Treatment of periodontal and preimplant defects
Horizontal ridge augmentation
Bone healing after tooth extraction reduces the size of the alveolar crest (Fig 6-1), thereby compromising dental implant placement. Performing a bone graft yields the necessary volume needed to reconstitute the loss of substance.
The graft must be securely transfixed with microscrews or micropins that anchor it to the recipient site. The junction between the graft and the donor site must be remodeled and improved by introducing bone chips or bone chips mixed with resorbable substitute biomaterial.
Clinical case
A maxillary central incisor (tooth 11) previously restored with a fixed prosthesis using a coronoradicular anchorage was extracted because of root fracture (Fig 6-2). The chronic infection provoked bone resorption (Fig 6-3). Owing to the vertical and horizontal defect, an esthetic and functional dental implant restoration could not be performed.
Figures 6-4 to 6-6 show the computed tomography (CT) scan analysis of the restored zone. Figure 6-7 shows the coronal oblique slices of the ramus distal to tooth 47 and the harvest zone. Figures 6-8 to 6-25 show the detailed steps of the intervention.
Surgical protocol
Autogenous bone graft harvested from the ramus using the Piezotome and the BS (Bone Surgery) tips (Satelec).
1. Disinfection of intraoral and extraoral tissues: Use povidone-iodine (eg, Betadine, Purdue Pharma), or chlorhexidine for patients who are allergic to iodine or its derivatives.
2. Local anesthesia at the recipient and donor sites: Additional anesthesia is given on the buccal and lingual nerves passing through the ramus and on the nasopalatine nerve for the maxillary recipient site.
Regional nerve block anesthesia is not recommended for two reasons:
- Local anesthesia is sufficient. Unlike teeth, bone structures are rarely resistant to anesthesia.
- The absence of regional anesthesia helps to keep complete control over the instruments used in close proximity to the inferior alveolar nerve.
3. Preparation of the recipient site (Fig 6-8):
- Large incisions extending on the lingual or palatal area expose the grafted bone.
- A full-thickness flap is elevated.
- The defect is measured.
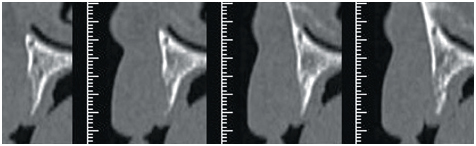
6-1 Coronal oblique reconstruction showing the loss of crestal width after healing.
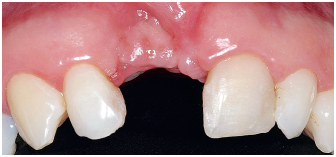
6-2 Extraction of tooth 11 due to root fracture.
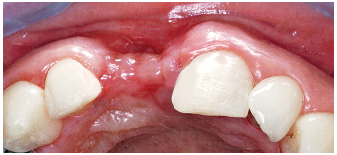
6-3 Occlusal view of the loss of substance.
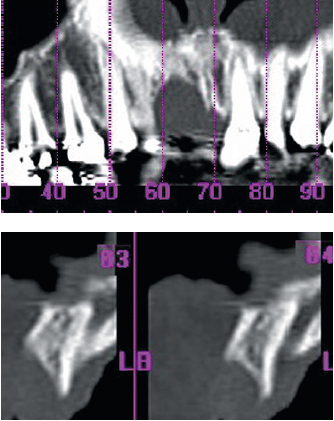
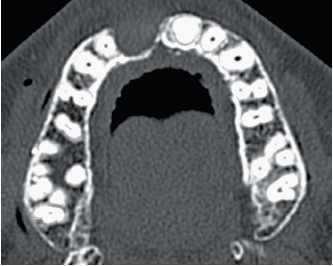
6-4 to 6-6 CT scans of the zone to be restored.
4. Harvesting of the ramus bone:
- The external oblique line is palpated.
- Incisions must be similar to the surgical removal of impacted third molars (ie, sulcular then along the ascending branch, slightly oblique toward the exterior). An additional mesial releasing incision allows better surgical comfort.
- Wide elevation avoids excessive tension on the tissues (Fig 6-9).
- Osteotomy:
| – | Longitudinal cut with the BS1 tip. The depth into the bone tissue is easily determined because of the markings (every 3 mm) indicated on the tip (Fig 6-10). |
| – | Two lateral transversal cuts with the BS1 tip (Fig 6-11). |
| – | An apical cut with the BS2 tip. The major advantage of the piezoultrasonic tips is their safety when used in proximity to soft tissues (Fig 6-12). |
| – | The corners of the block to be isolated are cut. |
| – | Using a flat Palti osteotome (Hu-Friedy), the bone block is dislodged without excessive force (Fig 6-13). The previous cuts must be deepened in case of difficulty in lifting the bone graft. In the ramus area, the removal of the piece of bone does not require the use of surgical chisels. Once the block is detached (Fig 6-14), it is then checked and directly submerged in physiologic saline solution. |
| – | A bone trap is installed and bone chips harvested using a BS4 tip. The BS6 tip allows harvesting of thin slices of bone, which help to fill the residual spaces between the graft and the recipient site. |
| – | Hermetic O-type suturing with a 3/0 slow resorbable suture (Fig 6-15). |
5. Adaption and fixing the graft at the recipient site: A delicate but essential step for the graft’s integration (De Carvalho et al 2000).
The use of ultrasonic-based surgery facilitates precision remodeling and recovery of bone chips.
- Fitting the bone block: the graft must be in close contact with the recipient site surface (Fig 6-16).
- The graft and the recipient site are adjusted with the BS1 tip (Figs 6-17 and 6-18).
- Graft fixation with osteosynthesis microscrews. The placement of two microscrews prevents rotational movement. The graft perforations are initially done on sterile gauze saturated with physiologic saline solution (Fig 6-19); then the block is adapted and screwed onto the recipient site (see Fig 6-20). It is also possible to make the initial hole in the gauze. Once the first microscrew is fixed on the site, the second perforation can then be made (Fig 6-21). Graft fixation can also be done with the aid of a cortical bone block clamp. Finally, remodeling of the graft is done using a BS4 tip (Fig 6-22), and bone chips are placed between the graft and the recipient site (Figs 6-23 and 6-24).
- An apical periosteal incision and partial thickness flap elevation allow complete coverage of the bone volume.
- Hermetic mattress suturing with a 4/0 silk nonresorbale suture (Fig 6-25). The provisional tooth is adjusted out of occlusion.
Please note: A splinted provisional tooth is preferred over a removable prosthesis during the 4-month healing period. A splinted provisional prosthesis limits the transfer of forces on the bone graft, which can provoke fibrosis between the bone structures.
The ultrasonic device and its tips are inseparable for this technique. The BS tips are indicated and perfectly adapted for this type of surgery. The BS1 tip is marked every 3 mm, allowing perfect control of the osteotomy. The BS2 tip permits the famous apical cut that is so difficult to perform with a rotary instrument. Using this tip helps in preserving the integrity of the surrounding soft tissues. The BS4 is the tip of choice for rapid retrieval of bone chips and for adapting and remodeling the graft.
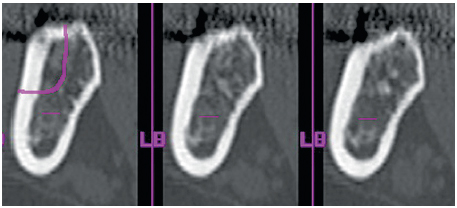
6-7 Coronal oblique section of the harvesting site on the ramus.
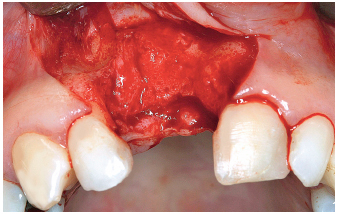
6-8 Preparation of the recipient site for a ramus bone block graft. Note the divergent releasing incisions that favor the flap vascularization.
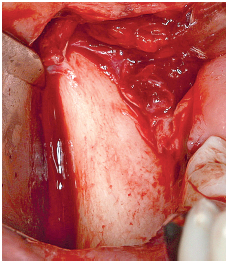
6-9 A large flap elevation of the donor site prevents tissue tension.
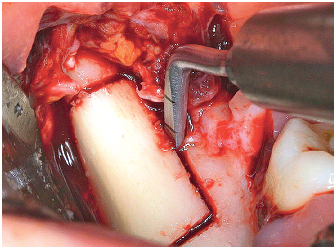
6-10 Longitudinal slice with the BS1 (Satelec) tip. The depth can be controlled because of the tip markings every 3 mm. In this case, the depth is 7 mm.
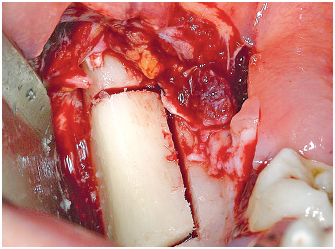
6-11 Outline of the transverse vertical sections.
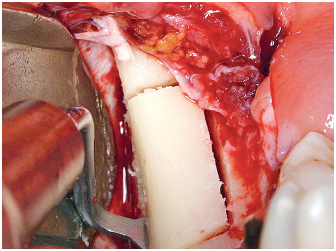
6-12 Apical section respecting the soft tissues close to the cutting zone using the BS2 tip (Satelec).
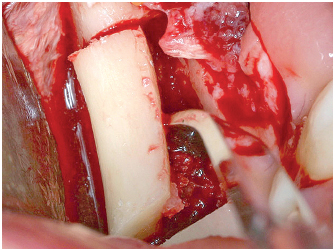
6-13 Dislodging the bone block without excessive force with a flat Palti osteotome (Hu-Friedy).
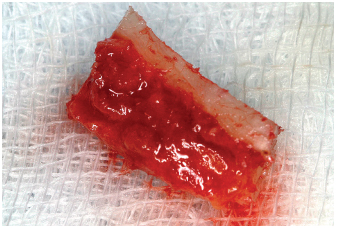
6-14 The bone block is checked then immersed in physiologic saline solution.
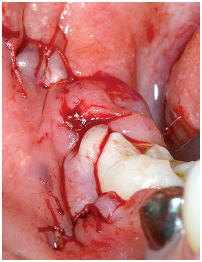
6-15 Hermetic O-type suturing using a slow resorbable 3/0 suture.
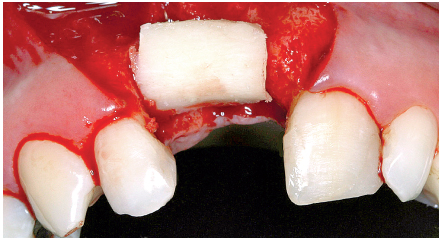
6-16 Graft adaptation and intimate contact with the recipient site.
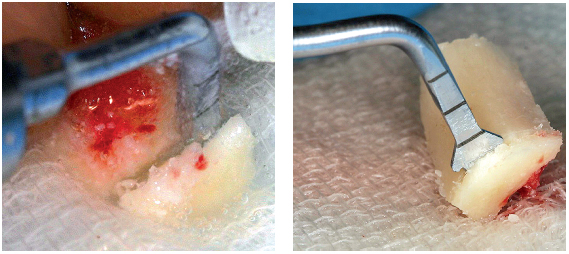
6-17 and 6-18 Remodeling of the graft using a BS1 tip before adaptation to the recipient site.
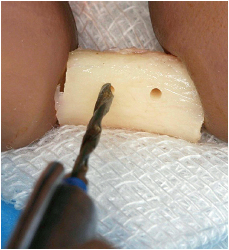
6-19 Drilling through the graft is performed on sterile gauze saturated with physiologic saline solution.
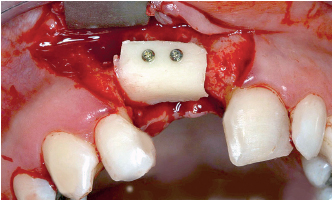
6-20 Graft fixation is considered a difficult step in the surgical procedure, but it is necessary for the success of the graft. Fixing it with two microscrews prevents rotational movement.
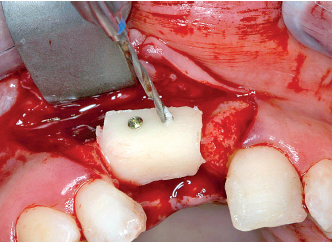
6-21 It is also possible to make the initial hole on the sterile gauze. After screwing the first microscrew onto the recipient site, the second perforation can then be made.
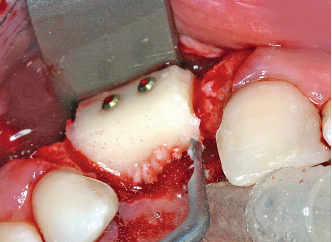
6-22 Remodeling the graft with the BS4 tip (Satelec).
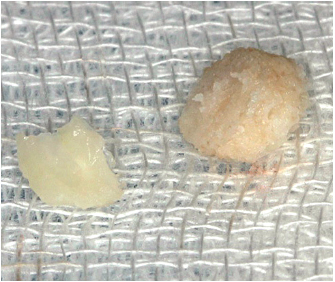
6-23 Bone chips harvested on the donor site after 4 minutes of bone scrapping.
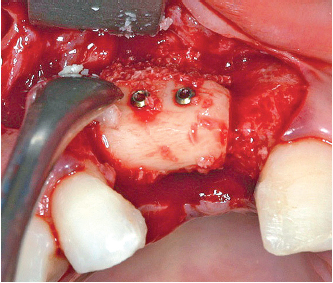
6-24 The bone chips are placed between the graft and the recipient site. An inlay/onlay position allows an increase in height and width.
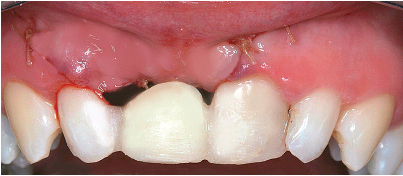
6-25 Hermetic matress suturing with a nonresorbable 4/0 silk suture. A temporary tooth is splinted with no occlusal contact.
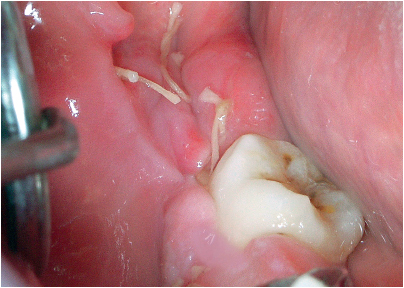
6-26 Healing of the mucosa of the donor site after 2 weeks.
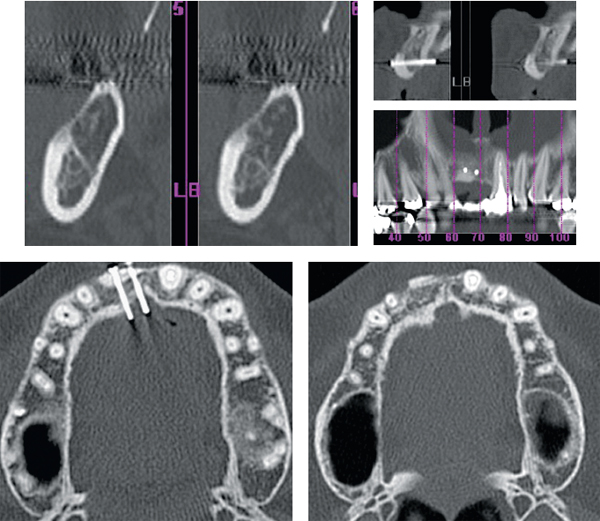
6-27 to 6-31 CT slices of the donor (28) and recipient sites (29, 30, and 31) before placement of the dental implant.
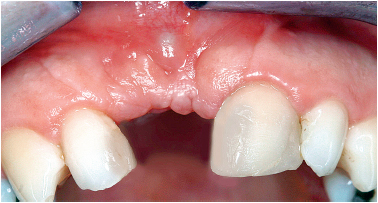
6-32 Osteosynthesis microscrews become visible under the mucosa after 3 to 4 months.
For 2 hours of surgical intervention, 15 to 20 minutes are devoted to osteotomy of the bone block and 5 to 8 minutes to harvesting bone chips. This estimated time frame depends on the bone quality.
Postoperative results
Surgical side effects occur less frequently in the area of the ramus than in the area of the chin (Clavero and Lundgren 2003). The postoperative results are significantly improved when using piezosurgery compared with those achieved using conventional instruments (Gruber et al 2005) (Fig 6-26).
The results can be compared with the postextraction conditions of an impacted third molar because of a similar flap elevation. Therefore, the postoperative conditions are not complicated, and the same postoperative instructions are prescribed to the patient. Our clinical experience, however, shows that the symptoms are significantly reduced, and the sutures can be removed after only 15 days. An example of a postoperative prescription follows. This prescription may also apply for interventions such as sinus floor elevation or piezoperiotomy, which are described later in this chapter.
Postoperative instructions
• To limit bleeding:
| − | Take lots of rest. During the 3 days following surgery, avoid sports and all other activities that accelerate the heartbeat. |
| − | Do not drink hot liquids. Eat warm and soft foods. |
| − | Avoid sucking and exploring the surgical zone with your tongue. |
| − | In case of bleeding, lie down and put pressure on the surgical site with your fingers and clean gauze for at least 20 minutes. |
• To limit pain:
| − | Follow the analgesic drug prescription. Begin an hour before the intervention, then continue regularly for 48 hours without waiting for the pain to recur. |
| − | In case of pain, continue with the same dosage. |
| − | Avoid smoking within the week following surgery. |
| − | Chew on the side opposite to the surgical site. |
| − | The pain varies from person to person and depends on the type of intervention. |
• To limit the swelling:
| − | Place a cold compress (eg, ice pack wrapped with a towel) on the facial area next to the site of the operation. |
| − | Follow the anti-inflammatory drug prescription. |
• Regarding oral hygiene:
| − | The teeth at a distance from the operated area may be brushed as usual. |
| − | Toothbrushing on the surgical site must not be done until the 15th day after surgery. It should be done gently and gradually with the prescribed soft bristle toothbrush and recommended technique. |
| − | A mouth rinse compensates for this limited brushing. |
| − | Do not stimulate the treated zone in any way. Pay attention to what you eat, to strong pressures, to wearing compressive removable prosthesis, and to any other stimuli. |
| − | This zone must remain nonfunctional for a month. |
• In case of emergency:
| − | It is normal to develop a hematoma and feel a dull pain on the bone harvest site. Call us in case of severe and throbbing pain, inflammation that makes swallowing difficult, persistent bleeding, or other alarming concerns. |
• The sutures will be removed after 15 days.
Healing
This new ultrasonic technology in surgery promotes bone healing (Horton et al 1975; Vercellotti et al 2005) essential for the future success of dental implant treatment. The most likely hypothesis for this observation is better control of the temperature while using the Piezotome (Tuffreau and Garbarini 2006). However, further biologic studies are needed to explain the acceleration of the healing process clinically observed with this instrumentation.
Two phenomena compete during the healing stage:
- Bone apposition: Helps to join the bone graft with the recipient site (Figs 6-27 to 6-31) by osteoconduction, osteogenesis, and osteoinduction.
- Bone resorption: Explained by the absence of mechanical stress of the attached bone tissue. The osteosynthesis screws become apparent 3 to 4 months after the surgery. The literature describes this phenomenon as “tent-like.” These figures show the type of remodeling and the volume that we can obtain after 4 months of healing (Figs 6-32 and 6-33).
If we refer to the biologic principles of healing after dental extraction, 3 months are necessary to replace the bony table and the socket with new bone (Atwood 1979). From clinical experience, a period of 4 months seems to strike a satisfying compromise between the time needed for apposition and too much time, leading to resorption. Minor resorption is often observed, which at this period is insignificant for the placement of the dental implant (Fig 6-34). Note that the screws were removed when the dental implant was placed.
At this stage, a submerged connective tissue graft was added. The objective was to accentuate the buccal prominence and to optimize the level of the papilla.
Figure 6-35 shows the completed restoration 6 months later. The gingivoplasty resulted in a regular gingival surface and good integration of the restoration in the esthetic zone.
Vertical ridge augmentation
A vertical defect of the alveolar crest is more difficult to correct. In the mandible, it is often possible to just place a membrane or to insert bone chips stabilized by the placement of a resorbable or nonresorbable membrane. These bone chips can be conveniently harvested in the ramus area.
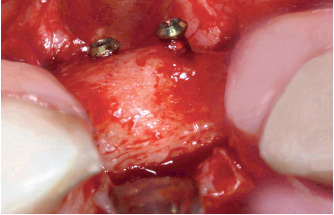
6-33 Bone resorption around the osteosynthesis screws.
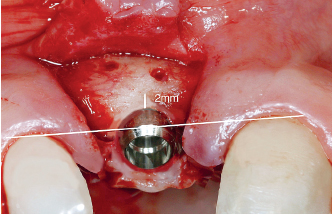
6-34 Dental implant placement after unscrewing the osteosynthesis screws.
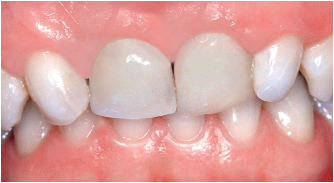
6-35 Definitive restoration 6 months later.
Clinical case 1
The following clinical case illustrates this technique (Figs 6-36 to 6-41).
Two inlay/onlay block grafts can be done for clinical situations that exibit a significant loss of substance. The bone is harvested either from the ramus or the chin. The surgical protocol is identical to the case previously described.
Reconstruction of bone loss through the sinus cavity
The rehabilitation of the partially or completely edentulous posterior maxilla with dental implants has shown very predictable long-term results (Albrektsson et al 1986; Adell et al 1990; Lekholm et al 1994; Lindquist et al 1996; Buser et al 1997; Weber et al 2000). However, some patients present unfavorable conditions in this particular zone of the dental arch. Often, these patients have either been edentulous for a long period of time, and/or they have experienced some form of trauma that has led to the loss of hard tissues. These circumstances may manifest as maxillary sinus pneumatization and/or alveolar ridge resorption, both of which compromise the vertical bone dimensions that are critical for dental implant placement in that location (Fig 6-42).
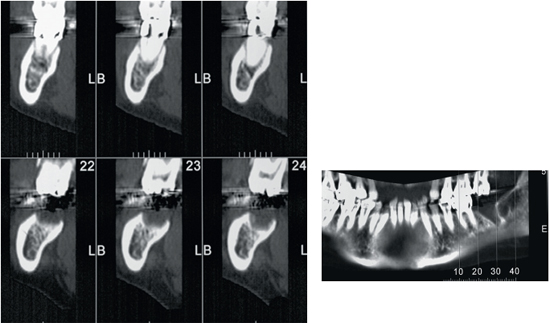
6-36 and 6-37 Preoperative CT scan of the bone loss after extraction of tooth 37 as a result of improper healing.
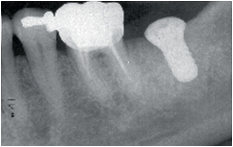
6-38 Placement of a WN dental implant (Straumann) on the alveolar bone grafted with bone chips from the ramus and covered by a resorbable membrane.
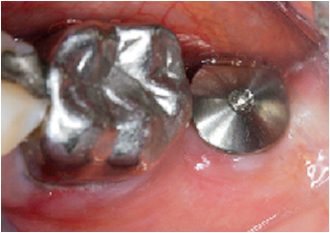
6-39 Tissues surrounding the healing abutment after 12 weeks.
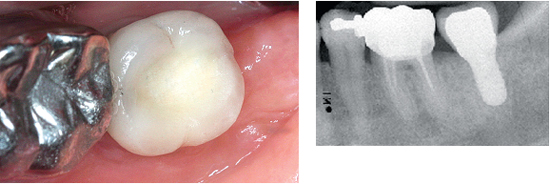
6-40 and 6-41 Clinical aspect and periapical view a year later.
To overcome these problems, bone grafting of the maxillary sinus has become a very popular and predictable procedure.
To perform a successful sinus floor augmentation, it is important to understand the maxillary sinus function and how it could be affected by the surgical intervention. The maxillary sinus (Fig 6-44) is lined with flattened, pseudostratified, ciliated epithelium. It is composed of basal cells, goblet cells that synthesize and discharge glycoprotein-containing mucus, seromucinous glands, and ciliated columnar cells. The ciliated epithelium clears sinus fluid that is removed by antigravitational movement. The natural ostium facilitates drainage of sinus fluid through the middle meatus of the nose, which is located cranially. In a healthy sinus, mucociliary clearance spreads from the sinus floor in a starlike pattern, ascends the sinus walls, and passes through the ostium (Takahashi 1984; Stammberger 1989; Kennedy and Zinreich 1991).
A sinus floor elevation generally does not interfere with sinus function when it is performed on a healthy sinus (Regev et al 1995; Timmenga et al 1997; Zimbler et al 1998; Watelet and Van Cauwenberge 1999; Peleg et al 1999; Van den Bergh et al 2000). On the other hand, the same procedure performed on an unhealthy sinus can contribute to fluid stagnation and bacterial overgrowth, leading to exacerbated sinusitis. Local preexisting conditions (eg, polyps that present an obstacle for the elevation of the sinus mucosa) require appropriate management prior to sinus floor elevation to avoid unexpected complications.
Thus, not only is the evaluation of the intraoral conditions important in identifying potential complicating factors but also the overall medical status of any patient who is planning to undergo this procedure. This presurgical evaluation may reveal potential contraindications, whether local or systemic.
Finally, to identify potential local contraindications, patients must undergo a thorough radiographic evaluation is necessary to identify any underlying sinus pathology and anatomic disturbances.
The CT scan is superior to conventional radiography in visualizing certain tumors, forms of rhinosinusitis, and sinusitis (eg, of odontologic origin).
For any of these diagnoses, the recommended treatment modalities (eg, endoscopic surgery, root canal therapy to alleviate sinusitis due to necrotic pulp) should be performed. Further diagnostics can then confirm the resolution of the given problem prior to the sinus floor elevation.
There are important anatomic obstacles (Fig 6-45) that might be contraindications to surgery when lifting the membrane (ie, elevation of the membrane must be large enough to allow placemen/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


