Sports Dentistry and Mouth Protection
Developmental Evaluation of Child and Adolescent Athletes
Medical Assessment
Participation in athletic activities at both the recreational and organized sports levels continues to attract a large number of developing children and adolescents. Many dentists who are involved in the treatment of pediatric patients may be unaware of their patients’ involvement in sports simply because standard medical and dental history forms do not usually include questions that elicit this type of information and parents are often unaware of the dentist’s need to know. Therefore it is advisable as part of a thorough medical history to ask parents routinely about their child’s athletic activities.1
A complete medical examination by a physician is a necessity because several medical conditions in children and adolescents may limit or disqualify them from participating in athletics. The Americans with Disabilities Act of 1990 lists only a few conditions that absolutely disqualify an athlete; one such condition is infectious mononucleosis. Play ability must be determined on a case-by-case basis,2 as exemplified by recent reports of sudden cardiac deaths among otherwise healthy, adolescent athletes.
Growth Assessment
Another important aspect in the overall evaluation of pediatric dental patients who have identified themselves as participants in sports is the assessment of the developmental and behavioral characteristics of the individual patient. This information, together with an evaluation of the child’s physical growth, can be a valuable guide to the dentist in offering sound advice to the patient and parents for selecting age-appropriate athletic activities because a prediction of athletic injuries can often be based on the child’s stage of psychosocial development and physical maturity. Young children are often not ready to cope psychologically with the complex rules or physical demands associated with some team sports.3
Participation in sports involves many health hazards for growing children and adolescents. Parents who permit their children to engage in athletic pursuits run a calculated risk to enable the child or adolescent to achieve beneficial goals. The physical and mental health benefits that are gained, such as improving overall physical function, relieving anxiety, and improving school performance, must be evaluated by informed parents and judged to outweigh the risks of injury to the child or adolescent athlete.2
An Athlete’s Bill of Rights suggests several factors that are necessary to improve the risk/benefit ratio in safeguarding the health of high school athletes: “Proper conditioning helps to prevent injuries by hardening the body and increasing resistance to fatigue. Careful coaching leads to skillful performance, which lowers the incidence of injuries. Good officiating promotes enjoyment of the game as well as the protection of players. Right equipment and facilities serve a unique purpose in protection of players. Adequate medical (and dental) care is a necessity in the prevention and control of athletic injuries.”4
Intraoral Assessment
Just as the long bones in young children are not yet fully formed and are more prone to fracture and dislocation during athletic activities, so too is the alveolar bone surrounding the primary teeth less dense, often resulting in traumatic dislocation injuries such as avulsion or intrusive luxation. Intrusive luxation of a primary incisor is potentially one of the most serious traumatic injuries to the underlying developing permanent tooth bud. In addition to the possibility of ankylosis of the traumatized primary incisor, causing delayed or ectopic eruption of the permanent tooth, the underlying developing permanent tooth bud may also be displaced in the crypt. If this displacement occurs during the morphodifferentiation stage of tooth development, an abnormal curvature in the root or crown of the formed permanent tooth may result in a dilacerated tooth. If the traumatic insult occurs later during the apposition stage, when the deposition of dentin and enamel matrix takes place, a localized enamel hypoplasia of the crown of the permanent tooth may result in Turner tooth (Figure 40-1).
Young athletes in the early mixed dentition phase should be evaluated radiographically and clinically for the natural processes of root resorption, exfoliation of the primary teeth, and eruption of the permanent successors. Particular attention should be given to space loss associated with the premature loss of primary teeth. In the late mixed-dentition phase, the presence of a class II, division I malocclusion is indicative of an accident-prone dental profile and a causal factor for sports-related dental injuries.5 The clinical presence of an inadequate lip seal and excessive overjet place the protruding maxillary permanent incisors at greater risk for traumatic injury, especially in young athletes who participate in contact sports (Figure 40-2). The dentist should keep in mind that the large pulp chambers close to the surface in immature permanent teeth are highly susceptible to pulpal exposures in the event of a traumatic tooth fracture.
The evaluation of developing third molars in adolescent athletes is of particular importance. Not only can an athletic season suddenly be interrupted by the annoying and often painful eruption of third molars with associated acute pericoronitis, but mandibular fractures in the gonial angle region of developing third molars can also occur in adolescent athletes.6
The labial mucosa, specifically that in the mandibular anterior region of adolescent athletes, should be evaluated for the presence of soft tissue changes such as leukoplakia associated with the habitual use of smokeless tobacco (Figure 40-3). Snuff dipping is a common habit among athletes, and unfortunately it is occurring at an increasing rate, even among young children. Child and adolescent athletes should be warned at every opportunity about the serious intraoral and systemic dangers of this addictive habit. The use of smokeless tobacco has been associated most frequently with baseball; however, amateur wrestlers and male athletes who compete in sports that are organized according to weight classifications sometimes dip snuff to suppress appetite and control body weight.7 Thus, an evaluation by the dentist should also include a sports-specific dietary history.
Intraoral piercing is another high-risk fad that is associated frequently with young athletes. Postpiercing complications may result in acute medical conditions such as hemorrhage and swelling, local and systemic infections, airway obstruction, or allergic reactions (Figure 40-4). Tongue jewelry also may lead to tooth fractures, gingival recession, or alveolar bone loss and is particularly dangerous during sports activities.8 Most athletic regulatory agencies have banned the use of tongue jewelry during participation in sports.
Dietary Assessment
Amateur boxers and wrestlers often practice aberrant eating behaviors and intentionally become dehydrated to meet weight classification requirements. These practices can have a negative impact not only on strength and performance but also on the cardiovascular system. On exertion in such situations, hyperthermia and even death can result. Female athletes who participate in sports such as gymnastics or ballet and engage in similar aberrant eating behaviors are subject to the same systemic manifestations. Unhealthy nutritional practices may also predispose these young athletes to the possibility of injuries such as tibial stress fractures and shin splints.9
Especially with female adolescent athletes, the dentist should be alert for signs of the severe eating disorders of anorexia nervosa and bulimia. Enamel erosion on the lingual surfaces of the teeth (Figure 40-5), known as perimolysis, is associated with the binge-purge cycle and persistent vomiting. An accompanying clinical feature can be enlargement of the parotid glands.10 An extreme form of this type of eating disorder may progress to a condition known as the female athlete triad. This condition includes an extended eating disorder combined with intensive training and progresses to amenorrhea and osteoporosis.11 These severe eating disorders are often associated with psychological problems. In such instances, the dentist is obliged to recommend an appropriate referral for counseling.
At the other end of the spectrum are athletes such as football players, who desire to add bulk for increased size. This can present a dilemma for the dentist because one method of accomplishing this goal is to increase carbohydrate intake substantially. Dietary guidelines that minimize the effects on the teeth of highly cariogenic diets should be recommended. For example, it should be emphasized that the quantity of carbohydrates ingested is less critical for the dentition than the frequency of exposure or the type of carbohydrates consumed. Fruit, pretzels, and diet soda can be recommended as substitutes for sticky candy and sugar-containing soft drinks. Furthermore, these alternative foods can be consumed in greater quantities one or two times a day by those athletes desiring weight gain rather than bathing the teeth continuously with cariogenic sugars.12
One popular method of replacing fluids lost during athletic competition is ingesting sports/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


 Outline
Outline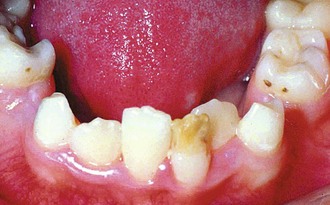
 FIGURE 40-1
FIGURE 40-1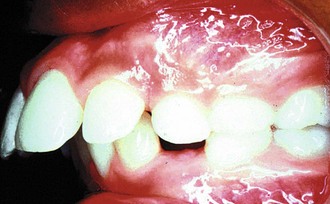
 FIGURE 40-2
FIGURE 40-2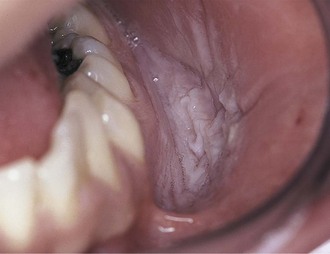
 FIGURE 40-3
FIGURE 40-3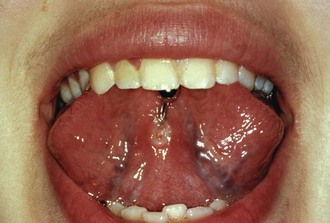
 FIGURE 40-4
FIGURE 40-4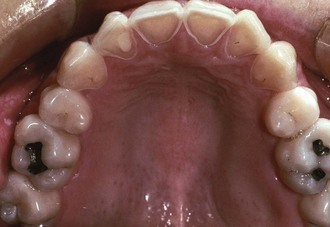
 FIGURE 40-5
FIGURE 40-5