4
Restorative Dentistry
Problems related to restorative dentistry constitute a significant portion of urgent dental treatment. Therefore, the dental profession serves its patients well by diagnosing and treating a full range of restorative urgencies. This section addresses the diagnosis and treatment of reversible pulpitis, root sensitivity, improper proximal contact, incomplete tooth fracture (cracked tooth syndrome), crown fracture, porcelain fracture, loose cast restoration, and fixed partial denture failure.
Symptoms of Reversible Pulpitis
A number of restorative situations can result in reversible pulpitis or symptoms compatible with that diagnosis. Caries in proximity to the pulp or a lost or defective restoration or fractured cusp are well-known examples. latrogenic etiologies—such as improper pulpal protection associated with restorative procedures and a restoration (any material) with improper occlusal contacts (a “high filling”)–can also cause reversible pulpitis symptoms as can a tooth in traumatic occlusion.
Diagnosis
A diagnosis of reversible pulpitis is made from a thorough history and careful clinical and radiographic examination of the patient (Table 4-1). Note that pain lingering more than a few seconds after stimulus removal and hot sensitivity relieved by cold almost always indicate irreversible pulpitis.
Table 4-1 Clinical Differential Diagnosis of Pulpal Pathology

Primary and Recurrent Caries
Caries and iatrogenic factors associated with tooth restoration can lead to pulpal pain. The clinician diagnoses dental caries on the basis of clinical and radiographic findings, while the degree of pulpal involvement determines the treatment necessary.
Treatment
| Step 1 | Isolate the involved tooth with a rubber dam to minimize pulpal contamination in case of exposure. |
| Step 2 | Remove gross caries. If a carious pulp exposure appears imminent, treatment options are direct or indirect pulp cap, or endodontic treatment; proceed to Step 5. |
| Step 3 | Place a sedative temporary restoration, such as zinc oxide eugenol (eg, IRM, LD Caulk). |
| Step 4 | Reappoint the patient for definitive treatment. |
| Step 5 | If caries approaches the pulp, cover the demineralized dentin or exposed pulp with a calcium hydroxide preparation (eg, Dycal, LD Caulk). |
| When wet necrotic caries is removed and a layer of leathery demineralized dentin remains over the pulp, an indirect pulp cap may be attempted. An indirect pulp cap is indicated when complete caries removal would result in pulp exposure (Figs4-1 and 4-2), but no periapical involvement exists. Teeth with a history of only mild hypersensitivity and slight provoked pain that does not linger may be treated in this manner. | |
| A direct pulp cap may be necessary if the “wet” (gross) caries proceeds into the pulp chamber. Asymptomatic teeth with small exposures (less than 1 mm diameter; Fig 4-3) and easily controlled hemorrhage (by gentle pressure with a cotton pellet) have the best pulp-capping prognosis. A suppurative exudate or large exposure usually contraindicates pulp capping. A lack of hemorrhage may indicate pulp necrosis, a walling off of a pulp horn, or very minimal pulpal trauma. The latter two conditions are amenable to pulp capping, but necrosis requires endodontic therapy. A symptomatic tooth is usually not a pulp-capping candidate. | |
| Step 6 | Follow with a layer of light-cured glass-ionomer cement (eg, Vitribond, 3M Dental) or compomer (eg, Dyract, LD Caulk) for flu oride content and strength to resist occlusal forces. |
| Step 7 | The objective of all pulp capping is the preservation of pulp vitality. Any capping procedure has a guarded prognosis, and these patients require regular follow-up. |
| Note: | Placement of calcium hydroxide (Fig 4-4) and glass-ionomer cement or compomer in the depths of the cavity is suggested after excavation of any carious lesion in close proximity to the pulp. These materials ensure proper pulpal treatment in the event of an undetected microexposure. Calcium hydroxide stimulates dentin bridging; however, 89% of bridges have tunnel defects, thus not hermetically sealing the pulp. Therefore, if time permits and the cavity warrants, the treatment of choice for posterior teeth is proper basing, then restoration with bonded amalgam or posterior composite as indicated (Fig 4-5). Bonded amalgam resists microleakage and provides far superior resistance to occlusal forces compared to temporary cement or composites. In limited time situations, place a sedative noneugenol temporary over the pulp cap. If this course is taken, allow 6 weeks for healing before placing the final restoration. |
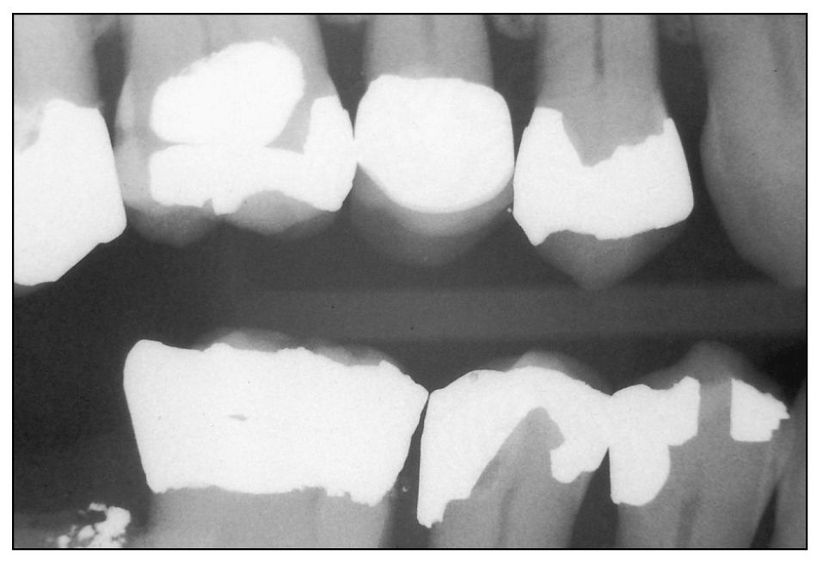
Fig 4-1 Tooth 29 (distal) with caries under the restoration. Removal of defective restoration and caries may result in pulp exposure.
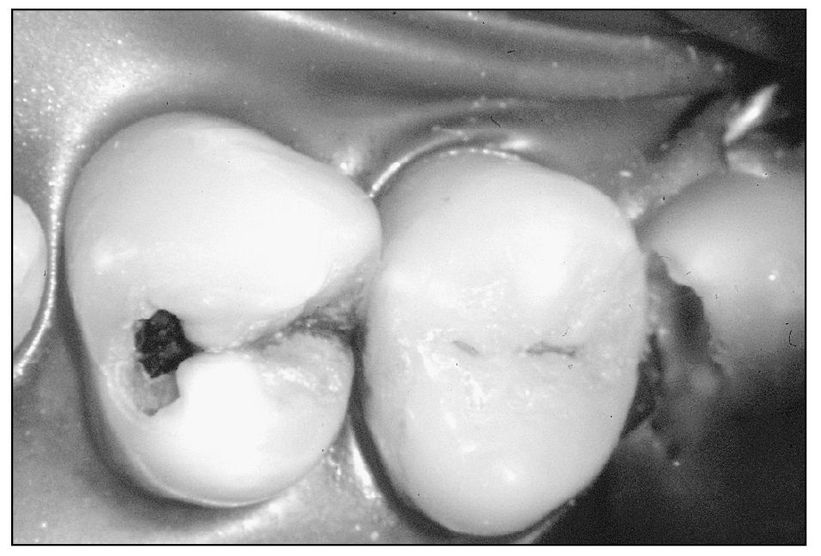
Fig 4-2 Premolar with deep proximal and occlusal caries.
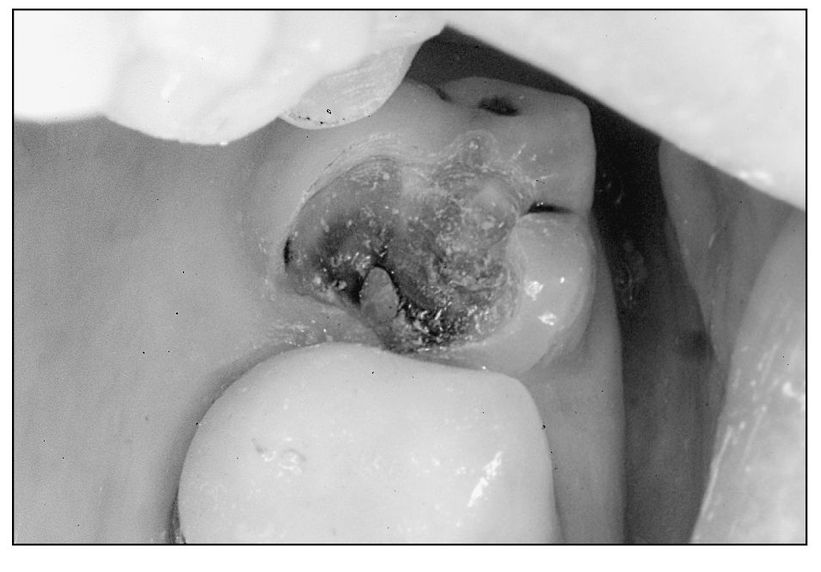
Fig 4-3 Small pulp exposure amenable to pulp capping.
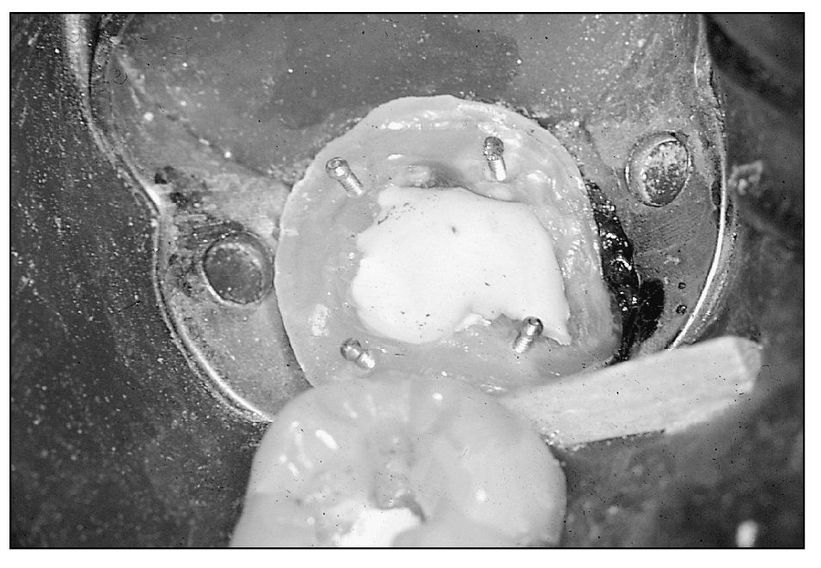
Fig 4-4 Calcium hydroxide placed in close proximity to pulp.

Fig 4-5 Placement of bonding agent for bonded restoration.
Lost Restoration or Fractured Cusp
A defective or lost restoration or a fractured cusp (Fig 4-6), without pulpal involvement, often requires urgent treatment. These situations may or may not present symptoms. If symptoms occur, they are similar to reversible pulpitis, often with the addition of sensitivity to sweets.
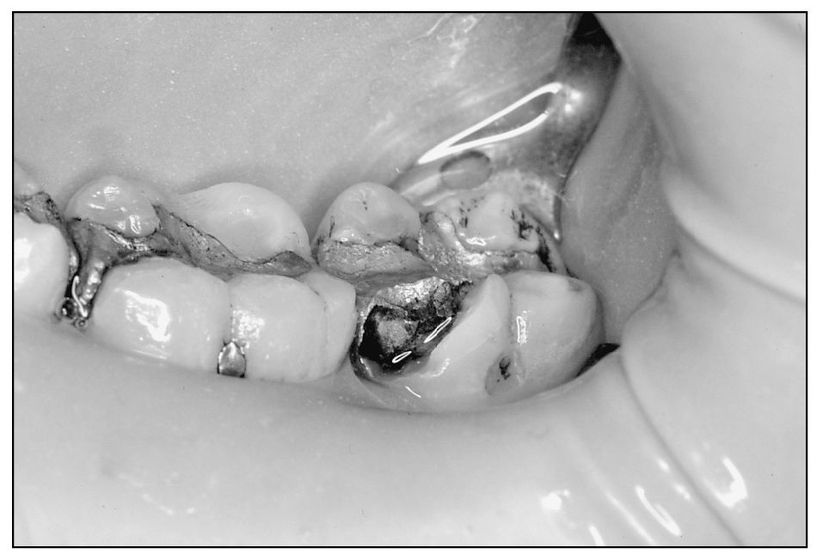
Fig 4-6 Fractured mesiofacial cusp of tooth 18.
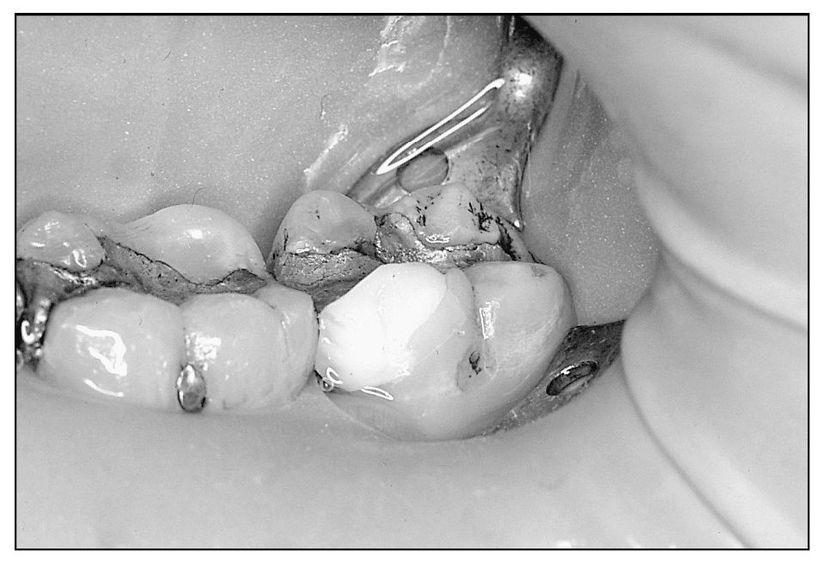
Fig 4-7 A composite temporary restoration replacing mesiofacial cusp of tooth 18.
Treatment
| Step 1 | Smooth rough edges to minimize irritation to oral soft tissues. If time permits or if patient is symptomatic, proceed to Step 2. |
| Step 2 | Create mechanical undercuts if necessary (often in an existing restoration). Many failures have been observed when bonding only is depended on for retention. If retention is inadequate for an intracoronal temporary restoration, proceed to Step 4. |
| Step 3 | Place a glass-ionomer cement or composite resin in the fractured area (Fig 4-7). If the patient is symptomatic, place calcium hydroxide in the area closest to the pulp. |
| Step 4 | Fit an aluminum, stainless steel, or plastic crown form (plastic crowns usually require more occlusal reduction than metal). Proximal slices with a No. 69L bur may be necessary to allow placement of the temporary crown. |
| Step 5 | Cement crown with a suitable luting agent. Use a noneugenol temporary cement (Temp Bond, NE Kerr), especially if a bonded restoration will follow. The residual eugenol may inhibit or retard the polymerization reaction of resin liner or cements. |
| Step 6 | Take care to adjust the occlusion on any temporary restoration, as even a relatively soft cement can set up in superocclusion and, with function, cause further irritation of the pulp before the restoration wears down. |
| Note: | If time permits, repair the symptomatic or asymptomatic lost restoration or fractured cusp with a “permanent” restoration (eg, well-retained bonded amalgam that can act as a core for a crown if indicated). The adhesive seals dentinal tubules and prevents microleakage, thus reducing sensitivity. In particularly sensitive teeth, a dentin desensitizer (Microprime, Danville Engineering, or Gluma Desensitizer, Miles) may be used prior to bonding. |
High Restoration (Superocclusion)
Any restorative material placed in superocclusion can result in symptoms compatible with reversible pulpitis. If a metal restoration is “high,” a shiny spot will almost always be present (Fig 4-8), and this area can be reduced. Use a marking medium such as Accu-film (Parkell) to locate high spots or interferences on metallic or nonmetallic materials. Make sure to check all occlusal positions and combinations of positions. Often overlooked movements are lateral protrusive and crossover. Crossover is the extreme lateral position when the mandibular canine “crosses over” the maxillary; anterior teeth should contact-posterior contact usually represents an interference (Fig 4-9). Take care during adjustment to maintain centric holding areas, since their removal can result in teeth drifting and the potential development of more interferences.
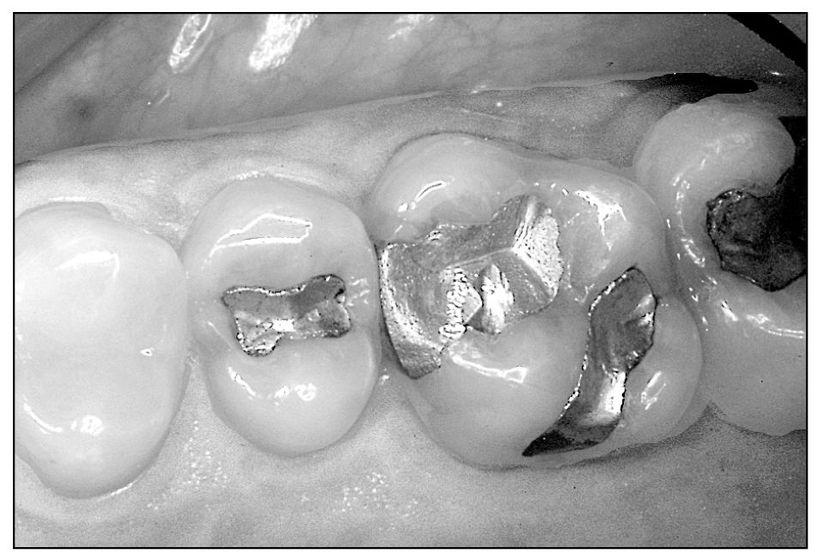
Fig 4-8 “High” amalgam restoration showing shiny spots in mesial fossa and lingual groove.
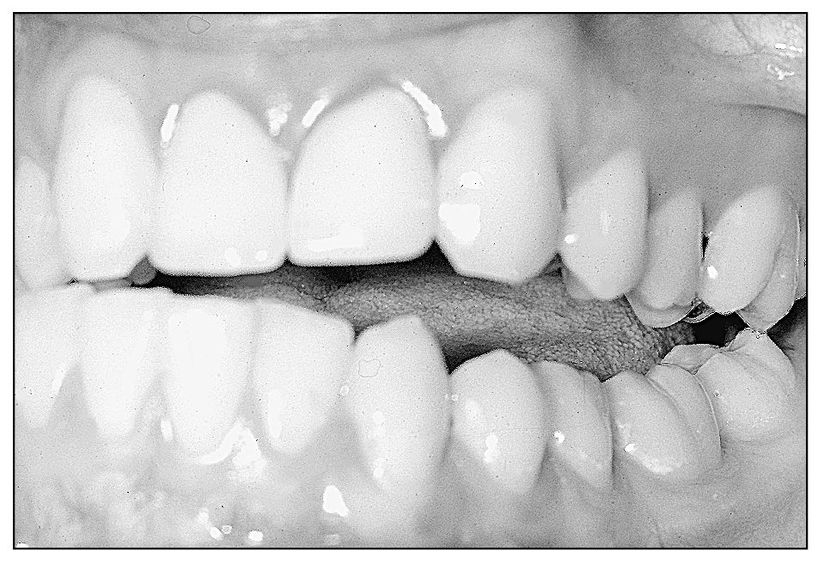
Fig 4-9 Crossover interference on distofacial cusps of teeth 14 and 18.
Treatment
Use the following steps to assess centric prematurities:
| Step 1 | Place a strip of shimstock (Artus or Parkell) on the tooth with the suspected high spot (Fig 4-10), and ask the patient to close lightly in the intercuspal position. |
| Step 2 | Gently pull the shimstock, and if it pulls away, the centric holding area has been overreduced. If occlusal contact exists, the strip will not pull out. |
| Step 3 | Place shimstock on an adjacent tooth (sometimes both must be checked), and gently pull with the patient in maximum intercuspation (MI); if the strip pulls away, the restored tooth is high. |
| Step 4 | Repeat the same procedure while assisting the patient in centric relation closure to assess prematurities there. |
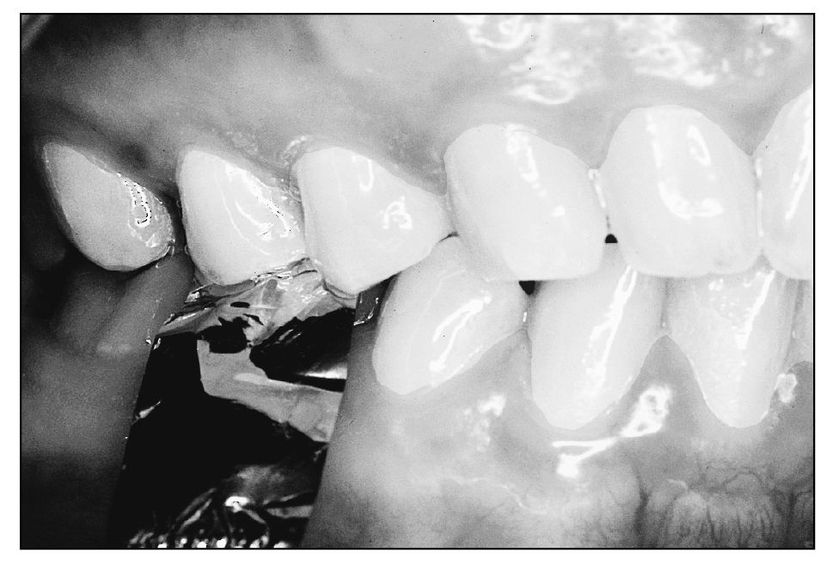
Fig 4-10 Shimstock is used to detect interference between the second premolars.
Eccentric interferences can also be checked with shimstock:
| Step 1 | Place the strip on the restored tooth and have the patient close; tug the strip and it should hold, verifying that MI contact is cor rect. |
| Step 2 | Have the patient move in each excursion while gently pulling the shimstock. If the strip releases as the patient begins to move, there is no interference. If teeth grasp the strip, an interference may be present in the excursion being executed except in the case of a guiding tooth. |
A method for verifying eccentric interferences as opposed to normal occlusal contact involves using two shimstocks at the same time:
| Step 1 | Place one shimstock on the tooth with the suspected interference and the other on a guiding tooth for that movement. For example, if a balancing interference on a maxillary right first molar in a patient with canine guidance is suspected, place shimstock on the right first molar and left canine. |
| Step 2 | Gently pull both strips simultaneously while the patient makes a left lateral excursion. If the molar grasps the strip and the one on the canine pulls out, a balancing interference exists. If the opposite occurs, there is no interference on the molar. |
| Step 3 | Repeat this procedure while inducing side shift by gently guiding the mandible in the direction of the movement being tested (an assistant can hold one of the shimstocks). |
| Note: | Another consideration when adjusting a seemingly high restoration is Thielemann’s principle, which states that an anterior “interference” may be caused by a posterior, opposite-side prematurity shunting the mandible. The result is a horizontal impact diagonally across the arch (Fig 4-11). However, there are corollaries to this law: clinical examples exist of posterior to anterior same-side, and anterior to posterior same- and opposite-side horizontal impact masquerading as high restorations and interferences. Be prepared to check the entire occlusion, especially in cases of recurring “high spots.” |
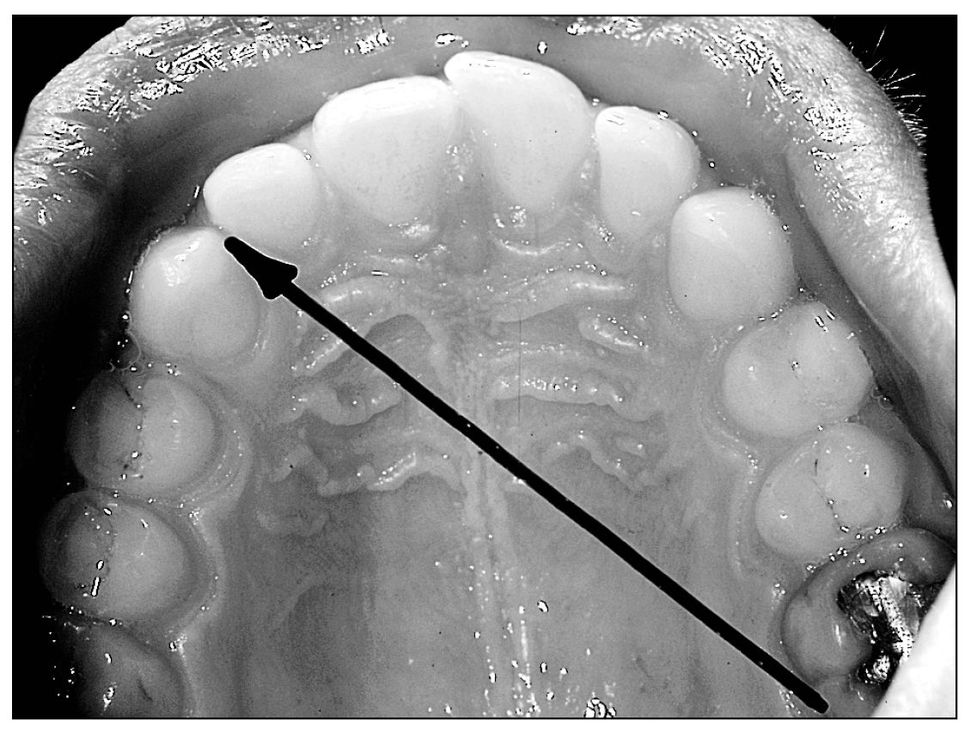
Fig 4-11 Thielemann’s principle depicting a prematurity in the molar area causing impact on the opposite-side canine-lateral incisor area.
Root Sensitivity
Root sensitivity is an urgent problem that can mimic reversible pulpitis in its diagnostic presentation. A sensitive root may react to sweet, hot, cold, or biting pressure, and digital contact with the gingival area; erosion and/or gingival recession may be seen. An abfraction lesion may also be present (Fig 4-12). Abfraction occurs when hyperocclusion flexes the tooth at the gingival, weakening the area and making it susceptible to erosive and abrasive elements (acid from food, horizontal toothbrushing, etc). Therefore, check occlusion, as noted in the previous paragraphs, for interferences whenever these lesions are observed.

Fig 4-12 Gingival abfraction lesions on teeth 11 and 12.
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


