1. INTRODUCTION
Before implant treatment, it is essential to diagnose and plan each case appropriately. Several tools can be used to make this critical phase of treatment more predictable.
Many clinicians extract teeth because implant rehabilitation will provide greater predictability for their treatment. However, dentists should aim to preserve teeth because it has been scientifically established that implants have survival rates similar to those of teeth1.
A detailed anamnesis, followed by clinical, laboratory, radiographic, and photographic examinations, is fundamental to define the best surgical and rehabilitation strategy. Specialties involved in treatment should perform their procedurescarefully. Biologic failure may compromise tooth viability and require the placement of an implant. The patient must be healthy and without any pathological condition that impairs the osseointegration process or must not take medications that interfere with bone metabolism2.
One of the factors that must be taken into account before performing implant rehabilitation is the patient’s bone age. To avoid severe discrepancies between teeth and implants due to maxillomandibular growth, implants should be placed after bone growth is completed3.
In young patients, children, or adolescents, the treatment protocol is to extract the tooth and maintain the prosthetic space to install the implant later on after the patient reaches bone maturity. In adult patients, this window is not necessary and it is possible to place the implant at different times after the extraction. Establishing an adequate diagnosis, surgical–prosthetic planning, and adequate implantation chronology are critical factors for the successful rehabilitation with implants.
OBJECTIVES
At the end of the chapter the reader should be able to:
-
Determine the reason for extraction and its repercussions on bone and soft tissue.
-
Determine the ideal three-dimensional position of the implant.
-
Select implants for surgical–prosthetic rehabilitation.
2. EVIDENCE-BASED LITERATURE
2.1. TOOTH IMPAIRMENT
Dental caries, advanced periodontal disease, root resorption, fractures, and recurrent endodontic lesions can lead to tooth loss4. A recommendation of extraction should consider the extent of the present pathology and if there is no possibility of maintaining the tooth in function with an appropriate esthetic (Figs 01A–L). Depending on the case, there may be more significant impairment of the remaining bone tissue and sometimes the installation of an implant in the bone socketmay be contraindicated. Clinical and radiographic examinations are usually necessary to establish this diagnosis5.












01. A–L Mandibular left central incisor with a facial gingival recession from an endoperiodontal lesion (A). Clinical and radiographic evaluation (B) shows that the tooth has slight extrusion, grade 1 mobility, and sufficient periodontal support in the interproximal and lingual region. Extraction is not recommended as long as the endoperiodontal lesion is resolved. After periodontal and endodontic treatment (C–H), a mixed flap was used to perform apicectomy and root coverage surgery with a connective tissue graft (I, J). Postoperative follow-up at 3 and 12 months after surgery was without periodontal pockets (K, L). Surgical procedure: Dr Fausto Frizzera; endodontic treatment: Dr Victor Valentim and Dr Igor Daroz under the guidance of Dr Jaílson Vitali in the FAESA Integrated Clinics course.
The integrity and thickness of support tissues are essential in surgical planning6. A tooth may have extensive caries with no significant gingival or bone impairment. In these cases when restoration is not feasible, placement of an implant is recommended. Similarly, teeth that need to be extracted due to root resorption share this same feature, unless it is associated with the periodontium. Endoperiodontal lesions have the potential to destroy support tissues in height and thickness and should be diagnosed and controlled before surgery.
Endodontic lesions are usually present near the root apex, with bone loss restricted to this region. The possibility of lesion resolution by endodontic treatment should be verified. Extraction should only be recommended if the endodontic treatment presents a poor prognosis (Figs 02A–K). The presence of bone defects makes it challenging to install the implant in the socket due to the higher risk of not obtaining apical anchorage of the implant since the lesion is often underestimated or not detected by conventional radiographic examinations7.











02. A–K Patient with a gummy smile and lesion in the periapical region of tooth 22 (A–D). Radiographically, we note how periapical radiography underestimated the size of the lesion. The indicated treatment (E–G) involved periodontal and endodontic surgical procedures. The right maxillary first molar clinical crown was enlarged to its left counterpart, except for tooth 22, which underwent curettage of the periapical lesion, apicectomy, retrograde obturation, and bone grafting. After 1 year of follow-up, it was possible to observe the repair of the periapical lesion of tooth 22 and an adequate periodontal support, where the minimum ratio between crown and root should be 1:1, without the presence of pockets or tooth mobility (H–K). Surgical procedure: Dr Fausto Frizzera; endodontic treatment: Dr João Batista Gagno Intra.
Concerns about placing implants in areas with periapical or periodontal lesions have resulted in several studies8–10; the current consensus recommends not to install implants in regions with acute processes. As long as the area is debrided during the surgical procedure before implant placement, chronic lesions do not impair osseointegration11.
Extensive loss of periodontal support can compromise the function and esthetics of a tooth and immediate implant placement (Figs 03A–G). In these cases, an adequate treatment plan to recover the lost tissues and obtain more favorable results is needed12. In patients with more significant tissue loss, it is often necessary to perform staged implant rehabilitation. If tissue gain is still limited, grafting procedures may be performed or a dentogingival restoration may be recommended13. In these patients, oral hygiene instructions, periodontal treatment before implant placement, and periodic follow-up are of great importance to prevent future peri-implant problems14,15.







03. A–G This patient complained about the maxillary anterior teeth, especially tooth 21 (A). Radiographically, there is an unfavorable crown/root ratio and extensive bone loss (B–D). Clinically tooth 21 presents with mobility and severe attachment loss (E–G). Even though there is sufficient apical bone, implant placement at this moment is contraindicated due to the present defect and the need for its resolution.
Root fractures and cracks are a significant dilemma in the diagnosis and clinical treatment. They can occur in the vertical, horizontal, or oblique direction and the recommendation for tooth extraction depends on its extension and direction. Horizontal and oblique fractures in the cervical third can be treated by orthodontic or periodontal procedures, or by a combination of both. However, if there is a vertical or oblique fracture extending to the middle or apical third, tooth extraction should be considered16.
Vertical fractures and cracks are difficult to diagnose and may not be noticed for months or years. Their presence implies the need for extraction since no treatment is effective for vertical fractures17,18. Maintaining the tooth will cause an infectious process. Additionally, the micromovement of fragments further stimulates the inflammatory response and bone resorption, which may cause extensive bone defects and make future implant placement difficult or unfeasible. Early diagnosis is essential for preserving bone tissue and avoiding bone grafts and higher morbidity for the patient19. Currently, no noninvasive diagnostic method can confirm the presence of a vertical root discontinuity, so a number of clinical and radiographic findings are taken into consideration to establish this diagnosis. Clinical, radiographic, and periodontal evaluation, as well as transillumination, fistula tracking, pulp vitality testing, and mobility are used to diagnose vertical root fractures18. The presence of a periodontal pocket in an isolated surface of a tooth is a common sign of a root fracture. Radiographic signs of fracture may include increased periodontal ligament, periapical radiolucency, bone loss, and separation of root fragments20.
Even after these evaluations, doubt may persist; in these situations, exploratory surgery may be performed to verify the actual presence of a crack or fracture, or cone beam computed tomography (CBCT) can be requested. If the diagnosis is confirmed, the tooth should be extracted. Depending on the amount of bone, it is possible to place an implant and grafts during the same procedure (Figs 04A–G).







04. A–G Presence of extensive bone defect in the buccal surface of tooth 11 (A). In addition, the tooth had an unfavorable crown/root ratio and a broad intraradicular post (B). Clinical evaluation showed the presence of a deep and isolated pocket only in the facial surface of tooth 11, with presence of suppuration (C). The diagnosis of root cracks on the facial surface was established and the tooth was removed (D–G).
2.2. IMPLANT PLACEMENT TIMELINE
The timing of implant placement after extraction was established by consensus21; different types were classified according to the timing of implant placement (Figs 05A–D).




05. A–D Different implant placement types defined based on tooth extraction. Type I: implant placed in fresh socket (A); type II: early implant placement, after complete soft tissue healing, between 4 and 8 weeks after extraction (B); type III: immediate implant placement, after considerable bone healing assessed by radiographs, between 12 and 16 weeks after extraction (C); type IV: late implant placement, installed in healed ridges, 16 or more weeks after extraction (D).
If the treatment aims to rehabilitate the patient immediately after extraction, care should be taken. Any problems in diagnosing or planning can lead to future complications. The individualized rehabilitation planning begins after initial assessments of the patient and their systemic and local conditions are performed.
Surgical installation of an implant aims to rehabilitate one or more teeth. Taking into account the current rehabilitative philosophy where reverse planning is performed before surgical procedures, a number of factors (Figs 06A–D) regarding the tooth and site to be implanted and their maxillomandibular relationship should also be considered14.
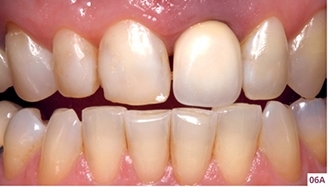



06. A–D Fracture of tooth 21 due to occlusion trauma in protrusion; a balanced occlusion should be established to allow adequate rehabilitation with an implant (A). Before implant placement, orthodontic, surgical, or combined treatment may be required to balance the occlusion (B), convergence of the roots of the teeth adjacent to the edentulous area (C), and inadequate prosthetic or interocclusal space (D).
Orthodontic and oral rehabilitation should be employed to verify the need to reestablish the patient’s vertical dimension, anterior guide, and lateral and protrusion movements. Stable occlusion is critical to successful rehabilitation and is of paramount importance in situations where an immediate provisional is placed without occlusal contacts22,23. If the patient has loss of posterior occlusal support or parafunctional habits, the provisional and implant may receive excessive loads and the success of the treatmentis compromised24,25.
2.3. BONE EVALUATION
Implant placement in the ideal three-dimensional(3D) position will depend on bone availability. Therefore, it is essential to request a CBCT scan before surgery. This radiographic method allows the visualization of the existing bone and gingival contour (if a soft tissue retractor is used during the computed tomography scan) and whether immediate implant placement is possible, reducing the patient’s total treatment time. The CBCT also allows us to verify the need for bone regeneration before implant placement (Figs 07A–H).








07. A–H Assessment of bone and gingival condition in the soft tissue using CBCT: socket with sufficient apical bone for immediate implant placement (A); socket with limited apical bone that does not allow immediate implant placement (B); healed socket with enough bone for implant installation (C); healed socket with limited thickness with need for bone regeneration, which may or may not be combined with implant placement (D); healed socket with limited height and thickness with the need for bone regeneration before implant placement (E). It is possible to detect bone defects with three (F), two (G), or only one (H) remaining wall.
The CBCT scan is essential for diagnosis and individualized treatment planning with dental implants5. Individual treatment planning of each patient increases the predictability of treatment. For excellent outcomes, such as those required by patients, errors from inaccurate diagnosis or treatment planning must be avoided26. Besides being an essential tool for diagnosis, the CBCT scan allows us to accurately assess bone height and thickness and their relationship with anatomical structures. It also allows virtual planning for guided surgeries27. It is possible to classify the dentulous or edentulous ridge into six types (Figs 08A–L and 09A–F) according to Benic and Hämmerle28.






08. A–L Classification of bone defects according to Benic and Hämmerle28.






09. A–F Clinical images of the six classes of bone defects according to Benic and Hämmerle28.
0 Slight loss of bone tissue
1 Intact socket
2 Narrow buccal defect
3 Wide buccal defect
4 Defect in thickness
5 Defect in height and thickness
When indicated, CBCT should be used in a way that favors patients and facilitates surgical procedures. In many situations the clinician may have questions about the thicknessof the bone ridge or the prognosis of a tooth with a radiolucent apical lesion.
Evaluation by panoramic or periapical radiographs is indicated to evaluate teeth, periodontal condition, bone ridge, and their relationship with anatomical structures in a general context (Fig 10).

10. Panoramic radiographs allow to assess the patient’s general oral condition and evaluate the distance from the ridge to anatomical structures such as the maxillary sinus (1), nasal fossa (2), incisive foramen (3), mandibular canal (4), mental foramen (5), and basilar process (6). It is still possible to verify the relationship between the edentulous area and the roots of the adjacent teeth and plan the rehabilitation.
The patient must have periodontal and dental health before implant placement (Figs 11A–C to 13A–C). Conventional radiographs are good tools for initial planning but are limited due to overlapping images and may not allow true visualization of the extent of the defect present at or around the tooth. CBCT allows the verification of the dimensions of the defect and the density and topography of the existing bone. Therefore, the ideal position of the implant placed immediately after tooth removal can be determined. Such a concern exists because the position the implant is placedinto influences the amount of soft tissue around it.



11. A–C Patient with periodontal and dental health, except for tooth 24. The patient complained of the esthetics. Deep periodontal pockets, mobility, and painful sensitivityare present.










12. A–J Radiographic examination demonstrates the presence of a bone defect around the root of tooth 24 (A). Tomographic evaluation of the defect demonstrates extensive buccal bone loss with sufficient apical bone for immediate implant placement (B–J).



13. A–C This patient had high esthetic demands and reported dissatisfaction with gingival staining in the buccal region of tooth 24. Radiographic and photographic protocol done by Odontopixel.
2.4. SOFT TISSUE EVALUATION
Due to the different clinical and histological characteristics of gingival tissue, the soft tissue surrounding the implant is called the peri-implant mucosa. In esthetic areas, it is essential that visually this tissue is similar to the adjacent mucosa. If there is adequate keratinized mucosa around the implant, it should be pink and firm (Figs 14A–E); otherwise, it may appear red and loose29.





14. A–E The tooth was extracted and an implant placed in the ideal 3D position (A). Due to the adequate primary stability, an immediate provisional was made. The socket was regenerated and a connective tissue graft (B) was added to increase the soft tissue volume and prevent exposure of the peri-implant margin. Clinical and radiographic follow-up at 6, 12, and 36 months after surgery (C–E). Surgical procedure: Dr Fausto Frizzera; restorative procedure: Dr Marco Masioli; laboratory technician: Igor Hand.
Like the periodontium, the peri-implant tissue will also have a sulcus (Fig 15).

15. Schematic illustration of the difference between dental and peri-implant tissues.
The depth of the sulcus will vary depending on several factors such as implant position, prosthetic component, region, and bone anatomy. The presence of peri-implant pathology should be diagnosed by the presence of recession or bleeding on probing (Figs 16A–C)30.



16. A–C Presence of recession around the implant, with exposure of the implant surface, limited amount of attached gingiva, presence of biofilm, and peri-implant bleeding, which may result in peri-implantitis.
Histologically, peri-implant tissue is similar to gingival tissue. An epithelial tissue adhesion with hemidesmosomes to the prosthetic component is present, similar to teeth31. In contrast, the peri-implant mucosa has reduced blood supply and collagen fibers do not adhere directly to the implant, as occurs on the root surface of teeth. Most of them are parallel to the implant, forming a collar around the implant, providing tonicity and consistency to the mucosa32.
The orientation of collagen fibers is also related to the quality of the periimplant mucosa33. It is also possible to find fibers oriented in different directions, especially in thicker tissues with more keratinized mucosa (Figs 17A–F).






17. A–F Clinical differences between thin (A–C)
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses



