-dose chemotherapy before HCT, an even higher percentage (approximately 75% to 80%) developed clinically significant oral mucositis.83
Morbidity
Oral mucositis can be very painful and can significantly affect nutritional intake, mouth care, and quality of life.16,42 For patients receiving high-dose chemotherapy before HCT, oral mucositis has been reported to be the most debilitating complication of transplantation.4,80 In patients immunosuppressed because of chemotherapy, increased severity of oral mucositis was found to be significantly associated with an increased number of days requiring total parenteral nutrition and parenteral narcotic therapy, increased number of days with fever, incidence of significant infection, increased time in the hospital, and increased total inpatient charges.83 A reduction in the next dose of chemotherapy was twice as common after cycles with mucositis than after cycles without mucositis.17 Mucositis is not only a concern for pain and suffering, but can also cause dose-limiting toxicity of cancer chemotherapy with direct effects on patient survival.
Pathogenesis and clinical presentation
The mucosal surfaces throughout the oral cavity have different cellular turnover rates, which can vary from 4 to 5 days for nonkeratinized buccal and labial mucosa to 14 days for the orthokeratinized hard palate. The more rapid the cell division rate of the progenitor epithelial cells, the higher the susceptibility to damage from chemotherapy and radiation therapy. The mechanisms involved are more complex, however, than simply direct damage to oral epithelial cells from chemotherapy or radiation therapy. The currently accepted model for the pathogenesis of mucositis postulates five stages associated with tissue damage and healing. Initiation of direct tissue injury is thought to be mediated by production of reactive oxygen species resulting in cell death. This stage is followed by activation of second messengers that upregulate the production of proinflammatory cytokines in mucosal epithelium and submucosal tissues and lead to widespread tissue injury. Through feedback mechanisms, these cytokines can amplify the cascade of tissue injury further, leading to ulceration and secondary infection. The final stage is characterized by the stimulation of epithelial proliferation and differentiation, leading to mucosal healing.77
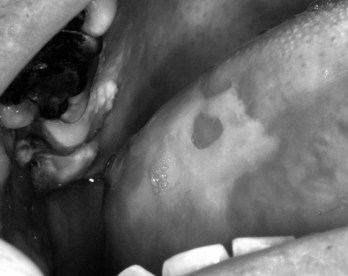
Histologically, the mucosal damage is characterized by mucosal atrophy, inflammatory cell infiltrates, collagen degradation, and edema.49 Clinically, these changes are initially evident as mucosal redness. As the damage increases to basal epithelial cells, ulceration can manifest as isolated lesions. The process progresses to confluent ulcers, often covered by a white pseudomembranous fibrin exudate (Figure 50-1).
Because of the complex cascade of events that occur, lesions may arise 1 to 2 weeks after stomatotoxic chemotherapy. Lesions are usually limited to nonkeratinized areas such as the buccal and labial mucosa, lateral tongue, and soft palate. Keratinized tissues, such as the attached gingiva, dorsal tongue, and hard palate, are less commonly affected. Mucositis typically heals 2 to 4 weeks after the last dose of stomatotoxic therapy has been delivered.43 Oral infections caused by organisms acquired during hospitalization and the reactivation of latent viruses (e.g., herpes simplex virus [HSV], cytomegalovirus [CMV], varicella-zoster virus [VZV]) can also influence the clinical presentation of mucositis and may prolong the duration of ulcerative lesions.
Management
Management of mucositis currently is focused on palliation of pain and efforts to reduce the influence of secondary factors on mucositis. Based on an extensive systematic review of the literature, the Mucositis Study Group of the Multinational Association for Supportive Care in Cancer and the International Society of Oral Oncology (MASCC/ISOO) has developed clinical practice guidelines for the management of mucositis.37 These guidelines are discussed subsequently and addressed in Table 50-1.
| CLASS OF AGENT | AGENT | STATUS OR MASCC/ISOO* GUIDELINE REGARDING MANAGEMENT OF ORAL MUCOSITIS |
|---|---|---|
| Cryotherapy | Ice chips placed in the mouth starting 5 min before administration of chemotherapy and replenished as needed for 30-60 min, depending on half-life of agent | Recommended during administration of bolus chemotherapy with 5-fluorouracil, edatrexate, and melphalan55 |
| Growth factor | IV keratinocyte growth factor-1 (Kepivance, Amgen) | Recommended in patients with hematologic malignancies receiving high-dose chemotherapy and total body irradiation before autologous stem cell transplantation; FDA-approved in this population79,85 |
| IV fibroblast growth factor-20 (Velafermin, CuraGen) | Development for chemotherapy-induced mucositis recently halted because of negative results from clinical trials45 | |
| Anti-inflammatory agents | Benzydamine hydrochloride mouth rinse | Recommended for patients receiving moderate-dose RT, based on previous evidence,24,44 but not FDA-approved; phase III trial halted because of negative results of interim analysis |
| Antioxidants | IV amifostine (Ethyol, MedImmune) | No guideline; insufficient evidence of benefit for radiation-induced oral mucositis6,9 |
| Topical N-acetyl cysteine (RK-0202, RxKinetix) | Currently in clinical trials for radiation-induced oral mucositis68 | |
| Promoters of healing | Topical glutamine (Saforis, MGI Pharma) | Currently in clinical trials for chemotherapy-induced oral mucositis63 |
| Antimicrobial agents | Antimicrobial lozenges | Not recommended for prevention of radiation-induced oral mucositis3 |
| Systemic acyclovir and analogues | Not recommended for prevention of chemotherapy-induced oral mucositis3 | |
| Chlorhexidine mouth rinse | Not recommended for prevention of radiation-induced oral mucositis or for treatment of chemotherapy-induced oral mucositis3 | |
| Topical coating agents | Topical sucralfate | Not recommended for prevention of radiation-induced oral mucositis3 |
| Laser therapy | Laser | Suggested when necessary technology/training is available in patients receiving high-dose chemotherapy or chemoradiotherapy before hematopoietic cell transplant5,55,71 |
FDA, Food and Drug Administration; RT, Radiation therapy.
* Multinational Association for Supportive Care in Cancer and the International Society of Oral Oncology.
Pain control
The combination of long-term indwelling venous catheters and computerized drug administration pumps to provide patient-controlled analgesia has significantly increased the ability to control severe mucositis pain while reducing the dose and side effects of opioid analgesics. The MASCC/ISOO guidelines recommend patient-controlled analgesia with morphine for patients undergoing HCT.3
Maintenance of oral hygiene
Multiple studies have shown that good oral hygiene plays an important role in the management of oral mucositis.8,10,47 The MASCC/ISOO guidelines recommend use of a standardized oral care protocol including brushing with a soft toothbrush, flossing, and use of nonmedicated rinses (e.g., saline or sodium bicarbonate rinses). Patients and caregivers should be educated regarding the importance of effective oral hygiene.53
Therapeutic interventions
Various agents have been studied to prevent oral mucositis or to reduce its severity, including cryotherapy, growth factors, anti-inflammatory agents, antibacterial agents, promoters of healing, and mucosal coating agents. Table 50-1 lists selected agents studied more recently for oral mucositis. The MASCC/ISOO recommendations are also provided for agents where a guideline exists.
Salivary gland dysfunction
Saliva has an important role in maintaining oral health. Although the effects of ionizing radiation on salivary gland tissue have been well documented, the corresponding effects of cancer chemotherapy have not. Overall, the studies on effects of various chemotherapeutic agents on salivary gland function have produced inconsistent results, with trials showing varied effects on flow rate, sialochemistry, and dry mouth complaints.34,41,60 No histopathologic investigations of major salivary glands have been reported, but a postmortem study showed minor salivary gland damage after the administration of various chemotherapeutic agents, with changes evident in the first 3 weeks after chemotherapy administration followed by gradual healing with minimal or no sequelae several weeks to months after therapy. Clinical observations support the contention that alterations in salivary function associated with cancer chemotherapy are generally reversible, in contrast to the alterations seen after salivary gland exposure to radiation therapy.
Attempts to manage salivary gland dysfunction can have beneficial effects on the quality of oral health of cancer patients. Frequent rinsing with normal saline can help keep mucosal surfaces moist, clear debris, and stimulate salivary gland function for short periods. Saliva replacements (mouth-wetting agents) may provide temporary symptomatic relief. Other strategies to stimulate salivary glands include the use of “taste stimulation” with sugar-free gum or candies and regimens that use cholinergic drugs. Bethanechol, cevimeline, and pilocarpine, which directly stimulate salivary glands, have been reported to be useful for treating xerostomia when functional salivary gland tissue remains.46 Increasing the ingestion of moist foods (e.g., flavored gelatins), sauces, and gravies can ameliorate the discomfort of eating. Dry or cracked lips should be kept lubricated with agents such as lanolin-based creams and nonperfumed, nonmedicated skin moisturizing agents. The use of antibiotic-containing topical agents on the lips may be indicated to prevent secondary infection, especially in immunosuppressed patients.
Neurotoxicity
Direct neurotoxicity from cancer chemotherapy has been noted with certain chemotherapeutic drugs (most commonly the microtubular agents vincristine and vinblastine, and taxol). This neurotoxicity may result in severe, deep-seated, throbbing mandibular or maxillary pain that can mimic dental pathology (i.e., toothache). Neurotoxicity is generally considered a dose-limiting complication for these drugs, and prompt diagnosis is important.52 Appropriate dental/periodontal examinations (including tooth vitality testing as necessary) must be performed to rule out pulpal or periodontal sources of pain. Opioid-containing analgesics may be useful in controlling pain, and the use of neurologically active medications may be considered. The neurotoxicity may be transient and generally subsides shortly after dose reduction or cessation of chemotherapy.
Taste dysfunction is a neurosensory problem that can be associated with cancer chemotherapy.12,22 Taste receptors are neuroepithelium-derived cells, with a turnover rate of approximately 10 days. They generally regenerate if not irreversibly damaged. In addition, the damage to olfactory receptor cells must be considered when a patient has taste dysfunction. Aberrations in taste perception can vary from hypergeusia to hypogeusia to dysgeusia. Some patients simultaneously report several different symptoms—hypergeusia with some tastes and dysgeusia with others. Patients receiving cancer chemotherapy occasionally report a bad taste that results from the diffusion of drug into the oral cavity, known as “venous taste phenomenon.”
Alterations in dental and skeletal growth and development
As the number of long-term survivors of childhood cancer has increased, the risk for damage to developing dental and skeletal structures from cancer therapies has become apparent. Chemotherapy-related damage to developing teeth includes hypoplastic dentin and enamel, shortened and conical roots, taurodontic-like teeth, microdontia, incomplete enamel formation, and complete agenesis of teeth.15,33,50,67 Eruption patterns may be altered, and changes in alveolar, mandibular, and maxillary bone growth and development can have orthodontic and cosmetic implications. The addition of radiation to treatment protocols (e.g., cranial irradiation for leukemia or total body irradiation for HCT) significantly increases the risk for damage to developing teeth.
Osteonecrosis of the jaws related to bisphosphonate therapy
In recent years, osteonecrosis of the jaws (ONJ) has emerged as a new oral complication in patients receiving bisphosphonate therapy. Although this complication has also been reported in patients receiving oral bisphosphonates for osteoporosis, cancer patients receiving intravenous bisphosphonates are at significantly higher risk.56 The complication manifests as exposed bone in the mandible or maxilla, often accompanied by infection, pain, and swelling (Figure 50-2). The risk for bisphosphonate-associated ONJ seems to be related to a combination of (1) the antiresorptive potency of the bisphosphonate administered, (2) the amount of the drug deposited in bone, and (3) the occurrence of situations requiring bone to heal or remodel. Most cases have been reported after dental extractions or dental surgeries, but bisphosphonate-associated ONJ can also occur spontaneously.

FIGURE 50-2 Osteonecrosis of the jaw related to bisphosphonate therapy.
(Courtesy Dr. Cesar Migliorati. From Migliorati CA, Siegel MA, Elting LS: Bisphosphonate-associated osteonecrosis: a long-term complication of bisphosphonate treatment, Lancet Oncol 7(6):508-514, 2006.)
Studies have shown that the risk for osteonecrosis increases with duration of bisphosphonate therapy and varies by the bisphosphonate agent used. One study reported that of 105 patients receiving intravenous zoledronic acid, risk for osteonecrosis was 1% after 12 months of use, 7% at 24 months, and 21% after 24 months. In the same study, of 127 patients receiving either intravenous pamidronate alone or intravenous pamidronate before or after intravenous zoledronic acid, risk for osteonecrosis was 0% up to 24 months, 2% at 36 months, and 7% at 48 months.2 Another study found that the frequency of ONJ in bone malignancy cases, treated with mainly intravenous zoledronate or pamidronate, was 1 in 87 to 114 (0.88% to 1.15%). If extractions were done, the calculated frequency of ONJ was 1 in 11 to 15 (6.67% to 9.1%). In this study, the frequency of ONJ in osteoporotic patients, mainly receiving weekly oral alendronate, was 1 in 2260 to 8470 (0.01% to 0.04%). If extractions were done, the calculated frequency was 1 in 296 to 1130 (0.09% to 0.34%). The median time from initiation of therapy to the onset of ONJ was 12 months for zoledronate, 24 months for pamidronate, and 24 months for alendronate.51
Effective treatment protocols have not yet been identified for ONJ. It is generally believed that stopping bisphosphonate administration may not promote healing because it is estimated that bisphosphonates may remain in bone for up to 10 years. Prevention is crucial. Patients should receive a dental evaluation before receiving intravenous bisphosphonates. Any dental disease requiring surgery or extractions should ideally be completed and allowed to initially heal before the start of bisphosphonate therapy.54
Indirect Oral Toxic Effects
Although direct toxic effects are generally the most visible oral complications of cancer chemotherapy, indirect oral effects can potentially be of more concern. The most important indirect toxicities are oral infections associated with myelosuppression and immunosuppression associated with damage to myelogenous stem cells and cellular elements of the immune system. Preexisting oral and dental infections can spread, with the oral cavity serving as the point of entry for organisms into deeper tissues and the systemic circulation.32,40 Other indirect toxic effects to the oral cavity are thrombocytopenia, anemia, and GI toxicity (i.e., nausea, vomiting, and alteration in absorption of nutrients).
Oral mucosal infections
Fungal infections
Factors affecting oral colonization and infection risk include alterations in competing oral bacterial flora (most commonly associated with the use of systemic antimicrobials), decreased salivary gland flow rates, and immunosuppression. The latter is especially related to neutropenia. Alteration in host oral bacterial flora in cancer patients with myelosuppression supports increased candidal colonization. With the development of new strategies to prevent and treat fungal infections, however, the fungal organisms associated with oral infections are changing. The widespread use of fluconazole prophylaxis has been associated with increasing numbers of Candida glabrata (Torulopsis glabrata) and Candida krusei infections that may have decreased sensitivity to fluconazole and other antifungal agents.84
More recent Cochrane reviews addressed the efficacy of various antifungal drugs in prevention and treatment of oral candidiasis in cancer patients.11,87 Nystatin, although commonly used, was found to be ineffective, possibly because it is not absorbed in the GI tract. Drugs partially absorbed from the GI tract, such as topical clotrimazole or miconazole, were found to be effective and can be useful for superficial oral infection. Persistent or locally invasive infection (including atrophic and erythematous candidiasis), especially when a risk exists for systemic spread, should be treated with appropriate systemic agents. Systemic azoles (e.g., fluconazole, itraconazole, ketoconazole) that are fully absorbed in the GI tract are very effective against the organisms and generally considered the most effective way to prevent or reduce fungal colonization and subsequent infection. These drugs are secreted in saliva; salivary concentrations of fluconazole are directly proportional to plasma concentrations.38 It has been suggested that systemic antifungals may be less effective for oral candidiasis in patients with decreased salivary production because of reduced oral delivery of the drug through saliva. In one study, salivary concentrations of fluconazole were not found to correlate to response to therapy,27 however; this area requires further research.
Viral infections
Herpes group viruses can cause significant oral disease in patients receiving cancer chemotherapy.70,72,73 HSV, VZV, CMV, and Epstein-Barr virus (EBV) are recognized causes of oral lesions in cancer patients. Most infections with HSV, VZV, and EBV represent reactivation of latent virus, whereas CMV infections can result from either reactivation of latent virus or newly acquired virus. Other viruses causing oral lesions in cancer chemotherapy and HCT patients are adenovirus, coxsackieviruses, and human herpesvirus. The diagnosis of viral lesions in the mouth can be made through direct immunofluorescent examination of scrapings from lesions, />
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses