The available intraoral donor sites are found primarily in the mandible and, in the maxilla (eg, maxillary tuberosity). However, only the mandibular sites commonly provide a sufficient volume of bone.
Two mandibular regions are most frequently used as donor sites: (1) the anterior region (mental symphysis) and (2) the posterior laterodistal region of the mandibular body and the ramus.
Chin graft
Anatomy of the chin region
In the chin, the harvesting zone is limited distally by the mental foramina, superiorly by the dental root apices, and inferiorly by the inferior border of the mandible. It is recommended that the central part of the chin not be harvested to avoid making a depression and altering its form. However, harvesting of the chin is possible provided that the inferior border of the mandible is left intact (Fig 5-1).
When harvesting in this region, the clinician must be careful to avoid the vasculonervous pedicles of the chin as well as the incisors and canines. This area is described as a loop located anterior to the foramina and must be identified on a preoperative computed tomography (CT) scan. The apices of the incisors and canines follow a topography median to the cortical plate. In spite of this position, the vasculonervous pedicles can be torn during deep corticocancellous bone grafting.
At the opening of the mental foramen, the nerve divides into three or four branches. One descends toward the chin; the others move toward the anterior vestibule and toward the mucus and cutaneous sides of the lips.
The size of the grafts in this site range from 45 to 50 mm (6 to 13 mm long by 6 to 9 mm wide). There is easy access to the site, and the harvesting is done under local anesthesia. The bone obtained is of excellent quality (ie, essentially cortical with a little cancellous bone).
A preoperative profile teleradiogram and CT scan are essential to know how much bone thickness is available and to correctly determine whether the graft is corticocancellous (Fig 5-2).
Surgical approach
The initial approach can be sulcular at the level of the incisor-canine group, thus leaving an invisible scar on the vestibular area. But when the flap is of a significant size, raising the flap to the basal border with releasing incisions may leave scars that can annoy the patient. In 2004, Tuslane and Andréani proposed that an inverted V-shaped incision be used on the labial mucosa. This incision is convenient and, according to these authors, allows the harvesting of fairly large grafts.
We recommend making an incision on the mucogingival line (Fig 5-3). This protects the anatomy, makes releasing incisions unnecessary, and allows easy access to the harvest site. Moreover, this incision protects the marginal periodontium, and careful suturing of this region does not leave a visible scar.
In all cases, the procedure is performed using a full-thickness flap (Fig 5-4). Preservation of the periostium contributes to the healing process, but it must be pushed aside so as not to obstruct the incision of the ultrasonic tip. After raising the flap and exposing the site, the clinician can control the desired surface and thickness of the graft, which must be previously verified on the preoperative CT scan.
Sectioning is most often done with a graduated straight saw tip (eg, BS1 [Satelec] or OT6 [Mectron]), which allows continuous control of the depth of the tip’s incision relative to the internal cortical plate (Fig 5-5). As a general rule, the incision lines must be placed 3 mm below the tooth apices and at least 5 mm from the basal border of the mandible (Fig 5-6). Laterally, a safe distance of 5 mm from the mental foramen is required. This is particularly important when the CT scan reveals an extension of the mental nerve’s anterior loop from the foramen.
Since a chin graft is situated on a one-dimensional plane, its elevation is more delicate than that of the ramus graft. Harvesting without difficulty is possible if the cortical graft lies on spongy tissue (Fig 5-7). Otherwise, it is essential to make one or two small lateral surface cuts on the graft to allow an osteotome to be placed cortically and to progressively dislodge the graft. In some cases, the graft can be removed with the aide of a surgical mallet (Fig 5-8). The harvested graft is often corticocancellous (Fig 5-9).
Protecting the internal cortical plate is vital to avoid hemorrhagic risk or hematoma of the buccal floor.
Compression and a resorbable collagen sponge or Surgicel (Johnson and Johnson) ensures hemostasis. The suture is carried out in a single plane if the incision has been done on the mucogingival line, which is another advantage of this choice of incision. Postoperative edema and hematoma formation can be minimized or even prevented by the simple application of compression and the immediate application of an ice pack. Nonetheless, the patient must be informed of the short-term risk of an unesthetic postoperative ecchymosis.
The intervention is technically made easy by the use of ultrasonic instruments; nevertheless, it involves risks that should not be underestimated.
1. Vascular: Particularly in case of rupture or harvesting of the internal cortical plate.
2. Nervous: Lesion of the incisive-canine pedicle is frequent and estimated to occur in 2% to 25% of cases according to the authors. The consequences may be hypo- or hyper-esthetics.
3. Osseous: Risk of fracture of the basal bony border if the graft is harvested too close to the border.
4. Esthetics: Asymetric contracture of chin muscles is mentioned in the literature. It rarely occurs if the incision has been made on the mucogingival line.
5. Dental: Devitalization of incisors or canines is possible if the apex is traumatized during harvesting. The risk is assessed in the literature to be from 3% to 10%. Secondary devitalization may also originate from periapical lesions.
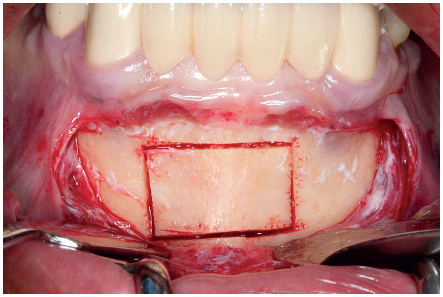
5-1 Cortical bone harvesting of the chin (clinical case courtesy of Dr A. Aalam).
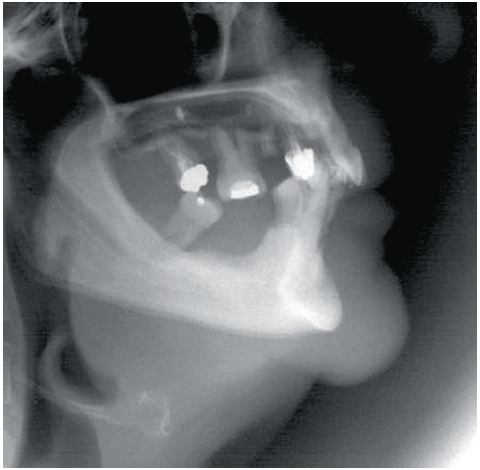
5-2 Profile teleradiogram showing the chin area.
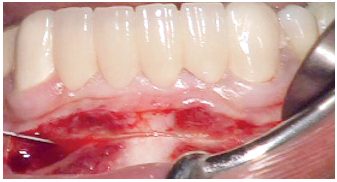
5-3 Incision on the mucogingival line.
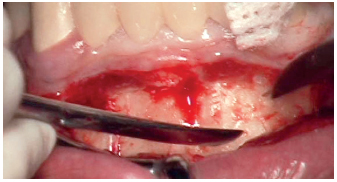
5-4 Full-thickness flap preparation exposing the bone to be harvested.
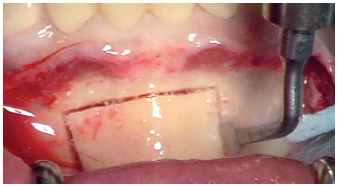
5-5 Exposed donor site.
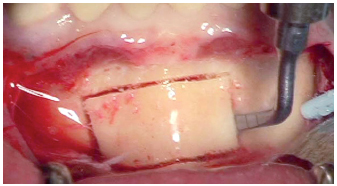
5-6 Control of the depth during harvesting using the BS1 tip (Satelec).
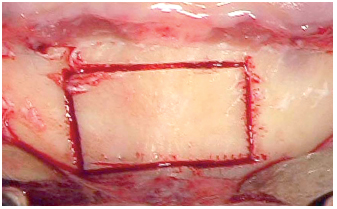
5-7 Anatomic zone of the chin graft.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


