OF INTACT AND
COMPROMISED SOCKETS:
Fausto Frizzera, Jamil A. Shibli, Ana Carolina M. Marcantonio, and Elcio Marcantonio Jr

1. INTRODUCTION
About 12 million implants are placed annually worldwide1 according to the implant placement chronology that follows tooth extraction as proposed by Hammerle et al2 at the Gstaad conference in Switzerland (Fig 01). The different chronologies of implant placement vary mainly regarding time and surgical morbidity. Satisfactory biologic and clinical results, associated with safety and long-term stability, have always been the objective of scientific research carried out in implantology. Although these are primary treatment factors, patient satisfaction and the number of surgeries are underassessed.

01. Among the types of implant placement, the one that requires the most training is type I; its biggest advantage is reduced treatment time, morbidity, and number of procedures.
Results have centered on patients’ expectations; total treatment time, cost, number of surgical procedures, safety, and clinical outcomes should all be taken into account. From the patient’s point of view, treatment should be done as quickly as possible least painfully, and least costly, providing an excellent outcome.
The major concern regarding the technique for implants and immediate provisionals (IIP) is the position the gingival margin (GM) will assume after surgery and in the long term. Different clinical situations may require maintaining or modifying this process. In the past, a gingival recession (GR) of approximately 1 mm in the first year was expected3; to reduce the chance of recession, soft and bone tissue regeneration4 (Table 01) is recommended. The initial step to maintaining or modifying the position of the GM is correct three-dimensional (3D) placement of the implant in the socket. If the implant cannot be placed in the ideal position, delayed implant placement is recommended.

Table 01 Studies on immediate implant placement according to different protocols. Bone and gingival grafts, flapless surgery, and immediate implant-supported provisional restoration increase the risk of GR around the implant. The use of these techniques for immediate implant placement allows the reduction or even prevention of recessions (adapted from Chen and Buser5)
Gingival biotype and the type of bone defect are predictive factors of possible alterations that may occur after extraction and will be addressed in this chapter. A protocol to increase esthetic predictability in the treatment of intact and compromised sockets will be presented.
OBJECTIVES
At the end of the chapter the reader should be able to:
-
Understand the treatment of intact and compromised sockets.
-
Learn the methods to avoid esthetic complications after surgery.
-
Comprehend the proposed surgical protocol.
2. SCIENTIFIC BACKGROUND
2.1. GINGIVAL BIOTYPE
Gingival biotype is characterized by the quantity and quality of periodontal and peri-implant tissue, which is initially described as thin or thick6. The ideal method for classifying the gingival biotype has not yet been developed. It is possible to use the visual and translucency methods, direct gingival perforation with ultrasonic devices, or cone beam computed tomography (CBCT) with lip retractor7.
A gingival thickness of 1 mm or less around the teeth is classified as a thin biotype. A thick biotype presents a thickness of 1 mm or more. Around implants, soft tissue thickness greater than 2 mm is classified as thick; it is considered thin if it is equal to or less than 2 mm8,9. Assessing the thickness of tissue around the teeth is complex. In implants, thickness can be measured with a caliper after removal of a screwed in crown.
Measurement of soft tissue thickness can be performed 2 mm apically to the GM through tissue perforation. This is an invasive procedure that requires anesthesia. The compression caused by the probe or needle may affect measurement accuracy10. The use of an ultrasonic device is a noninvasive method; however, its use to verify soft tissue thicknessis limited because its accuracy in detecting the low thickness of gingival tissue is low7. The assessment of tissue thickness by CBCT with soft tissue retraction is a noninvasive and accurate method but it is costly and emits ionizing radiation. It is indicated when CBCT is already required for treatment planning when placing an implant or evaluating a graft.
The simplest but no longer accurate clinical diagnosis of biotype is done by inserting a probe into the gingival sulcus. In a thick biotype, the instrumentwill not show through the soft tissue; on the other hand, in a thin biotype it will11. The visual method is not reliable to determine biotype because it tends to overestimate tissue thickness8,12.
The occurrence and magnitude of changes in periodontal/peri-implant tissue will depend mainly on the patient’s gingival biotype (Figs 02A–D and 03A–F). Clinically, tissue trauma and a defective buccal bone wall may lead to esthetic complications, such as recession of the soft tissue margin or a volume defect on the ridge13.




02. A–D Clinical aspects of thin biotypes, with longer triangular or rectangular (A, B) crowns. Thick biotype with shorter, usually quadrangularped clinical crowns (C, D).






03. A–F Tissue characteristics of thick (A–C) and thin (D–F) biotype.
2.1.1. THIN GINGIVAL BIOTYPE
Patients with a thin biotype have an extremely delicate gingival tissue, with a scalloped architecture of soft tissue and bone. Gingival tissue and bone are thin. Bone fenestration or dehiscence may be present14 (Figs 04A–F). The tissue has lower resistance to injuries and is often associated with GR15. In patients with a thin biotype, greater care is required when planning and performing surgical procedures to avoid esthetic and biologic complications16–18.






04. A–F Characteristics of the buccal bone wall: intact (A, D), fenestration (B, E), and dehiscence (C, F).
GM recession after IIP is more frequent in patients with a thin periodontal biotype compared to those with a thick biotype19. Although the difference is a few millimeters, be aware that discrepancies in the position of the GM in the anterior region cause esthetic complaints. Surgery usually does not recover all lost tissue20. Another factor that should be taken into consideration is that these values represent the change that occurs in the early years after implant placement. Gingival tissue recession tends to increase over time, especially in individuals with a thin biotype15,21 (Figs 05A–H and 06A–F).








05. A–H Immediate implant and provisional rehabilitation (without bone or gingival graft) performed on tooth 22 after 18 years (A–C). After osseointegration, a zirconia abutment and a ceramic crown were placed (D, E). Four years after treatment, the patient returned and complained of peri-implant margin recession with exposure of the zirconia abutment and presence of thin tissue (F–H).






06. A–F A connective tissue graft was used to treat these changes. Surgical procedure: Dr Elcio Marcantonio Jr; restorative procedure: Dr Rogério Margonar.
To avoid extensive changes in soft tissue architecture when planning for IIP in patients who have thin, modifying tissue thickness, a soft tissue graft is recommended. Studies show that modification on the biotype around implants with subepithelial connective tissue grafts demonstrated greater long-term stability in GM levels and better esthetic results19,22. Additionally, it is possible to create a more favorable ridge contour, using the soft tissue graft to compensate for the buccal bone loss that occurs after extraction even after performing guided bone regeneration23 (Figs 07A–J to 09A–I).










07. A–J Connective tissue graft to be placed on the buccal region of the socket (A–C). The area was prepared (D–F) to receive the graft that was stabilized by sutures (G–J).

08. Sequence for connective tissue graft suturing.









09. A–I Tooth 21 with vertical fracture and absence of buccal bone wall (A, B). The tooth was carefully extracted and the socket was prepared to receive a tapered implant stabilized in the lingual bone wall. A temporary and a slightly exposed subepithelial connective tissue graft was done (C–G). Note the gain in height requiring conditioning of the tissue to the level of the gingival margin with the homologous tooth (H, I). Surgical procedure: Dr Elcio Marcantonio Jr; restorative procedure: Dr Rogério Margonar.
2.1.2. THICK GINGIVAL BIOTYPE
Patients with a thick gingival biotype present a flat soft tissue and bone architecture. The buccal bone wall and gingiva are thick, presenting greater resistance to mechanical, pathological, and surgical injuries14. Faced with aggressive inflammation, the tissue tends to form a periodontal pocket rather than a GR. Surgical procedures performed in thick biotypes are favored due to greater vascularization, easier closure of the flap by first intention, and protection of the area7.
A thick gingival biotype around an implant ensures greater stability of long-term results. In IIP situations, it is important that there is abundant tissue in the region, both in height and thickness, because this may prevent future surgical procedures. Excess tissue in height can be eliminated by simple tissue conditioning with provisional restoration or by gingivoplasty.
Studies evaluating IIP in intact sockets where the buccal gap was filled with bone graft material and had a thick gingival biotype showed stability of the GM in the first years of evaluation. Remodeling the buccal bone wall is a concern because of the volumetric changes of the ridge. In such situations, it is possible to perform a connective tissue graft to increase the volume of this region24. In teeth that have a buccal bone defect and a thick biotype, a connective tissue graft at the moment of implant placement is recommended. The defect will affect bone remodeling and a greater GR; a decrease in buccal volume can be expected.
2.2. CLINICAL ASPECT OF THE SOCKET
The socket condition will determine the recommended treatment as well as possible tissue changes that may occur. The socket itself can be considered a defect surrounded by bone walls. Its self-limiting healing causes 3D tissue loss. The use of biomaterials may reduce this volumetric contraction but the presence of bone defects may lead to a worse prognosis regarding preservation of tissue architecture.
Different surgical approaches can be traced to obtain an adequate contour of the bone and gingival tissue. The type of bone defect present should be evaluated for immediate implant placement and to avoid complications during the healing period. A loss of one of the alveolar walls may change the pattern of bone formation after extraction, reducing its 3D volume and increasing the risk of GR and loss of papillae25. The absence of buccal bone does not prevent immediate implant placement. It is possible to achieve primary stability and osseointegration because it will be anchored in the lingual wall. However, it is important to evaluate the bone defect after extraction and perform the necessary interventions to ensure appropriate esthetic and functional results for the patient.
2.2.1. INTACT SOCKET
An intact socket presents the most favorable situation for immediate implant. If there is sufficient remaining bone structure to place the implant in the ideal 3D position, the IIP technique can provide excellent results. Currently, minimally invasive procedures are frequently used. A flapless IIP favors healing, treatment time, the number of surgeries, and morbidity without compromising the final result11,26–28.
A thick biotype favors the long-term maintenance of the ideal position of the GM. A thin biotype should be grafted to modify it into a thick biotype. Buccal bone thickness in the anterior region of the maxilla is usually a concern because the buccal bone wall tends to be thin. Horizontal reduction of the alveolar ridge is expected after extraction, which may require a gingival graft24.
Volume loss occurs mainly in the coronal third of the buccal bone crest after IIP in intact sockets29. In addition to the expected post-extraction bone remodeling, a saucer effect also occurs around the implant. An immediately placed implant does not prevent alveolar remodeling30, even if a bone graft and membrane are used31.
The GM tends not to migrate apically in the presence of a thick biotype because even when losing part of its volume, the height of the buccal bone crest is maintained. A study by Kois32 demonstrated that the soft tissue margin tends to be stable when the distance from the buccal bone crest to the GM is less than or equal to 3 mm. Buccal bone reconstruction is possible as long as the implant is properly positioned in the socket, taking into account the bone loss that occurs after extraction. A sufficient gap between the implant and the buccal bone wall needs to be respected and filled with a slow resorption biomaterial5. Presence of the buccal bone wall at the time of implant placement favors graft placement and incorporation.
Initial studies on IIP demonstrated no concern about implant diameter and placement, features of the provisional implant, use of grafts, or delicate flapless surgery5. Long-term follow-up showed GR and its recommendations were limited to patients without risk factors (nonsmokers, with a buccal bone thickness greater than 1 mm and thick biotype) only in the premolar region33.
Due to limited scientific evidence, the consensus recommendations33 were not to perform immediate implants in esthetic areas due to the high risk of GM recession. The recommendation was to perform alveolar ridge preservation and implant placement after 4–8 weeks34,35. However, with the evolution and application of the technique, studies with appropriate surgical techniques22,36,37 have demonstrated that in intact sockets it is possible to maintain the GM. The technique consists of IIP combined with bone graft to fill the gap and modification of soft tissue biotype (Figs 10A–E to 12A–G).





10. A–E In patients with intact sockets and a thin biotype, there is a need to modify the gingival biotype to thick when performing immediate implants. A careful detachment is performed on the cervical third of the socket to place the gingival graft into the buccal surface.
 PLACEMENT OF AN IMMEDIATE MORSE TAPER IMPLANT COMBINED WITH CONNECTIVE TISSUE GRAFT AND CERABONE
PLACEMENT OF AN IMMEDIATE MORSE TAPER IMPLANT COMBINED WITH CONNECTIVE TISSUE GRAFT AND CERABONE










11. A–J Patient with provisionals and impaired tooth 11 (A–C). The tooth had a long post and deep subgingival caries in the interproximal surface; after post removal, the presence of a buccal and lingual fracture was detected. Minimally traumatic extraction was performed. The socket was intact (D, E). The region was cleaned and prepared to receive a 3.5 × 13 mm tapered implant with Morse taper connection (F, G). The gap was grafted with inorganic bovine bone and the buccal surface received a connective tissue graft (H–J).







12. A–G Appearance immediately after gingival graft suture and provisional installation (A–C). Postoperative situation at 14 (D) and 180 days (E–G). Surgical procedure: Dr Fausto Frizzera; restorative procedure: Dr Marco Masioli.
Recent clinical and preclinical studies38,39 have suggested that the socket shield technique, which intentionally maintains the root fragment in the buccal portion of the socket, combined with immediate implant placement may favor volume maintenance in the esthetic region. These findings are based on the fact that bone tissue is maintained by the periodontium and its vascularization, avoiding the bone and tissue collapse normally observed after tooth removal. This procedure requires high technical dexterity; maintaining a buccal root fragment in position is not always easy.
The technique advocates root removal with the aid of rotatory instruments and periotomes, as well as removal of any soft tissue present in the periapical portion or soft tissue lesions adjacent to the fragment to be maintained (Figs 13A–K to 15A, B). It is important that the implant is positioned at the same level as the dental fragment; if necessary, a bone graft should be used to fill the gap. It is also necessary to avoid this technique in regions with higher occlusal demand.











13. A–K Tooth 21 with subgingival fracture associated with a short root. The socket shield technique, with immediate placement of a 4.3 × 13 mm implant and immediate placement of the provisional, maintaining the buccal root fragment (A–D). Two months after the procedure it was possible to verify a satisfactory contour of the buccal tissues (E–H), which was maintained after 3 years of follow-up (I–K). Surgical procedure: Dr Jamil Shibli; restorative procedure: Dr Susana D’Avila.


14. A, B In the socket shield technique, the compromised tooth is extracted and the root fragment in contact with the vestibular bone is maintained.


15. A, B The implant and provisional are placed and the fragment assists in the nutrition and maintenance of the buccal bone wall.
2.2.2. COMPROMISED SOCKET
The literature does not agree on the best treatment option for defective sockets. Most studies assume that IIP after extraction should be restricted to intact sockets27. However, from a clinical perspective, most teeth that should be extracted in the anterior region have a thin buccal wall40.
The involvement of one of the socket walls makes it difficult to maintain the tissue architecture after extraction. It is essential to identify the type of defect present before performing any surgical procedure and alert the patient to possible tissue changes that may occur. Implant placement in regions with a bone defect should only be performed if the defect is treatable; otherwise a delayed approach is recommended. The morphology of the bone defect in the free surfaces (buccolingual) is classified according to its 3D characteristics (Figs 16A–F and 17A–D).






16. A–F Types of socket defects: shallow and deep V (A, B), shallow and deep U (C, D), and shallow and deep wide U (E, F).




17. A–D Buccal bone neoformation after guided bone regeneration depends on the defect and bone envelope characteristics. This can be difficult if the bone envelope is narrow (A, B) or facilitated if it is wide (C, D). The buccal portion of the implant should be positioned 3–4 mm from the inner portion of the buccogingival tissues.
According to the vertical extent of the defect, the defect may be classified as shallow, when less than half of the wall has been damaged cervically/apically, or deep if more than half of the alveolar wall is compromised. Guided bone regeneration of shallow defects is more predictable41–43 but horizontal and vertical enlargement of bone and gingival tissue is possible in both situations.
Defects in width prompt more postoperative tissue changes than defects in height. The mesiodistal morphology of the defect can be classified19 as: V-shaped, where there is a narrow defect with a pointed apex and closed angle; U-shaped, wider defect with a rounded apex and open angle; wide U-shaped, defect with greater amplitude and width and rounder angle with extension of loss to the adjacent tooth. In the latter, immediate implant placement should be avoided. For V-shaped or U-shaped defects, an immediate implant may be placed after extraction provided that guided bone regeneration is performed and the implant is positioned within the bone envelope44.
The horizontal extent of the defect in the buccolingual direction is a predictor of new bone formation on the buccal surface of the implant. The size of the bone envelope should be measured by creating a line that joins the proximal bone ridges; from this line, the distance to the end of the palatine bone is measured. The bony envelope may be classified as narrow if it is less than 7.5 mm or wide if greater than 7.5 mm45. The higher this value, the greater the possibility of placing the implant within the bone envelope to maintain a distance of 3–4 mm from the implant platform and the inside of the buccogingival tissue. To aid buccal bone formation, a smaller diameter implant can be selected and installed 4–5 mm from the buccal GM, which allows a larger gap to be filled with biomaterials.
New studies have demonstrated the possibility of reconstructing the buccal bone after immediate implant placement in defective sockets and limiting soft tissue apical migration40,46–49. After placing 18 Nobel Perfect Groovy implants, sockets with complete buccal bone loss were grafted with autogenous bone particles removed from the mandibular ramus region. Complete reconstruction of the buccal bone was demonstrated even without using membranes47. In a later study40, IIP was combined with autogenous bone grafting but performed in intact sockets or with buccal bone defects; it was possible to obtain satisfactory esthetic results and a bone wall in the buccal region of 1 mm when measured 1 mm below the implant platform. In these two studies, a buccal volume discrepancy was also reported in the region receiving the implant and bone graft; these defects presented as a depression in the ridge contour after extraction.
Sockets with buccal bone defects were treated with a modified IIP approach by using a block-shaped bone graft removed from the tuberosity and adapted in the socket (Figs 18A–J to 20A–F). Rosa et al48 demonstrated how to reconstruct the buccal bone without using membranes and maintaining the position of the GM. The proposed technique was called immediate dentoalveolar restoration, showing stability of long-term results after 58 months in 18 patients.










18. A–J Patient with fractured tooth 21; minimal traumatic extraction was performed and an implant was placed with torque allowing the placement of an immediate provisional restoration.














19. A–N To reconstruct the defective buccal wall, a block bone graft (A–D) was collected. The graft was placed in the buccal region and the spaces filled with autogenous bone and inorganic bovine bone (E–H). The provisional was made on the same day and installed over the implant without occlusal contacts (I). Postoperativeimages at 7 and 30 days (J, K). Radiographic (L) and initial clinical appearance and after 180 days (M–N). Surgical procedure: Dr Elcio Marcantonio Jr; restorative procedure: Dr Rogério Margonar.






20. A–F In the immediate dentoalveolar restoration technique, the compromised tooth is extracted and the implant placed in the ideal position. Then bone particles removed from the tuberosity are inserted into the socket and the remaining space. A provisional is placed without occlusal contacts; after a period of osseointegration and graft incorporation, final case resolutionis reached.
Sarnachiaro et al49 performed a study to verify the increase in bone thickness after treating maxillary sockets with buccal bone defects with an immediate implant combined with a resorbable membrane, particulate autogenous bone graft, and a custom healing abutment. Ten cases were treated in this study; five implants were placed in the premolar, three in the canine, and two in the incisor region. A CBCT immediately after surgery and after graft incorporation, between 6 and 9 months, demonstrated the reconstruction of the buccal bone wall with an average thickness of 3.7 mm and 3 mm, respectively, in its coronal portion.
Kan et al25 presented a similar proportion of cases where there was recession of the GM greater than 1.5 mm regardless of whether surgery was performed with or without a flap; the recession was associated with the type and width of the bone defect. The worst results were found in patients with wide U-type defects. In addition, flap elevation in regions with a bone defect may further impair alveolar involvement. An improperly designed and sutured flap may increase the risk of gingival and papillary recession in the implant region and adjacent teeth.
These studies showed favorable results in relation to bone tissue but they do not clarify why they did not use gingival grafts and what might occur in peri-implant soft tissue in long-term follow-up (Figs 21A–F to 25A–L). Research performed on intact sockets has shown that minimizing or avoiding recession of the peri-implant margin when a connective tissue graft is used together with with IIP24,50–52 is possible; it is also possible to move the tissue margin coronally, leaving soft tissue slightly exposed, and use a provisional with a concave subgingival profile36,53. The space created by the subcontouring of the provisional prosthesis allows the thickness of the buccal soft tissue to be increased, making it less prone to buccal recession, as demonstrated after short-term and long-term follow-up37,46,52,54.
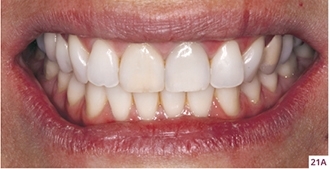





21. A–F Initial clinical presentation of the patient showing a periodontal pocket on the distal surface of tooth 21 due to cementum/dentin resorption. This was in addition to a periapical fistula and gingival harmony with a maximum Pink Esthetic Score score of 14.
















22. A–P Computed tomography images showing buccal bone fenestration, apical lesion, and internal resorption (A–F). After years of monitoring by an endodontist and no definitive resolution of the apical problem and presence of a periodontal pocket, the patient decided to replace her tooth with an implant. The treatment plan was explained to the patient, together with the rehabilitation options. Tooth 21 was carefully extracted with forceps to maintain the integrity of the crown (G–J). Alveolar dehiscence and the presence of a gingival thickness of 1.3 mmwere clinically confirmed. The socket was instrumented on its palatal wall and a 3.5 × 13 mm implant was installed with a torque of 50 N/cm2 (K–M). The Ostell device confirmed the high primary stability for the immediate installation of a provisional (N, O). According to the ridge anatomy, a cemented prosthesis was planned. The extracted tooth was reshaped with resin and used as the provisional over the prepared prosthetic component (P).















23. A–O Inspection of the socket confirmed distal bone loss and the implant’s ideal positioning (A–D). A collagen membrane (Geistlich Bio-Gide) (E–G) was placed under the alveolar defect, and a bone graft (Geistlich Bio-Oss Collagen) (H, I) filled the socket to the level of the gingival margin. The prosthetic component was installed with a torque of 20 N/cm2. The provisional crown was cemented and fine occlusal adjustments (J–L) were performed. Postoperative aspect at 7 (M, N) and 30 (O) days; healing was extremely favorable.
















24. A–P At the time of manufacturing the definitive prosthesis, a slight color change of the tissue was noticed due to the metallic abutment. It was suggested to the patient to use connective tissue grafting to increase the tissue volume or to use a zirconia abutment (A–D). The patient chose the less-invasive option, and a lithium disilicate veneer (tooth 11) and crown (tooth 21) were fabricated and cemented; note the improvement in tissue staining (E–P).












25. A–L Tomographic examinations at 6 and 12 months showed total reconstruction of the buccal bone (A–C). At the 3-year (D–I) and 4.5 year (J–L) follow-up, tissue staining was maintained. Still, a small discrepancy between the gingival margin of the two maxillary central incisors and a loss of volume in the buccal region of the implantwere observed, which reduced the Pink Esthetic Score score to 12. Although the patient had no complaints regarding this alteration, it was attributed to the nonuse of a gingival graft to compensate for the ridge’s physiologic remodeling. Surgical procedure: Dr Fausto Frizzera; restorative treatment: Dr Laerte Mattos.
In a randomized controlled trial45, the IIP technique was performed on maxillary incisors with buccal bone defect to evaluate peri-implant changes 1 year after surgery. After extraction, a narrow implant was placed. Patients were randomly divided into three groups: control, no soft tissue graft; MUCO, 3D collagen matrix (Geistlich Mucograft); and CONJ, subepithelial connective tissue graft removed from the palate. All sockets were reconstructed with bone graft (Geistlich Bio-Oss Collagen) and resorbable membrane (Geistlich Bio-Gide); a provisional with undercontoured cervical and absence of occlusal contacts was installed over the implants. Migration of the GM was 0.72 mm (± 0.57), 0.42 mm (± 0.60), and –0.04 mm (± 0.3), respectively in the control, MUCO, and CONJ groups. Results showed that recession was significantly lower in the CONJ group compared to the control group. In addition to limiting the migration of the GM, the connective tissue graft promoted better ridge contour and greater soft tissue thickness in the buccal region of the implant (Figs 26–28).



26. A–C This patient had subgingival fracture in tooth 24 at the middle third of the root, with fistula and buccal bone loss.















27. A–O The tooth was extracted with the aid of a periotome and the socket was cleaned and prepared to receive a 3.5 × 13 mm tapered implant (Flash, Prosthetic Systems Connection).




















28. A–T The implant was placed with a primary stability of approximately 50 N/cm2; a titanium UCLA abutment was manually installed and marked 2 mm apically at the occlusal level of tooth 25 (A). The prosthetic component was removed, worn, and reinstalled to verify its interocclusal relationship; then a denture tooth was relined with flow resin (B–D). The socket was then filled with a collagen membrane (Geistlich Bio-Gide), bone graft (Geistlich Bio-Oss Collagen) and a 3D collagen matrix (Geistlich Mucograft) (D–H). The provisional was adjusted, polished, and then screwed with a torque of 20 N/cm2 (I, J). Six months after surgery, the gingival margin was in harmony with the adjacent teeth but a slight loss of volume was noted. The prosthetic rehabilitation was completed with a screwed ceramic crown (K–P). At the 4-year follow-up (Q–T). Surgical procedure: Dr Fausto Frizzera; restorative procedure: Dr Luiz Guilherme Freitas de Paula.
The porcine collagen matrix is capable of maintaining the height of the GM. Although the best results are obtained by using a connective tissue graft (Figs 29A–G), new biomaterials have been researched and developed to effectively replace the subepithelial connective tissue graft, showing promising results for increased tissue volume55.







29. A–G After performing surgery to treat compromised sockets, it was possible to obtain satisfactory and stable clinical and radiographic results after 5 years (initial (A, D), 6 months (B, E), and 12 months (C, F). Follow-up of the clinical case was previously described in Chapter 1. Surgical procedure: Dr Fausto Frizzera; restorative procedure: Dr Mateus Tonetto.
3. CLINICAL APPLICATION
Although an ideal treatment protocol for sockets is sought, it is necessary to assess the risks and benefits of each type of treatment and respect the biologi changes that occur after extraction. The immediate approach presents considerable benefits if the proper protocol is followed (see Figs 30–34 and Tables 02 and 03). Even in situations where there is compromised buccal bone, it is possible to reconstruct defects in V and U as long as the implant is installed in the ideal 3D position. It is still possible to limit short- and long-term peri-implant and papillary margin height loss by using a connective tissue graft.




30. A–D Protocol for immediate implant placement in compromised sockets. The implant should be positioned toward the lingual, at least 3 mm from the inner portion of the buccal gingiva (A). A slow resorption biomaterial is placed in the socket to completely fill the gap; it is still possible to slightly extend the buccal gingiva to increase its volume (B). A 2–3 mm thick connective tissue graft should be sutured at or beyond the gingival margin (only 20% of the graft can be exposed), its height should be greater than or equal to 5 mm, and its width should correspond to the distance between the mesial and distal papilla (C). A provisional with cervical undercontour should be placed without compressing the graft (D).

Table 02 Decision-making for the treatment of intact sockets

Table 03 Decision-making for treating a compromised socket
The treatment protocol used to prevent complications in the treatment of these clinical situations consists of:
-
Clinical and tomographic evaluation
-
Minimally traumatic surgery and flapless extraction
-
Placement of a narrow implant in the ideal 3D position.
-
Temporary confection with cervical undercontour and without occlusal contacts
-
Placement of a connective tissue graft on the buccal surface
-
Guided bone regeneration with inorganic bovine bone with 10% porcine collagen
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


