5
General Anatomy and Physiology
- the normal structure and function of the human body
- the circulatory system and associated medical conditions relevant to the dental team
- the respiratory system and associated medical conditions relevant to the dental team
- the digestive system and associated medical conditions relevant to the dental team
- the nervous system and associated medical conditions relevant to the dental team
Dental nurses must have a good underpinning knowledge of the normal structure and function of the human body, and especially of the oral cavity and its surroundings, to be able to understand the subjects of human health, the processes involved in the onset of human disease, and the methods available to prevent disease or to treat it when already present.
The anatomy and physiology of the head and neck structures and the oral cavity are discussed in detail in Chapters 9 and 10 respectively. This chapter deals with the anatomy and relevant physiology (that is, the functioning) of the main organ systems, to provide the necessary underpinning knowledge and understanding of the human body as a whole in relation to dentistry and dental nursing.
Definitions
The scientific discipline that deals with the life processes of living organisms is called biology. The study of the structures of the human body and their relationships to one another is called human anatomy, and the study of how the body actually functions is called human physiology.
The subject of anatomy covers not just the gross structure of the human body – muscles, bones, organs, etc. – but the equally important microscopic structures of the cells and tissues themselves that make up these gross structures. The microscopic anatomy of the tissues is not relevant to this text, but is covered in detail for those interested in Basic Guide to Anatomy and Physiology for Dental Care Professionals.
Cell biology
The basic unit of living organisms is the cell, and all (except red blood cells) contain a nucleus that holds the individual genetic material (DNA) that makes each of us unique. The DNA is held as chromosomes which separate and duplicate during cell division and growth.
Most cells are specialised in their roles and actions, and perform certain functions within the body. When similar specialised cells are grouped together to carry out these particular functions, they are called tissues. Groups of tissues that perform different functions are called organs – such as the heart or the liver – while those that have related functions are called systems – such as the digestive system or the respiratory system.
There are four basic types of cell in the human body.
- Muscle cells – these generate forces and produce motion; they may be attached to bones to allow limb movement or enclose hollow cavities so that their forces cause expulsion of the cavity contents (such as the movement of food through the digestive tract).
- Nerve cells – these can initiate and carry electrical impulses to distant areas of the body along their length to produce many actions, such as to cause muscle cells to contract or glands to release chemicals or fluids in the body (such as the salivary glands).
- Epithelial cells – these cover the body surface as skin or surround organs or line hollow structures within the body; they act to separate areas of the body from each other and from the external environment, to prevent the uncontrolled movement of harmful micro-organisms.
- Connective tissue cells – these connect various parts of the body together by anchorage and support, as in the whole bony skeleton and tendons and ligaments, and also contain the specialised connective tissue cells making up the blood and lymph systems.
All these cells require a source of fuel to produce the energy they need to work and carry out their individual functions, and this fuel is provided by the food that we eat. The energy it contains is released for use by the cells by the action of food digestion in the digestive system, and is used for any of the following actions.
- Maintain body temperature above or below that of the surroundings – this is called homeostasis.
- Produce movement to allow food gathering, and therefore the production of more energy.
- Allow reproduction to occur, for the survival of the species.
In addition, the body cells require oxygen to be able to burn the food eaten to produce the energy they require to function. Oxygen is brought into the body through the respiratory system, and transported around the body to every cell that needs it by the circulatory system.
Table 5.1 The body systems
| System | Composed of | Functions |
| Cardiovascular | Heart, blood vessels, blood | Transport of blood to lungs for oxygenation Transport of oxygenated blood to body Transport of deoxygenated blood back to lungs |
| Respiratory | Nose, throat, larynx, trachea, lungs |
Exchange of oxygen and carbon dioxide between the body and the atmosphere |
| Digestive | Mouth, salivary glands, pharynx, oesophagus, stomach, intestines, pancreas, liver, gall bladder | Digest, process and absorb nutrients from food Excrete waste products |
| Nervous | Brain, spinal cord, nerves, sensory organs | Give consciousness Regulate and co-ordinate body activities |
| Musculoskeletal | Bone, cartilage, tendons, ligaments, joints, skeletal muscle | Support and protect internal organs Allow movement |
| Immune | White blood cells, lymph, spleen, bone marrow, thymus | Defend against infection Produce red and white blood cells |
| Endocrine | All glands that secrete hormones | Regulate and co-ordinate body functions |
| Urinary | Kidneys, ureter, bladder, urethra | Regulate blood plasma Excrete waste products |
| Reproductive | Male or female sex organs | Reproduction |
| Integumentary | Skin | Protects against injury and dehydration Maintains body temperature |
The human body has 10 organ systems, each with various components and specific functions to allow the continuation of life, as shown in Table 5.1. The 10 body systems are identified in the first column, with those of particular relevance to the dental nurse listed as the first four. The second column identifies the structures that make up that system, while the third column states the function(s) of the system as a whole. These functions help to illustrate how the systems work together to enable the body to work effectively and maintain life. So for example, the circulatory system is responsible for the transport of oxygen around the body but the cells that actually carry it are made by structures within the immune system.
The four main body systems of relevance to the dental nurse are the circulatory system, the respiratory system, the digestive system and the nervous system.
Circulation
The main component of the circulatory system is the heart, a muscular pumping organ situated in the thorax (chest cavity). It is connected by blood vessels to every tissue in the body, and carries out the following actions.
- Pump oxygenated blood from the lungs to the body tissues so that they can work.
- Collect deoxygenated blood from the body and transport it to the lungs where the waste products it contains are excreted, by being breathed out.
The heart has four chambers within its structure; the upper two are called the atria and the lower two are the ventricles. The atria and ventricles are separated by one-way valves that allow blood flow in the direction of atria to ventricles only, and the left and right sides of the heart also have no communication between them. The right side of the heart transports only deoxygenated blood, from the body to the lungs, while the left side of the heart transports only oxygenated blood, from the lungs to the rest of the body again (Figure 5.1).
Figure 5.1 Gross anatomy of the heart.
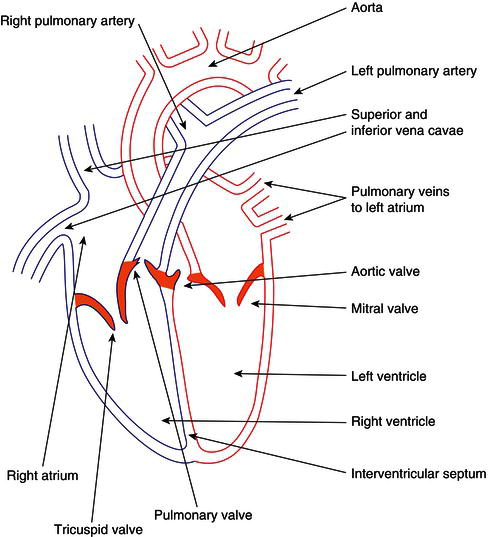
Action of the heart
Deoxygenated blood is collected from the whole body through the veins and transported to the right atrium via the inferior and superior venae cavae. As the heart beats, it pumps this blood through the one-way valve between the two right heart chambers (tricuspid valve) and into the right ventricle. The next beat pumps it out of the right ventricle and into the pulmonary artery where it passes to the lungs for reoxygenation.
Once oxygenated, the blood returns to the left atrium through the pulmonary vein, then it is pumped through the one-way valve (mitral valve) into the left ventricle. The next heartbeat pushes this blood out of the heart into the aorta, and then back around the whole body to reoxygenate all the cells and tissues and allow them to continue their normal functions.
The heartbeat itself begins on the top surface of the right atrium in a group of specialised muscle cells called the sinoatrial node or pace-maker. These cells receive electrical stimulation from two sets of nerves from the brain; one set speeds up the rate of the heart beat and the other set slows it down. In this way the heart rate is regulated to allow both exercise and rest as necessary. After each heartbeat, the blood is prevented from flowing backwards again by the one-way valves within the heart itself, which snap shut as the blood pressure increases within the successive heart chambers.
Circulatory system
The circulatory system is an enclosed loop of blood vessels, with the heart at its centre. The blood vessels taking oxygenated blood around the body are the arteries, the largest of which is the aorta, and these gradually decrease in size away from the heart to become arterioles and then capillaries. The capillaries are just one cell thick, and this allows the oxygen that they carry to be released into the surrounding tissues so that it can be used to burn food nutrients and create energy.
As oxygen passes out of the capillaries, the waste product of the energy production – carbon dioxide – passes from the surrounding tissues into the capillaries. This gas exchange process is called internal respiration (Figure 5.2). The deoxygenated blood then travels from the capillaries into small veins called venules, then into larger veins until it reaches the heart in one of the largest veins, the venae cavae. Deoxygenated blood from the upper body is transported to the superior vena cava, and that from the lower body to the inferior vena cava. This is the systemic circulation.
At the same time, and with each heartbeat, the deoxygenated blood in the right side of the heart is pumped to the lungs through the pulmonary artery (the only artery to carry deoxygenated blood). Here, the carbon dioxide is released into the lungs to be breathed out while oxygen that has been breathed in travels from the lungs into the blood capillaries, so that the blood is reoxygenated again. This gas exchange is called external respiration (Figure 5.3). The oxygenated blood is then transported to the left side of the heart in the pulmonary vein (the only vein to carry oxygenated blood) so that it can then be pumped back around the body. This is the pulmonary circulation (Figure 5.4).
Figure 5.2 Internal respiration.
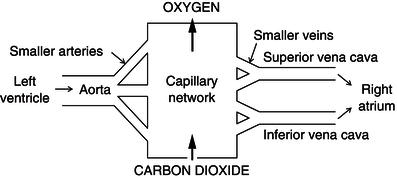
Figure 5.3 External respiration.
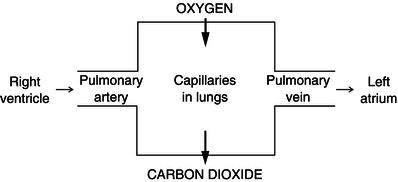
Figure 5.4 Circulation (deoxygenated blood shaded blue).
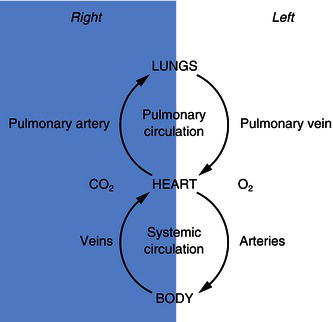
Blood vessels
When the blood leaves the heart in the arteries, it is under greatest pressure as a result of the heartbeat, so the walls of the arteries are elastic to allow them to expand as the powerful surge of blood passes along them. Once the initial wave of the pumped blood has passed, the artery walls relax back to their normal size again until the next heartbeat. This difference in pressure within the arteries can be measured and recorded as a person’s blood pressure. The maximum pressure of the blood in the arteries occurs during the peak of ventricular contraction, or systole, while the minimum pressure occurs at the end of ventricular contraction, or diastole.
So, blood pressure is recorded as systolic pressure over diastolic pressure, and in a healthy adult at rest it is usually around 120/80 millimetres of mercury, and is measured using a sphygmomanometer and a stethoscope, or an automated device (Figure 5.5). Also, when the artery passes over bone, the blood surge can be felt as the pulse at various sites around the body.
- Carotid pulse – at either side of the neck where the carotid arteries lie across the neck vertebrae, and above the surrounding muscles.
- Brachial pulse – at the inner surface of the elbow where the brachial arteries lie over the elbow joints.
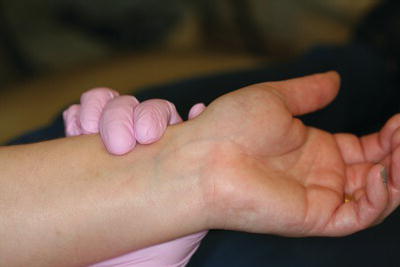
- Radial pulse – at the inner surface of the wrists as the radial arteries lie over the radius bone of the lower arms (Figure 5.6).
- Femoral pulse – at the top of the inner thighs as the femoral arteries lie over the femoral bone of the upper legs.
Figure 5.5 Measuring blood pressure.
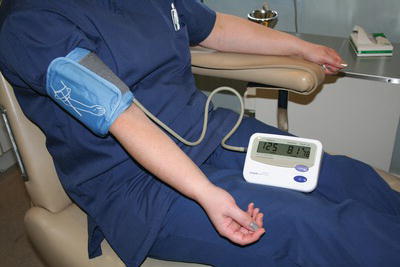
Figure 5.6 Taking the radial pulse.
In comparison to the arteries, the veins contain little elastic tissue. It is not required because the pressure of the blood surge is greatly reduced by the time it reaches the venous side of the circulatory system, as it is so far away from the source of the heartbeat. Indeed, the larger veins contain one-way valves along their length to prevent the blood from flowing backwards between heartbeats, in a similar action to that of the valves within the heart itself.
Blood
The circulatory system is filled with about 5 litres of blood in an adult, and it is regulated and kept at a temperature of around 37°C by the process of homeostasis. It consists of several cell types floating in a straw-coloured fluid called plasma.
- Erythrocytes – red blood cells.
- Leucocytes – white blood cells.
- Platelets – thrombocytes, which are fragments of larger blood cells called megakaryocytes.
Erythrocytes are biconcave disc-shaped cells (like a doughnut) with no nucleus, so they cannot divide and replace themselves but have to be constantly produced in the body by the red marrow of certain bones, such as the pelvis and the spinal vertebrae.
Their lack of nucleus and their shape provide the maximum space available for them to carry out their main task – to transport oxygen around the body. They achieve this by attaching oxygen to the red pigment they contain – haemoglobin. As discussed previously, oxygen is vital to all cells to be able to produce energy and carry out their various functions. It is picked up by the erythrocytes in the capillaries of the lungs during external respiration, transported around the body by the circulatory system to wherever it is needed, and then released into the tissues during internal respiration. The presence of the red iron-based protein haemoglobin within the erythrocytes gives blood its characteristic red colour. When the haemoglobin is bound to oxygen molecules, as in arterial blood, it has a bright cherry-red colour, and when there is little oxygen present, as in venous blood, it has a dark reddish-purple colour.
Leucocyte is the collective name for a group of several cells that are mainly concerned with defending the body against attack by micro-organisms and disease. They are made in several areas of the immune system, such as the lymph nodes and bone marrow, and circulate throughout the body at all times. However, when the body comes under attack from micro-organisms, massive numbers of leucocytes pass around the circulatory system to the area of disease, and then squeeze through the capillary walls to the body tissues that are under attack. Here, they surround and destroy the micro-organisms so that the disease is stopped from spreading. In very severe infections, the leucocytes are helped to destroy the invaders by the presence of antibodies released from the body’s immune system.
Platelets (or thrombocytes) also contain no nucleus, as they are just separate fragments of a larger blood cell found in the red bone marrow. Platelets are concerned with the coagulation of blood at the site of injury to prevent excessive blood loss. They achieve this by physically helping to plug damaged blood vessels by acting as a meshwork for the successful formation of a blood clot, as well as by releasing powerful chemicals that assist further in clot formation.
Plasma is the fluid part of the blood that carries the blood cells within it. It consists of about 90% water, with powerful chemicals called plasma proteins floating within, as well as the three types of blood cells. Plasma acts as the transport system of the body, by carrying numerous cells and chemicals from one area to another as they are needed. A summary of its functions is as follows.
- Transport of erythrocytes to allow oxygenation of the body tissues.
- Transport of waste carbon dioxide, dissolved in the plasma, from the body tissues to the lungs for exhalation and removal from the body via the respiratory system.
- Transport of digested food nutrients from the digestive system to the body tissues, for use as fuel to create energy.
- Transport of waste products from these cells to the kidneys, where they are filtered out as urine which is then excreted from the body through the urinary system.
- Transport of leucocytes to the site of any micro-organism attack, to allow the body to defend itself from disease.
- Formation of antibodies and antitoxins from special plasma proteins called globulins, which help the body resist against more severe infections.
- Transport of powerful chemicals called hormones, from the glands where they are made to the area of the body where they are required.
- Transport of the plasma protein fibrinogen to the site of any injury, to assist in blood clotting.
Relevant disorders of the circulatory system
Several disorders affecting the circulatory system are relevant to the dental nurse, as they may have an impact on the particular dental treatment offered. They may affect the suitability of local anaesthetics or conscious sedation techniques used, and patients suffering from some disorders may even present as a medical emergency during treatment. The recognition and management of medical emergencies are discussed in Chapter 6.
In particular with disorders of the circulatory system, the disclosure of any of the following points by the patient during medical history taking should be taken into full consideration by the dental team, with regard to the patient’s dental treatment.
- Heart conditions – any medical condition that affects the efficiency of the heart may prevent it from coping adequately during stressful situations, such as when experiencing pain, anxiety and fearful events like undergoing dental treatment.
- Blood disorders – in particular, those blood disorders that prevent adequate clotting of the blood, as the patient may then experience an uncontrolled haemorrhage; also, any disorders affecting the oxygen-carrying capacity of the blood which contraindicates the provision of dental treatment under some types of sedation techniques.
- Medications – certain medications may react with some types of local anaesthetics used in dentistry, especially those containing adrenaline as a vasoconstrictor, and possible interactions may occur with:
- thyroxine – for an underactive thyroid gland
- some antidepressants.
- Other medications
- Hormone replacement therapy (HRT) for menopausal women is often linked to a raised blood pressure, so adrenaline should be avoided.
- Elderly patients may be on a complicated cocktail of various medications, and the more drugs taken, the more likely an adverse reaction is to occur.
- Some antihypertensive drugs have an unwelcome side-effect of causing gingival tissue overgrowth, or gingival hyperplasia, which can make good oral hygiene levels difficult to achieve.
- Diuretics given to patients with hypertension act by encouraging fluid removal from the body; unfortunately this can result in reduced salivary flow and the patient will experience a dry mouth, or xerostomia.
Any medication (prescribed or ‘over the counter’) can be investigated for any potential side-effects or contraindications to dental treatment, by looking them up in the British National Formulary (BNF – Figure 5.7). This book is provided to all registered dentists by the Department of Health, and further information on how to receive copies is available at www.pharmpress.com.
The most relevant disorders of the circulatory system are outlined below.
Figure 5.7 British National Formulary.

Heart failure
This occurs when the pumping efficiency of the heart itself is inadequate, resulting in its inability to pump enough blood with each beat to allow the body to function normally, and to carry out its normal metabolic activities. It may involve either one of the ventricles or both together.
Heart failure occurs either due to a problem with the heart itself or due to a medical condition that increases the workload of the heart as it pumps blood around the body (that is, something that makes the pumping action less efficient or something that restricts the flow of blood away from the heart, so that more effort is required to achieve blood flow).
Those due to a problem with the heart itself include those listed below.
- Myocardial infarction – a ‘heart attack’, where there is a sudden reduction in the oxygenated blood supply to the heart itself through a coronary artery, often due to blockage by a blood clot (thrombus), and causing a section of the heart muscle itself to die – this is acute heart failure and often (but not always) results in cardiac arrest (the cessation of the pumping action of the heart).
- Myocarditis – inflammation of the heart muscle itself, usually as a result of a viral infection.
- Valvular disease – affecting any of the heart valves so that the filling or emptying of the heart itself is inadequate, and it has to work harder to overcome the resistance to efficient blood movement that the diseased valve causes.
Those due to a medical condition elsewhere that causes an increased heart workload include the following.
- Angina – a condition of myocardial ischaemia (reduced blood flow) caused by the narrowing and partial blockage of the coronary arteries, due to the presence of fatty deposits or atheromatous plaques. This is often referred to as ‘coronary artery disease’. When the heart workload increases, especially during exercise or at times of increased anxiety, the narrowed arteries are unable to supply sufficient oxygenated blood to the cardiac muscle, and symptoms similar to (but not as intense as) a heart attack are felt.
- Renal failure – kidney failure results in the sufferer being unable to remove sufficient waste fluids from the body (during urination). This fluid retention causes an increased blood/fluid volume which requires more work by the heart to pump it around the body. Eventually, a point is reached where the coronary arteries are unable to supply sufficient oxygenated blood to the cardiac muscle for it to work effectively, resulting in myocardial ischaemia.
- Hypertension – raised blood pressure at rest (rather than during exercise) means that the heart has to pump more strongly to move blood from the left ventricle into the aorta and so out to the body tissues, putting a constant strain on the cardiac muscle itself. In some cases the coronary arteries are unable to supply sufficient oxygenated blood, and myocardial ischaemia develops.
All these conditions except myocardial infarction (MI) are categorised as chronic heart failure, as the ineffectiveness of the pumping action of the heart deteriorates over time, rather than occurring suddenly as it does during an MI.
The plaques of fatty cholesterol that become deposited within the coronary arteries of an angina sufferer cause turbulence in the blood flow through these blood vessels. This not only restricts the volume of blood that can flow through them but it also allows any freely circulating platelets to become attached to the fatty deposits, causing the formation of a blood clot inside the blood vessel itself. This clot is correctly called a thrombus.
If the thrombus becomes detached from the blood vessel wall, it will naturally be carried by the circulating blood until it becomes trapped at a narrower point in the circulatory system, causing a sudden obstruction of blood to the tissues beyond. Once circulating, the clot is referred to as an embolus, and depending which blood vessel is obstructed, the results may be catastrophic.
- Angina – partial obstruction of one or more coronary arteries.
- Myocardial infarction – full obstruction of one or more coronary arteries.
- Stroke (cerebrovascular accident) – full obstruction of an artery supplying the brain.
- Pulmonary embolism – full obstruction of one of the pulmonary arteries supplying the lungs, often by an embolus originating as a deep vein thrombus (DVT) in the leg veins.
Cardiac arrest
The sudden failure of the heart to beat at all (asystole) or to beat ineffectively without pumping the blood (fibrillation) is called cardiac arrest, and is often the end result of a myocardial infarction. A cardiac arrest may also occur due to respiratory arrest, electrocution, severe blood loss, anaphylaxis, drug overdose or for other reasons including severe anxiety – a state that can be seen in some patients who have a profound fear of dental treatment.
Rheumatic fever
This occurs when a patient has suffered a previous illness that has caused damage to the heart valves. Any future episodes of bacteraemia (bacteria in the blood) such as those that can occur following invasive dental treatment, including scaling, can cause i/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


