Chapter 4
Reorganising the Occlusion
Click on the DVD icon to watch the video
Aim
The aim of this chapter is to demystify “reorganising the occlusion” so as to make this important aspect of dental care more accessible, but at the same time to highlight potential areas of difficulty.
Outcome
At the end of this chapter, the clinician should:
-
understand the difference between reorganising an occlusion and conforming with the presenting intercuspal position (ICP)
-
recognise when occlusal reorganisation is indicated
-
be familiar with the principles involved in occlusal reorganisation:
-
using centric relation (CR) as the starting point for reconstruction
-
deciding on the vertical dimension
-
designing the pattern of occlusal contacts in ICP and mandibular excursions
-
-
appreciate the practicalities of reorganising, including the recognition of cases that are potentially more difficult.
Introduction
A “reorganised occlusion” is an occlusion in which the pattern of occlusal contacts is deliberately changed or reconstructed.
Reorganising the occlusion is not something that needs to be undertaken for many patients, but there are times when such action is the only way, let alone the most appropriate and easiest means, to solve a clinical problem. It is a procedure that has to be done with care. Its exponents often make it appear mystical or impossibly technical. Actually, the underlying principles are very simple and will be familiar to all practitioners. Occlusal reorganisation should not, therefore, be viewed as intimidating. That said, the importance of the basic technicalities should not be underestimated, and careful thought and preparation are needed prior to the application of the technical skills necessary to complete the procedure successfully.
One of the reasons that this can seem a deeply intimidating subject is that reorganising the occlusion cannot simply be done by following an instruction manual. Every case is different, reflecting the huge diversity of form and condition of teeth and their relationships. Consequently, it is essential to grasp the principles fully before thinking through the technical detail for any given individual.
In a sense, reorganising the occlusion brings together all of the basic occlusal concepts that were introduced in Chapters 1 to 3. In this chapter, we will refer back to these chapters, and their animations, and forwards to Chapter 8, along with its videos detailing clinical procedures.
Why Bother?
The answer to this is relatively simple. You reorganise an occlusion because the existing ICP is unsatisfactory for your restorations, or because there is a specific problem that really can only be solved by reorganising the occlusion. That is all very well, but it is still not very clear which clinical circumstances dictate or suggest reorganisation. This question is perhaps best answered with some examples. Those given below are not the only circumstances where you may wish to reorganise, but they do illustrate a range of situations where reorganising may either be necessary or worth the effort and cost. Decisions about whether to conform to an existing occlusion or to reorganise it are not always black and white.
Example 1: The Complete Denture
Making a complete denture may not seem like reorganising the occlusion, but that is exactly what it is. The complete denture has an occlusion that is built from nothing. If there are no teeth, there can be no occlusion (Fig 4-1). Whenever you make a new set of complete dentures, you effectively have to rebuild the occlusion such that the teeth fit together without displacing the denture every time the mouth is closed. This rebuilt occlusion is, to a greater or lesser degree, reorganised, even if you try to recreate what was there before. Normally, though, you start afresh, using as your starting point a jaw position determined by the temporomandibular joints (TMJs), which is of course CR, as described in the previous chapter (Fig 3-1).
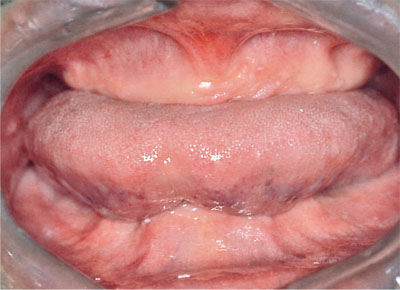
Fig 4-1 “Big Mac”: where there are no teeth there is no ICP. Instead, the TMJs are used as the starting point for denture construction, with the occlusion reorganised around CR.
Although making dentures may not seem to fit a common image of reorganising the occlusion, the basic principles used to make complete dentures are the same as those used to reorganise the occlusion for dentate people. However, as we will see, although CR is used as the starting point to create a new ICP for both complete dentures and natural teeth, there are significant differences in the way the excursive contacts are arranged. With complete dentures, the widely accepted ideal is to have bilateral excursive contacts occurring simultaneously between as many anterior and posterior teeth as possible. This “balanced articulation” is simply the means to stop the dentures from tipping during function. Balanced articulation is an example of an “occlusal scheme”, and selecting an occlusal scheme is an important part of reorganising. We discuss occlusal schemes later in the chapter, but Box 4-1 gives a flavour of their history.
Box 4-1 Balanced articulation
Balanced articulation has long been used to construct complete dentures, but it does not perform well when used to reconstruct dentate patients – as both the Gnathologists and Pankey–Mann–Schuyler groups discovered to their embarrassment in the middle of the 20th century. These two groups of dentists, working independently on the west and east coasts of America, did much to pioneer the practicalities of occlusal reconstruction. Each group had its own characteristic techniques and instrumentation. For almost 30 years both groups restored dentate patients with balanced articulations. Then, in the late 1950s, both groups acknowledged that there were problems with this approach: patients often suffered discomfort from heavy non-working-side contacts. Furthermore, these interferences appeared to cause wear, fracture and mobility of the restored teeth. Consequently, for dentate patients both groups abandoned balanced articulation in favour of what they observed to work naturally in healthy dentitions. The Gnathologists favoured canine guidance while the Pankey–Mann–Schuyler followers preferred group function, but both stipulated disclusion of the posterior teeth on the non-working side and in protrusion (see Table 4-1).
| Occlusal scheme | RCP–ICP relationship | Excursive contacts | Comments |
| Gnathological (1964) | Coincident, with tripod contacts | Canine-guided lateral excursions, posterior disclusion in all excursions. Anterior and posterior contacts are mutually protected1 | Good for restoring cases without a large horizontal component of RCP–ICP slide. Real purists would insist on the use of a fully adjustable articulator and all that goes with it. |
| Youdelis (1977) | Coincident, with tripod contacts | As for gnathological, but designed to drop into group function if canines wear or move | Useful option where excursive parafunction cannot be controlled or where the canine is compromised |
| Pankey–Mann–Schuyler (1963) | Area of freedom2 between ICP and RCP (<0.5 mm) and morphology functionally generated | Anterior guidance determined functionally on temporaries. Either canine guided or group function | The potential for error with the functionally generated path technique, which is used to determine the occlusal morphology of posterior teeth is considerable |
| Area of freedom in centric (1982) | Area of freedom between ICP and RCP (0.5 mm ± 0.3 mm); cusp to fossa occlusion | Either canine guided or group function, but anterior guidance will be delayed during posterior contact in area of freedom | Useful where there has been a large horizontal component in the RCP–ICP slide before treatment. Area of freedom needs careful adjustment |
| Balanced occlusion (1960) | Area of freedom between ICP and RCP | Balanced working and non-working contacts in lateral excursions. Balanced anterior and posterior contacts in occlusion | Keeps complete dentures stable during excursions, but difficult to manage in the natural dentition and risk of non-working-side overloading |
| Nyman and Lindhe (1983) | RCP and ICP must have even contact | Bilaterally balanced excursive contacts determined in provisional (long-term temporary) restorations and then copied into definitive restorations | This is used in cross arch bridges where there is advanced, but controlled, periodontal disease. Balanced contacts give stability to an otherwise mobile bridge |
Notes:
1: “Mutually protected” means that in ICP the posterior teeth support maximum biting force while the anterior teeth are just out of contact, but in excursions the anterior teeth provide guidance to disclude the posterior teeth and protect them from lateral loading. To avoid locking the condyles into CR, this guidance should start shallow and then become steeper.
2: Area of freedom (freedom in centric) is designed to prevent condyles being locked into CR.
Example 2: Rebuilding the Aging Dentition
In a mouth affected by decades of dental disease there is often extensive tooth loss and multiple restorations. This is now a common occurrence in people from late middle age onwards. The result, after years of repeated cycles of damage and restoration, is a patchwork of spaces and heavily restored teeth. Remaining teeth drift and overerupt, and many may have huge restorations or poorly constructed crowns. An example of this sort of problem is shown in Fig 4–2. There comes a point where a path has to be chosen: the dentist and the patient have to make a decision. Do you leave things ticking over and patched up to conform to what is there, or will this lead to difficult problems in the future? Does a bold step need to be made to remove the remaining teeth and reorganise the occlusion with a complete denture or implant-retained prosthesis? Or, would it be better to use the remaining natural teeth as a basis for building a stable, functional and aesthetic (reorganised) occlusion, and if so is it a sensible investment? The application of basic principles is important, and some lateral thought and imagination may be required to do this successfully.
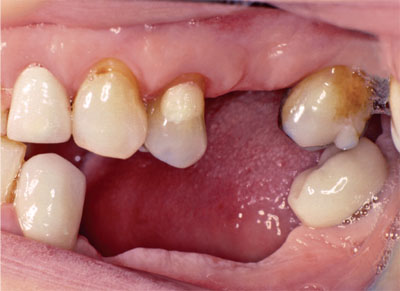
Fig 4-2a Patient with missing, tilted and heavily restored teeth. Before reconstruction, deflective contacts and interferences were removed.
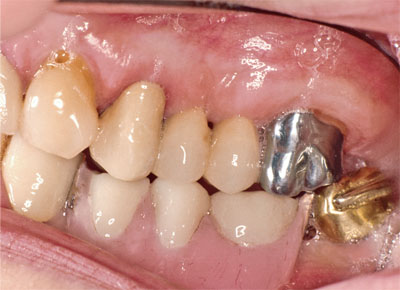
Fig 4-2b Notice the lower occlusal plane levelled with a new gold crown to eliminate the presenting protrusive interference.
Example 3: Protecting and Restoring a Worn Dentition
When teeth suffer excessive wear this can affect appearance and function, as well as causing symptoms of sensitivity and pulp damage. The reasons for wear are discussed elsewhere and, clearly, understanding why it has occurred is important in planning its management. Irrespective of cause, if treatment is indicated to make the teeth look better, to prevent the symptoms associated with wear or to prevent the wear progressing, the teeth need to be/>
Stay updated, free dental videos. Join our Telegram channel

VIDEdental - Online dental courses


