According to Harris (1997), bone resorption may have four main causes:
- Pathologic (eg, periodontal diseases, cysts)
- Surgical (eg, extraction of impacted cuspids, apicoectomy)
- Congenital (eg, micrognathy, oligodontia, palatal clefts)
- Physiologic (eg, tooth loss, age, pneumatization of the maxillary sinus)
The most frequent causes of the loss of bone substance are aggressive periodontitis and postextraction trauma related to wearing an unadapted removable prosthesis. The following clinical case shows the consequences of these bone pathologies.
This radiographic example shows a 40-year-old woman in good general health but with severe chronic periodontitis that has been stabilized for 2 years with conventional periodontal treatment (ie, initial nonsurgical treatment, periodontal surgery, and replacement of tooth 16 with a conventional fixed bridge) (Fig 2-2).
For the past 15 years, she has received regular maintenance every 4 months. The periodontal situation after 15 years was acceptable. However, bone loss evolved on the distal of tooth 15, which also showed signs of occlusal trauma (Fig 2-3).
An occlusal adjustment was completed and maintenance care was reinforced. The patient returned for follow-up after 2 years (1997) with a marked mobility of her fixed prosthesis. The radiograph showed terminal bone loss requiring the extraction of tooth 15 (Fig 2-4). A three-dimensional vertical and horizontal loss of substance is inevitable after healing (Fig 2-5).
Healing conditions depend on three factors:
1. Size of the defect: Healing quality depends on the critical size of the bone defect, which is specific to the type of bone. A defect above the critical size cannot heal properly and will induce a loss of substance.
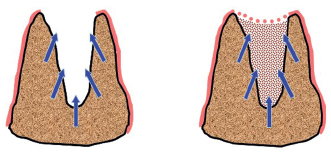
2. Number of walls: The number of bony walls determines the behavior of the overlying soft tissues. If the remaining bony walls are reduced to one or two walls, the unsupported soft tissues will collapse into the defect (Figs 2-6 and 2-7).
3. Type of defect: A close infrabony defect will heal more easily than an open defect, as the filling of the defect is mechanically easier (Fig 2-8). When the defect is open, it indicates the need for bone surgery. The correction of the loss of substance has to be done with a bone block graft, a bone filling material, or a membrane with or without bone chips. Through the use of powerful ultrasonic devices and their wide range of tips mountable on a handpiece, it is now possible to perform osteotomies, osteoplasties, and separation of the soft and hard tissues to correct these losses of substance.
As with any oral surgery, bone surgical techniques (eg, manual, mechanical, or ultrasonic) present indications and contraindications.
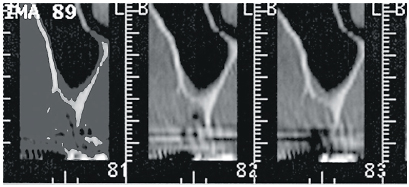
2-1 Loss of substance after tooth extraction making bone reconstruction compulsory prior to dental implant placement (computed tomography [CT] scan slices 81–83).
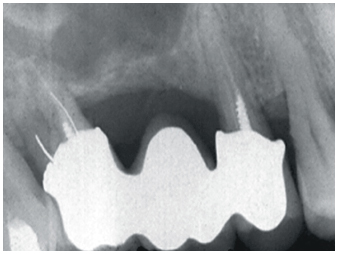
2-2 View of stabilized severe chronic periodontitis in 1980, 2 years after periodontal surgery.
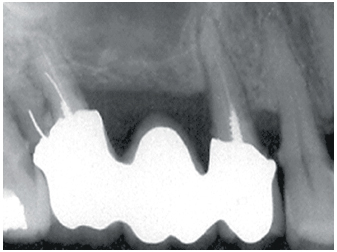
2-3 View in 1995: Bone loss on the distal part of tooth 15 presenting signs of occlusal trauma.
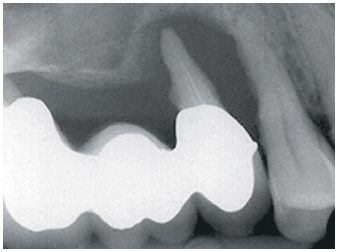
2-4 View in 1997: Significant tooth mobility and bone loss, resulting in tooth extraction.
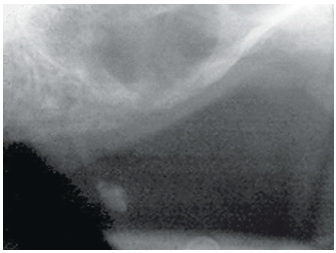
2-5 View after healing: Notice the important loss of substance.
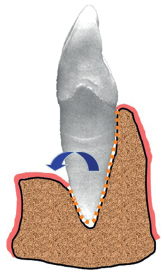
2-6 One-wall, open infrabony defect (absence of buccal bony wall) before tooth extraction.
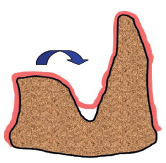
2-7 One-wall infrabony defect after healing without correction of the loss of substance.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses